How to Identify Bruxism in Kids: Early Signs and Symptoms
Discover early signs of bruxism in children and learn how to identify symptoms of kids teeth grinding.

If you've ever tiptoed into your child’s bedroom and heard a sound like sandpaper wrestling, you might suspect bruxism—the clinical term for grinding or clenching teeth. While the noise can make any parent cringe, the bigger concern lies beneath the enamel. Childhood bruxism can carve grooves into both baby and adult teeth, disrupt jaw development, and affect sleep quality. The good news is that recognizing it early is crucial, and the science on identifying bruxism has become robust.
This article serves as your research-backed guide to pediatric bruxism. We'll simplify clinical jargon, incorporate the latest findings, and provide practical steps to address the issue.
Understanding Pediatric Bruxism
Pediatric bruxism refers to repetitive jaw-muscle activity that results in tooth grinding or clenching in those under 18. It manifests in two forms: awake bruxism (during the day) and sleep bruxism (at night). Most children grind their teeth at night, making it easy to overlook unless you're vigilant.
The condition isn't rare. According to a 2024 review by Leung et al., prevalence ranges from 14 to 20 percent in kids, although estimates vary depending on definitions and measures. A broader review by Al-Jewair and colleagues in 2026 places the global average around 18 percent, cautioning that parental self-reports may undercount quieter clenchers.
Persistent bruxism can:
- Wear down enamel, exposing sensitive dentin
- Trigger temporomandibular joint (TMJ) pain and clicking. For more on TMJ pain relief, you might find our article on jaw pain relief strategies useful.
- Increase the risk of cracked fillings or fractured baby teeth
- Disrupt sleep, leading to daytime sleepiness and mood swings
- Set the stage for malocclusion, complicating future orthodontic treatment
The consequences are real. The Al-Jewair review indicates enamel loss in up to 60 percent of pediatric grinders, with 20 percent eventually experiencing chronic jaw pain. Ignoring the issue isn't an option.
Common Signs and Symptoms of Bruxism in Children
Detecting grinding early involves observation and listening. While asleep, children usually don't notice their own noise, making you the primary detector. Here are evidence-backed signs to watch for:
- Audible grinding or clicking during sleep
The unmistakable sound often prompts clinic visits. In the Leung review, over 80 percent of diagnosed cases had a parent report nightly noise. - Morning jaw or facial pain
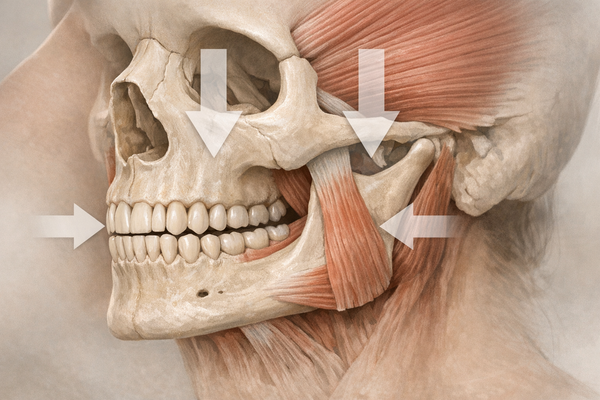
Grinding stresses the masseter and temporalis muscles. Kids may say their cheeks feel "tired" or that yawning hurts. This can be similar to adults who experience jaw pain related to stress. - Headaches after waking
Muscle tension can radiate upward. A study by Zhang et al. in 2025 found children with sleep bruxism were twice as likely to experience morning headaches compared to non-grinders. - Worn or flattened tooth surfaces
Dental exams may reveal shiny facets on molars or shortened edges on front teeth before pain arises. - Tooth sensitivity to cold
When enamel thins, nerves become sensitive. Kids might avoid cold foods or drinks without saying why. - Cheek biting or tongue indentations
Chronic pressure can create scalloped borders or small ulcers inside the mouth. - Restless sleep and frequent awakenings
Grinding episodes often occur during lighter sleep stages, disrupting rest. Parents report tossing, turning, or mild snoring.
While none of these signs alone confirm bruxism, together they strongly suggest it. If you hear grinding and notice dental wear, there's a high chance of sleep bruxism, closely linked to nocturnal awakenings (Leung et al. 2024).
The Connection Between Sleep Disorders and Bruxism
Is bruxism merely a noisy habit or a symptom of something deeper? Evidence increasingly suggests the latter. For many kids, grinding is part of a larger sleep-disorder picture.
Consider pediatric obstructive sleep apnea (OSA). When throat tissue collapses and blocks airflow, the brain triggers brief awakenings to restart breathing. These arousals coincide with jaw-muscle activity. A 2026 review by H. M. Selvakumar et al. notes that up to 50 percent of children with OSA also exhibit sleep bruxism. The relationship may be bidirectional: airway obstruction can provoke grinding, while jaw motion might help reopen the airway. For those interested in the connection between sleep disorders and bruxism, our article on sleep disorders and bruxism offers more insights.
The connection extends to broader sleep disturbances like night terrors, restless legs syndrome, and insomnia. Zhang et al. (2025) tracked 400 children in a sleep clinic, finding that kids with any sleep disorder were 2.8 times more likely to grind their teeth than healthy sleepers, even after adjusting for age and caffeine intake. The authors propose a shared neurochemical pathway involving dopamine and serotonin, neurotransmitters that affect both arousal and motor activity.
If your child grinds and also snores, gasps, or wakes up sweating, consult a pediatrician about a sleep study. Treating the underlying disorder often reduces grinding. Mayo Clinic’s pediatric sleep center advises that bruxism rarely exists alone (Mayo Clinic).
Beyond breathing issues, factors like anxiety, ADHD, and screen time can elevate arousal thresholds, increasing the likelihood of nighttime clenching. The American Academy of Pediatrics notes that children with over two hours of evening screen time report poorer sleep and are more likely to show bruxism-related wear (AAP). Essentially, anything disrupting restorative sleep can exacerbate grinding.
Diagnostic Approaches for Pediatric Bruxism
Diagnosis involves both art and science, typically beginning in the dental chair.
1. Detailed History
Your dentist or pediatrician will inquire about nighttime noises, jaw pain, headaches, snoring, and stress levels. Since children often under-report pain, clinicians rely heavily on parental observations (Leung et al. 2024).
2. Clinical Examination
The dentist looks for wear patterns, fractures, or gum recession. They also palpate jaw muscles for tenderness and check the TMJ for clicking or limited motion. According to Al-Jewair’s 2026 review, standardized indices like the Tooth Wear Index can quantify severity, though not widely used in pediatric practice.
3. Parafunctional Screening
Kids may unconsciously chew pencils or bite nails. Noting these habits helps form a more complete behavioral picture. For more on similar habits, consider reading about unconscious jaw clenching.
4. Sleep Questionnaires
Tools such as the Children’s Sleep Habits Questionnaire add structure to parental reports. When results suggest possible OSA, clinicians may recommend overnight polysomnography.
5. Polysomnography (PSG)
The gold standard for diagnosing sleep bruxism uses surface electromyography (EMG) on the jaw to record muscle bursts during sleep stages. While PSG isn't routine for every grinder, it's essential when airway obstruction or neurological disorders are suspected (Selvakumar et al. 2026).
6. Wearable Bite-Strip Devices
New at-home EMG strips can log clenching episodes over several nights. They're less precise than PSG but more affordable, making them a reasonable screening tool.
In short, most cases are diagnosed based on clinical examination and parent reports. Advanced sleep studies are reserved for severe cases or when coexisting conditions are suspected.
Management and Treatment Options
Treatment for bruxism often involves a combination of behavioral adjustments, dental devices, and medical care for underlying issues. Think of it as a personalized anti-grind toolkit.

Behavioral Strategies
Stress reduction
Children experience stress too. Homework, sports, or family tension can increase muscle activity during sleep. Simple coping tools—like deep breathing before bed, journaling, or discussing worries—can lower arousal. The American Dental Association recommends mindfulness exercises for kids, highlighting small pilot studies that reduced self-reported grinding by 30 percent after eight weeks (ADA). For adults, similar strategies can be found in holistic approaches for bruxism.
Sleep hygiene
Consistent bedtimes, a cool, dark room, and a no-screens-before-bed rule help stabilize sleep patterns, reducing grinding. The AAP suggests avoiding caffeine after noon and promoting physical activity earlier in the day. For more on improving sleep quality, explore our article on sleep hygiene and bruxism.
Jaw relaxation techniques
Applying a warm compress to the masseter muscles for 10 minutes before bed can relax tight fibers. Some clinicians teach kids to place their tongue on the roof of the mouth and let the jaw hang slightly open—an easy daytime drill to break clenching habits. For more detailed techniques, our piece on jaw relaxation techniques can be useful.
Dental Interventions
Custom mouthguards (occlusal splints)
A thin acrylic appliance worn over teeth creates a smooth surface, preventing trauma. In a study cited by Leung et al. 2024, nightly splint use reduced enamel wear progression by 70 percent over 12 months. Downsides include cost and potential bite alteration if used long-term without monitoring. To explore more about mouthguards, read our comprehensive guide on choosing the right bruxism mouth guard.
Intermittent splint schedule
Some dentists suggest wearing the guard every other night to maintain bite equilibrium while protecting enamel. Your child’s growth stage and orthodontic risk will guide the schedule.
Orthodontic correction
Crowded teeth and overbites can create abnormal contact points that trigger grinding. Early orthodontic interventions, like palatal expanders, may reduce bruxism by harmonizing the bite.
Medication (rare)
Short-term muscle relaxants are sometimes prescribed for older teens with acute jaw pain, but they're not first-line for younger kids. A 2024 review by Conti et al. cautions that pharmacologic options lack robust pediatric data.
Treat underlying sleep disorders
If PSG confirms OSA, interventions like adenotonsillectomy or CPAP can significantly reduce grinding events (Selvakumar et al. 2026).
When to Seek Professional Help
Not every instance of tooth grinding requires immediate attention, but certain scenarios should prompt you to seek help:
- Grinding sounds persist more than three nights per week for over a month
- Your child wakes up with jaw pain, earaches, or regular headaches
- You notice chipped enamel, flattened tooth surfaces, or gum recession
- Snoring, gasping, or breathing pauses accompany grinding
- Daytime sleepiness, irritability, or concentration difficulties appear. These could also be signs of bruxism-related issues.
Al-Jewair’s 2026 review emphasizes early referral to a pediatric dentist to prevent significant dental damage. Meanwhile, Selvakumar’s OSA review warns that ignoring airway issues may prolong sleep disruption and grinding.
Your first step is usually the family dentist, who may involve a sleep specialist, ENT, or behavioral therapist depending on findings. Early multidisciplinary care is more effective than a wait-and-see approach.
Conclusion
Pediatric bruxism sits at an intersection of dentistry, sleep medicine, and child psychology. Research indicates that up to one in five children will grind or clench their teeth. While many will outgrow the habit, a significant number risk cracked teeth, TMJ problems, and sleep disruption.
The path forward is straightforward: listen for nighttime noises, watch for dental wear and morning headaches, and monitor overall sleep quality. Clinical exams and, when needed, sleep studies refine the diagnosis. From there, combine behavioral adjustments, mouthguards, and treatment of any underlying sleep or bite issues.
Acting early makes it easier to protect both teeth and sleep. A little vigilance today can save enamel and sanity tomorrow.