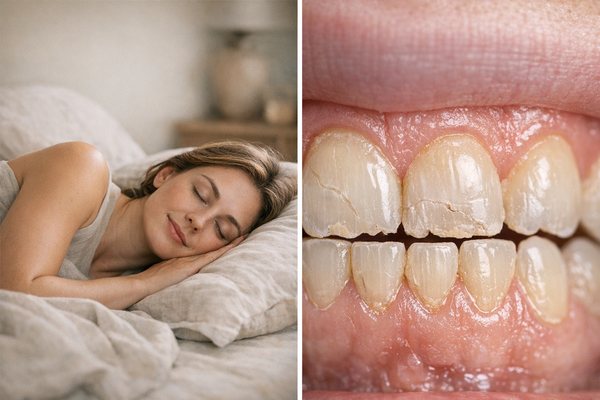
How Sleep Positions Affect Teeth Clenching and Bruxism: A Guide to Avoid Jaw Pain
Discover how sleep positions impact bruxism and jaw pain, with tips for optimal posture.
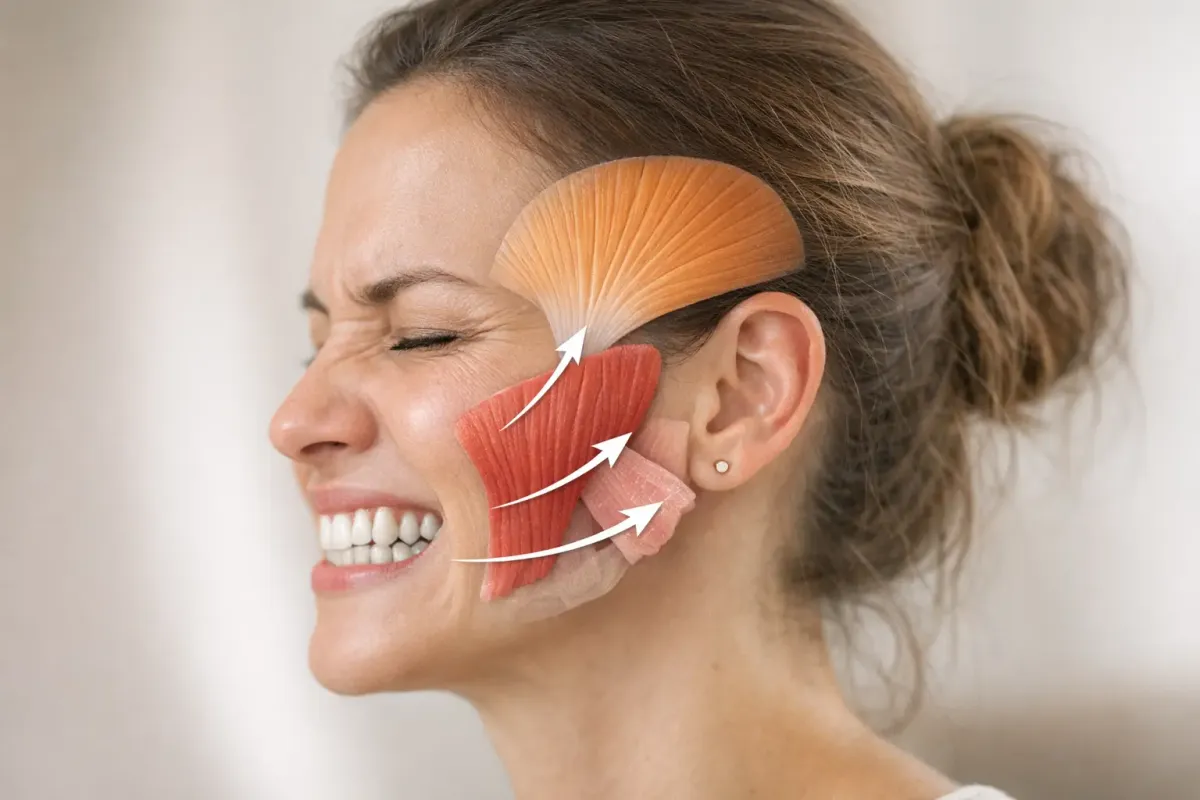
If you wake up with a sore jaw or your partner says you sound like a trash compactor at night, your sleep position and teeth might be in an unhealthy relationship. Researchers have explored this connection using electromyography, motion sensors, and pillow experiments. What they've found is fascinating and useful: how you sleep can increase or decrease the muscle activity that causes bruxism, the clinical term for teeth grinding and clenching.
This guide breaks down the latest research into practical advice. Discover what studies reveal about bruxism, why some mornings hurt more, and how simple posture adjustments might protect your enamel and sanity. Grab a pillow and let's dive in.
Understanding Bruxism: What It Is and Why It Matters
Symptoms and Causes
Bruxism involves involuntary grinding or clenching of teeth, mostly during sleep. The Mayo Clinic notes the classic signs as worn tooth surfaces, temple-centered headaches, and jaw muscles that feel overworked. Experts define bruxism into two types: awake and sleep bruxism. We focus on the latter here.
How common is it? The prevalence is around 8–15% of adults, though studies with jaw-mounted sensors suggest up to one-third of people experience occasional grinding monthly. Kids can reach as high as 40%, usually decreasing after permanent teeth come in. These numbers matter because early intervention can prevent costly dental repairs later.
Why does it happen? Stress and anxiety are major contributors, but other triggers are emerging. A study by Zeb et al. 2024 used electrodes to show that postural changes can increase masseter activity quickly. Other factors include misaligned bites, alcohol, caffeine, and some medications. Bruxism also associates with sleep disorders like obstructive sleep apnea (OSA) and restless legs syndrome. To explore how stress contributes to bruxism, you might find our article on stress and bruxism insightful.
Impact on Health
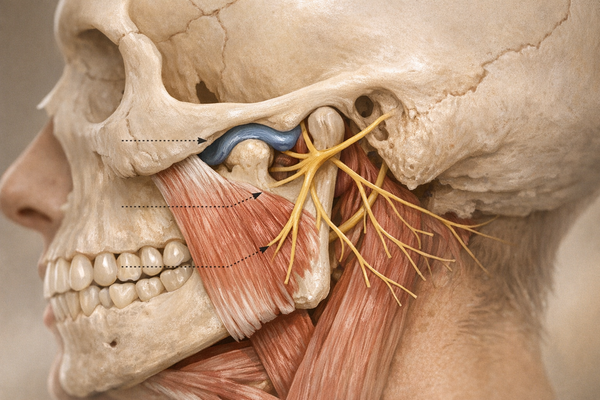
Grinding teeth is more than a nighttime annoyance. It can chip or fracture teeth, worsen gum recession, and inflame periodontal tissue over time. The temporomandibular joint (TMJ) often takes the strain, causing jaw clicks and aches many feel in the morning. A study by El-Gendy et al. 2022 found reduced mouth-opening in chronic grinders, indicating that ongoing micro-trauma stiffens jaw muscles. The effects can spread further: chronic pain can lead to daytime fatigue and even increase blood pressure. Bruxism is a whole-body issue, not just a dental quirk.
Consider Jessica, a 34-year-old graphic designer. She thought her cracked molar was from crunching ice. Her dentist's X-rays showed flattened cusps across several teeth, indicating years of nocturnal grinding. After using a custom night guard and training to sleep on her back, her jaw soreness and headaches diminished in under a month. For more on the types of mouth guards that might help, explore our guide on choosing the right bruxism mouth guard.
The Science of Sleep Positions and Their Impact on Jaw Health
Common Sleep Positions
Most people sleep in one of three positions: back (supine), side (lateral), or stomach (prone). Studies from the National Sleep Foundation show 60% of people prefer side sleeping, 30% back sleeping, and fewer stomach sleeping. Each position affects how gravity interacts with your jaw and neck muscles.
These preferences can change with age. Seniors often sleep on their sides due to spinal arthritis, while infants frequently end up on their stomachs unless repositioned. Habits evolve, so a posture change that doesn't work now might be effective later.
How Each Position Affects the Jaw
1. Back sleeping keeps the head neutral, allowing the jaw to relax midline, which can reduce clenching. However, those with untreated OSA might clench to keep airways open.
2. Side sleeping creates asymmetry. Lying on your right side can pull the mandible toward the pillow, slightly rotating the jaw. Zeb's study found that muscle activation can increase by 10% on the side you lie on. Alternating sides balances the strain, but favoring one side can stress that TMJ.
3. Stomach sleeping is problematic. It twists the neck and compresses the jaw against the mattress. Karabicak et al. 2025 found the highest muscle activity in prone sleepers before treatment. If you're experiencing jaw pain after sleeping, consider reading about how sleep positions impact bruxism.
In summary, posture affects muscle loading. Even small shifts can influence bruxism. While fancy pillows are helpful, avoiding stomach sleeping might be more effective.

Jaw Pain After Sleeping: What's the Connection?
Analyzing Jaw Pain Triggers
Morning jaw pain results from biomechanics and neurochemistry. Grinding causes micro-trauma and lactic acid buildup in the jaw muscles. Zeb's study found that muscle activity spikes during REM sleep, when dream content and sympathetic output increase, adding tension.
The direction of force also matters. Lateral forces during side and stomach sleeping can strain one TMJ more than the other, causing unilateral soreness. If the pain is on the pillow-side joint, posture may be to blame. For more insights into one-sided jaw pain, our article on stress and one-sided jaw pain might be useful.
Dehydration is another possible cause. Dehydrated muscles cramp more easily, and mouth-breathing can dry tissues further. Drinking water before bed and using a saline nasal rinse can help reduce pain.
Role of Sleep Disorders
Sleep apnea is significant. Those with OSA often push the jaw forward to breathe. A study by Attia et al. 2024 found higher TMJ loading in untreated apnea cases. After CPAP or mandibular advancement therapy, jaw pain scores dropped, suggesting that some bruxism is an airway defense. For a broader understanding of how sleep disorders affect bruxism, see our article on sleep disorders and bruxism.
Using a position-responding mandibular advancement device (PR-MAD) in mild OSA patients reduced apnea events and morning soreness, as reported by On et al. 2024. This offers dual benefits: airway support and muscle relaxation.
Not all jaw pain is due to bruxism. If discomfort is paired with clicking or locking, there might be a primary TMJ disorder. Still, sleep posture is a factor you can improve.
Optimizing Sleep Positions for Bruxism Relief
Best Positions for Reducing Jaw Pain
1. Supine with a thin pillow: Lying on your back keeps the mandible centered. Use a low-profile pillow to avoid chin-tucking, which can cause clenching in apnea-prone sleepers.
2. Modified side-lying: If side sleeping is preferable, place a bolster under the top arm and a contoured pillow under the head. This reduces the downward pull on the jaw. Some suggest a small pad between teeth to relax the masseter, but check with your dentist first.
3. Avoid stomach sleeping: Stomach sleeping misaligns the jaw. If you can't stop immediately, use a body pillow to roll only halfway forward, gradually moving to lateral or supine positions.
Pro tip: Keep a mirror on the nightstand. Before bed, check your resting jaw position; the tongue should be near the roof of the mouth, teeth slightly apart. This visual check builds muscle memory.
Sleep Aids and Devices
Mandibular advancement devices: PR-MADs, as mentioned in the On et al. 2024 study, move the jaw forward, treating apnea and often reducing bruxism.
Occlusal splints: Custom night guards cushion biting surfaces and distribute force. Karabicak et al. 2025 found splints reduced morning pain similarly to jaw exercises. Combining splints with posture improvements enhances results. For more on effective jaw pain relief, see our article on jaw pain relief.
Pillow technology: Memory-foam pillows with side cutouts reduce pressure for side sleepers. Cervical rolls keep the neck aligned during back sleeping. The Sleep Foundation guide highlights wedge pillows that prevent stomach rolling.
Biofeedback buzzers: Wearable sensors detect clenching and vibrate gently, encouraging relaxation without waking the sleeper. They are costly, but users report fewer dental issues. For more on biofeedback devices, explore our article on biofeedback for bruxism.

Complementary Therapies for Bruxism and Jaw Pain
Exercise and Relaxation Techniques
Yoga programs combine stretching and slow breathing, proven stress reducers. A trial by Ozmen & Unuvar 2024 on face yoga and dry needling noted a 30% pain reduction and improved sleep quality. Another study by Atilgan et al. 2024 reported better mouth-opening and lower stress in women with TMJ pain.
No need for headstands: a 10-minute routine of neck rolls, jaw movements without contact, and deep breathing can reduce bruxism intensity.
Apps like Calm or Headspace offer “jaw release” tracks. Users follow cues to melt tension from the temples to the shoulders, all for less than a latte. For more relaxation techniques, see our article on jaw relaxation techniques.
Manual Therapy
The RCT by El-Gendy et al. 2022 combined myofascial release with education, showing decreased masseter tenderness and better sleep. Massage boosts blood flow, removing metabolic waste that causes stiffness. For more on the role of physical therapy, explore physical therapy in TMJ management.
If professional therapy is unaffordable, try self-massage. Press fingertips over the masseter, open your mouth halfway, and make slow circles for a minute each side. Pair this with temple rubs and scalp mobilizations for a low-cost pain relief option.
When to Seek Professional Help
Identifying Severe Symptoms
Some signs suggest it's time to consult a professional:
- Cracked teeth or failed dental restorations without obvious cause
- Locking or dislocating jaw during yawning or chewing
- Persistent headaches unresponsive to medication
- Tinnitus or earache without infection
- Partner reports loud grinding despite posture changes
Insurance tip: Most dental plans cover occlusal guards under code D9944 or D9945 every five years. Knowing this can prevent billing issues.
Consultation and Treatment Options
Your first step is often a dentist trained in sleep medicine. They can provide a bruxism monitor or refer you for a sleep study if apnea is suspected. In Karabicak et al. 2025, combining posture therapy with dental oversight led to faster improvements than self-help alone.
For rehabilitation-focused care, a physical therapist experienced with craniofacial disorders can guide jaw and neck alignment exercises. Psychologists may address anxiety. Multimodal care outperformed single treatments in the yoga trial mentioned earlier.
Expect results in 6–12 weeks as you retrain sleep posture and reduce muscle hyperactivity. Set reminders and track pain scores to stay motivated.
Conclusion: Taking Control of Your Sleep and Jaw Health
Your jaw spends about a third of its life in your sleep position. Evidence shows that posture affects muscle firing patterns, determining if you wake refreshed or sore. Back sleeping with proper neck support is ideal, but any position keeping the mandible neutral and airway open is beneficial. Pillows, splints, stretches, and manual therapy offer additional protection.
Start with easy changes: avoid stomach sleeping, upgrade your pillow, and do jaw stretches before bed. If pain persists, seek professional help. A quieter night and better morning could be just a turn away.