Exploring New TMJ Treatments: Innovative Therapies for Pain Relief
Discover cutting-edge TMJ therapies for effective pain relief and improved jaw health.
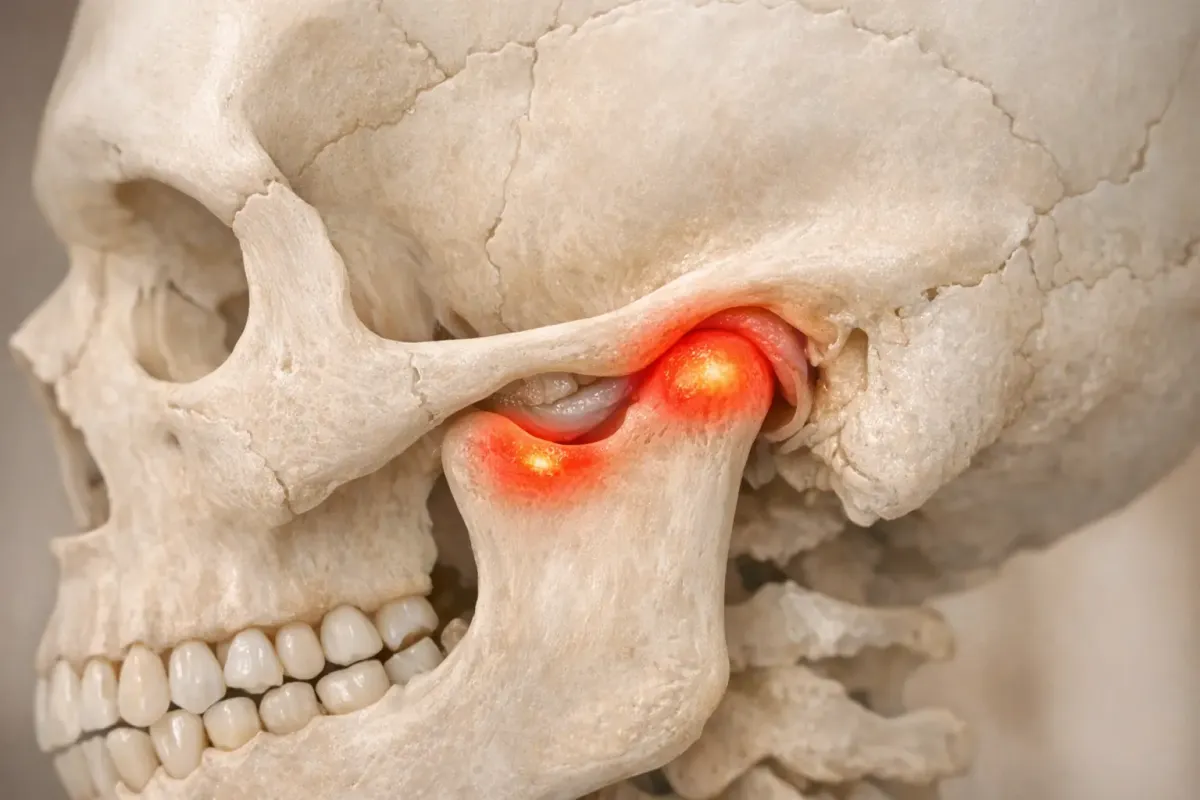
Jaw pain can disrupt sleep, mood, and even your morning smoothie routine. If you've spent late nights researching the difference between a click and a pop, you know temporomandibular joint (TMJ) disorders can be complex. Fortunately, researchers are exploring innovative treatments involving stem cells, advanced cellular therapies, and digital tools that could redefine TMJ care. This article reviews the latest evidence to help you make informed decisions about treatment options.
The following information is sourced from peer-reviewed studies and reputable medical institutions. No pseudoscience or myths—just solid data to discuss with your dentist, oral surgeon, or sleep specialist.
Understanding TMJ Disorders and Current Challenges
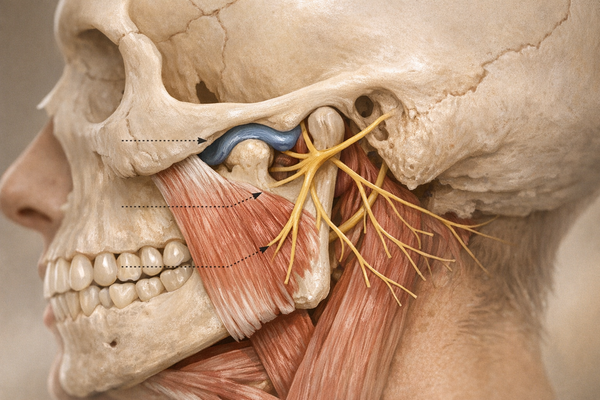
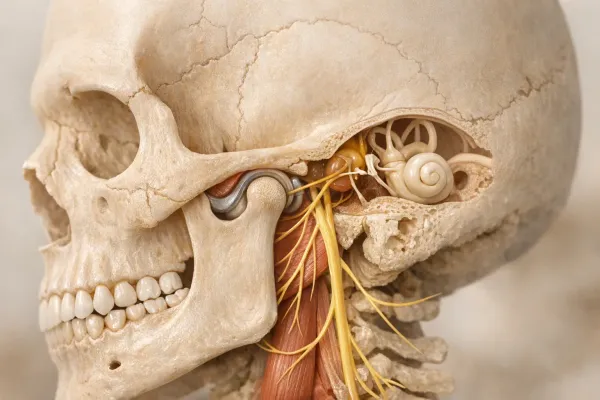
Your TMJ functions like a small sliding hinge, enabling you to talk, chew, and yawn without unhinging your jaw. When it malfunctions, pain, limited opening, and various noises can occur. According to the Mayo Clinic, TMJ disorders are categorized into myofascial pain, internal derangements like disc displacement, and degenerative diseases such as osteoarthritis (OA). Despite the subtype, discomfort and dysfunction are common issues.
Conventional treatments usually start conservatively with soft-food diets, NSAIDs, physiotherapy, and occlusal splints. If these fail, injections or surgery may be considered. A consensus paper by Manfredini et al. emphasizes that most cases improve with simple measures but notes persistent challenges:
- High relapse rates after discontinuing splints
- Lack of treatments for cartilage repair in TMJ OA
- Variable surgical outcomes, especially in arthroplasty
Such challenges drive interest in biological and technology-driven solutions aiming to address the root causes of TMJ disorders.
Traditional medications often fall short, especially when bruxism or sleep apnea adds extra strain. These conditions involve neural and respiratory systems, making mechanical solutions insufficient. The aim is to develop treatments that respect the jaw's biology, not just its mechanics.
Current research focuses on two main goals:
- Regenerating damaged tissue to restore normal joint function;
- Precisely controlling pain pathways beyond standard anti-inflammatories.
Let's explore how stem cells, ferroptosis control, advanced pain modulators, and digital dentistry may achieve these goals.
Stem Cell Therapy: A New Horizon for TMJ Treatment
Stem cells are versatile tools in biology, capable of transforming into bone, cartilage, fat, or connective tissue based on biochemical signals. In joints affected by osteoarthritis, regenerating worn cartilage is crucial. Two animal studies published in 2025 suggest this could soon be possible.
Potential of Mesenchymal Stem Cells
A rat model of TMJ OA explored adipose-derived stromal/stem cells (ADSCs). Mei Ziyi et al. used extracellular vesicles (EVs) released by ADSCs and injected them into inflamed joints. These EVs deliver proteins, lipids, and even mitochondria, leading to:
- Reduced inflammatory cytokines in synovial fluid
- Thicker cartilage with improved collagen structure
- Enhanced mobility in jaw-opening tests
EVs transferred healthy mitochondria, reprogramming local immune cells to foster a healing environment. As EVs don't replicate, they bypass some regulatory challenges of live cell therapies, potentially speeding up human trials.
The second study by Zhang Zerou et al. focused on chondrocyte senescence, using an ADSC-enriched adipose extract to suppress markers of cell aging, resulting in reduced cartilage fibrosis in rabbits.
These studies highlight the potential of fat-derived cells. Harvesting from a patient's body reduces rejection risks. However, dosage guidelines, delivery methods, and long-term safety data are still needed.
Extracellular Vesicles and TMJOA
EV therapy might complement minimally invasive arthrocentesis, where joint fluid is flushed. Adding healing EVs during this process could yield therapeutic concentrations quickly due to the TMJ's small space.
Mechanistically, EVs shift macrophages to an M2 phenotype, promoting tissue renewal. Mitochondrial transfers likely enhance cellular repair energy. If human trials confirm similar results, future treatment protocols could include biologic booster shots alongside traditional care.
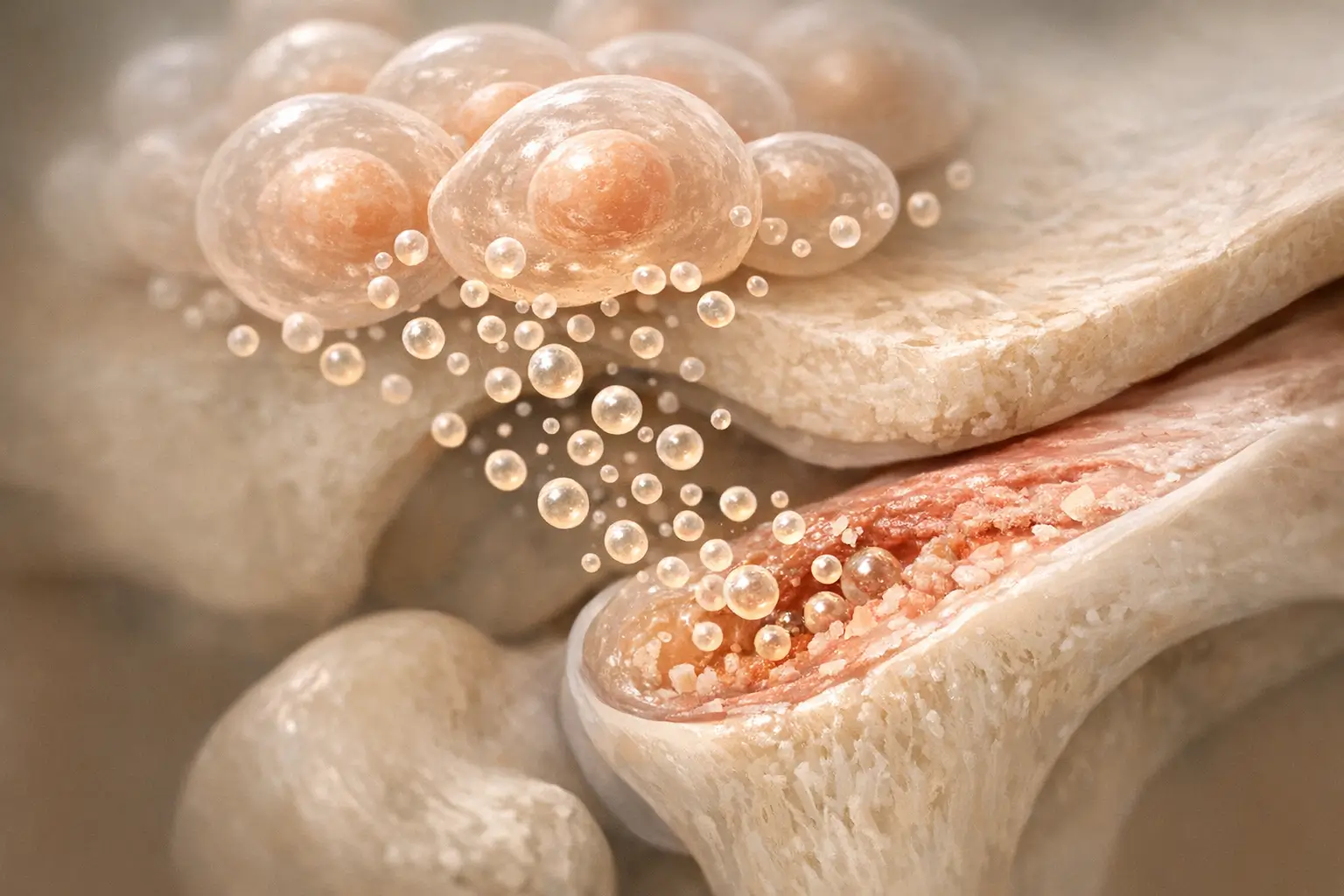
The Role of Ferroptosis in TMJ Osteoarthritis
Ferroptosis, a form of programmed cell death triggered by iron-induced lipid peroxidation, contributes to inflammation. Unlike apoptosis, ferroptosis is chaotic, exacerbating oxidative damage. While studied in knee OA, Zhang Yuxin et al. have begun exploring its role in TMJ OA.
Their review maps genes and pathways linking iron metabolism to cartilage breakdown. Key insights include:
- Chondrocytes in OA accumulate free iron, leading to lipid peroxidation.
- The cystine/glutamate antiporter stalls in OA, depleting the joint's antioxidant defenses.
- Enzymes detoxifying peroxides, like GPX4, are suppressed.
Targeting ferroptosis involves blocking iron influx, boosting antioxidants, or both. Proposed treatments include ferritinophagy inhibitors, iron chelators, and GPX4 activators. This approach could halt disease progression early, rather than merely managing symptoms.
Similar strategies are being tested in neurodegenerative research, with some drugs in clinical trials. Repurposing these for TMJ OA might accelerate treatment availability.
Although data is preclinical, the mechanism aligns with stem cell findings: reducing oxidative stress creates a better environment for tissue repair. Future therapies could combine iron-chelating mouth rinses with EV injections for comprehensive care.
Innovative Approaches in Pain Management
Pain is often the driving factor for seeking aggressive TMJ treatments. Two promising areas are ion channel modulators and optimized appliance protocols.
Transient Receptor Potential Channels
Nerves sense heat, cold, and stress through transient receptor potential (TRP) channels. The review by Varunya Chantadul et al. examines TRP subtypes linked to dental inflammation and orofacial pain:
- TRPV1: Known for its role in spicy food sensations, it mediates inflammatory jaw pain.
- TRPA1: Senses oxidative stress and cold sensitivity.
- TRPM8: Responsive to cooling, explaining why menthol is soothing.
Pharmaceuticals are developing selective antagonists to numb pain without affecting protective sensations. Topical TRPV1 blockers are in trials, potentially leading to a gel or slow-release implant for TMJ pain.
TRP channels also interact with estrogen and serotonin pathways, providing insights into why TMJ disorders often affect women and flare with stress. Blocking specific TRPs may relieve pain without systemic side effects.
Optimizing Occlusal Splint Therapy
Splints are a common treatment for bruxism and myofascial pain, but compliance can be an issue. The ElMohandes protocol modifies traditional splints by adding grooves to help the mandible find a natural position. Key findings include:
- Reduced wear time to 8 hours per day, mostly at night.
- Lowered muscle hyperactivity within two weeks.
- No significant occlusal changes after three months, minimizing bite alteration concerns.
This approach allows for comfortable wear without compromising pain relief. Digital scanning technology helps create precise devices, turning splints into effective, personalized treatments.
By combining custom low-profile splints with targeted TRP modulation, pain can be managed effectively while structural therapies address underlying issues.

Digital Dentistry: Transforming TMJ Treatment
Digital dentistry has revolutionized treatment, moving away from outdated methods. Tang W L et al. reviewed dynamic navigation systems (DNS), which integrate cone-beam CT data with real-time tracking to guide procedures with precision.
In TMJ applications, DNS assists with:
- Accurate placement of mini-screws for procedures
- Precise bone grafting without nerve damage
- Guided delivery of injectables into small joint spaces
Dynamic Navigation Systems
DNS uses optical cameras to track instruments, offering sub-millimeter accuracy and reducing operation time and radiation exposure. This means shorter procedures and fewer errors.
The technology also aids in virtual splint planning, ensuring adjustments are precise. DNS logs can contribute to machine-learning models for refining future treatments, akin to a GPS for dentistry.
Costs vary, but as DNS becomes more common in implantology, it will likely become more accessible for TMJ care. Discuss this technology with your provider to explore your options.
Addressing TMJ and Sleep Disorders
Obstructive sleep apnea (OSA) and TMJ disorders often coexist. OSA's symptoms can strain jaw muscles and joints. A trial by Attia A M M et al. explored how different OSA treatments impact TMJ health.
The study compared continuous positive airway pressure (CPAP), mandibular advancement devices (MADs), and lifestyle changes over six months. Results showed:
- MADs improved apnea and TMJ pain scores more than CPAP, likely due to mandibular repositioning.
- CPAP alleviated daytime sleepiness but had neutral TMJ effects.
- Lifestyle changes offered modest improvements in both areas.
If you use a dental appliance for OSA, it may also benefit your TMJ. However, poorly fitted MADs can cause joint pain. Digital scans and DNS planning can reduce this risk.
The study recommends regular TMJ assessments for OSA patients. If CPAP use leads to jaw stiffness, consider adding a low-profile splint or adjusting treatment. Collaboration between sleep physicians and dentists is crucial.
Bruxism often spikes during apnea. Smart splints that track and provide biofeedback can help relax muscles. Discuss these options at your next dental appointment.
Conclusion: The Future of TMJ Therapy
TMJ care is evolving from generic treatments to targeted, biology-driven interventions. Stem cell-derived extracellular vesicles offer cartilage repair potential, while ferroptosis inhibitors address oxidative damage. For pain management, TRP channel modulators and improved splints provide relief without systemic side effects.
Digital navigation systems enhance surgical precision, and integrated approaches align sleep apnea treatments with jaw health. While no single solution exists, combining these innovations can transform TMJ disorders from chronic challenges into manageable conditions.
Stay proactive with dental checkups, monitor sleep quality, and discuss these studies with your healthcare team. The jaw you save may be your own—and you'll impress at your next dinner party with your knowledge.