Natural Bruxism Solutions: Manage Without a Mouth Guard
Discover effective natural bruxism solutions without using a mouth guard.

You wake up with a stiff jaw and teeth that feel like they ran a marathon overnight. Your dentist hands you a bulky plastic mouth guard, and you nod politely while thinking, "There has to be another way." Good news: there is. Researchers are uncovering a growing list of natural and low-tech fixes for bruxism, the involuntary grinding or clenching of teeth. Below, you will find the evidence, the how-to, and a reality check for every option—so you can decide which path makes the most sense for your nightly grind.
This article digs into peer-reviewed studies such as Davis et al. 2026 and Shafiee and Nourizadeh 2025, along with guidance from stalwarts like the American Dental Association. You will get plain-language breakdowns of why your jaw muscles misbehave plus realistic strategies—no night guard required.
Understanding Bruxism and Its Impacts
Bruxism is the medical term for grinding, gnashing, or clenching your teeth when you are not consciously chewing food. It comes in two main flavors:
- Sleep bruxism: This happens while you are snoozing. Because it is involuntary, people often learn about it only after a partner complains about the noise or a dentist spots telltale enamel wear.
- Awake bruxism: This shows up during the day as jaw clenching or tooth tapping, usually during stressful tasks or deep concentration.
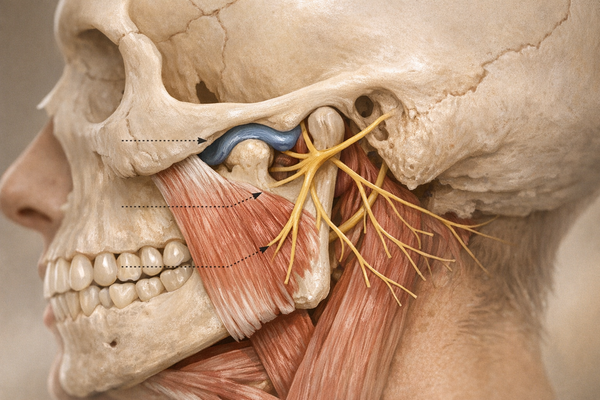
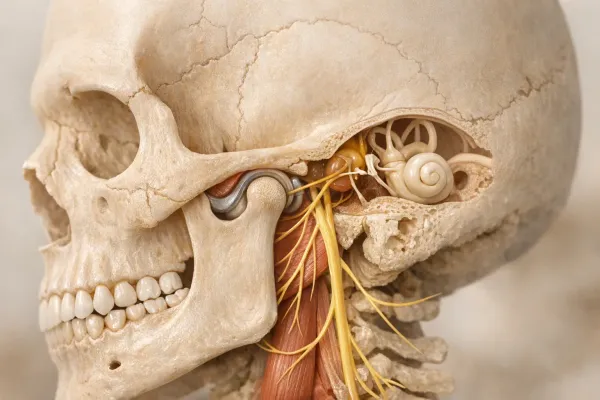
Both types fire the masseter and temporalis muscles far harder than normal chewing does. A single night can load those muscles with forces up to 250 pounds. Over weeks to years, the habit leads to flattened biting surfaces, cracked fillings, and tension headaches.
According to a comprehensive review by Davis et al., sleep bruxism sits at the crossroads of dental, neurological, and psychological disciplines. Prevalence estimates range from 8 to 31 percent of adults. Special populations, such as individuals with Down syndrome, are even more vulnerable. A 2023 meta-analysis by Alam et al. reported rates over 42 percent in that group.
Dentally, the fallout is obvious: chipped enamel, jaw tenderness, and sometimes tooth loss. Systemically, the condition also disrupts sleep architecture. Micro-arousals fragment deep sleep, leaving you foggy and irritable the next day. Left unchecked, the chronic stress of nocturnal muscle contractions can aggravate temporomandibular disorders (TMD) and even heighten risk for tension-type headaches.
The classic management plan is a rigid or thermoflexible occlusal splint that separates the arches. Mouth guards act like a bumper between two cars on a parking lot collision course. Although effective, they do not treat the root cause, and many users abandon them due to bulk or drooling. That is why clinicians are increasingly exploring non-invasive or minimally invasive options, most of which you can combine to build a personalized anti-grind toolkit.
The Role of Stress Management in Bruxism Relief
Stress is a usual suspect in both sleep and awake bruxism. When cortisol climbs, so does muscle tension. A rapid evidence review by Matheson et al. 2023 concluded that psychological factors are as important as biomechanical ones in TMD and related bruxism. Tackling mental strain can therefore tone down jaw overactivity.
A dozen relaxation or psychoeducational therapies exist, but two have the strongest track record: mindfulness-based practices and cognitive behavioral therapy (CBT). You can think of them as brain workouts that rewire trigger-response loops between emotion centers and motor neurons.
Mindfulness Techniques
Mindfulness is not just incense and vague positivity. It is the skill of noticing thoughts and body sensations without judgment. Magnetic resonance imaging studies show that regular mindfulness meditation dampens amygdala activity, the brain's alarm bell. Less alarm equals lower sympathetic tone, which in turn relaxes jaw muscles.
Practical moves include:
- Body scan before bed: Lie down, breathe slowly, and mentally sweep attention from toes to scalp. When you hit the jaw, consciously unclamp it. Over time your nervous system learns that relaxation cue and reproduces it during sleep.
- 4-7-8 breathing: Inhale for 4 counts, hold for 7, exhale for 8. Research from the Mayo Clinic suggests the pattern can drop heart rate and blood pressure within minutes.
- Mindful chewing: During meals, set your fork down between bites and focus on flavor instead of rushing. This resets habitual clenching loops that sometimes spill into nocturnal grinding.
Consistency matters. The literature points to a minimum of eight weeks of daily practice for measurable results, mirroring protocols in mindfulness-based stress reduction (MBSR) programs.
Cognitive Behavioral Therapy (CBT)
CBT unpacks dysfunctional beliefs and replaces them with reality-based narratives. For bruxism, the dysfunctional belief might be "I must power through this report, even if my jaw is throbbing." A CBT therapist guides you to recognize the early mouth tension and intervene with micro-breaks or self-talk like "Jaw is tight; quick stretch now."
In Matheson's 2023 review, CBT earned a "moderate" strength of recommendation for TMD pain reduction. While the paper did not isolate bruxism alone, the overlap in muscle groups and pain pathways suggests comparable benefit. Insurance coverage varies, but many therapists offer telehealth sessions, shrinking cost and commute barriers. A typical course is six to twelve weekly sessions paired with homework exercises.
Bottom line: mastering your stress response is not kumbaya fluff. It is neurologically grounded muscle rehab that can lower clenching frequency and intensity, especially in mild to moderate cases.
Botox as a Non-Invasive Treatment
Botulinum toxin type A, best known for erasing forehead lines, works by blocking acetylcholine release at the neuromuscular junction. Less acetylcholine means weaker muscle contractions. For jaw muscles locked in a nightly CrossFit session, that can be game-changing.
Henien et al. 2025 followed 118 patients with temporomandibular myofascial pain treated with Botox. Participants received 25 to 50 units targeted into the masseter and sometimes temporalis muscles. Pain scores dropped 47 percent on average at one month and remained lower than baseline for at least three months. Adverse events were mild—mostly injection-site soreness or temporary chewing fatigue.
Procedure snapshot:
- Consultation: A maxillofacial surgeon or dermatologist assesses jaw size, muscle bulk, and bite alignment. Photos track changes.
- Injection day: The clinician marks points along the muscle belly, cleans skin, and inserts a fine needle. Each side takes roughly 2 minutes.
- Post-care: No massaging the area or strenuous chewing for 24 hours. Full effect kicks in at around 10 days.
Pros and cons:
- Pros: Rapid pain relief, visible reduction in hypertrophic jawlines, minimal downtime.
- Cons: Temporary (3-4 months), repeat costs, potential smile asymmetry if toxin diffuses into zygomatic muscles.
The American Dental Association notes that off-label Botox use for bruxism is rising, but practitioners should employ ultrasound or electromyography guidance to improve placement accuracy. If you crave a guard-free night yet need a predictable fix, Botox is worth a chat with a qualified clinician.
Exploring Electrical Stimulation Devices
Contingent electrical stimulation (CES) devices are wearable gadgets that train jaw muscles the way a smart watch nudges you to stand. The star of the show is GrindCare®, a forehead-mounted sensor that detects masseter EMG spikes. When it senses clenching, it delivers a micro-pulse to the trigeminal nerve branch. The pulse is not painful; users describe it as a gentle tap that prompts the brain to relax the jaw.
Sladeckova et al. 2025 explored CES during full-mouth rehabilitation in heavy grinders. Over eight weeks, CES reduced nocturnal muscle activity by 67 percent compared with baseline. Importantly, the reduction persisted for two weeks after stopping treatment, hinting at neuromuscular re-learning.
How GrindCare® works:
- An adhesive patch positions the sensor on the temple before sleep.
- The device calibrates to your individual EMG threshold in the first night.
- During subsequent nights, it issues sub-sensory pulses each time activity tops that threshold.
- Data syncs to an app so you can track progress in graph form—handy for biohackers.
Clinical pearls:
- Expect adaptation: some users need a week to stop noticing the pulses.
- Electrodes must be replaced every 2-3 uses, which adds cost.
- Contraindications include epilepsy or implanted electrical devices like pacemakers.

While CES is not a cure-all, it takes the crown for people who love tech toys and want an option they can turn on and off as needed. Combine it with mindfulness for a one-two punch: software prompts plus human self-awareness.
Repetitive Transcranial Magnetic Stimulation (rTMS)
rTMS uses focused magnetic fields to modulate neuronal firing in targeted brain regions. Originally developed for depression, it is now tested for sleep disorders and chronic pain.
Lanza et al. 2023 reviewed rTMS across primary sleep disorders, including preliminary work on sleep bruxism. Low-frequency (1 Hz) stimulation applied to the motor cortex reduced jaw-closing muscle activity by up to 39 percent in pilot trials. The therapy likely works by down-regulating hyperexcitable corticobulbar pathways that drive the masseter during micro-arousals.
What an rTMS session looks like:
- You sit in a reclining chair wearing earplugs (for coil clicking sound).
- A figure-of-eight coil positions over the primary motor cortex face area, mapped via neuronavigation.
- Trains of pulses (e.g., 1200 pulses, 1 Hz) fire for about 20 minutes.
- You feel a rhythmic scalp tapping but no pain.
Advantages:
- Non-invasive, no needles.
- Effects can last weeks to months after a short treatment course.
Limitations:
- Costly, with limited insurance coverage.
- Accessibility mainly in major academic centers.
- Still experimental for bruxism; larger randomized trials are pending.
If you already seek rTMS for depression or insomnia, ask whether adding a bruxism protocol is possible. Otherwise, you might wait until the evidence matures.
Diet and Lifestyle Changes for Bruxism Relief
Nutrition and daily habits play quieter but crucial roles in jaw health. What you sip at 4 pm may determine how calm your masseters are at midnight. Shafiee and Nourizadeh’s 2025 narrative review highlights lifestyle adjustments as first-line strategies, particularly for patients with dental implants who cannot tolerate guard pressure.
Avoiding Stimulants
Caffeine: Coffee, energy drinks, and dark chocolate all crank up central nervous system arousal. In sensitive individuals, caffeine has a half-life of up to nine hours. If you down a large latte at 3 pm, a quarter of that caffeine is still partying in your bloodstream at midnight, keeping jaw muscles twitchy. Learn more about the effects of caffeine on bruxism.
Alcohol: While booze feels sedating, it fragments REM sleep later in the night and increases sympathetic surges that correlate with bruxism episodes. Swap late-night cocktails for herbal tea laced with magnesium-rich cacao nibs, which some small trials suggest can relax muscle fibers. Explore how alcohol impacts teeth grinding.
Incorporating Relaxation Techniques
Beyond mindfulness, simple home practices can buffer your system against nightly clenching:
- Warm compress: A microwaved moist towel over jaw joints for 10 minutes before bed loosens connective tissue. Cleveland Clinic therapists recommend pairing heat with gentle side-to-side jaw glides.
- Yoga or tai chi: Slow, low-impact movement lowers cortisol and improves proprioception, teaching you to notice tension early.
- Magnesium glycinate supplementation: Although human bruxism trials are scarce, magnesium supports neuromuscular relaxation and boasts a benign safety profile. Discuss dosage with your clinician, especially if you have kidney issues. Consider reviewing the role of magnesium in teeth grinding.
- Blue-light hygiene: Screens delay melatonin, which can delay deep sleep onset and prolong the light sleep stages where bruxism spikes. Use a screen filter after sunset or, better, stash the phone in another room.

Finally, keep an eye on micronutrient balance if you adhere to restrictive diets. Low calcium or vitamin D can impair neuromuscular function. A quick blood test through your primary care provider helps catch deficiencies early.
Conclusion: Embracing Natural Bruxism Solutions
You now have a buffet of guard-free options, from calming your mind with mindfulness apps to persuading your jaw with well-placed Botox or smart electrical pulses. Not every tool fits every mouth. Some folks tame grinding with simple caffeine curfews and body scans, while others need the muscle-chilling power of Botulinum toxin A. The common thread is listening to your nervous system and picking interventions that respect your lifestyle and risk tolerance.
Start small: ditch the 5 pm espresso, test a guided meditation, and track morning jaw tension in a journal. If clenching persists or pain escalates, layer on additional strategies like CES or a professional CBT program. Mouth guards still have their place, but they no longer own the entire field. With evidence growing in peer-reviewed journals and tech innovations hitting the market, you can manage bruxism on your terms—plastic optional.