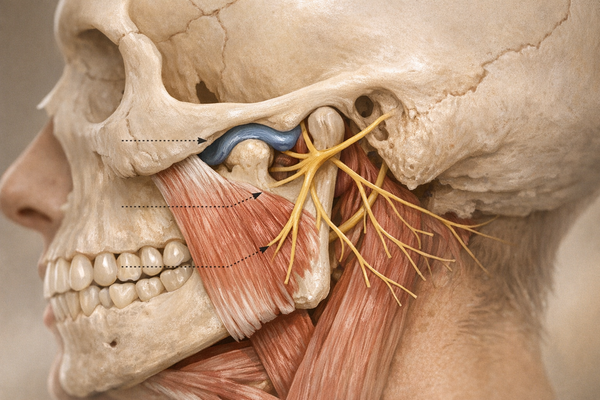
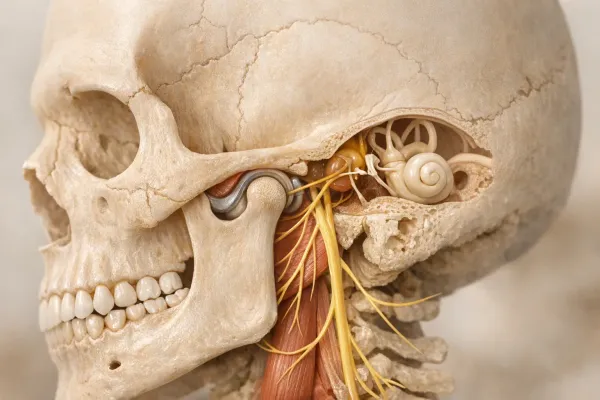
How to Choose the Right Bruxism Treatment: A Comprehensive Guide
Discover the best bruxism treatment options for your needs. Compare and choose wisely.
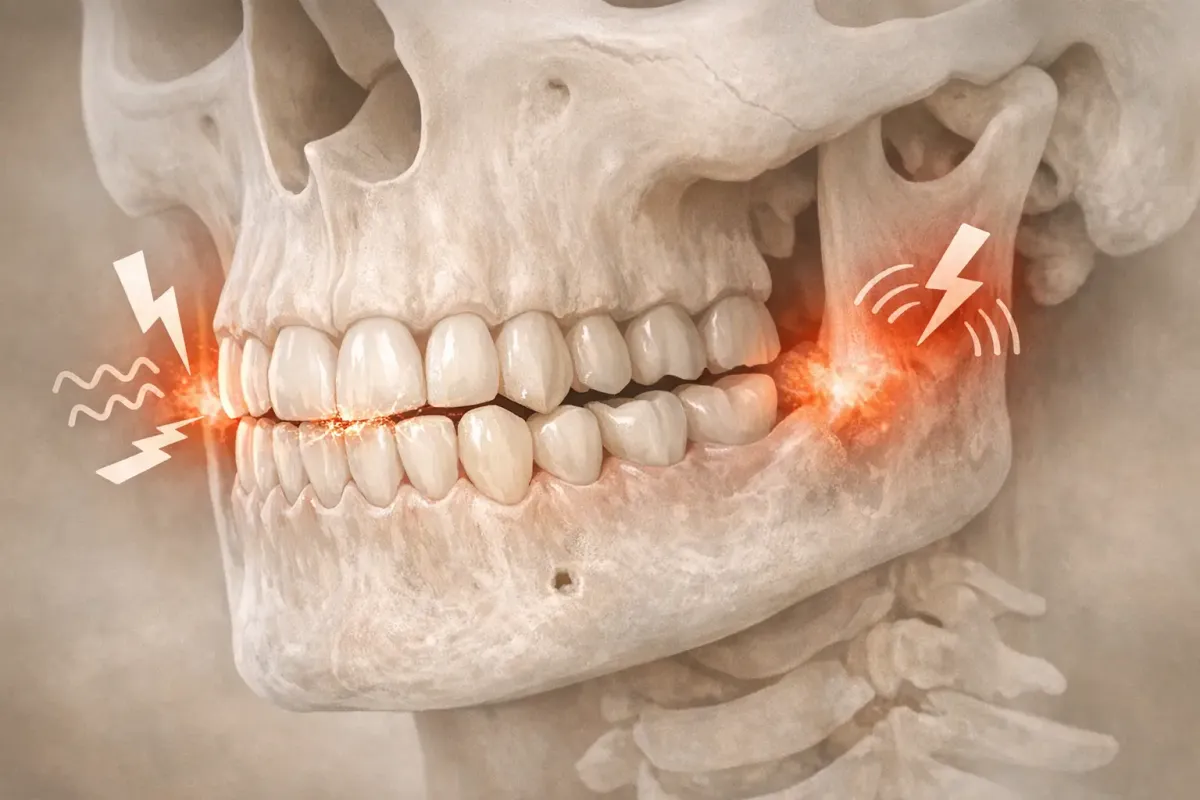
Grinding your teeth might seem trivial until you wake up with a sore jaw, headache, and a partner nudging you because you sound like a rusty chainsaw. That unwanted noise is bruxism, and if you're reading this, you probably want it gone. Thankfully, researchers and clinicians are busy testing everything from relaxation techniques to botulinum toxin. The evidence is clear on what works, what might help, and what is mostly hype. This guide walks you through that evidence so you can choose a bruxism treatment that fits your lifestyle, mouth, and budget.
Below, you'll find plain-language summaries of recent studies, comparisons of popular therapies, and practical questions to ask your dentist or sleep specialist. Keep the facts close and the jargon at arm’s length.
Understanding Bruxism: Causes and Symptoms
Bruxism is the repetitive clenching or grinding of teeth, and it shows up in two main types. Awake bruxism occurs during the day while you’re concentrating or stressed. Sleep bruxism kicks in after you doze off and is classified as a sleep-related movement disorder. A 2025 meta-analysis by Stanisic et al. indicates awake bruxism prevalence at roughly 23 percent of adults, while sleep bruxism ranges from 6 to 13 percent in the general population, according to the American Dental Association’s resource page.
Bruxism sits at the crossroads of neurology, psychology, and dentistry. Stress, caffeine, misaligned bites, and certain medications all play roles, yet no single trigger explains every case. A systematic review by Graham et al. highlights that many with bruxism also report temporomandibular disorders (TMD), headaches, or sleep apnea. Left unchecked, bruxism can chip teeth, loosen fillings, and overwork jaw muscles.
Key Causes of Bruxism
- Stress and Anxiety: Heightened cortisol levels correlate with increased muscle activity in the jaw. Daily worries often translate into clenching. Explore how stress and anxiety trigger teeth clenching at night.
- Sleep Disturbances: Fragmented sleep, obstructive sleep apnea, and restless leg syndrome are linked to nighttime grinding. Learn more about the connection between sleep disorders and bruxism.
- Neurochemical Factors: Dopamine imbalance and certain antidepressants (particularly SSRIs) can raise bruxism risk.
- Malocclusion: Although bite issues were once blamed for all bruxism, current evidence shows they are contributing rather than primary causes.
- Lifestyle Stimuli: High intake of caffeine, alcohol, or nicotine boosts jaw-muscle activity, especially before bed.
Common Symptoms to Recognize
- Audible grinding or clicking sounds during sleep reported by a partner
- Morning jaw stiffness or pain in the temples
- Flattened, chipped, or cracked teeth
- Sensitivity to hot, cold, or sweet foods due to enamel wear
- Frequent tension-type headaches, particularly upon waking
- Indentations on the sides of the tongue or inside the cheeks
Spotting these signs early can save you from expensive dental repairs down the road. Now that you know the basics, explore the tools available to put bruxism in its place.
Exploring Bruxism Treatment Options
No single fix suits everybody. Effective management usually combines several approaches: tweaking daily habits, protecting teeth with dental devices, and addressing medical or psychological drivers. A 2024 systematic review by Ainoosah et al. evaluated different occlusal splints—the classic night guards—and found that while designs vary, they all reduce tooth wear and self-reported pain when used consistently. Yet splints only protect teeth; they do not stop the muscle activity itself. That's where lifestyle changes, physical therapy, or pharmaceuticals may earn their keep.

Lifestyle Changes
Think of lifestyle tweaks as the low-hanging fruit. They cost little and may reduce grinding intensity enough to skip costlier therapies.
- Stress Management: Daily mindfulness sessions, slow breathing techniques, or guided relaxation can reduce awake bruxism episodes. The Mayo Clinic notes that people who incorporate stress-reduction routines often report fewer clenching incidents. Discover natural jaw tension relief solutions that can help.
- Caffeine and Alcohol Curbs: Cutting off stimulants after noon and keeping alcohol to moderate levels help stabilize sleep stages, lowering nocturnal grinding. Understand the effects of alcohol on teeth grinding.
- Sleep Hygiene: Sticking to regular bedtimes, keeping screens out of the bedroom, and using blackout curtains can trim micro-arousals linked to sleep bruxism. Explore how sleep hygiene can improve bruxism.
- Jaw Awareness Exercises: Setting phone alerts that remind you to drop your tongue from the palate and relax your jaw trains muscle memory away from clenching.
Dental Interventions
Your dentist’s office is ground zero for mechanical defenses. The goal is simple: create a barrier so teeth glide rather than grind, and distribute bite forces more evenly.
- Occlusal Splints: Custom acrylic or soft guards worn overnight remain the gold-standard dental intervention. The review by Ainoosah et al. found no clear winner among hard, soft, or dual-laminate splints, so comfort and durability should guide your choice. Compare the differences between OTC and custom night guards.
- Repositioning Devices: Some splints adjust lower-jaw position to reduce muscle hyperactivity. Evidence is mixed, and they may affect swallowing or speech if worn during the day.
- Dental Corrections: When a severely misaligned bite or missing teeth exaggerate forces, orthodontics or restorative work can redistribute pressure. These are long-term projects rather than quick fixes.
Dental devices excel at shielding enamel but do not address the neural or psychological roots of bruxism. That gap has prompted the rise of newer options, including small injections with big effects.
Botulinum Toxin: A Modern Approach
Botulinum toxin type A (BTX-A) has shifted from smoothing forehead wrinkles to relaxing overactive jaw muscles. In bruxism, tiny doses injected into the masseter and temporalis muscles reduce clenching strength without paralyzing everyday chewing. A comprehensive overview by Coelho et al. summarizes 27 clinical trials and concludes that BTX-A decreases grinding episodes and pain scores for three to six months per session.
Effectiveness of Botulinum Toxin
Multiple head-to-head trials pit BTX-A against splints, medication, and dry needling. In a 2025 systematic review by Yacoub et al., BTX-A lowered electromyographic activity by up to 80 percent and cut self-reported pain in half compared with baseline. A 2024 randomized study by Şahin et al. found BTX-A outperformed dry needling and diazepam in reducing myofascial pain after eight weeks.
Key perks include:
- Minimal downtime—most people return to normal routines within hours
- No reliance on nightly compliance, unlike splints
- Objective reduction in muscle force, protecting dental work even when you forget a mouthguard
Potential Risks and Benefits
BTX-A is not magic sauce for everyone. Benefits must outweigh possible downsides:
- Temporary Weakness: Over-injection can make chewing tough meats or chewing gum hard for several weeks.
- Cost: Injections average $300–$700 per session, often out of pocket.
- Repeat Visits: Effects fade after three to six months, requiring maintenance shots.
- Side Effects: Mild bruising, headaches, or asymmetry are uncommon but documented.
- Skill Dependent: Precision is key. Always seek clinicians trained in orofacial applications rather than cosmetic injectors dabbling in jaw muscles.
Despite these caveats, BTX-A offers a powerful adjunct or alternative when splints or lifestyle shifts fall short.
Pharmacological and Manual Therapies
Before needles or custom plastic guards, many people reach for a pill or book a massage. Both pharmacological and manual therapies aim to dampen muscle hyperactivity and relieve pain, but the evidence varies.

Medications for Bruxism
Common pharmaceutical options include muscle relaxants, anti-anxiety agents, and certain antidepressants. Yet results are mixed, and side effect profiles can be substantial.
- Clonazepam: Sometimes prescribed for sleep bruxism, this benzodiazepine may reduce muscle activity but carries risk of dependency and next-day drowsiness.
- Gabapentin: An anticonvulsant studied for neuropathic pain, it shows modest reductions in bruxism scores but may cause dizziness.
- Buspirone: A non-benzodiazepine anxiolytic with fewer sedation issues. Evidence is still preliminary.
- Dopaminergic Agents: Small studies test levodopa in sleep bruxism linked to Parkinson’s disease, but general applicability is limited.
The prospective randomized study by Şahin et al. compared diazepam, dry needling, BTX-A, and manual therapy. Diazepam showed quick pain relief but lost efficacy by week four, and participants reported grogginess and cognitive fog. Medications can bridge short periods of severe symptoms, yet most guidelines advise against long-term use due to tolerance and side effects.
Manual Therapy Techniques
Hands-on approaches like physical therapy, myofascial release, and trigger-point massage target overloaded jaw muscles. A 2024 trial by Pires et al. examined adults with bruxism-related myofascial pain. After six weeks of targeted stretches and posture correction, participants displayed improved craniocervical posture and reduced pain scores.
Common techniques include:
- Myofascial Release: Sustained pressure on trigger points within the masseter and temporalis muscles eases tightness and improves circulation.
- Stretch-and-Spray: Alternating cold sprays and gentle stretching breaks pain-spasm cycles.
- Postural Training: Forward head posture stresses the jaw. Therapists coach neutral spine alignment to rebalance muscle loads.
- Dry Needling: Fine needles inserted into tight bands stimulate local twitch responses, reducing muscle tone. The Şahin study found pain relief comparable to manual therapy but less durable than BTX-A.
Manual therapy shines for people wary of medications or injections. Sessions feel relaxing, improve range of motion, and teach self-care exercises. They do require multiple visits and skilled practitioners for lasting results.
Evaluating the Impact of Bruxism Treatments
Managing bruxism is about more than silencing crunching noises. It touches quality of life, dental integrity, and even long-term orthopedic health. Treatments should therefore be assessed across several dimensions.
Quality of Life Improvements
Pain relief, better sleep, and less daytime fatigue top the list of patient-reported outcomes. In the randomized trial by Pires et al., manual therapy plus home exercises improved sleep quality scores by 25 percent. Meanwhile, the BTX-A studies cited above consistently show drops in headache frequency and jaw stiffness. A good clinician will track these subjective improvements through validated questionnaires like the Oral Health Impact Profile or the Pittsburgh Sleep Quality Index.
Considerations for Dental Health
Teeth and restorations take a beating from uncontrolled bruxism. If you have crowns, veneers, or implants, protection is non-negotiable. A 2024 meta-analysis by Häggman-Henrikson et al. examined implant survival in bruxers versus non-bruxers. Failure rates doubled in untreated bruxers, underscoring the need for night guards or adjunct therapies. Occlusal splints remain the frontline defense here, but when high bite forces persist, BTX-A can serve as a force damper. Regular dental checkups catch micro-fractures early, allowing for minor adjustments rather than costly reconstructions later.
Balanced jaw forces also protect the temporomandibular joint (TMJ). Chronic overload can inflame the joint capsule, leading to clicking or locking. Splints that reposition the jaw too aggressively may shift loads onto the TMJ, so device design should be individualized and monitored.
Making Your Decision: Factors to Consider
Choosing a bruxism treatment is not one-size-fits-all. Mix and match based on severity, personal comfort, budget, and professional guidance. The INfORM/IADR best-practice statement by Manfredini et al. emphasizes a stepped-care model—start conservative, escalate only if necessary.
Personal and Clinical Considerations
- Symptom Severity: Mild tooth wear and daytime awareness often respond to stress management and jaw exercises alone. Discover effective jaw relaxation techniques for nighttime clenchers.
- Medical History: Neurological disorders, pregnancy, or certain medications may steer you away from BTX-A or benzodiazepines.
- Dental Status: Recent implant surgery? Opt for immediate protective splints and consider BTX-A to minimize overload.
- Budget and Insurance: Splints have upfront costs but last years. BTX-A spreads smaller payments over time yet rarely receives insurance coverage for bruxism. Learn about bruxism treatment costs.
- Lifestyle Fit: Night-shift workers with irregular sleep may benefit from devices that work regardless of schedule, while globetrotters may prefer portable solutions like guided relaxation apps.
Consulting with Healthcare Professionals
Your first call is usually your dentist, who can spot enamel wear and recommend splints. If pain dominates, a physical therapist or orofacial pain specialist joins the team. Sleep bruxers may need a polysomnography referral to rule out apnea. For BTX-A, look for practitioners credentialed in dental or maxillofacial applications. Always:
- Ask about evidence backing the recommended therapy and any alternatives.
- Review potential side effects and how outcomes will be measured.
- Set realistic timelines—many therapies show peak benefits after several weeks.
- Schedule follow-up visits to tweak or combine treatments as your symptoms change.
Smart, shared decision-making beats trial-and-error every time.
Conclusion
Bruxism sits at the junction of stress, muscle overactivity, and dental wear. Luckily, today’s toolbox is wide open: lifestyle tweaks, splints, manual therapy, targeted meds, and precision BTX-A injections. The strongest evidence supports starting conservatively, layering protective splints and stress management before moving to pharmaceuticals or injections when symptoms persist. Every mouth and every life are different, so partner with qualified professionals, track your progress, and adjust your plan as needed. A quieter night's sleep and happier teeth are well within reach.