Understanding Jaw Pain Relief: What Works and What Doesn't for TMJ
Discover effective solutions for jaw pain relief TMJ. Find what works best.

Jaw pain can truly disrupt your day. Chewing becomes painful, yawning sounds like bubble wrap, and sleep turns into a grind-fest. You’re here for clear answers on temporomandibular joint (TMJ) disorders, so let's get started. We’ll look at what research says, sift through the hype, and guide you toward lasting relief for jaw pain.
The evidence you’ll find here comes from peer-reviewed studies and credible medical organizations. Blue links take you to primary sources. No guesswork, no fluff—just data in plain language you can use today.
Understanding TMJ Disorders and Jaw Pain
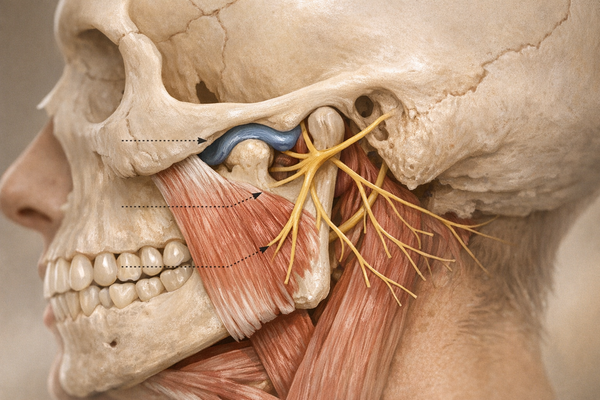
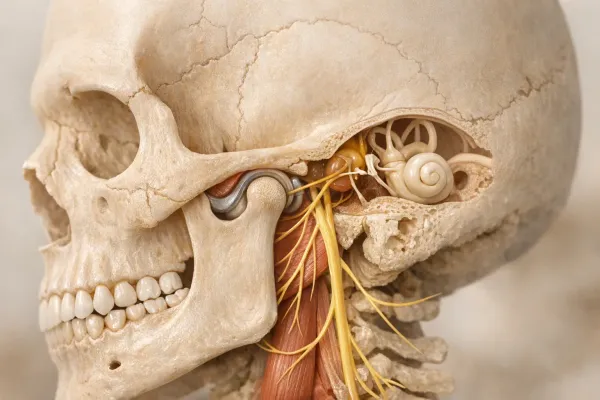
Your TMJ is a small hinge that lets your jaw open, close, and slide like a mini skateboard ramp. When something disrupts that movement—like a displaced disk, inflamed muscle, or excessive tooth grinding—you develop TMJ disorder (TMD). Pain can radiate from your temples to your shoulders, so it's not just a jaw issue.
According to a 2024 systematic review by Madhuri et al., TMD affects up to 15% of adults, with women reporting symptoms more often than men. Another review by Alowaimer et al. in 2024 notes that stress-related muscle tightness, malocclusion, arthritis, and even posture can trigger pain.
Why does this matter for your health? Chronic jaw pain disrupts sleep, increases cortisol, and can worsen headaches or vertigo. Ignoring TMD is like ignoring a smoke alarm because it’s “only in one room.” Long-term inflammation can lead to habits—like clenching or poor posture—that affect your whole body.
If you’re researching TMJ solutions, know that the root cause can be structural, muscular, biochemical, or a combination. This article sorts treatment options into what usually works, what sometimes works, and what rarely helps. Ready for some pain relief intel? Keep reading.
Conservative Treatments for TMJ Relief
First up: everything to try before surgery. Conservative care includes physiotherapy, medication, self-management habits, and simple tools like heat packs or soft diets.
Physiotherapy and jaw-specific exercise. A 2025 study by Kong et al. tracked 120 patients with disk perforations. They found that targeted stretching, postural correction, and manual mobilization reduced pain by 50% in eight weeks (Kong, Huh, & Kho 2025). Good news: these exercises may look silly but are free, and you can do them during Netflix ads.
Try this: each morning, stand in front of a mirror, place your tongue on the roof of your mouth, and slowly open your jaw until you feel a stretch—then close. Repeat ten times. Follow with five chin-tucks to reset neck posture. Two minutes total, no excuses.
Drug therapy. Over-the-counter NSAIDs reduce inflammation, while short-term muscle relaxants can stop nighttime clenching. The same Kong study found faster pain relief when medication accompanied exercises, but the benefits leveled out after three months—so drugs buy you time, not a cure.
Tip: Take doses with meals to protect your stomach and log them in a phone app to avoid double-dipping on ibuprofen during a busy day.
Lifestyle tweaks. Avoid chewy gum, favor softer foods for a few weeks, and use ice after long meetings if you notice jaw tension. The Mayo Clinic suggests good sleep hygiene and stress management to reduce parafunctional habits like day clenching.
Try this stress-breaker: set a silent timer to buzz every hour. When it does, check that your teeth are apart and your shoulders are low. These “micro audits” can stop jaw tension before it escalates.
Heat and cold. Apply moist heat for 20 minutes followed by five minutes of ice to calm a flare-up. While not glamorous, a randomized segment in the Alowaimer review recorded moderate pain reduction with simple thermal cycles, similar to low-dose ibuprofen Alowaimer et al. 2024.
Benefits and Limitations
- Benefits: Low cost, minimal risk, empowers you to self-manage flares.
- Limitations: Requires discipline. Some patients plateau if structural damage exists. Meds can mask pain, tempting you to push through activities that aggravate the joint.
The Role of Occlusal Appliances in TMJ Management
Occlusal appliances—night guards, anterior repositioning splints—are dental tools that cushion biting forces and may decrease muscle activity during sleep.
How They Work
Your jaw acts like a tripod balanced on your molars and joint sockets. When you grind, it rattles. A splint spreads the load more evenly. An anterior repositioning splint (ARS) brings the jaw slightly forward. A 2025 meta-analysis by Wang et al. reviewed 18 trials, concluding that ARS devices cut pain scores by an average of 2.1 points on a 10-point scale after three months, slightly outperforming soft night guards.
Mechanistically, occlusal guards may:
- Reduce microtrauma to the joint surfaces.
- Interrupt muscle memory of clenching patterns.
- Increase joint space, allowing the inflamed disk to heal.
When to Use Them
The American Dental Association suggests using a guard when conservative rehab stalls. Mahdi and Al-fahham 2025 found that custom hard acrylic guards were more durable than over-the-counter models, though softer versions were sometimes more comfortable. Nightly use for at least six weeks is key. If your morning bite feels strange or headaches worsen, see your dentist to adjust the fit.
Real-world scenario: Sarah, a 34-year-old coder, used a store-bought guard and quit after three nights due to discomfort. Her dentist later fitted a custom acrylic splint; discomfort vanished within a week, and jaw clicks faded by month two. Initial cost is higher, but compliance drives success.
Bottom line: appliances work best as an adjunct, not a standalone solution. Think of them as seatbelts—essential during a crash but not the reason you drive safely in the first place.
Innovative Approaches: TENS, Ultrasound, and Laser Therapy
Tech enthusiasts rejoice; gadgets have entered the TMJ arena. Transcutaneous electrical nerve stimulation (TENS), therapeutic ultrasound, and low-level laser therapy (LLLT) promise quick sessions and minimal effort. Let's see if they deliver.
TENS. By sending mild electrical pulses through surface electrodes, TENS aims to block pain signals and relax muscles. A 2025 trial by Bhoi et al. compared 30 TMD patients receiving TENS, ultrasound, or LLLT over four weeks. The TENS group reported a 40% drop in pain, slightly edging out ultrasound and tying with laser. The placebo (sham device) cohort only saw a 10% dip.
Many clinics rent portable TENS units for $20-$30 per month. Once settings are dialed in, you can treat yourself during a podcast commute. Just mind battery levels—nothing kills a relaxing buzz like mid-pulse shutdown.

Ultrasound. Therapeutic ultrasound uses sound waves to heat deep tissues. In the same trial, ultrasound reduced muscle tenderness but lagged behind TENS in improving mouth-opening range. Still, for patients who dislike the tingling sensation of TENS, ultrasound offers an alternative.
Low-Level Laser Therapy. LLLT, also called cold laser, aims to boost cellular energy production and cut inflammation. Bhoi’s study notes that laser therapy achieved the fastest onset of pain relief—within the first week—but gains plateaued by week four. Meanwhile, Alowaimer’s 2024 review calls the overall evidence “promising but inconsistent,” mainly due to varied laser settings.
Comparing New Technologies
- TENS: Best for muscle-driven pain, accessible for at-home use once a clinician sets initial parameters.
- Ultrasound: Therapist-delivered, good for deeper tissue heating, modest evidence for mobility gains.
- LLLT: Quick sessions, minimal sensation, needs more standardized protocols to confirm long-term value.
Takeaway: tech tools shine as pain modulators but rarely fix underlying biomechanical issues. Pair them with exercise or splints for sustainable results.
Acupuncture and Alternative Therapies
The needle-curious among you may wonder if ancient practices hold modern merit. A controlled trial from 2024 put acupuncture through a rigorous test. Liu et al. randomized 90 TMD patients to true acupuncture, sham needling, or standard care. After six sessions, the true acupuncture group logged a 3-point pain drop versus a 1-point dip in sham and zero change in standard care.
Effectiveness and Evidence
Why might acupuncture work?
- Stimulates endorphin release, the body’s natural painkillers.
- Improves local blood flow, aiding tissue repair.
- Encourages relaxation, reducing bruxism triggers like stress.
Yet efficacy depends on practitioner skill and point accuracy. Benefits taper after three months unless sessions continue every two weeks. Other complementary approaches—yoga, mindfulness, magnesium supplements—show anecdotal promise, but robust data are thin.
Insurance pearls: in the U.S., about half of major carriers reimburse acupuncture for pain management. Call ahead; nothing spikes jaw tension like a surprise bill.
Verdict: acupuncture earns a provisional green light for short-term relief, especially if you’re needle-friendly and want a drug-free option. Just budget for maintenance visits.
Surgical Interventions: When Are They Necessary?
Sometimes the joint deteriorates beyond what conservative options can manage. In those cases, surgery steps in. But how do you know when you’re in “knife territory”?
Madhuri’s 2024 review and a historical overview by Dolwick & Widmer 2024 outline the main surgical categories:
- Arthrocentesis. Saline irrigation to flush inflammatory debris.
- Arthroscopy. Keyhole surgery to trim adhesions or reposition a disk.
- Open-joint surgery. Disk repair, graft, or joint replacement for severe degeneration.

Pros and Cons
Pros:
- Rapid mechanical correction when a disk is folded like origami and can’t self-reset.
- High success rates for specific indications—arthrocentesis resolves closed-lock cases up to 80% according to Madhuri’s review.
Cons:
- Cost, potential nerve injury, scar formation.
- Requires downtime; you’ll be on a broth diet longer than you might like.
- No guarantee against relapse if underlying habits go unaddressed.
Long-term Outcomes
Dolwick & Widmer trace TMJ surgery history from the 1970s era of flawed implants to modern joint prostheses with 10-year survival rates above 90%. Still, their review stresses that long-term quality of life hinges on sustained rehab and lifestyle change—not the metal joint alone. Likewise, a 2025 study by Cao et al. saw comparable five-year pain scores between surgical and well-executed conservative groups, underscoring that surgery should follow, not replace, holistic care.
Typical timeline: two weeks liquid-only diet, six weeks soft foods, and three months before unrestricted chewing. Physical therapy usually starts day three post-op, focusing on gentle range-of-motion exercises to prevent scar tightening.
Conclusion: Finding the Right Jaw Pain Relief Solution for You
TMJ disorders rarely respond to a single solution. The evidence presented here supports a layered approach: start with education, exercises, and bite management. Add an occlusal appliance if clenching is a problem. Use gadgets—TENS, ultrasound, laser—when pain spikes. Consider acupuncture if you prefer a drug-free assist. Keep surgery as a last resort, not the first option.
Your practical checklist:
- Day 1–7: Begin mirror-based stretching; log pain and diet in a notes app.
- Week 2: Try heat/ice cycles and audit posture hourly.
- Week 4: If pain persists, consult a dentist for a custom guard.
- Month 2: Layer in TENS or acupuncture to speed recovery.
- Month 4+: Re-evaluate with a specialist; discuss imaging or surgical options only if function remains limited.
Your next steps? Track symptoms, film your posture, and share both with a dentist or orofacial pain specialist. Show them the studies linked here to demonstrate your commitment to evidence-based solutions. With the right mix of science, persistence, and a touch of irreverence, relief is more than possible—it’s likely.