Decoding Jaw Pain: Could Stress Be the Culprit?
Explore if stress causes jaw pain and how to relieve it. Learn about jaw tension linked to anxiety.

If you've ever woken up with a sore jaw or noticed your teeth clenching during a stressful work call, you're not alone. Researchers have been investigating the link between mental stress and jaw pain for decades. Thanks to new imaging tools and large-scale studies, we now have a clearer picture. Stress could be the culprit behind your jaw tension.
Fortunately, you can understand these signals and take action. Here's the current science in plain language, along with a guide to giving your jaw muscles a break.
Understanding Jaw Pain and Its Connection to Stress
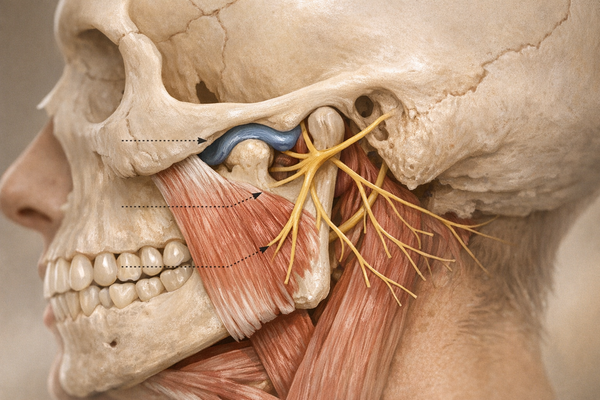
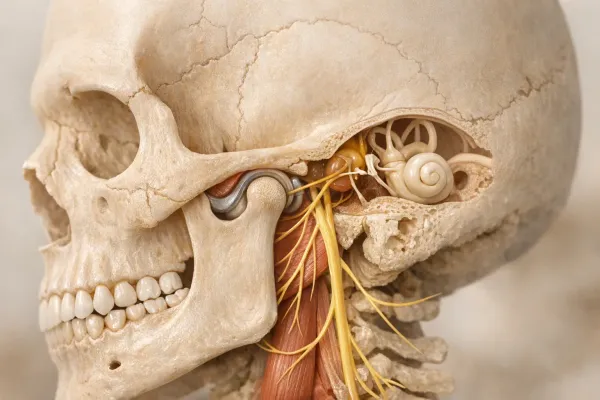
Jaw pain often falls under a broader category called temporomandibular disorders (TMD). The temporomandibular joint is the sliding hinge that lets you talk, yawn, and chew. When it's strained, you might feel aching near the ear, hear clicking sounds, or experience headaches and ear fullness unrelated to infection. This condition can sometimes be exacerbated by stress and anxiety, which are common triggers.
Many patients first visit an ear-nose-throat specialist because the ache mimics an ear problem. One U.S. survey of 1,800 otolaryngology referrals revealed that 12% were redirected to dental specialists for hidden TMD. This overlap shows how easy it is to misidentify the cause if stress and jaw mechanics aren't considered early.
How common is it? A massive German study, part of the NAKO Health Study, found that TMD symptoms affect roughly one in four people. Researchers like Herpel and colleagues didn't just count cases. They identified chronic stress, anxiety, and poor sleep as major risk factors.
These psychological factors keep appearing. A review by Saini et al. confirmed that high stress nearly doubles the odds of jaw pain, with anxiety worsening it. The takeaway: if your mind is racing, your jaw muscles might be too.
Symptoms linked to stress-driven TMD include:
- Aching or stiffness in the jaw on waking
- Headaches that feel like a tight band around the temples
- Clicking or grating noises when you chew or open wide
- Difficulty opening the mouth fully
- Facial pain that flares during stress
If these aches persist, they can affect your social life, disrupt sleep, and lead you to a soft-food diet. Identifying the stress link early is crucial. For more insights on this, you might want to explore natural jaw tension relief methods.
How Stress and Anxiety Manifest as Jaw Tension
Stress originates in the brain but doesn't stay there. When you perceive a threat—like a tense email—the hypothalamus activates the sympathetic nervous system. Heart rate rises, breathing quickens, and muscles across the body tighten. Your jaw muscles, especially the masseter and temporalis, are major players in this tension.
Picture a typical workday: your inbox pings, the Zoom camera lights up, and without noticing, you hold your breath and clench your teeth. Multiply that by eight hours, and you've got a stress workout focused on your face.
Animal research has traced this process. A study by Zhao et al. explored a signaling loop from the amygdala—your brain’s fear hub—to the trigeminal motor nucleus. Stress increased firing along this pathway, creating measurable jaw tension even at rest.
Humans show a similar pattern, measured by electromyography. Chronic clenching fatigues muscles, restricts blood flow, and sensitizes pain nerves. This is often seen in conditions like anxiety-induced nighttime teeth clenching.
Psychological and Physiological Pathways
Psychology plays a key role. Traits like high neuroticism or perfectionism can intensify muscle tension. Hekmati et al. found a correlation between anxiety scores and masseter muscle activity. Stress hormones like cortisol also lower pain thresholds, making normal chewing feel painful.
Caffeine, deadlines, and doom-scrolling can exacerbate this stress. In one trial, participants who consumed caffeine before a math task showed increased jaw tension compared to a decaf control. Translation: that extra latte might be fueling your jaw workout.
If you have generalized anxiety, these pathways rarely settle. Over time, the jaw's cushioning disk may slip, cartilage can wear, and inflammation can create mechanical issues in addition to muscle pain.
The Role of Bruxism: Grinding and Clenching Under Stress
Bruxism is the term for grinding or clenching your teeth, often without noticing. It can occur while awake or asleep, and stress influences both forms. This condition is closely related to jaw pain and bruxism.
Awake and Sleep Bruxism
Awake bruxism often occurs during focused activities like coding or studying. You might catch yourself clenching or chewing your cheek. Although you're awake, your brain is busy, making it hard to control. A simple reminder like a sticky note saying "Lips together, teeth apart" can help break the habit.
Sleep bruxism is more elusive. It shows up as rhythmic bursts of muscle activity. A study by Chung et al. found that PTSD-related nightmares increase nocturnal grinding. Wearable sleep devices can detect these bursts, providing valuable data for you and your dentist.
A review by Leung et al. noted the same stress connection in children. The behavior is ageless, and sleep doesn't shield against it. For children specifically, the article on pediatric bruxism can offer more insights.
Bruxism wears down enamel and strains muscles, causing morning stiffness or midday pops. If your jaw feels worked out without your consent, you might be dealing with sleep bruxism.

Impact of Jaw Pain on Quality of Life
Chronic jaw pain isn't just a nuisance; it can severely impact quality of life. It complicates nutrition as chewy and crunchy foods become difficult, leading to a reliance on softer foods that may lack nutrients.
With the rise of remote work, constant snacking can exacerbate the pain cycle by giving the jaw little rest. The social aspect is also affected, as speaking can aggravate the joint, making long conversations uncomfortable.
A meta-analysis by Cayrol et al. found reduced pain thresholds in the face and neck, making sufferers withdraw from physical interactions. The feedback loop of anxiety and pain, highlighted by Saini et al., shows the importance of addressing psychological factors in TMD treatment. For those interested in exploring solutions, biofeedback therapy might offer a promising approach.
Common impacts reported by patients include:
- Difficulty concentrating due to facial pain
- Sleep disruption from grinding sounds or discomfort
- Lower mood and increased fatigue
- Financial costs from dental treatments and therapy

The chronic nature of TMD can strain relationships, as partners may notice grinding and irritability. Recognizing this ripple effect is key to addressing it.
Effective Strategies to Manage Stress-Induced Jaw Pain
While no magic solution exists, several evidence-based strategies can help manage jaw tension and its underlying causes.
Lifestyle Changes
- Mindfulness or breathing exercises: Five minutes of diaphragmatic breathing can reduce heart rate and jaw tension. Free apps can guide you through this practice.
- Posture checks: Slouching can lead to clenching. Set hourly reminders to align your posture.
- Caffeine moderation: Reduce stimulant intake to see if it eases tension.
- Stretch breaks: Simple mouth-opening stretches can lower muscle tone.
- Bedtime routines: Limit screen time before bed and consider relaxation techniques to reduce nocturnal bruxism.
- Self-massage: Applying pressure to the masseter can reduce pain intensity. For more tips, check out jaw relaxation techniques.
- Hydration: Stay hydrated to prevent muscle cramps and limit alcohol intake, which can provoke clenching.
Consistency is key with these interventions, which are generally low-risk and cost-effective.
Professional Treatments
If self-care isn't enough, consider professional treatments:
- Occlusal splints: Custom night guards protect enamel and reduce grinding damage. Learn more about their benefits in our custom mouth guard guide.
- Physical therapy: Techniques like trigger-point release can restore jaw function.
- Cognitive behavioral therapy (CBT): CBT can lower pain and muscle activity by addressing stress and thought patterns.
- Botulinum toxin injections: In severe cases, injections can temporarily weaken jaw muscles.
- Medication: NSAIDs and low-dose tricyclic antidepressants can reduce pain and improve sleep.
- Dental adjustments: In rare cases, orthodontic work may be needed to correct bite misalignment.
Coordinate care for the best results. Many clinics offer integrated TMD programs that combine different treatments.
When to Seek Professional Help
Don't ignore persistent jaw pain. Seek professional help if you experience:
- Sharp or locking pain that limits jaw movement
- Swelling, fever, or redness around the joint
- Grinding sounds paired with a bone-on-bone sensation
- Tingling or numbness in the face
- Frequent headaches despite over-the-counter medication
- Cracked or loosening teeth from grinding
Early assessment can prevent chronic pain syndromes. Many providers offer telehealth options for initial screenings.
Conclusion: Taking Control of Your Jaw Health
Your jaw is more than a tool for eating; it's an indicator of your emotional state. Stress, anxiety, and poor sleep can increase muscle tension, creating a cycle of pain and clenching. Understanding this link—supported by diverse scientific research—can guide you in addressing the issue.
By managing stress and caring for your jaw, you can reverse the cycle. Start with lifestyle changes, seek professional help if needed, and monitor your progress. Your jaw will thank you, and you may find the rest of your body relaxing in response.