Advanced TMJ Treatments: Exploring Botox and Beyond
Discover cutting-edge TMJ treatments, from Botox to dry needling, and how they compare to traditional methods.
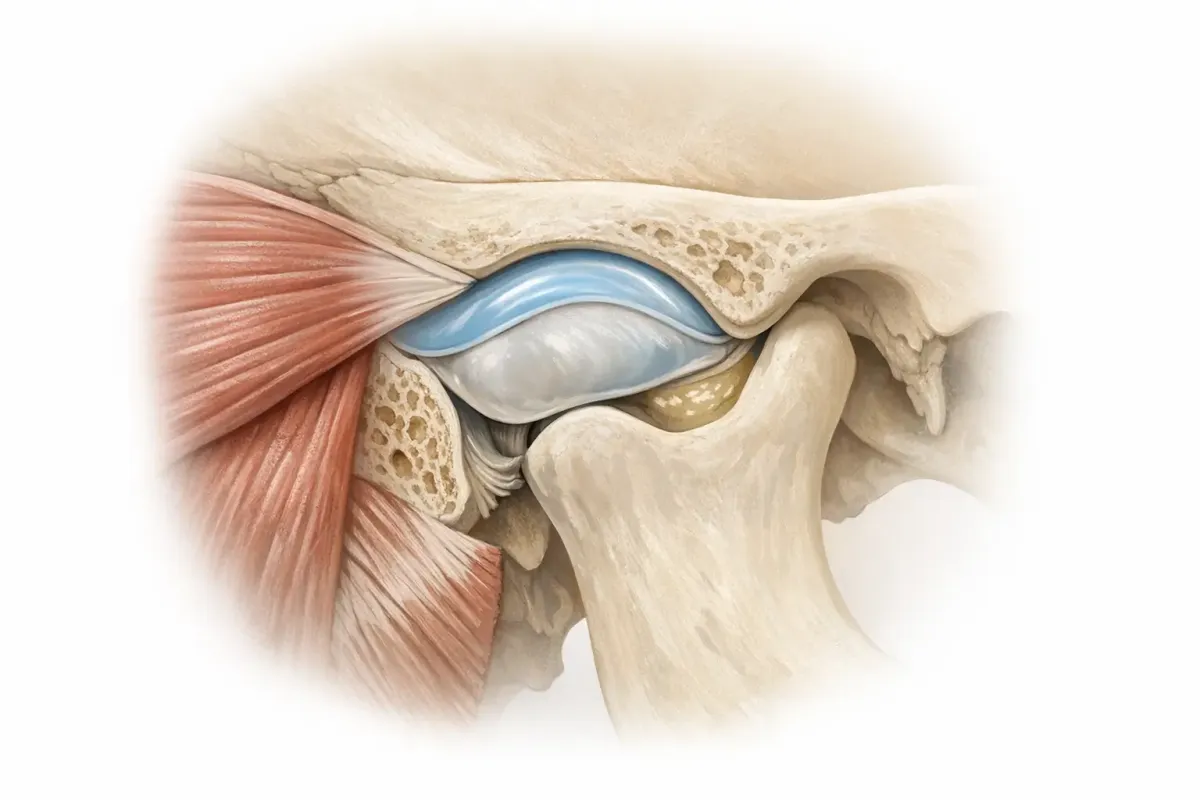
You chew, yawn, and shout without thinking about the temporomandibular joint (TMJ) just in front of your ears. But when it starts to hurt, you notice every click and spasm. If you’re here, you might have tried soft foods and mouth guards but still wake up with a clenched jaw. The good news is that researchers are exploring advanced TMJ treatments like Botox and dry needling, which offer more than just another ibuprofen bottle.
This article takes you on a tour of advanced TMJ treatments, starting with the buzz around Botox and moving through dry needling, stem cells, and hormones. Each claim is linked to peer-reviewed research or reputable medical sources, so you can verify the facts before considering any treatment.
Understanding TMJ Disorders
Common Symptoms
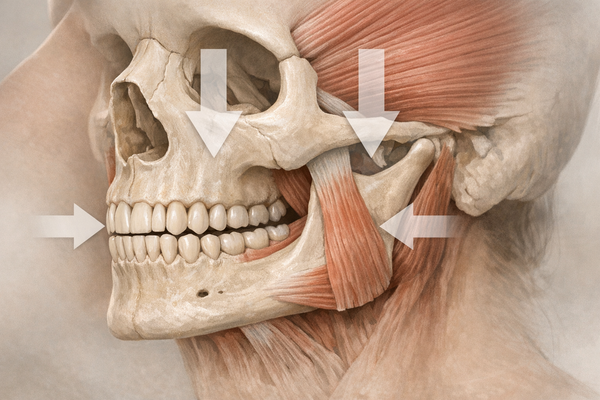
The TMJ acts like a sliding hinge where your jawbone meets the skull. When it malfunctions, you may notice:
- Popping or clicking while opening your mouth
- Jaw muscle pain, often worse in the morning
- Difficulty chewing or talking for long periods
- Headaches radiating from the temples
- Occasional ear pain or ringing
A review by Nieves Del Rio et al. (2025) shows that TMJ pain is rarely caused by one factor. Grinding your teeth, injuries, arthritis, and stress all play a part. Studies like Sfeir et al. (2025) reveal that up to 31% of adults report TMJ-related discomfort.
Diagnosing TMJ disorders involves a multifaceted approach. Practitioners may press on jaw muscles, listen for joint noises, and use X-rays or CT scans to rule out fractures or cysts. MRI is the gold standard for visualizing soft tissue but is usually reserved for surgical planning due to cost. If pain radiates to the ear, an otolaryngologist may be consulted to rule out infection, highlighting the collaborative nature of TMJ care.
Psychological factors can amplify symptoms. Studies show that anxiety, sleep apnea, and chronic pain can worsen jaw complaints. Clinicians often screen for triggers like high caffeine intake, poor posture, and stress to create a comprehensive treatment plan.
Traditional Treatments
Initial care for TMJ disorders is conservative. Rest, moist heat, anti-inflammatory medications, and a soft diet are recommended first. If pain persists, a dentist might recommend a night guard. Physical therapy can teach posture corrections and gentle stretches. Some clinics offer muscle relaxants or low-level laser therapy. According to the Mayo Clinic, these methods help many, but some patients need stronger relief.
Small daily changes can enhance conservative care. Opt for softer foods like shredded meats, steamed veggies, and smoothies. Set reminders to unclench your jaw by placing the tip of your tongue on the roof of your mouth, with teeth slightly apart, and breathe through your nose. Proper workspace ergonomics, like having a monitor at eye level, can prevent neck strain linked to TMJ pain. These adjustments can sometimes reduce pain scores significantly.
Botox for TMJ: A Modern Solution
Mechanism of Action
Botulinum toxin type A, commonly known as Botox, blocks acetylcholine, which causes muscles to contract. When injected into the masseter or temporalis muscles, it relaxes overactive fibers, reducing clenching and joint pressure. Effects typically appear within a week and last three to four months as nerve endings regrow.
Clinical Efficacy
A cohort study by Henien Marianne et al. (2025) followed 118 adults with TMJ pain who received two Botox treatments 12 weeks apart. Pain scores decreased from 7.1 to 2.9 on a ten-point scale. Jaw opening improved by 6 millimeters, allowing for easier eating.
Side effects were mild, with 8% reporting temporary chewing fatigue and 2% experiencing slight smile asymmetry, which resolved in six weeks. A review by Alexander et al. (2025) suggests Botox is comparable to steroid injections for short-term relief, though costs can add up with repeated sessions.
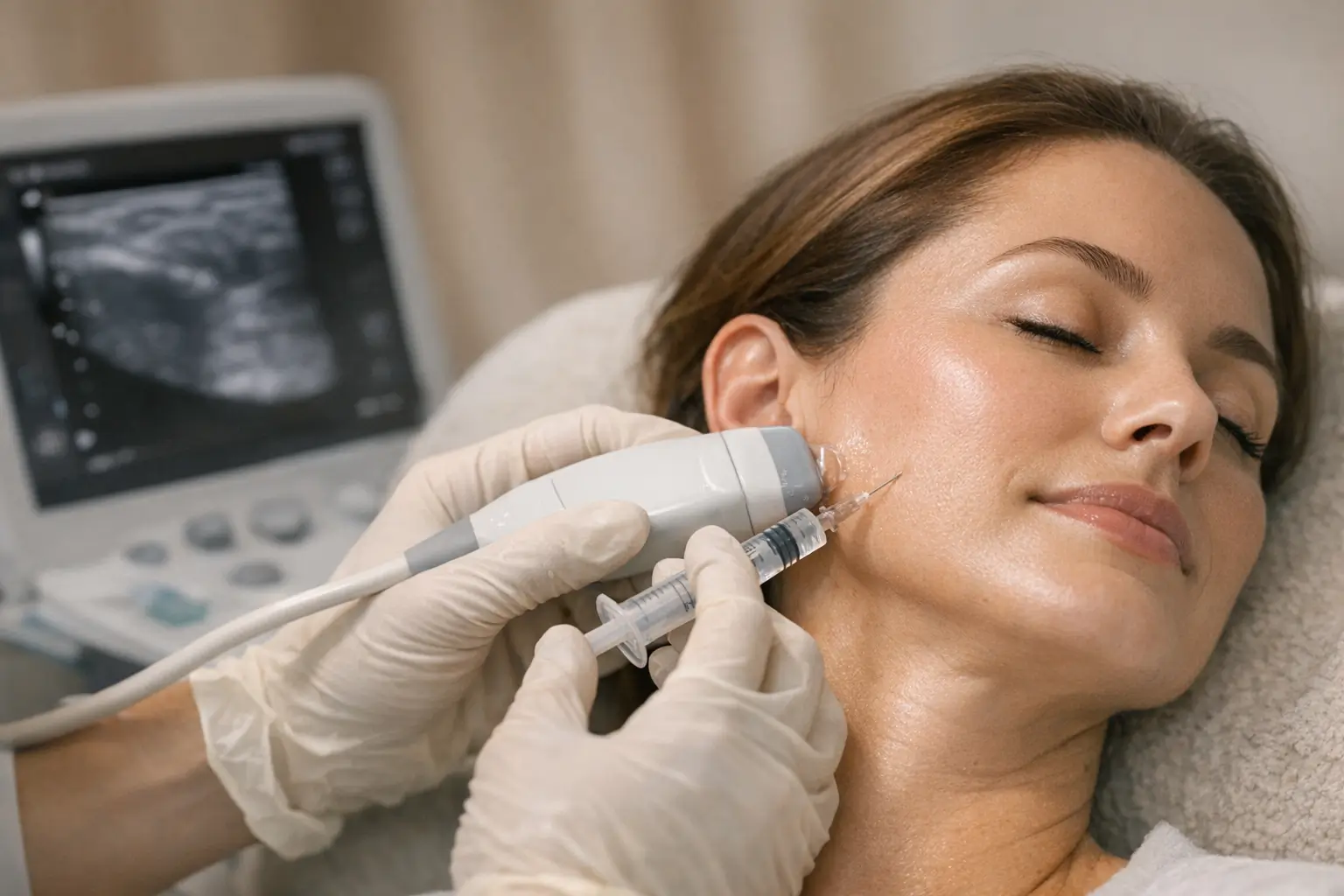
On treatment day, the clinician maps injection sites by asking you to clench, highlighting bulky areas. Ultrasound guidance is becoming popular to avoid blood vessels and minimize bruising. Post-treatment care is simple: avoid rubbing the area or lying flat for four hours. You can usually drive yourself home and return to work. A small study suggests foods rich in magnesium, like spinach and almonds, may modestly extend the effects.
Is it worth trying? If other treatments have failed, Botox offers a reversible, outpatient option. Expect to pay $400–$900 per session in the U.S., as insurance coverage varies.
Dry Needling: An Emerging Therapy
Procedure Overview
Dry needling is different from acupuncture, though both use thin needles. A physical therapist or dentist inserts sterile needles into myofascial trigger points around the jaw, neck, and shoulders. The mechanical disruption and local twitch response help reset muscle tone.
A pilot study by Weng (2025) involved 40 patients receiving six weekly sessions. Jaw opening increased by 8 millimeters, and pain scores dropped 45%. Sessions last about 20 minutes with minimal soreness.
Patient Experiences
Patients often describe a brief zing as the needle hits a trigger, followed by a dull ache that eases quickly. Compared to Botox, dry needling is cheaper—$60–$120 per visit—and avoids drug exposure. However, effects may be shorter-lived. In Weng’s study, one-third requested booster sessions after three months.
Combining needling with home stretches can extend relief. Contraindications include bleeding disorders or needle phobia. The American Academy of Orofacial Pain recommends checking practitioner credentials.
Pairing dry needling with manual therapy enhances outcomes, according to a 2024 meta-analysis in the Journal of Manipulative and Physiological Therapeutics. Therapists who follow needling with joint mobilizations and stretches report twice the improvement at eight weeks compared to needling alone. At home, a warm shower before self-massage helps integrate the treatment into the body’s healing process.
Biological Interventions: Stem Cells and More
Stem Cell Therapy
Stem cells, often used for spinal and knee issues, are now being explored for TMJ. Researchers harvest mesenchymal stem cells from bone marrow or fat and inject them into the joint. These cells can differentiate into cartilage-like tissue and reduce inflammation.
Weng (2025) reviewed 24 TMJ patients who received autologous stem cell injections. MRI scans at 12 months showed partial disc regeneration in 58% of cases. Pain scores dropped 60%, and mouth opening improved by 9.5 millimeters. No immune reactions occurred since the cells came from the patient.
The process involves light sedation and bone marrow extraction, followed by centrifugation. Fat-derived cells are easier to collect but may yield fewer cartilage-creating cells. After injection, patients often wear a splint for 48 hours. The post-op diet resembles that of wisdom tooth recovery.
Costs exceed $3,000, and the procedure remains off-label in many areas. Long-term safety is still under study, though initial results are promising.
Hyaluronic Acid and PRP
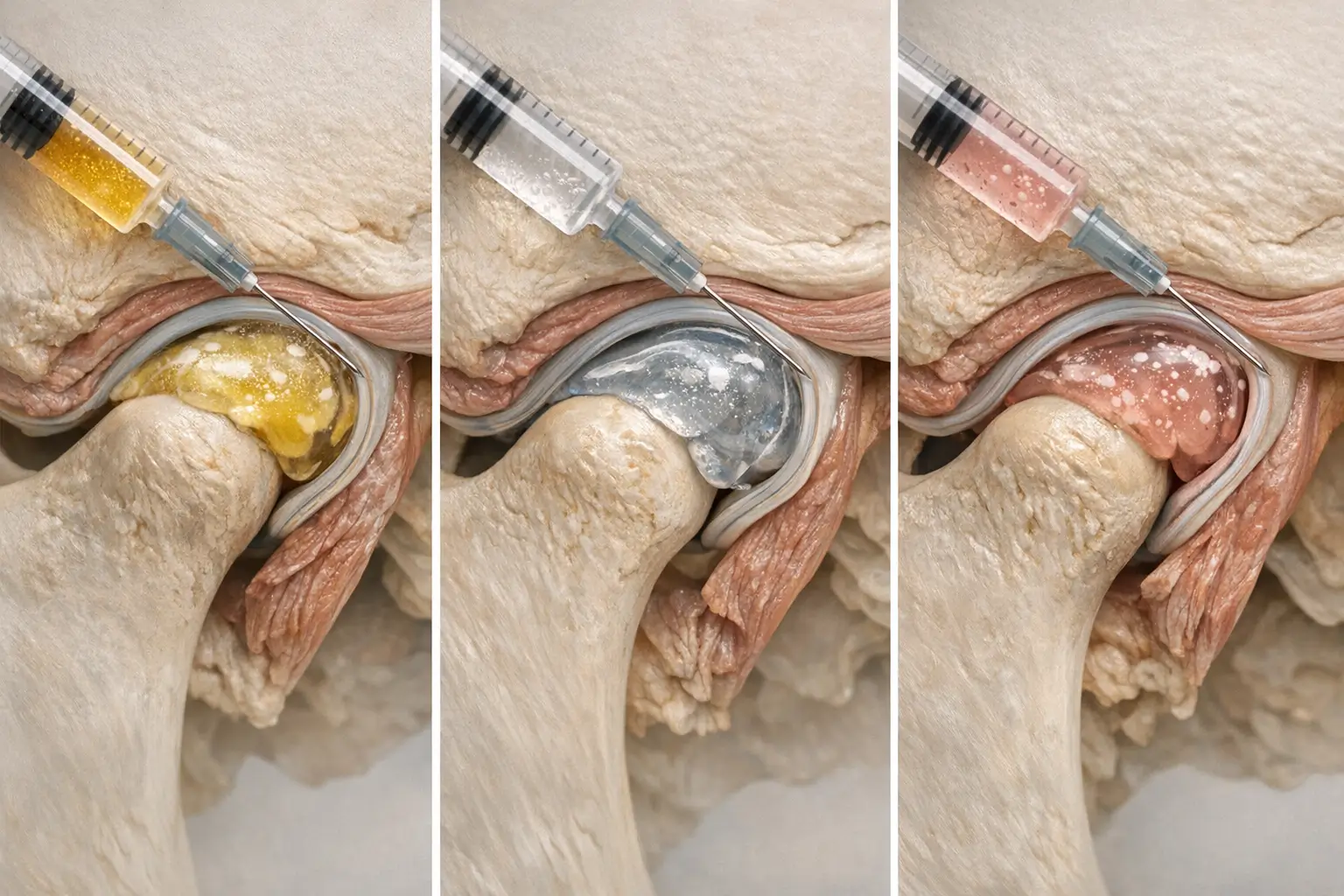
Hyaluronic acid (HA) acts as joint lubricant, while platelet-rich plasma (PRP) is derived from your blood to concentrate growth factors. Both are injected into the TMJ with imaging guidance.
In a study by Chivu et al. (2025), 60 participants received either HA or PRP. At six months, HA users reported 40% pain reduction, while the PRP group saw a 55% reduction. No major adverse events occurred, and both treatments were well-tolerated.
The Role of Hormones in TMJ Treatment
Sex Differences
Women report TMJ disorders nearly twice as often as men, especially during reproductive years. A study by Tomura et al. (2025) reveals that 17β-estradiol increases inflammation in joint cartilage, while dihydrotestosterone (DHT) seems protective.
This hormonal influence may explain symptom spikes during menstrual phases or menopause. Hormone modulation might help, though human evidence is limited.
Hormonal Therapies
Future treatments may involve localized hormone blockers or enhancers for the TMJ. Early research is looking into selective estrogen receptor modulators to calm cartilage cells. Currently, some clinicians work with endocrinologists to adjust systemic hormone therapy for TMJ patients.
Altering hormones is not a simple fix. Side effects can include mood swings and metabolic changes. Until more research is available, these therapies remain experimental.
Keeping a pain diary that tracks intensity, sleep quality, and menstrual days can reveal patterns and guide treatment timing. Pregnant patients should be cautious, as rising relaxin levels can loosen jaw ligaments, but most injectables are paused for fetal safety. In such cases, conservative measures are prioritized.
Comparing Cutting-edge and Traditional Approaches
Effectiveness and Accessibility
How do these advanced options compare to traditional treatments? A trial by Yue et al. (2025) shows that structural factors greatly impact outcomes, meaning even advanced injections may not help if the disc is displaced. Dommeti et al. (2025) argue that reducing bite force, via splints or Botox, lowers joint stress more effectively than rest alone.
Cost and access are important. Physical therapy and splints are usually covered by insurance and require no specialized labs. Botox is widely available but requires repeat visits. Stem cells are costly and often not covered by insurance.
Patient Preferences
Surveys by the American Association of Oral and Maxillofacial Surgeons show that patients prioritize pain relief, convenience, and cost. Many start with conservative treatments and escalate if needed. Those who tried Botox reported the highest satisfaction, likely due to quick relief and low downtime. Dry needling was praised for affordability but criticized for short-lived effects.
The pandemic has increased the use of telehealth for TMJ care. Virtual appointments allow therapists to observe and adjust treatments like exercises or discuss candidacy for injections. Kaiser Permanente’s 2024 data showed that video follow-ups reduced travel costs by 60% and caught flare-ups sooner. Even advanced treatments like stem cells benefit from remote monitoring.
Conclusion
TMJ disorders are challenging, but you now have more options than just hot packs and soft foods. Botox provides quick muscle relaxation with few side effects. Dry needling offers a drug-free reset for muscles. Biological injections aim for healing, though evidence and coverage are catching up. Hormonal research adds a new dimension, especially for women noticing monthly pain changes.
No single therapy suits everyone. Start with a thorough diagnosis to rule out structural damage, and consider your budget, risk tolerance, and lifestyle. Partnering with a knowledgeable dentist, physical therapist, or oral surgeon increases your chances of finding relief. A combination of traditional and advanced treatments often delivers the best results.