Understanding Biofeedback Devices for Effective Bruxism Management
Explore how biofeedback devices help manage bruxism and reduce teeth grinding.

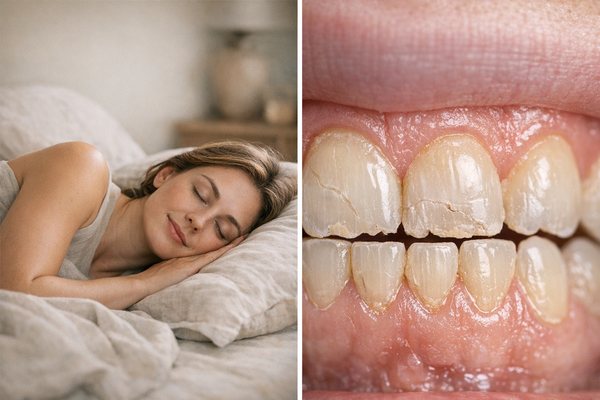
Bruxism, the medical term for tooth grinding and jaw clenching, is a significant issue in sleep lab data and dental charts. You might not feel it happening, but the damage can accumulate over time. Researchers have spent decades studying this problem. The latest studies are working on using biofeedback devices to help your jaw relax, and these devices can be worn to bed.
In the next few minutes, you'll learn what bruxism is, why your dentist keeps mentioning splints, and how biofeedback devices are changing treatment options. We will focus on peer-reviewed evidence, keep the language clear, and offer practical advice so you can decide if biofeedback is right for you.
What is Bruxism and Why It Matters
Bruxism is the repetitive grinding or clenching of teeth that occurs while you're awake or asleep. The American Dental Association identifies it as a leading cause of cracked enamel, worn fillings, and jaw pain. Many people only discover they grind their teeth when a partner notices or a dentist spots the wear.
The prevalence of sleep bruxism is estimated at 8 to 15 percent of adults, while awake bruxism is even more common, often occurring during stressful times. Diagnosing bruxism is challenging because it happens during sleep and the damage accumulates slowly. Polysomnography is accurate but expensive, so dentists often use questionnaires or nighttime audio recordings, which can miss silent clenching.
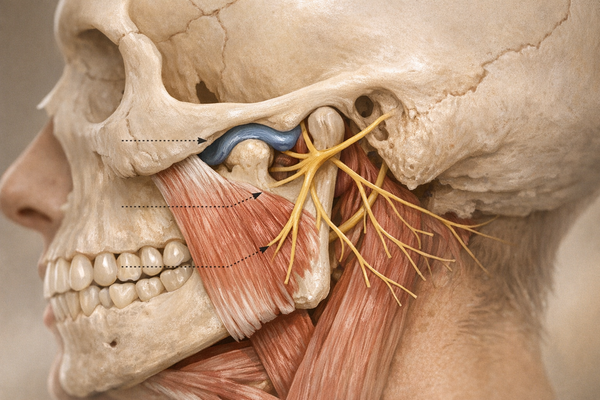
Why is this important? Beyond chipped teeth, bruxism is linked to tension-type headaches, temporomandibular joint (TMJ) disorders, and disrupted sleep. A 2025 study by Al-Hamad Khalid A et al. showed that repetitive jaw loading increases muscle fatigue, potentially worsening morning soreness. Meanwhile, a 2024 review by Ainoosah Sultan et al. notes that untreated grinding can shorten the lifespan of dental restorations, increasing future costs.
If you wake up with jaw tension or your dentist points out tooth wear, bruxism should be addressed before it impacts your quality of life further. Discover unexpected causes of nighttime teeth clenching and how to manage them effectively.
The Role of Biofeedback in Bruxism Management
Biofeedback is a therapeutic approach that turns bodily signals into cues you can recognize and adjust. Think of a smartwatch that vibrates when your heart rate spikes, but this time it's your jaw muscles being monitored. The goal is behavioral change: by noticing clench events in real time, you can interrupt the habit loop that drives bruxism.
How Biofeedback Works
Most bruxism biofeedback systems use surface electromyography (sEMG) or intraoral pressure sensors. When your jaw muscles exceed a preset threshold, the device sends a gentle alert. This can be a vibration, an auditory tone through bone conduction, or a micro-pulse inside a mouthpiece. The signal is subtle enough not to wake you fully, yet strong enough for your brain to register. Over time, this feedback trains your neuromuscular system to stay relaxed.
The concept is based on decades of research in psychophysiology. Operant conditioning shows that immediate cues are effective at shaping automatic behaviors. Biofeedback harnesses this science in consumer devices small enough to fit on a molar.
Types of Biofeedback Devices
- Intraoral mouthpieces: These resemble slim dental retainers but contain pressure sensors and electronics. When bite force exceeds the threshold, the mouthpiece vibrates locally. The prototype described in the Al-Hamad 2025 paper even transmits data to a smartphone for nightly reports.
- Adhesive sEMG patches: A disposable electrode pad sticks over the masseter. During clench spikes, it cues a small vibrotactile pod on your cheek. This style is popular for daytime use when wearing a mouthguard may feel awkward.
- Headband or temple sensors: Some devices integrate sEMG leads into a fabric band and use Bluetooth to trigger a wrist vibration. They double as sleep trackers, though false alarms can be an issue if the band slips.
- Smartphone-assisted earbuds: Experimental models route sEMG data to a phone app that pings an earbud. These remain niche, but early adopters like the hands-free audio option.
A 2023 systematic review by Vieira Maryllian de Albuquerque et al. grouped these tools into awake and sleep categories and found that wear-time adherence is higher when the hardware is thin and wireless. Learn more about how biofeedback offers a promising approach to bruxism therapy.
Clinical Evidence Supporting Biofeedback for Bruxism
We have innovative gadgets, but do they work? The short answer is yes, though the evidence is still developing. Let's explore the highlights.
The intraoral system developed by Al-Hamad’s team underwent testing to verify sensor precision and moved to a pilot trial with twenty volunteers. Results showed a 58 percent reduction in peak bite force over two weeks and no adverse events. Clinically, tooth-on-tooth contact time dropped from an average of 17 minutes per night to just under 8.5 minutes, suggesting significant enamel protection.
On the systematic front, Vieira et al. 2023 compared biofeedback with splints, behavioral therapy, and no treatment in adults with awake bruxism. Across eight randomized controlled trials, biofeedback produced a mean decrease of 32 percent in EMG activity, outperforming relaxation coaching by about ten percentage points. The review noted small sample sizes, but consistency across studies boosts confidence.
Mechanistically, sEMG logs show that feedback alerts occur within 200 milliseconds of a clench burst. Neurophysiology studies suggest that such rapid cues integrate into the brain’s startle pathway, rewiring patterns without the cognitive load of conscious counting. The result is learning that persists even when you're half asleep.
Clinically important side effects are rare. Participants mainly report momentary sleep fragmentation during the first nights. Data from over 150 cumulative patient-years in the Vieira review showed no increase in TMJ pain or dental fractures, a concern sometimes raised with vibratory devices.
The gold standard trial is still pending, but current data is sufficient for many dentists to recommend biofeedback as a front-line option if splints fail or cause gag reflex issues.

Comparing Biofeedback with Traditional Bruxism Treatments
Occlusal Splints vs. Biofeedback
Occlusal splints, also known as night guards, have been a common treatment for decades. They create a physical barrier that redistributes bite forces and prevents enamel wear. However, they do not stop the muscle activity that causes grinding. A 2025 trial by Tandon et al. compared splints with sleep hygiene plus progressive muscle relaxation. After eight weeks, both groups showed similar reductions in perceived stress, but EMG data revealed that splints alone reduced clench episodes by just 13 percent.
Biofeedback, on the other hand, targets the habit itself. Users receive an immediate cue, learn to relax the jaw, and over time the nervous system rewrites the default pattern. Although head-to-head comparisons are limited, a 2023 analysis by Lei Qun et al. concluded that adding biofeedback to a slim splint reduced EMG levels 28 percent more than splinting alone. For more on selecting the right mouth guard, check out this comprehensive guide.
Comfort is also a consideration. Splints can warp if cleaned in hot water and may trigger drooling or speech issues. Modern intraoral biofeedback guards are thinner—some are under 2 millimeters—so user compliance increases. Battery life is the trade-off; expect weekly charging.
Sleep Hygiene and Muscle Relaxation
Cognitive behavioral strategies are effective for stress-driven bruxism. Regular bedtimes, low caffeine intake, and guided jaw relaxation are affordable and have no side effects. The same Tandon trial found that muscle relaxation reduced grinding episodes by 11 per hour, compared with 8 for splints. Effective, but patients need consistent practice.
Biofeedback can complement these habits. Many apps include wind-down reminders with EMG logging, creating a dual loop of accountability. The Sleep Foundation notes that combining relaxation audio with a feedback mouthpiece provides both top-down and bottom-up control. In simple terms, you're teaching your mind to stay calm while also nudging your jaw when it forgets. Discover natural ways to relieve jaw tension without invasive methods.
Cost is another factor. Custom splints can be expensive, while over-the-counter guards are cheaper but less durable. Biofeedback devices fall in the middle; as manufacturing scales, prices are approaching mass-market fitness tracker territory.
Integrating Biofeedback Devices into Your Daily Routine
Buying high-tech gear is one thing, but using it nightly is another. Success depends on three factors: fit, feedback threshold, and follow-through.
- Get the fit right. If you choose an intraoral device, ask for a boil-and-bite kit or a 3-D printed custom tray. A loose fit triggers false alarms and disrupts sleep. Many companies offer mail-in impression kits you can complete at home.
- Calibrate the threshold. Most apps include a jaw-clench test during setup. Do not skip it. Your baseline force is unique. Too sensitive, and the device vibrates at every swallow. Too lax, and grinding slips through.
- Pair with wind-down rituals. Insert the mouthpiece after brushing your teeth, then start the companion app’s five-minute relaxation track. This anchors the habit and triggers your parasympathetic system.
- Review the data weekly. Graphs showing a reduction in microbursts make the invisible visible, reinforcing motivation. If numbers plateau, adjust thresholds or consult your dentist.
- Daytime check-ins. If stress triggers clenching at your desk, use an adhesive sEMG patch during high-stakes calls. Training by day enhances overnight gains.
Compliance numbers tell the real story. In the Vieira 2023 review, average nightly wear time was 6.3 hours, which is within normal adult sleep. Drop-outs usually occurred in week two when the novelty wore off. Incorporating the device into an established bedtime routine—similar to phone charging—increased retention.
If you use a CPAP for sleep apnea, check compatibility. Most feedback guards fit comfortably under a nasal mask, but full-face straps may press on the electronics. Do a quick dry run before bedtime. For more details on managing sleep disorders related to bruxism, explore this resource.

Future Directions in Bruxism Management Technology
The biofeedback scene is just getting started. Engineers are borrowing techniques from neurorehab and sports wearables to make devices smarter, smaller, and more personalized.
A 2025 review by Guokai Gu et al. on biofeedback in stroke rehab discusses machine-learning algorithms that adapt thresholds dynamically. Applying this to bruxism could mean your mouthpiece notices when you're stressed and adjusts sensitivity accordingly.
Energy harvesting is another frontier. Piezoelectric films in the guard could convert bite pressure into micro-charge, reducing the need for nightly charging. Early prototypes generate enough current to run low-power Bluetooth beacons, and progress is rapid.
Expect multimodal sensors too. Combining EMG with heart-rate variability or skin response may predict grinding before it starts, issuing a cue to prevent a clench burst. Some dental schools are piloting smart splints that send data to cloud dashboards, allowing clinicians to adjust settings remotely, similar to telemedicine pacemaker checks.
Regulatory pathways are becoming clearer. The FDA now classifies most biofeedback mouthpieces as class II wellness devices, easing market entry while ensuring safety testing. Greater competition usually leads to lower prices and better design.
Finally, integration into broader sleep ecosystems is likely. Imagine your mouthguard communicating with a smart mattress or lighting system, adjusting room temperature and lighting to create an ideal sleep environment. The line between dental gear and whole-body sleep tech is blurring quickly.
Conclusion
Biofeedback devices shift bruxism management from passive protection to active retraining. Backed by emerging evidence from studies such as Al-Hamad et al. 2025 and the Vieira 2023 review, these gadgets reduce grinding episodes, preserve enamel, and work well with lifestyle changes. They are not magic solutions, but when calibrated and used consistently, they help break the grinding habit. Talk to your dentist, weigh the pros and cons, and consider adding a smart mouthpiece to your bedtime routine. Your teeth will thank you in the morning. For those interested in innovative therapies, explore new TMJ treatments that may complement bruxism management.