TMJ Pain Management: What Makes It Worse and How to Avoid It
Discover triggers of TMJ pain and tips to alleviate it. Learn more about effective TMJ pain management.
Jaw pain that shows up when you chew a sandwich or yawn mid-meeting is more than an annoyance. If the pain is coming from the temporomandibular joint (TMJ), it can snowball into headaches, ear pain, even neck tension that wrecks your day. Managing TMJ pain starts with knowing what makes it flare. Recent research has outlined new molecular culprits and lifestyle triggers. Good news: the same data point toward simple strategies you can implement to alleviate discomfort.
This guide breaks down the latest evidence on TMJ pain using plain language and a hint of skepticism. You'll learn why inflammation increases discomfort, how sleep-related tooth grinding sneaks in, and what exercises or nutrients can help reduce pain. Ready to explore the research and real-world fixes? Let's dive in.
Understanding TMJ Pain: Causes and Common Triggers
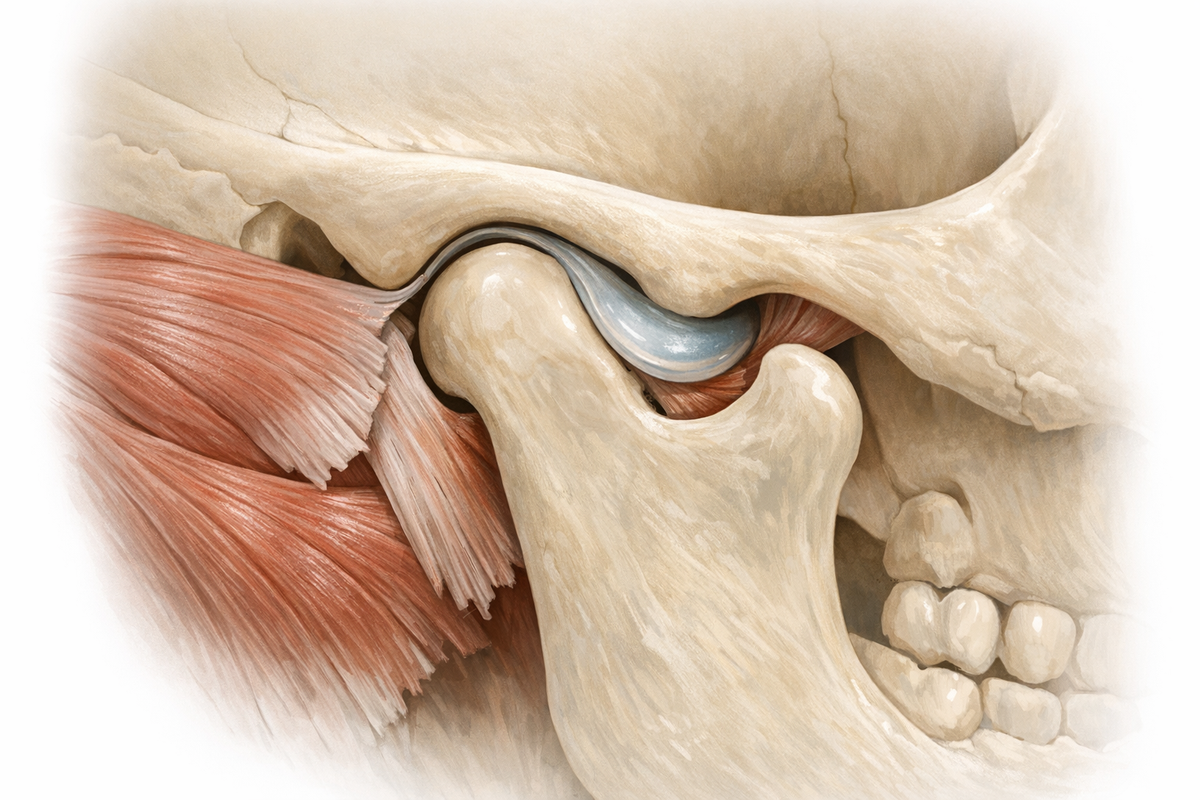
The temporomandibular joint works like a sliding hinge that lets your jaw open, close, and move side to side. Two bony knobs called condyles sit at the end of the lower jaw and fit into sockets in the skull. A thin cartilage disc cushions each contact point, while surrounding muscles control motion. Because the joint handles constant movement and force, even small irritations can turn painful.
Common causes of TMJ pain include:
- Cartilage wear or displacement
- Muscle overuse or spasm
- Inflammation inside the joint capsule
- Trauma, such as a blow to the face or whiplash
- Systemic conditions like arthritis
On the molecular side, cartilage health relies on proteins that keep tissue springy. When that balance tips, the disc and joint surfaces degenerate. For example, a 2026 study by Raut et al. showed that deleting the LOXL2 gene triggered osteoarthritis-like damage in the TMJ in animal models. The same paper noted that overexpressing LOXL2 protected cartilage from cell death driven by NF-κB, a key inflammatory switch. Your jaw joint dislikes inflammation but thrives with proteins that repair collagen.
Beyond biology, clinical experience and surveys point to lifestyle factors as potent pain contributors. The Mayo Clinic lists jaw clenching, gum chewing, and high stress as everyday culprits. Each of these loads the jaw muscles until they revolt with pain.
The Role of Bruxism and Sleep Disorders
Nighttime tooth grinding, known as sleep bruxism, is a prime offender. You might not feel the clench, but your TMJ feels the aftermath in the morning. A 2025 study by Yeon-Hee Lee and colleagues linked sleep bruxism to psychological stress markers, anemia, and jaw muscle tenderness. The researchers followed 120 adults and used electromyography during sleep to measure grinding episodes. People with more bruxism also reported higher morning jaw pain and stiffness.
Sleep apnea exacerbates this issue. When the airway collapses, the brain jars you awake with a mini burst of muscle activity, often including jaw clenching, increasing TMJ load each night. The Cleveland Clinic notes that treating sleep apnea or using a mandibular advancement device can reduce both snoring and joint pain.
Key takeaway: if you wake up with a sore jaw, investigate bruxism and sleep quality. A custom night guard, stress management, or a sleep study can break the cycle.
Inflammation and Its Impact on TMJ Pain
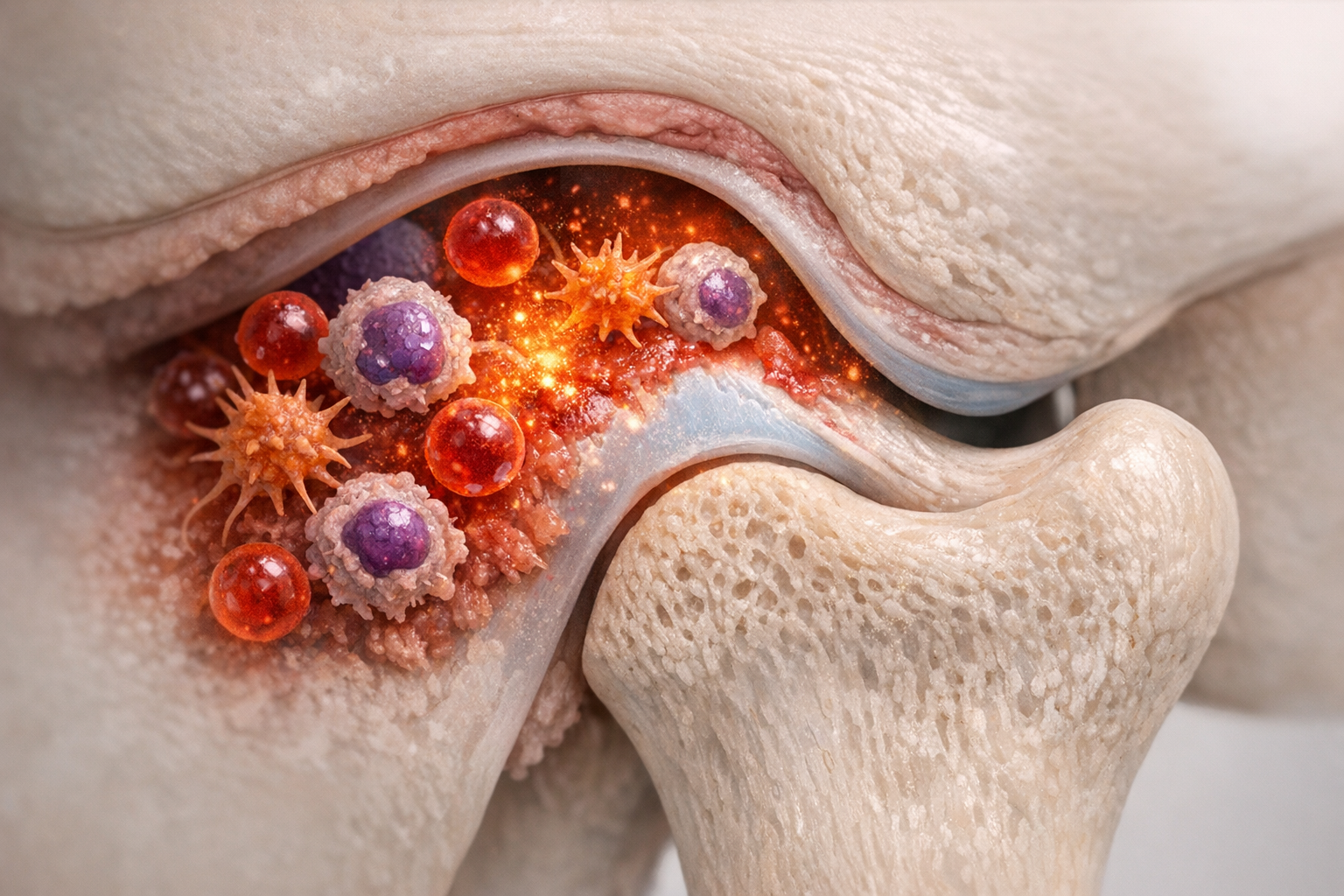
Inflammation is the body’s cleanup crew, but when it overstays, tissues suffer. In the TMJ, chronic inflammation bathes cartilage and bone in enzymes that erode collagen and irritate nerves. Swelling inside the tight joint capsule also boosts pressure, which your brain flags as pain.
At the cellular level, immune cells release cytokines—chemical text messages that tell neighboring cells to fight. Too many cytokines switch chondrocytes (cartilage cells) from builders to quitters. They stop making collagen and start leaking destructive enzymes.
A 2025 study by Chen Wenqian et al. revealed that eosinophils, a type of white blood cell, can actually dial back damage by prompting synovial fibroblasts to secrete lumican, a protective protein. This interaction reduced cartilage degradation in lab models through the TGF-β pathway. So not all inflammation is harmful, but balance is key.
Chondrocyte Ferroptosis and Cartilage Degradation
An emerging villain in TMJ degeneration is ferroptosis, an iron-dependent form of cell death. Think of it as rust inside your joint. Chen B Y et al. (2024) demonstrated that low oxygen combined with inflammation triggers HIF-1α and TFRC, two molecules that invite iron into chondrocytes. The iron sparks lipid peroxidation, leading to cell death. Dead chondrocytes leave potholes in cartilage, making movement gritty and painful.
Managing inflammation requires two approaches:
- Quenching excess immune signals with diet, easy movement, and, when prescribed, NSAIDs or corticosteroid injections.
- Supporting antioxidant defenses to block ferroptosis. Nutrients like vitamin E, selenium, and polyphenols in colorful fruits can help mop up free radicals.
Clinical advice from Johns Hopkins Medicine: maintain a diet high in anti-inflammatory foods like fish, berries, and leafy greens, and limit ultra-processed snacks. Adequate hydration helps keep cartilage supple, while smoking reduces blood flow and oxygen, worsening the hypoxic environment that accelerates ferroptosis.
Lifestyle Factors That Worsen TMJ Pain
Daily choices either soothe the joint or exacerbate pain. Here are some key factors:
Dietary Choices
Crunchy baguettes, giant burgers, and sticky candies force your jaw open wide and make the condyles grind harder into their sockets. If you already have cartilage thinning, every bite turns into microtrauma. Follow these tips:
- Swap hard crusts for softer whole-grain bread.
- Cut food into small bites instead of taking large mouthfuls.
- Limit caffeine. High doses may increase clenching by activating your nervous system.
- Watch alcohol. It disrupts sleep architecture and exacerbates bruxism spikes.
- Add anti-inflammatory staples: omega-3-rich salmon, turmeric-spiced dishes, plenty of produce.
Water is crucial too. Dehydrated cartilage loses its resilience. Aim for at least eight cups a day unless your doctor advises otherwise.
Posture and Daily Habits
That neck-craning phone scroll is not just straining your spine; it drags your mandible backward, jamming the condyles. Over time, poor posture shifts muscle firing patterns, leading some fibers to overwork and stiffen.
Practical fixes:
- Hold screens at eye level so your ears line up with your shoulders.
- Set a timer every 30 minutes to roll your shoulders and gently tuck your chin.
- At the desk, keep feet flat, hips slightly higher than knees, and elbows at 90 degrees.
- During phone calls, use earbuds instead of cradling the handset between shoulder and jaw.

Stress management is essential because the jaw often reflects emotional tension. Simple diaphragmatic breathing, meditation apps, or short walks can lower cortisol and reduce muscle tension around the TMJ.
Finally, reconsider gum. Chewing sugar-free gum has dental perks, but long sessions can overwork the masseter muscle. If you rely on gum for fresh breath, limit it to 10 minutes and choose soft mints for the rest of the day.
Effective TMJ Exercises for Pain Relief
Exercise for the jaw? Absolutely. Gentle movement lubricates the joint, strengthens stabilizing muscles, and reduces trigger-point knots. Keep the mantra: “low load, high frequency.” Aim to do each move two to three times daily, five to eight reps per set, unless pain dictates otherwise.
Gentle Stretching and Strengthening Techniques
- Controlled Mouth Opening
Place your tongue on the roof of your mouth behind the front teeth. Slowly open your jaw as far as comfort allows, keeping the tongue contact. Hold for three seconds, then close. This trains the joint to hinge rather than slide forward. - Resisted Closing
Put two fingers under your chin. As you try to close your mouth, offer mild resistance with the fingers, feeling the muscles engage without pain. Hold for three seconds and release. - Side-to-Side Glide
With your mouth slightly open, move your jaw gently to the left, hold two seconds, return to center, then glide to the right. Use a mirror to avoid jaw deviation or excessive neck movement. - Neck Flexor Activation
Lie on your back with knees bent. Nod your head as if saying yes, lifting the head just off the floor for five seconds. Strengthening deep neck flexors helps align the TMJ. - Massage and Heat
Before exercises, apply a warm pack for 10 minutes to loosen tissues. Afterward, use fingertips to massage the masseter and temporalis muscles in small circles.
The American Dental Association suggests pairing exercise with mindfulness: note when your teeth touch during the day. Ideally, your upper and lower teeth should be slightly apart at rest, with lips closed and tongue relaxed against the palate.
If sharp pain arises, reduce the range of motion or pause. Overstretching can inflame the joint. Consistency beats intensity: mini-workouts sprinkled through the day are more effective than one intense session.
Innovative Therapies for TMJ Pain Management
Beyond classic physical therapy and splints, researchers are testing new molecules and delivery methods to calm TMJ pain. One promising candidate is naringenin, a citrus flavonoid found in grapefruit and oranges.
Potential Benefits of Naringenin
A 2025 study by Hashemi et al. explored naringenin’s effect on dental pulp pain and related cognitive fog in rats. Oral supplementation reduced pain behaviors and improved performance in memory mazes, likely by reducing inflammation and oxidative stress. While the study did not target the TMJ directly, the anti-inflammatory pathways are similar.
Translating this to jaw pain, scientists theorize that naringenin could curb cytokine storms and protect chondrocytes from oxidative injury. Human trials are small but promising. Early pilot data at the University of São Paulo gave TMJ patients a 600 mg daily naringenin supplement for eight weeks and reported reduced jaw clicking and self-rated pain.
How to try it safely:
- Eat citrus fruits daily—whole fruit is better than juice for fiber and blood sugar control.
- Consider a standardized naringenin supplement after discussing it with a healthcare professional, especially if you take medications that interact with grapefruit.
- Combine with antioxidant-rich foods (berries, green tea) for a synergistic boost.
Other emerging options include low-level laser therapy, platelet-rich plasma injections, and neuromodulation devices that train the nervous system to lower pain signals. The American Association of Oral and Maxillofacial Surgeons notes these modalities are adjuncts, not stand-alone cures. Always start with conservative care: education, exercise, oral appliances, and stress reduction.
Conclusion
TMJ pain thrives on a perfect storm of mechanical overload, inflammation, and nervous-system misfires. You cannot swap out a jaw joint like a smartphone battery, but you can tweak the inputs that keep pain circuits active. Understand your triggers—late-night bruxism, slouched posture, crunchy foods—and remove them piece by piece. Feed the joint anti-inflammatory nutrients, practice gentle exercises, and consider evidence-backed supplements like naringenin under professional guidance.
The science is clear: when you calm inflammation and balance muscle forces, cartilage stands a fighting chance. Pair this knowledge with consistent self-care and the TMJ can move from daily headline to background noise. If pain persists or worsens, team up with a dentist, physical therapist, or orofacial pain specialist for tailored support. Your jaw may be small, but with the right strategy, it can stop shouting for attention and get back to simply helping you talk, chew, and yawn without drama.