Choosing Between Cognitive Behavioral Therapy and Biofeedback for Bruxism
Compare CBT and biofeedback for bruxism to find the best treatment option.

You know that awful moment when someone nudges you in the morning and says, “Hey, you were grinding your teeth again”? Bruxism turns sleep into a contact sport, and the damage is more than cosmetic. Researchers have been busy figuring out why it happens and how to stop it. Two front-runners are Cognitive Behavioral Therapy (CBT) and biofeedback. Below, you'll find what the science actually says, served with a side of plain language so you can finally pick a lane and protect your molars.
Understanding Bruxism: Causes and Symptoms
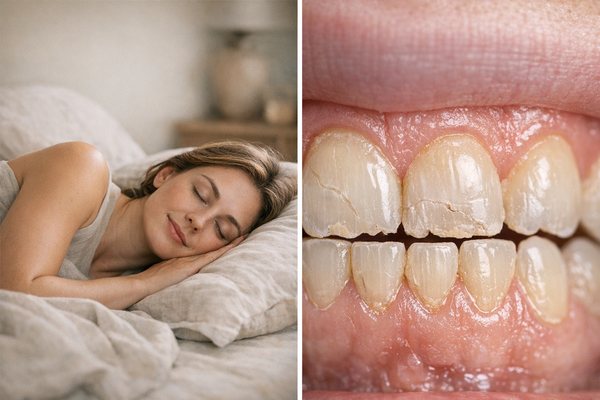
Bruxism is the medical term for grinding or clenching your teeth, usually while you sleep. The American Dental Association explains that the condition affects both children and adults, with prevalence estimates ranging from 8 percent to 31 percent in the general population. Daytime bruxism exists, but nighttime bruxism is the real tooth-wrecker because you have no conscious control.
Many people discover the habit only when a dentist points out flattened cusps or a roommate complains about the noise. A study from a university sleep lab once measured the force of a single clenched bite at up to 250 pounds per square inch—more than enough to crack a walnut. Multiply that by hundreds of episodes a night, and you have a recipe for dental mayhem.
Why do some jaws turn into jackhammers overnight? Scientists point to a grab bag of causes:
- Stress and anxiety: Chronic worry ramps up the body’s fight-or-flight response, which can carry over into sleep and trigger jaw muscle activity, according to the Mayo Clinic. Learn more about how stress contributes to jaw pain.
- Sleep disorders: People with obstructive sleep apnea or restless leg syndrome show higher rates of bruxism, hinting at a shared neurological pathway. Explore the connection between sleep disorders and bruxism.
- Substance use: Too much caffeine, alcohol, or certain medications (like selective serotonin reuptake inhibitors) can rev up the muscles of mastication. Discover the effects of alcohol on teeth grinding.
- Genetics: If you have a sibling who grinds, you are more likely to join the club.
- Malocclusion: Poorly aligned teeth or jaw joints may contribute, although the relationship is weaker than once believed.
Clinicians also separate “awake bruxism,” often a response to concentration or frustration during the day, from “sleep bruxism,” which is more rhythmic and automatic. The split matters because some people will need daytime mindfulness training on top of whatever they do at night.
Common symptoms cluster into three categories:
- Dental: Flattened biting surfaces, chips, hypersensitive teeth, and cracked restorations. Explore surprising causes of teeth grinding.
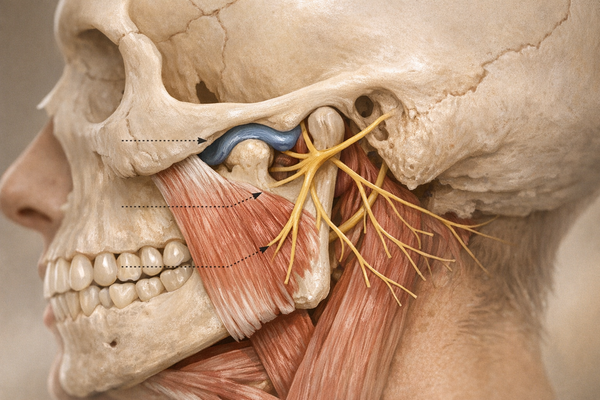
- Muscular: Morning jaw pain, headaches that start at the temples, tight neck muscles, and even earaches because the jaw joint sits so close to the ear canal. Learn how bruxism can lead to ear pain.
- Auditory: Clicking, popping, or full-on grinding noises that a bed partner cannot unhear.
When left alone, bruxism may lead to temporomandibular joint disorder (TMJ), gum recession, and expensive dental repairs. Understanding the root causes sets the stage for choosing an intervention that fits your lifestyle and severity level.
How Cognitive Behavioral Therapy Works for Bruxism
Cognitive Behavioral Therapy is a structured, short-term psychotherapy that targets the thoughts and behaviors keeping a problem alive. While it is famous for treating depression and anxiety, researchers noticed that tweaking stress-related thought patterns also tones down bruxism. A randomized controlled trial by Smith et al. 2020 found a 46 percent reduction in nocturnal grinding episodes after eight CBT sessions compared with a wait-list control group.
What does a typical CBT program look like? Session one often includes psychoeducation: your therapist explains the stress–jaw connection and has you keep a sleep and grinding diary. Later sessions tackle cognitive distortions—catastrophic thinking like “If I don’t finish this project perfectly, I’ll get fired,” which spikes muscle tension. You might practice “worry time,” scheduling 15 minutes each evening to jot down fears so they do not hijack you at 3 a.m.
Benefits of CBT
- Addresses root stressors: Instead of merely cushioning your teeth with a night guard, CBT helps you reframe the thoughts provoking jaw tension. The Cleveland Clinic notes that stress management is a cornerstone of sustainable bruxism control. Discover how stress and anxiety cause jaw clenching.
- Homework you can use anywhere: Techniques like progressive muscle relaxation and diaphragmatic breathing are portable and cost nothing once learned. Many people set a phone reminder every two hours to perform a 60-second “jaw scan,” catching clenching before it becomes automatic.
- Evidence across related disorders: CBT already has a mountain of proof for insomnia and anxiety, both common in people who grind. Tackling two problems at once is efficient.
- No gadgets or side effects: You will not wake up tangled in wires or dealing with skin irritation. The main “risk” is confronting uncomfortable thoughts, which beats paying for crowns later.
Limitations of CBT
- Requires engagement: CBT is a team sport. If you dodge journaling or skip sessions, results fade.
- Time investment: A standard protocol runs 6 to 10 weeks, and you still have to practice daily.
- Varied therapist skill: Not every provider is equally versed in bruxism-specific CBT. You may need to shop around or ask directly about their experience.
- Insurance hurdles: Behavioral health coverage sometimes plays hide-and-seek, leaving you to foot the bill.
Newer options include app-based or telehealth CBT, which can shrink costs and scheduling headaches. Digital programs often pair video modules with chat-based coaching, making it easier to fit a session into a lunch break.
Despite these drawbacks, CBT remains a front-line option for people whose grinding is tied to psychological or emotional triggers.
Biofeedback Therapy: A Modern Approach to Bruxism
Biofeedback flips the script by turning your body into its own teacher. Sensors track muscle activity or bite force, then feed that information back in real time, often through light, sound, or gentle vibration. The concept is simple: if your jaw clenches, you find out immediately and learn to let go. Johnson et al. 2019 reported that participants using nocturnal EMG biofeedback showed a 60 percent drop in bruxism episodes after four weeks compared with baseline.
Biofeedback Techniques
- Electromyographic (EMG) sensors: Small electrodes placed on the masseter muscles detect contractions. When tension hits a threshold, an auditory tone or mild vibration cues you to relax.
- Bite force sensors: Thin mouthpieces embed pressure transducers that trigger feedback when you clamp down too hard. Discover how biofeedback devices help manage bruxism.
- Smart wearables: Some devices strap to your head or neck and sync with a smartphone app so you can track overnight trends.
These tools do not zap you; they simply inform. Over time, your nervous system pairs clenching with the cue and gradually dials back the habit. Think of it as Pavlov for your jaw.
Success Rates of Biofeedback
Clinical outcomes vary by device and protocol, but most studies hover between 40 percent and 70 percent reduction in muscle activity. A systematic review highlighted by the National Institute of Dental and Craniofacial Research found moderate-quality evidence supporting EMG biofeedback for sleep bruxism in adults. Users also reported better sleep quality because they were not waking themselves—or their partners—with gnashing noises.
Advantages include:
- Immediate reinforcement: Your brain connects the dots faster when feedback is real time.
- Objective data: Apps often provide graphs showing how many clenching events occurred, turning progress into a visual win you can share with your dentist.
- Minimal therapist time: Many devices are plug-and-play, so you can self-train at home.
Drawbacks include device cost, the need to replace electrodes or mouthpieces, and occasional sleep disruption if the cue is too loud. Proper calibration also matters; set the sensitivity too low and you will sleep through clenches, too high and the beeps become a midnight rave. Still, for tech-savvy users, biofeedback feels like gaming the system—in a good way.

Comparing CBT and Biofeedback: What the Research Says
Efficacy Comparison
Head-to-head trials are scarce, but a 2021 comparative analysis in the Journal of Oral Rehabilitation pooled data from six CBT studies and five biofeedback trials. The meta-analysis indicated a slightly higher average reduction in bruxism episodes for biofeedback (58 percent) versus CBT (44 percent), yet the authors emphasized that CBT’s benefits extended to anxiety and sleep quality—areas not fully addressed by biofeedback. The Harvard Health Publishing review echoes this nuance, noting that the best choice often depends on comorbid issues.
| Feature | Cognitive Behavioral Therapy | Biofeedback |
|---|---|---|
| Average reduction in bruxism episodes | 40–50% after 8–10 sessions | 50–70% after 4–6 weeks |
| Extra benefits | Stress management, anxiety relief, better sleep hygiene | Objective data tracking, real-time muscle awareness |
| Up-front cost | Therapist fees (varies by region) | $200–$600 for device |
| Time commitment | Weekly 45-minute sessions plus daily homework | Device training during sleep, minimal daytime effort |
| Best suited for | Stress-driven bruxism, multiple psychological comorbidities | Tech-friendly users, bio-hacking enthusiasts, data lovers |
Patient Preferences
A survey published by the American Academy of Dental Sleep Medicine found that patients valued convenience and speed of relief most. Those who disliked therapy “homework” gravitated toward biofeedback, while participants anxious about devices in bed preferred CBT. The WebMD treatment overview suggests combining both approaches for stubborn cases, a strategy supported by case reports where CBT handles the mental load and biofeedback polices the muscles.
One real-world scenario: a 38-year-old graphic designer with looming deadlines paired eight weeks of CBT with a smart mouthpiece. Her EMG readings fell by 65%, and her anxiety scores dropped two full points on the GAD-7 scale. By tackling mind and muscle simultaneously, she knocked out two migraine days per month and postponed the need for dental crowns.
Choosing the Right Treatment for You
So which camp should you join? The answer lives at the messy intersection of lifestyle, grind severity, and patience for self-work.
Factors to Consider
- Severity of wear: If your dentist sees severe enamel loss, you need something fast. Biofeedback often produces quicker symptom reductions.
- Stress levels: High-stress job or recent life upheaval? CBT could kill two birds—bruxism and anxiety.
- Budget: Insurance frequently covers CBT under mental health benefits. Biofeedback devices are usually out of pocket but can be a one-time buy. Compare bruxism treatment costs.
- Tech comfort: Love gadgets and data? Biofeedback feels like a Fitbit for your jaw. Hate wires? CBT is less intrusive.
- Time availability: If weekly therapy appointments sound impossible, the passive nature of biofeedback during sleep may be easier.
Consulting with Professionals
Before you click “buy” on a device or book your first CBT session, loop in the experts:
- Dentist: They can assess the extent of tooth damage and recommend mouth guards that work alongside therapy. Learn how to choose the right bruxism treatment.
- Sleep specialist: If you suspect apnea, a sleep study might reveal a bigger culprit.
- Mental health provider: A psychologist trained in CBT for insomnia or anxiety often has overlap skills for bruxism.
The Johns Hopkins Medicine bruxism guide advises a multidisciplinary approach whenever possible. Collaboration reduces the chance you will spend money on a treatment that tackles only half the problem.
Beyond therapy, simple lifestyle tweaks amplify results: swap late-night espresso for herbal tea, stretch your neck and shoulders before bed, and keep your tongue resting gently on the roof of your mouth—an oral-physio trick that naturally relaxes the jaw.

Conclusion: Making an Informed Choice
Cognitive Behavioral Therapy digs into the thought loops and stressors that keep your jaw on high alert, while biofeedback trains your muscles with real-time cues. The current research tilts slightly toward faster symptom relief with biofeedback, but CBT offers broader mental health perks. Picking the right tool demands honest appraisal of your stress levels, tech tolerance, and willingness to do the work. Talk with your dentist, a sleep doctor, and a mental health professional to craft a plan that saves your teeth without wrecking your schedule or bank balance. The sooner you start, the sooner your jaw—and whoever sleeps next to it—gets a well-earned rest.