Understanding the Link Between Stress and One-Sided Jaw Pain
Explore how stress contributes to one-sided jaw pain and ways to manage it, focusing on jaw tension and related symptoms.

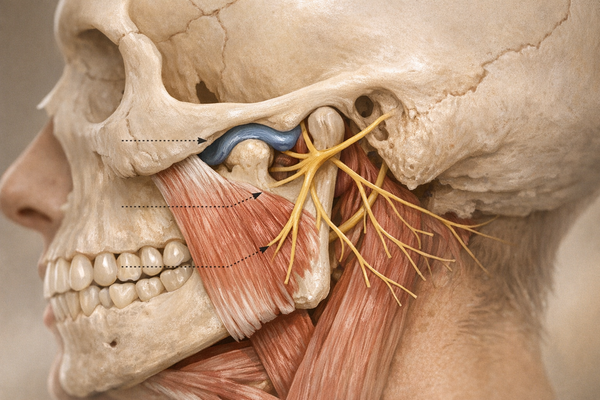
You might clench your jaw during rush-hour traffic and notice a dull throb behind one ear, dismissing it as “just stress.” That shrug is understandable but not entirely accurate. Research shows that psychological stress can affect your masseter muscles, leading to one-sided jaw pain that persists. In other words, what happens in your head often manifests physically.
This article compiles key evidence on stress, jaw tension, bruxism, and temporomandibular disorders (TMD). You'll get the lab data, plain-language explanations, and practical tips you can use tonight. Ready to unclench? Let’s dig in.
The Link Between Stress and Jaw Pain
Stress is a biological response meant to keep you alive when faced with threats. Your brain releases cortisol and adrenaline, priming muscles to react quickly. The downside? Daily stressors keep those muscles tense when they should be relaxed.
Several studies connect psychosocial stress to jaw pain. A 2019 review by Jochum and colleagues, published in 2019, found that people with high anxiety or life stress showed higher levels of jaw muscle tension, or myoarthropathy. They used surface electromyography to show that masseter and temporalis muscles remain tense even at rest.
A large epidemiological study, Pain, Stress and Mental Well-Being Over Three Generations, tracked over 4,000 participants. Researchers discovered that parents with chronic stress not only reported more one-sided jaw pain but also had children who developed similar complaints by adolescence.
Why one side specifically? Habitual behaviors often favor your dominant chewing side. When stress leads to subconscious clenching, the stronger side does more work. Over time, this asymmetry results in local inflammation and micro-trauma, causing pain on one side. To further understand how posture can exacerbate these issues, explore the link between posture and jaw pain.
You might wonder if stress can truly explain sharp pain near your ear. The answer is yes. Tension knots muscle fibers, reduces blood flow, and compresses tiny nerves near the temporomandibular joint. Less oxygen and irritated nerves result in pain. Left untreated, this cycle of pain and stress can become unending.
Muscular Tension in Stress-Related Jaw Issues
- Cortisol spikes increase baseline muscle tone.
- Prolonged contraction leads to micro-tears and trigger points.
- Nociceptors (pain sensors) in the jaw become hypersensitive.
- One-sided chewing habits magnify the imbalance.
If your smartwatch thinks you're working out while sitting, imagine what your jaw muscles endure all day.
Understanding Bruxism and Its Impact
You may have heard dentists mention “bruxism,” which means grinding or clenching teeth, often unconsciously. Bruxism comes in two types: awake (daytime) and sleep (nighttime). Both are sensitive to stress and can result in sharp pain when opening your mouth, often more pronounced on one side. For more on how stress and anxiety can trigger nighttime episodes, read about stress-induced teeth clenching.
Symptoms and Diagnosis
Tooth grinding might be compared to a wood chipper by your bed partner. However, many grinders are silent. Common signs include:
- Morning jaw stiffness or soreness, often unilateral
- Clicking or popping when yawning widely
- Flattened, chipped, or loose teeth
- Sensitivity to hot or cold due to enamel wear
- Tension headaches near the temples
Diagnosis usually comes from a dentist who notices wear patterns or from wearable electromyography devices during sleep studies. In children, sleep studies show rhythmic bursts of activity, according to a 2024 narrative review by Leung et al.. The same markers appear in adults, just more intensely.
Bruxism and Stress
Jochum’s 2019 analysis found a strong link between muscle activity, emotional distress, and jaw pain. Stress does not just coexist with bruxism; it intensifies it. Elevated cortisol correlates with more intense grinding episodes, especially during early REM sleep when muscle inhibition is low.
Think of your brain as an overzealous security guard. Each random thought (Did I pay that bill?) triggers the jaw muscle. You wake up unaware, but your jaw feels like it bench-pressed its own weight.
One-sided jaw pain occurs because grinders often favor one temporomandibular joint for leverage. Overuse builds lactic acid on that side, like a runner always circling a track the same way. For more on identifying if your jaw pain is linked to bruxism, check out key indicators of bruxism.
In short, stress drives bruxism, bruxism strains your jaw, and pain favors the side with the most activity.
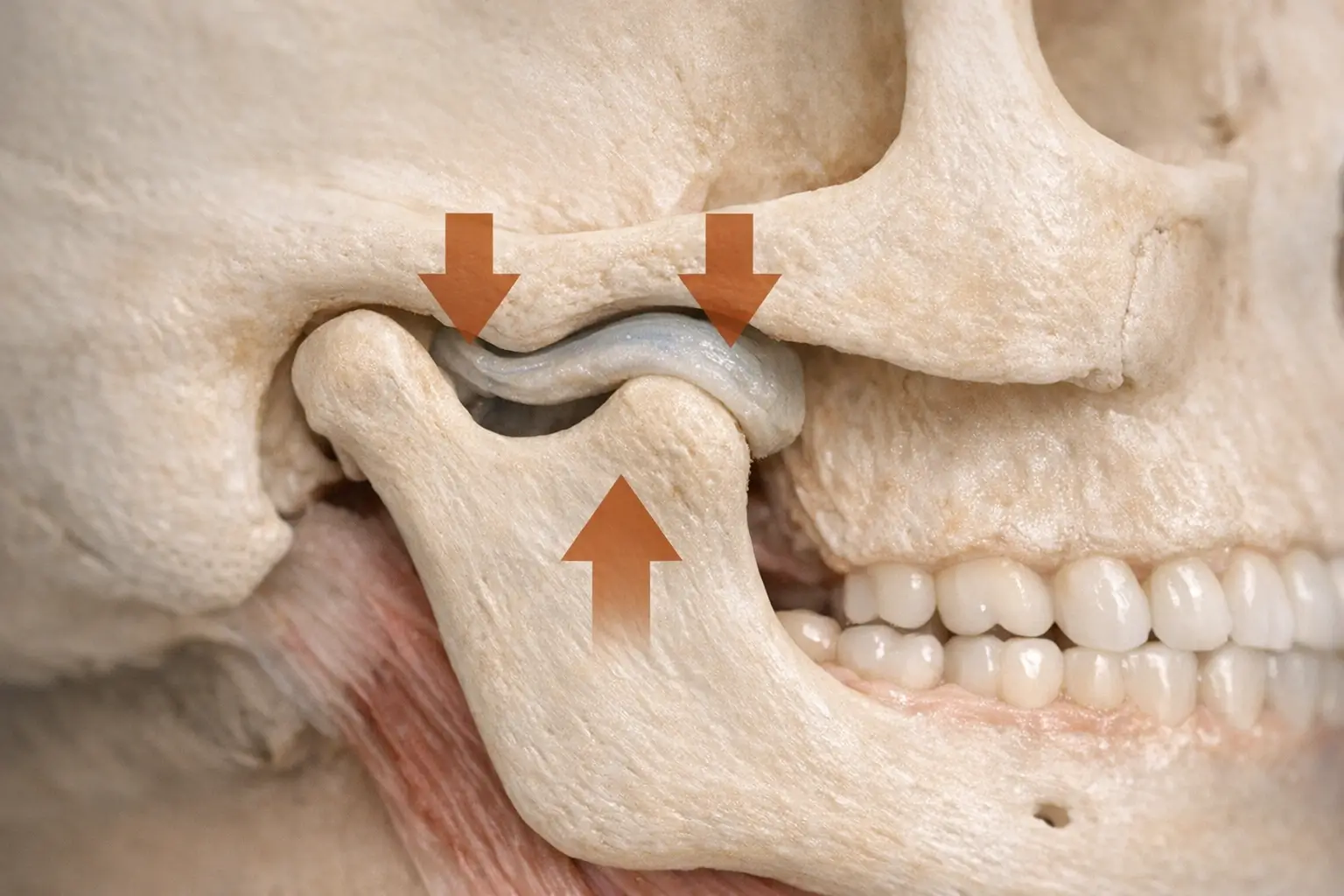
Temporomandibular Disorders (TMD): A Closer Look
Temporomandibular disorders (TMD) refer to issues affecting the jaw joint, chewing muscles, and ligaments. Think of TMD as the cranky landlord of your jaw apartment. It decides when things creak or rattle.
Symptoms of TMD
- Persistent pain under the ear or jawbone, often on one side
- Jaw locking or limited range of motion
- Clicking or grinding sounds in the joint during chewing
- Referred pain to the neck, shoulders, or ears
- Frequent headaches originating at the jaw hinge
The OPPERA (Orofacial Pain: Prospective Evaluation and Risk Assessment) studies provide key insights into TMD. Over a decade, researchers followed thousands of adults, recording psychological, genetic, and biomechanical data. Their findings, detailed in Slade et al., 2016, show that individuals with high-stress scores were more than twice as likely to develop painful TMD compared to low-stress peers.
The Role of Stress in TMD
Stress triggers a triple threat:
- Muscle hyperactivity causes micro-trauma and inflammation in the joint capsule.
- Altered pain processing in the central nervous system lowers your threshold, making normal chewing painful.
- Behavioral changes like poor posture or jaw tensing become ingrained habits.
OPPERA researchers found that cortisol metabolites in saliva predicted first-time TMD flare-ups. Stress hormones can forecast jaw pain like dark clouds predict rain. For effective ways to manage jaw pain, explore jaw pain relief for TMJ.
TMD often affects one side because the joint structure is naturally asymmetric. Disk displacement or inflammation on one side can cause localized pain under the corresponding ear.
Physiological Mechanisms: How Stress Affects the Jaw
We've covered the “what.” Now for the “how.” Stress affects the jaw through neuromuscular pathways and psychosomatic loops. Let’s break it down.
Muscle Activity and Jaw Pain
Surface EMG studies, like those by Stanisic et al., 2025, show that jaw-closing muscles fire more often and at higher amplitudes in stressed individuals. This constant readiness squeezes blood vessels, limiting oxygen and causing ischemic pain. Imagine flexing your bicep all day. Eventually, it burns. Now transfer that to your masseter during work.
Jochum’s 2019 paper shows that bruxers have upregulated sympathetic nervous system activity, evidenced by higher heart rates during clenching. Stress keeps the sympathetic dial turned up, and jaw muscles follow suit.
Psychosomatic Factors
“Psychosomatic” means mind-body. Chronic stress changes how your brain processes sensory input. Pain pathways become sensitized, making harmless jaw movements feel threatening. Functional MRI scans in OPPERA participants showed hyperactivity in the anterior cingulate cortex, linked to emotional interpretation of pain.
Stress can also reduce salivary flow. A dry mouth creates friction on soft tissues, which your brain may interpret as discomfort, adding another layer to the pain.
Consider posture. Stress often rounds shoulders and thrusts the head forward, changing how the mandible sits in its socket. Even a slight misalignment repeated thousands of times can overload one side of the joint. For natural ways to relieve stress-induced jaw tension, explore stress-free solutions for jaw tension.
Simple Ways to Manage Stress-Induced Jaw Pain
No single solution can eliminate stress or TMD. You need a toolbox. Below are science-backed strategies that address the problem from multiple angles.
Lifestyle Changes
- Sleep hygiene: Consistent bedtime, dark room, and no doom-scrolling can decrease nocturnal bruxism. Studies link fragmented sleep to higher muscle activity, so solid sleep is crucial. For more on how sleep quality affects jaw pain, see how sleep positions impact bruxism.
- Limit caffeine and alcohol: Both increase sympathetic activity and can intensify grinding, especially after 6 p.m.
- Exercise, but not jaw exercise: Whole-body cardio reduces cortisol, according to the American Psychological Association’s stress management guidelines. Leave chewing gum behind to avoid overworking your jaw.
- Anti-inflammatory diet: Foods rich in omega-3s combat micro-inflammation within the TMJ. Think salmon, walnuts, and flaxseed. Learn more about dietary influences in how your diet affects bruxism.
Relaxation Techniques
Experiment with different approaches. Some may work wonders, while others might not. That’s normal.
- Progressive muscle relaxation (PMR): Tense and release muscle groups from toes to scalp, ending with the jaw. PMR reduced clenching frequency in a pilot trial cited by Mayo Clinic’s TMJ resource.
- Guided biofeedback: Wearable devices buzz when your masseter tightens past a threshold, providing real-time cues to relax. Discover more about biofeedback devices for bruxism management.
- Mind-body therapies: Hippotherapy—horse-assisted therapy—showed reductions in bruxism intensity in a 2025 study by Geibel et al.. The rhythmic motion of riding appears to calm the autonomic nervous system.
- Box breathing: Inhale for four counts, hold four, exhale four, hold four. This Navy-SEAL approved method tempers adrenaline spikes and can be done at your desk before a meeting.
Consistency beats perfection. Ten minutes daily of any relaxation practice is better than a longer session once a month.
When to Seek Professional Help
DIY methods are good first steps, but sometimes professional help is needed. Here’s when to seek it:
- Pain intensity is 6 or more on a 10-point scale for over a week.
- Jaw starts locking, or you cannot open wider than two finger widths.
- Ear pain persists and radiates along the jawline, ruling out infection.
- Headaches increase after minor jaw movements.
A dentist or orofacial pain specialist will likely start with imaging—like panoramic X-rays or MRI—to rule out structural issues. For persistent cases, oral appliances such as stabilization splints can redistribute bite forces. The OPPERA cohort showed that early intervention with custom splints reduced pain scores by 30% within three months.
If trauma triggered your jaw pain, combined protocols may be required. Young adults with post-traumatic headaches sometimes develop jaw dysfunction as a comorbidity, discussed in Kothari et al., 2022. Neurology, physical therapy, and cognitive behavioral therapy each address a part of the pain.
Lastly, consider mental health professionals. Chronic stress rarely resolves on its own. A psychologist can teach coping mechanisms that reduce the stress fueling your jaw problems.
Conclusion
Jaw pain on one side is not just random bad luck. Stress acts like an invisible puppeteer, affecting your masseter muscles, triggering bruxism, and inflaming the temporomandibular joint. Evidence from myoarthropathy research to the large-scale OPPERA studies confirms that mind and mandible are connected—when one is tense, the other feels it.
The good news: you have multiple levers to pull. Lifestyle changes, relaxation techniques, and early professional guidance can break the cycle. Managing stress sooner helps your jaw clock out from its overtime shift. In the long run, caring for your mental well-being benefits not just your peace of mind but also pain-free chewing and talking. Give your jaw a break. It has enough work already.