Why Do I Grind My Teeth in My Sleep? Surprising Causes Revealed
Uncover surprising causes of teeth grinding during sleep, from stress to diet, in this comprehensive guide.

Picture this: you wake up, stretch, and feel your jaw complaining about a workout it never signed up for. Your partner says the nighttime sounds like two stones being rubbed together. That gritty noise is bruxism, the clinical name for teeth grinding, and you are not alone.
Researchers have spent decades puzzling over what causes teeth grinding while the rest of the body is at rest. Their findings go beyond just stress. Caffeine, irregular sleep schedules, and even vitamin deficiencies can play a role. Below is the evidence, explained simply and with a touch of humor, to help you decide what to do next.
Understanding Nocturnal Teeth Grinding: The Basics
Bruxism involves repetitive jaw-muscle activity like clenching, grinding, or gnashing. Dentists categorize it into two types: sleep bruxism and awake bruxism. You are here for the sleep variety, which affects about 13 percent of adults worldwide, according to a study by Manfredini et al. 2024.
How do you know if you're grinding? The signs often show up at your next dental cleaning:
- Flattened, chipped, or loose teeth
- Cracks in molars that resemble lightning bolts
- Tense cheek muscles or a tired jaw upon waking
- Complaints from a nearby sleeper
Dental students can identify these signs quite well. In a study, 79 percent of future dentists recognized wear facets and morning jaw pain as indicators of sleep bruxism (Şahin 2024). If the trainees notice, so will your hygienist.
Researchers also use tools like electromyography and audio sensors, but the key point is simple: rhythmic, involuntary muscle contractions wear down the hardest substance in your body each night. The American Dental Association’s bruxism page lists tooth surface loss, gum recession, and headaches as typical side effects. If untreated, the problem can lead to cracked fillings and chronic pain.
So grinding is common, diagnosable, and harmful if you like your enamel. But why does a resting brain engage your jaw? Let’s explore the first and perhaps most obvious trigger: stress.
The Stress Factor: How Anxiety Fuels Bruxism
Your brain doesn't shut down when you sleep. It cycles through stages, each with its own rhythm. Stress hormones can disrupt this pattern. A 2024 review by Voß et al. links higher stress levels with more frequent grinding, creating a cycle where poor sleep increases daytime anxiety and vice versa.
Stress and Sleep Disruption
Stress alters sleep architecture, leading to less time in deep, restorative stages and more in lighter phases where muscle activity spikes. Cleveland Clinic notes that disrupted sleep fosters jaw over-activity. Your jaw gets the memo to clench long before you reach dreamland.
The Role of Cortisol
Cortisol, a key stress hormone, usually peaks in the morning. Chronic stress shifts that pattern, leaving cortisol elevated at bedtime. High nighttime cortisol is linked to micro-arousals—brief wake-ups you may not remember. Each arousal is a chance for the jaw muscles to contract. A clinical trial combining manual therapy with home exercises found reduced pain and lower salivary cortisol in bruxers who addressed stress (Kadıoğlu et al. 2024).
Notice how your shoulders tense during stress? That tension often migrates to the jaw. Patients report that stressors like deadlines or bedtime doom-scrolling lead to aching molars in the morning. Identifying these pressure points, perhaps by keeping a “stress diary” by your bed, can help you spot patterns you can change.
If your days are packed with stress, your nights might be packed with tooth-grinding rehearsals. Managing stress is not just self-care; it's a way to protect your enamel.
Dietary Influences: Foods That Might Be Grinding Your Gears
Your jaw isn't the only high achiever; your diet can also ramp up bruxism. Food choices influence neurotransmitters, muscle function, and even tooth integrity. Two categories stand out: stimulants and nutrient gaps.
Caffeine and Sugar
That afternoon latte can linger in your bloodstream for over six hours. Stimulants increase nervous system activity, which affects sleep. A 2024 review found high caffeine consumers showed more enamel wear, possibly via bruxism pathways (Fontelle et al. 2024). Sugar isn't innocent either; blood sugar swings can wake your brain at night, setting the stage for jaw action.
Nutritional Deficiencies
Calcium, magnesium, and vitamin D help muscles relax. When you're low on these, muscles cramp. While hard data on bruxism is emerging, one trial found vitamin D with anti-inflammatories improved facial muscle pain (Kahraman et al. 2025). Nutrients help muscles relax, including those that clamp your teeth.
Alcohol also plays a role. A nightcap may feel relaxing, but alcohol disrupts REM sleep and dehydrates muscles, leading to twitchier fibers that seize any chance to clench. Replacing bedtime whiskey with a magnesium-rich smoothie often results in quieter nights within a week. Staying hydrated is crucial—sip water steadily so your muscles aren't running on empty electrolytes at night.

The Mayo Clinic advises limiting caffeine and alcohol close to bedtime. Swap the 3 pm energy drink for water or herbal tea, and consider foods rich in magnesium—like spinach and nuts—to pacify your jaw.
Lifestyle Choices: The Unseen Culprits
Diet is part of a broader lifestyle picture. How you move and sleep can protect or harm your oral health. Bruxism often pairs with habits that affect oral health.
Sedentary Behavior
Exercise is nature’s stress relief. People who get less than 150 minutes of activity a week report higher stress and worse sleep, according to a 2024 review by Ciantelli et al. Less movement means more pent-up energy, which appears as clenched jaws at night. Exercise also helps regulate cortisol, offering a double benefit.
The same review notes screen time as a risk factor. Blue light delays melatonin release, pushing bedtime later. Each hour of shifted sleep correlates with higher bruxism frequency. Melatonin signals your jaw muscles to relax, so when it's late, the grinding show runs overtime.
Poor Sleep Hygiene
Sleep hygiene is about routines that signal your brain to wind down. The National Institutes of Health lists irregular bedtimes, late-night snacking, and bedroom light pollution as common offenders. These factors shorten deep sleep and extend lighter cycles, increasing bruxism bursts.
The manual therapy trial showed that participants who stretched, breathed, and maintained consistent bedtimes saw bigger reductions in grinding than those who only received in-clinic treatment. Consistency beats passive fixes.
Quick lifestyle tweaks for significant benefits:
- Set a fixed bedtime and wake time, even on weekends.
- Power down screens 60 minutes before bed.
- Take a brisk walk after dinner.
- Keep the bedroom cool and dark.
- Mind your daytime jaw posture: lips together, teeth apart, tongue on the palate.
Think of lifestyle changes as compound interest for teeth: small efforts that add up to significant enamel savings over time.
Medical Conditions Linked to Teeth Grinding
Sometimes grinding is linked to underlying medical issues. Identifying these can be tricky as cause and effect blur.
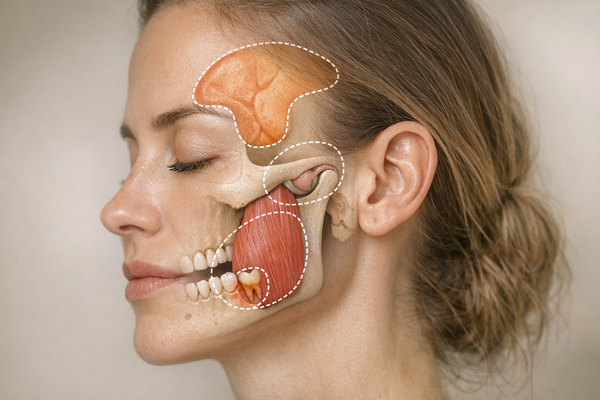
Temporomandibular Joint Disorders
The temporomandibular joint (TMJ) is your jaw’s hinge. When it misaligns or inflames, muscles overcompensate. A 2024 review by Voß et al. concludes that bruxism can cause and result from TMJ disorders. Picture a squeaky door: sometimes the noise causes damage, sometimes damage causes the noise.
In people with myofascial pain tied to TMJ, vitamin D plus diclofenac improved mouth-opening range and reduced tenderness compared to drug alone (Kahraman et al. 2025). This suggests systemic factors like nutrient status can modulate TMJ-related bruxism.
Other Health Issues
Migraines, sleep apnea, GERD, and some neurological conditions have been linked to teeth grinding in studies. Harvard Health notes untreated sleep apnea triples the odds of bruxism. With GERD, stomach acid irritates throat tissues, causing micro-awakenings that might trigger jaw contractions as a reflex.
Some medications—SSRIs, ADHD stimulants, and antihistamines—list bruxism as a side effect. If your grinding increased after a medication change, talk to your doctor. Sometimes a dose tweak or switch can save your mental health and your molars.
Screening for these conditions is important because mouthguards alone won't fix airway blockages or acid reflux. Collaborative care—with a dentist, physician, and sometimes a sleep specialist—is the best approach.
Preventative Measures and Treatment Options
No single solution works for everyone, but evidence supports behavioral and dental interventions.
Behavioral Therapies
Cognitive-behavioral therapy, mindfulness meditation, and biofeedback have been studied. In a clinical trial, adding relaxation exercises reduced grinding episodes by 40 percent (Kadıoğlu et al. 2024). Biofeedback devices, which alert you to jaw muscle activity, train subconscious relaxation. They cost more than a pillow but less than a crown replacement.
For tech enthusiasts, smartphone apps pair with EMG patches to alert you when you clench during the day. Users often find that daytime awareness reduces nighttime intensity. Combine this with a five-minute evening journal to track stressors, caffeine intake, and muscle tension, creating a low-cost feedback loop.
Other low-tech options:
- Jaw stretches before bed
- Guided breathing apps
- Progressive muscle relaxation
Dental Interventions
Mouthguards—or occlusal splints—are the frontline tool. They don't stop grinding; they protect teeth from damage. A 2024 review found custom-made guards more effective than over-the-counter options due to their fit and ability to promote a slightly open bite (Dhaliwal and Ouanounou 2024).

Custom splints can cost $300 to $800, but compare that to the cost of a ceramic crown, and they seem like a bargain. If budget is tight, boil-and-bite guards from the pharmacy are a temporary solution—just check them for wear and replace regularly.
For severe TMJ pain, dentists might adjust bite surfaces or suggest botulinum toxin injections to relax muscles. These are usually considered when other treatments fail.
Dietary changes also help in prevention. Swap coffee for chamomile tea, increase magnesium intake, and log meals to identify food triggers. Cleveland Clinic’s bruxism guidance supports these strategies.
Conclusion
Teeth grinding is not just a habit; it's a multi-factor phenomenon. Stress sets the stage, diet and lifestyle amplify it, and hidden medical issues add complexity. The good news is each factor offers a way to intervene. Start by tracking caffeine intake, creating calming evening rituals, and asking your dentist about a custom guard. If pain persists, consider screening for TMJ disorders, sleep apnea, or nutrient deficiencies.
Your jaw spends all day helping you talk and chew. Give it a break at night. Collaborate with healthcare professionals, adjust unnoticed habits, and you'll wake up with less noise in your head and more enamel on your teeth.