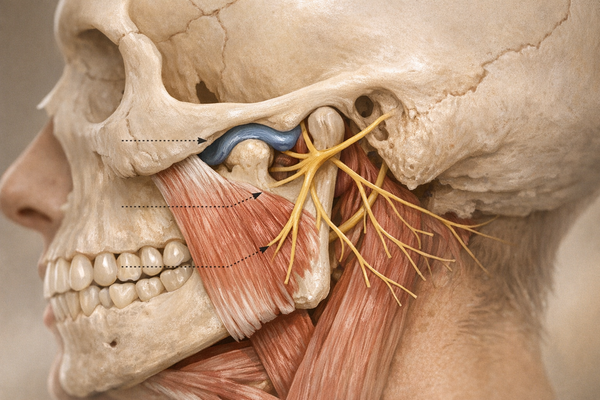
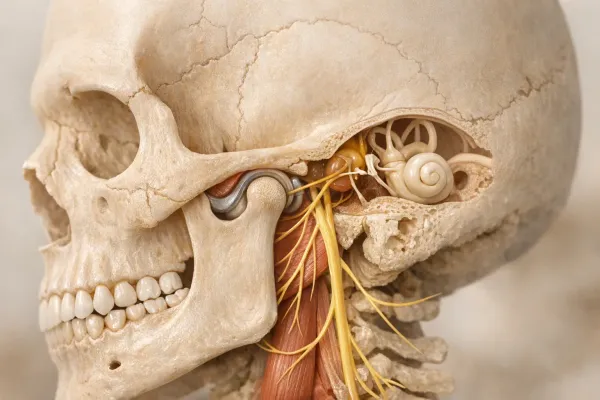
Why Am I Clenching My Teeth at Night? Uncovering Unexpected Causes
Discover unexpected causes of nighttime teeth clenching and how to manage them.
You wake up, pry your jaw apart, and wonder why your molars feel like they spent the night in a boxing ring. If you've been told you probably grind or clench—known as bruxism in dental terms—you may have Googled the usual answers and walked away with a shrug. Stress, caffeine, and late-night work emails often top the list. But current research reveals more complex causes of nighttime teeth clenching.
Below, you’ll discover what recent studies say about unexpected reasons for clenching teeth at night, plus practical ways to ease that nocturnal grip. Some of these factors might surprise you.
The Usual Suspects: Common Causes of Nighttime Teeth Clenching
Let's start with the basics. Bruxism’s common causes include psychological stress, anxiety, and poor daytime posture. The American Dental Association lists stress as a leading cause. Daytime muscle tension often carries into the night, keeping your jaw muscles active.
Medications are another factor. Selective serotonin reuptake inhibitors, amphetamines for ADHD, and some antipsychotics can increase muscle activity around the jaw. The Mayo Clinic notes that taking these medications in the evening may worsen nighttime clenching. If you're experiencing stimulant-induced bruxism, you may find it helpful to explore why ADHD stimulants like Adderall cause teeth grinding.
Lifestyle choices also play a role. High caffeine intake, alcohol before bed, and recreational drugs can keep your nervous system active. Misaligned teeth or an uneven bite can further contribute, as your jaw moves unconsciously to find a comfortable position. To understand the effects of caffeine on your bruxism, consider reading about caffeine and bruxism.
Additionally, don't overlook comorbid sleep disorders. Untreated obstructive sleep apnea (OSA) can trigger clenching as the body struggles to maintain airway stability. The National Sleep Foundation estimates that up to a third of people with OSA also grind their teeth. To learn more about the connection between sleep disorders and bruxism, check out Understanding Sleep Disorders and Their Connection to Bruxism.
These are well-known causes. If you’re still mystified, read on to explore lesser-known factors identified by new research.
The Role of Sleep Quality and Glycemic Management
Think blood sugar only matters if you have diabetes? Think again. A pilot study by Taniwaki et al. monitored real-time mandibular muscle activity (RMMA) alongside glucose data in adults who clench at night. They found that dysregulated glycemic patterns, particularly sharp nocturnal dips, were linked to spikes in RMMA, leading to grinding.
In simple terms, when your blood sugar drops, your jaw muscles get active. A sudden glucose drop can activate the sympathetic nervous system, prompting muscle action even while you sleep. You don’t need to be diabetic; poor sleep habits or an unbalanced dinner can cause similar effects.
Sleep stage distribution also matters. Participants who cycled quickly out of deep, restorative sleep experienced more RMMA bursts. If you frequently shift between light sleep and wakefulness, your nervous system never fully relaxes, keeping your jaw tense. For tips on maintaining good sleep hygiene to manage bruxism, see The Role of Sleep Hygiene in Managing Bruxism and Improving Quality of Life.
What You Can Do Tonight
- Eat a balanced snack with protein and complex carbs an hour before bed to stabilize glucose. Try an apple with peanut butter rather than a sugary treat.
- Limit alcohol, which can cause blood sugar to drop in the early morning. Learn more about the effects of alcohol on teeth grinding.
- If you use a continuous glucose monitor, check for dips around 1–3 a.m. and discuss them with your doctor or dietitian.
- Ensure deep sleep by keeping your bedroom dark, quiet, and cool. Consistent sleep-wake times help too.
Addressing glycemic swings won’t replace a mouth guard but can reduce the frequency and intensity of clenching episodes, protecting your enamel.
Altitude Changes: The Impact of Hypobaric Hypoxia
If you often fly across time zones or visit high-altitude places, your jaw may react to thin air. A study by Peña et al. exposed volunteers to simulated high-altitude conditions (hypobaric hypoxia) and found that sleep bruxism episodes doubled compared to sea-level nights.
Why does low oxygen cause jaw clenching? The authors suggest a respiratory link. Hypoxia makes breathing erratic, and each micro-arousal from unstable breathing activates brainstem centers that control chewing muscles. This sympathetic response, meant to open your airway, also triggers clenching. If you're curious about how sleep positions can influence nighttime teeth grinding, explore more about sleep positions here.
Consider a typical itinerary: board a late-night flight, nap in a pressurized cabin simulating 6,000–8,000 ft of altitude, land, and sleep in a hotel. Your body experiences prolonged lower oxygen saturation, keeping your airway defense reflex active through the first night.
Practical Hacks for Frequent Flyers
- Hydrate well; dehydration worsens altitude insomnia and muscle cramps.
- Use nasal saline spray or a humidifier in dry mountain air to keep your airway moist.
- Ask your dentist about a travel-friendly night guard for use on planes and in hotels.
- Plan an acclimatization day if you ascend above 8,000 ft. Even 24 hours of gradual ascent can calm the respiratory reflex loop.

Hormonal Influences: Estrogen and Temporomandibular Disorders
Hormones affect more than mood. Research shows that fluctuating estrogen can affect temporomandibular joint (TMJ) tissues and alter muscle function. This matters because TMDs and bruxism often co-occur. If you're dealing with TMJ pain, you might find relief through effective TMJ exercises.
Estrogen Levels
A systematic review by Zieliński and Pająk-Zielińska concluded that lower estrogen levels, such as during menopause or certain menstrual phases, correlate with higher rates of TMD pain. Less estrogen means less lubrication and elasticity in the TMJ disc, making the joint more sensitive to overload.
For some, clenching is an attempt to stabilize a joint that feels “off.” The review highlighted that estrogen receptors in jaw muscles and joint cartilage can alter muscle metabolism, potentially increasing clenching when estrogen drops.
Conversely, a review by Alam et al. explored estrogen replacement therapy (ERT) and found mixed results. While ERT improved joint lubrication in some cases, it didn’t universally reduce bruxism frequency. Hormonal balance may ease joint pain, but other triggers still need addressing.
Pregnancy and TMD
During pregnancy, estrogen and progesterone levels rise, yet a study by Minervini et al. reported a surprising increase in self-reported TMD symptoms among pregnant participants compared to non-pregnant controls. Fluid retention can swell joint tissues, while postural changes shift bite alignment. Combined with disturbed sleep in the third trimester, jaw muscles may overwork.
If you’re navigating perimenopause, pregnancy, or other hormonal changes, your jaw pain might not be "all in your head." Hormonal status should be part of any bruxism assessment, especially if clenching intensity increases unexpectedly.
Take-Home Tips for Hormone-Related Clenching
- Track bruxism episodes alongside menstrual cycles or hormone therapy doses to identify patterns.
- Discuss ERT or hormonal interventions with both your gynecologist and dentist; coordination is key.
- Use warm compresses on the jaw during hormone dip phases to keep joint tissues supple.
- Maintain an anti-inflammatory diet rich in omega-3s to counter joint swelling.
Bruxism in Children: A Unique Perspective
If you hear crunchy sounds from your child’s bedroom, note that children’s bruxism isn't just a smaller version of the adult problem. A review by Leung et al. points out that up to 30 percent of kids grind at some point, peaking around age six. To better understand what parents need to know about pediatric bruxism, visit Understanding Pediatric Bruxism.
Why the age gap? Developing nervous systems are learning to regulate muscle tone during sleep. Enlarged tonsils or adenoids that narrow the airway can cause pediatric bruxism, acting like a CPAP machine to maintain airflow. Unlike adults, many kids outgrow the habit as craniofacial structures mature and airways widen.
Red Flags Worth a Pediatric Check-In
- Permanent teeth showing visible wear.
- Morning headaches or jaw soreness in a child who can’t articulate grinding.
- Snoring or mouth breathing, signaling airway obstruction.
- Intensifying ADHD symptoms; some studies link stimulant meds to temporary bruxism.
The review emphasizes behavioral approaches—consistent bedtime routines, stress reduction through play—and, if needed, referral to an ENT to evaluate airway size. Custom night guards are rarely recommended for young children as baby teeth shift.
Therapeutic Approaches: Beyond the Basics
Mouth guards are a common fix but address the symptom, not the cause. Emerging research highlights interventions that target muscle tension at its roots. If you're looking for ways to manage bruxism without a mouth guard, consider natural bruxism solutions.
Manual Therapy and Home Exercises
A clinical trial by Kadıoğlu et al. assigned adults with bruxism to manual therapy and home exercises. Compared to splint-only controls, the therapy group reported larger drops in pain, stress, and nighttime muscle activity measured via electromyography.
The protocol included soft-tissue release of the masseter and temporalis muscles, gentle cervical spine mobilization, and self-stretching exercises. Participants did tongue-to-palate posture drills and controlled jaw opening exercises twice daily. Compliance was about 85 percent, suggesting the routine is manageable.
Why does this work? Chronic clenchers often have neck and upper-back stiffness, forming a kinetic chain that affects jaw tension. Loosening the chain upstream allows the jaw to relax downstream. Diaphragmatic breathing during stretches also activates the parasympathetic nervous system, reducing overall tension.
How to Build Your Own Program
- Learn the “goldfish” exercise: place your tongue on the roof of your mouth, one finger on the TMJ in front of the ear, another on the chin, then gently drop the lower jaw halfway and close. Repeat six times, three sets daily.
- Foam-roll the upper back for two minutes before bed; thoracic mobility reduces forward-head posture that strains the jaw.
- Use a tennis ball under the masseter. Lean into a wall, hold pressure for 20 seconds, release, and repeat.
- Finish with 3–5 slow nasal breaths, letting the abdomen expand, to cue full-body relaxation.

Manual therapy is not a one-off spa day. The study scheduled six in-office sessions over three weeks, proving frequency counts. If professional care is out of reach, even a virtual consult with a physical therapist can teach you safe techniques.
Conclusion: Managing Nighttime Teeth Clenching
Teeth clenching is not just a stress side effect. Blood sugar swings, thin mountain air, hormone fluctuations, and even developing airways in children can all trigger jaw tension. The good news: targeted adjustments—steadying glucose, planning for altitude, coordinating hormonal care, and embracing manual therapy—can reduce clenching.
If your enamel keeps taking hits, consult your dentist or sleep physician about these factors. A custom plan that combines biomedical insight with lifestyle strategies offers the best chance for restful nights and intact molars. For more tips on preventing nighttime teeth clenching, check out How to Prevent Nighttime Teeth Clenching.