The Role of Physical Therapy in TMJ Pain Management and Bruxism Relief
Explore how physical therapy aids TMJ pain and bruxism relief.

Picture this: You wake up with a sore jaw, a dull headache, and a vague memory of grinding your teeth through the night. You start your day with a Google search for “bruxism,” and suddenly, you’re reading about fractured molars and expensive night guards. But don’t worry. Physical therapy might just be the solution to help your jaw relax and improve your sleep quality. Let's explore what the research says, why it matters to you, and how to incorporate it into your life without turning your bathroom into a dental lab.
The following claims are grounded in peer-reviewed studies and reputable medical organizations. Opinions are clearly labeled. Let’s get into it.
Understanding Bruxism and TMJ Disorders
Let’s get on the same page with some definitions.
What is bruxism?
Bruxism refers to clenching or grinding your teeth. It can happen while you’re awake (awake bruxism) or asleep (sleep bruxism). Often, you might not realize it until someone else points it out or your dentist notices wear on your teeth.
Common signs include morning jaw fatigue, scalloped tongue edges, and unexplained shoulder tension. Some people also experience ear fullness or tinnitus, since the jaw shares nerve pathways with the ear. You can learn more about this connection in our article on ear pain linked to TMJ and bruxism.
What are TMJ disorders?
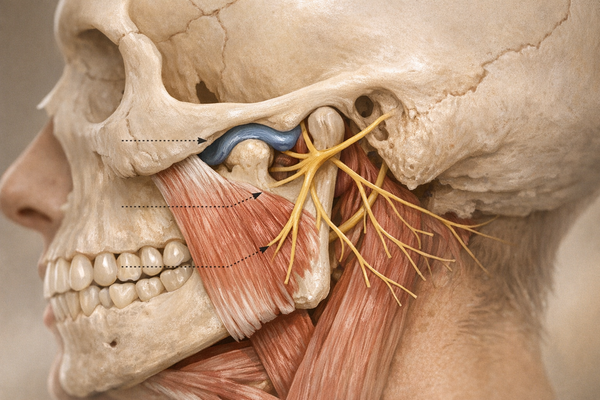
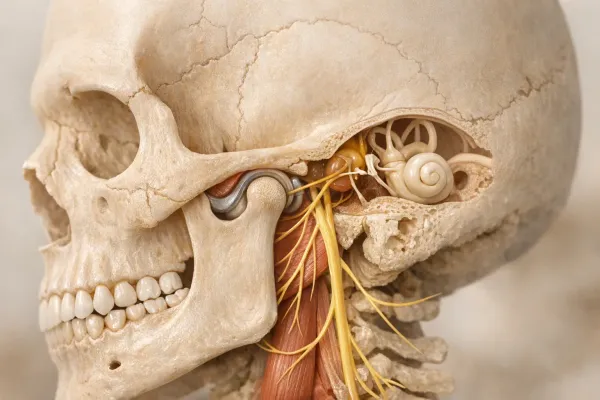
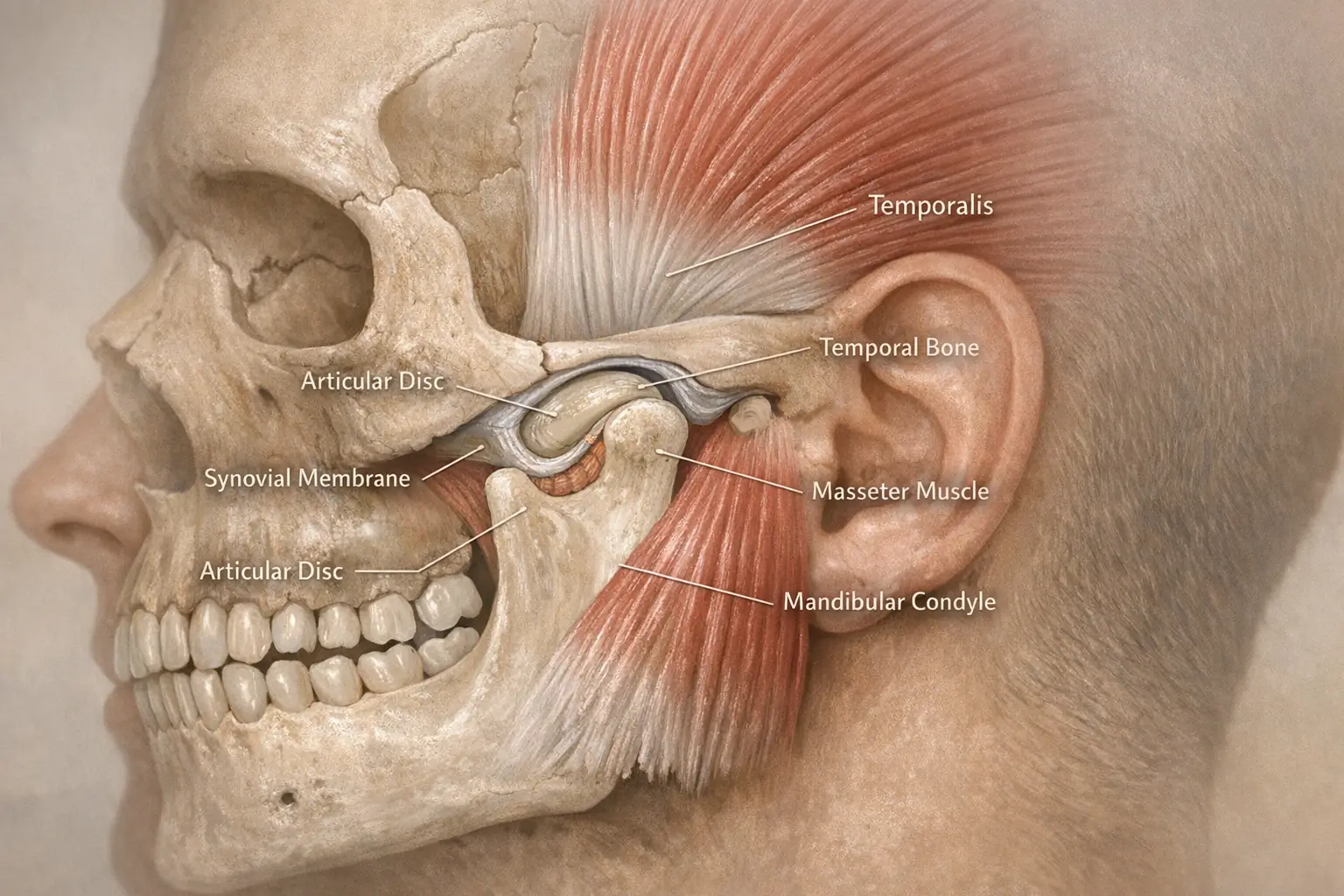
The temporomandibular joints (TMJs) are located just in front of your ears and function like small hinges for your jaw. A TMJ disorder, often called TMD, occurs when these joints or nearby muscles aren’t working smoothly. Symptoms can include clicking sounds, limited mouth opening, and pain.
How common are these issues?
Sleep bruxism affects about 6–9% of adults, but can rise to 50% in high-stress groups, according to a 2024 review by Leung et al. TMJ disorders are similarly widespread. A 2023 review by Matheson et al. estimates up to 12% of the population will experience significant TMD at some point.
The chicken-and-egg problem
Bruxism can strain jaw muscles, irritating the TMJ. Conversely, a painful TMJ can trigger clenching as a reflex. These conditions often exacerbate each other, which is why they’re grouped under “orofacial pain” management. For more insights, explore the triggers of TMJ pain and how to manage it.
Why you should care
- Untreated bruxism can lead to cracked fillings or teeth.
- Chronic TMJ pain can interfere with eating, talking, and sleeping.
- Both are linked to poor sleep quality and increased stress. Read more about how stress and anxiety trigger teeth clenching.
Common risk factors include high caffeine intake, alcohol before bed, untreated sleep apnea, and poor posture (thanks, laptops). Knowing these triggers can help tackle the problem from different angles.
Bottom line: Addressing muscle and joint health is crucial. Enter physical therapy.
Physical Therapy for Bruxism: An Overview
Physical therapists are movement specialists whose expertise goes beyond sore shoulders and knees. For bruxism, they focus on muscles you might not realize you’re overworking during sleep. Discover more about how physical therapy for bruxism can benefit you.
Typical treatment involves one to two sessions per week for four to six weeks. A 45-minute session might start with hot-pack relaxation, move to 10–15 minutes of hands-on work, and end with exercises and education. Many clinics offer hybrid models—an initial in-person visit followed by online sessions so you can practice exercises at home.
Manual therapy: Hands-on muscle reset
Manual therapy includes soft-tissue massage, trigger-point release, and joint mobilization. In a 2024 study by Kadıoğlu et al., patients received manual therapy plus home exercise. Results showed significant drops in pain and stress levels, and better sleep scores after just four weeks.
Quality of life improved, with participants reporting better function in work and social life—something oral appliances alone rarely achieve.
Exercise therapy: Teaching the jaw to behave
Exercises aim to improve coordination between jaw, neck, and shoulder muscles. A 2023 study by Yazici et al. showed that a single session of physical therapy can relax overactive jaw muscles, indicating both immediate and long-term value.
Your PT may also teach diaphragmatic breathing; better oxygenation reduces the “fight-or-flight” response that drives clenching. A five-second inhale and exhale pattern can serve as stress training.
Adjunct treatments inside the PT clinic
- Therapeutic ultrasound to improve blood flow
- Dry needling of trigger points (if allowed by state laws)
- Biofeedback to teach relaxation of jaw muscles. For more information on biofeedback, read our biofeedback therapy guide.
What the comparisons show
A study by Şahin et al. in 2024 compared manual therapy with Botox, dry needling, and medication. Manual therapy showed similar pain reduction without drug side effects or discomfort from injections.
Physical therapy isn’t one-size-fits-all, but evidence suggests it’s safe and effective as a frontline option. The American Physical Therapy Association supports this on its site, ChoosePT.com.
TMJ Exercises for Pain Relief
You can’t bench-press your jaw, but you can train it. Below are exercises that target mobility, strength, and relaxation. Consult a professional before trying these at home. Discover more about effective TMJ exercises for jaw pain relief.
Tip: Track symptoms in a notes app. If pain increases after exercise, reduce reps by 20%. If there’s no change after a week, increase hold times by two seconds. Safe self-experimentation often speeds up results.
1. Controlled opening and closing
How to do it:
- Place your tongue on the roof of your mouth.
- Slowly open your jaw until your tongue wants to move.
- Close slowly. Repeat 10 times.
Why it works: It keeps the joint’s hinge motion straight, reducing side glides that irritate tissues. A 2023 review by Shimada et al. found this improved mouth-opening range by 5 mm in four weeks.
2. Isometric jaw holds
How to do it:
- Place your thumb under your chin.
- Try to open your mouth while resisting with your thumb. Hold for 5 seconds.
- Repeat on each side by pushing the jaw sideways against gentle finger pressure.
Why it works: Gentle muscle activation recruits stabilizers often inactive due to modern lifestyles.
3. Cervical spine alignment drills
How to do it:
- Sit tall and draw your chin straight back (think “make a double chin”).
- Hold for 5 seconds and release. Repeat 10 times.
Why it works: Forward-head posture stresses the TMJ by forcing the jaw to protrude. Correcting your neck reduces that strain. Sarfraz et al. 2023 found adding neck posture drills accelerated pain relief. Learn more about how posture affects jaw pain.
4. Masseter stretch with hot pack
How to do it:
- Apply a warm compress on the cheeks for 5 minutes.
- Gently open the mouth while sliding the jaw downward and slightly forward.
Why it works: Heat relaxes muscles, making the stretch more effective. The Cleveland Clinic lists heat plus gentle stretching as first-line self-care for TMJ disorders.
Evidence snapshot
- Pain reduction: Shimada’s review documented a 30% pain score drop after 4–8 week exercise programs.
- Mobility gains: Average mouth opening improved by 5–8 mm, enough to bite into a sandwich without grimacing.
- Duration matters: Daily practice of at least 10 minutes was optimal for benefits.
It’s tempting to skip exercises once pain eases, but consistency is key. Think of it as brushing your joints.

Comparing Physical Therapy with Other Treatments
1. Medications
Over-the-counter NSAIDs, muscle relaxants, or short-term benzodiazepines may relieve pain or spasm. Downsides include stomach issues, drowsiness, and tolerance. Drugs rarely address root muscle coordination problems, so symptoms often return when you stop. Explore popular TMJ pain relief methods for more options.
2. Botox injections
Botulinum toxin temporarily paralyzes jaw muscles. According to Şahin et al. 2024, Botox reduced pain by about 60% at four weeks, but effects faded by month three. Repeat injections can be costly and cause chewing weakness. Discover more about advanced TMJ treatments like Botox.
3. Stabilization splints or night guards
These appliances distribute bite forces and protect enamel. They work well for many, but the Mayo Clinic notes they don’t ease all symptoms, especially daytime jaw tension. Learn about choosing the right TMJ mouth guard.
4. Physical therapy
Combining manual techniques, exercises, and education, a 2024 study by Salloum et al. found PT provided similar pain relief to splints plus ultrasound at four weeks. PT patients maintained improvements at 12 weeks, suggesting longer-lasting effects.
Scorecard
- Effectiveness: PT, Botox, and splints all reduce pain, but PT scores better on function and durability.
- Side effects: PT has minimal risks if done correctly. Meds and Botox carry potential adverse events.
- Cost: PT may require multiple visits, but splints, drug refills, or repeat injections add up too. Many insurance plans cover PT, and some states allow direct access without a physician referral, saving an extra copay.
A combination approach might be best. Start with PT, add a night guard for enamel protection, and reserve meds or injections for stubborn flare-ups.
Case Studies: Success Stories with Physical Therapy
Case 1: The stressed-out coder
“Alex,” 29, had waking headaches and jaw clicking that worsened before project deadlines. Baseline pain was 7/10. Following the protocol from Kadıoğlu et al., therapists used myofascial release and taught a five-exercise home routine. After six sessions over four weeks, Alex’s pain dropped to 2/10, sleep quality improved by 25%, and jaw clicking reduced. He now takes stretch breaks during coding.
Case 2: The night-shift nurse
“Bri,” 42, experienced severe sleep bruxism, confirmed by a partner and a cracked molar. A night guard didn’t help her exhaustion. A single session of manual therapy, mirroring Yazici et al., produced immediate muscle relaxation. Over eight weeks, Bri added posture drills and relaxation. Pain scores dropped from 8/10 to 1/10, and she reduced caffeine, which she and her dentist linked to clenching spikes. Read about how avoiding caffeine late at night can help with bruxism.
Case 3: The teenage violinist
Though our focus is adults, kids grind too. A study on laser acupuncture in children (Farouk et al. 2025) showed PT outperformed sham laser on muscle tenderness. This teen combined TMJ exercises with posture coaching. Result: fewer headaches and improved note accuracy, according to a proud dad’s update.
These results were maintained through telehealth, showing that distance isn’t always a barrier to jaw rehab.
What these cases teach
- Early intervention can prevent dental damage and joint issues.
- Combining manual therapy with home exercise yields lasting benefits.
- Lifestyle changes, like managing stress and improving posture, enhance results.
Anecdotal evidence isn’t the same as randomized trials, but these stories reflect real-world outcomes seen in controlled research.
Conclusion: The Future of Physical Therapy in Bruxism and TMJ Management
Clenching and jaw pain aren’t issues to “just live with.” Physical therapy offers a research-backed method to calm muscles, retrain the jaw, and improve chewing, talking, and sleeping without discomfort. Studies from 2023 and 2024 suggest PT is as effective as, or better than, splints, drugs, and injections for long-term relief, with fewer side effects.
Future research will likely refine the approach—session frequency, exercise selection, and order. Telerehab is gaining popularity, and wearable electromyography patches that alert you to clenching are in development. For now, if your jaw is troubling you, consider consulting a PT. Your teeth, sleep, and peace of mind will thank you.