Jaw Pain After Sleeping: How Sleep Positions Impact Bruxism
Explore how sleep positions can cause jaw pain and bruxism.

If you wake up with a sore jaw, you're not alone. More than eight percent of adults grind or clench their teeth in their sleep, a habit dentists call sleep bruxism. Until recently, most people blamed stress alone, but new research is investigating what happens after you close your eyes: your sleep position. In other words, the way you sprawl, curl, or lie flat may be influencing your jaw. To explore how different sleep arrangements impact jaw pain, you might find it helpful to understand how sleep positions influence nighttime teeth grinding.
This article explores the science of bruxism, delves into the impact of common sleep positions, and shows how shifting posture can ease jaw pain. The evidence comes from randomized trials, imaging studies, and guidance from major health organizations, so you get practical advice without the fluff.
Understanding Bruxism and Its Causes
Defining Bruxism
Bruxism is the medical term for grinding, clenching, or gnashing your teeth. During the day, you can often feel it and stop. Sleep bruxism, though, is involuntary and happens while you are unconscious. Dentists look for signs like flattened chewing surfaces, cracks in enamel, and headaches near the temples. If you're experiencing symptoms like these, it may be helpful to explore signs you grind your teeth for more detailed insights.
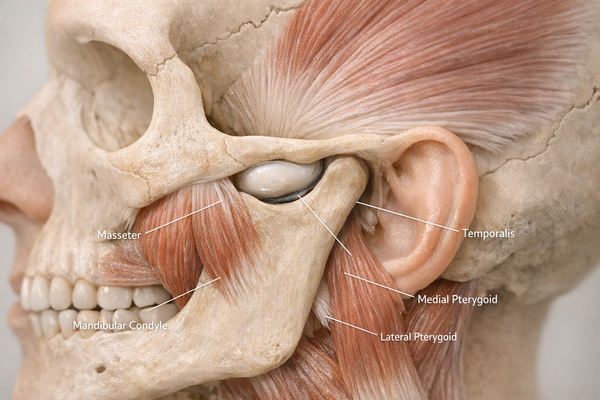
The Mayo Clinic defines bruxism as a “repetitive jaw-muscle activity characterized by clenching or grinding of teeth and by bracing or thrusting of the mandible.” Simply put, your jaw muscles keep contracting when they should be resting. Over time, this stress can inflame the temporomandibular joint (TMJ) and strain surrounding muscles. For those dealing with TMJ issues, understanding how to manage TMJ pain effectively can be crucial.
Common Causes of Bruxism
Bruxism has multiple triggers. Stress is a major factor, but modern studies highlight other contributors.
- Psychological factors. Anxiety and chronic stress increase muscle tone. In a cross-sectional analysis, researchers Coşkun Karataş and Menek reported that higher anxiety scores correlated with more bruxism episodes.
- Oral habits. Daytime gum chewing or nail biting keeps jaw muscles active, increasing night-time grinding risk. A large survey linked frequent oral habits to TMJ pain and bruxism symptoms.
- Sleep disorders. We will explore this later, but obstructive sleep apnea (OSA) often coexists with bruxism, suggesting breathing struggles activate jaw muscles. The connection between bruxism and sleep disorders like OSA is further explained in this article on surprising causes of teeth grinding during sleep.
- Medications and substances. Caffeine, alcohol, and some antidepressants raise muscle activity during sleep. The role of substances like caffeine in exacerbating bruxism is discussed in more detail in the caffeine and bruxism summary.
- Posture and biomechanics. The way you hold your head or sleep on a pillow can alter jaw alignment and muscle load, bringing sleep position into the conversation.
Several factors can accumulate. For instance, a stressed office worker who sips coffee late, scrolls on the couch, and sleeps on a lumpy pillow sets the scene for their jaw muscles to work overtime.
The Science of Sleep Positions
Common Sleep Positions
Sleep researchers categorize posture into three main types:
- Supine. Lying on your back, face and chest upward.
- Prone. Lying on your stomach, face down or turned to one side.
- Lateral (side). Sleeping on your left or right side, sometimes curled into a fetal pose.
The National Sleep Foundation notes that about 60 percent of adults favor a side position, 30 percent a back position, and the rest sleep prone. Each position affects the spine, airway, and jaw differently.
Impact on Jaw and Sleep
When you lie down, gravity shifts the relationship between your jaw and skull. In a supine position, your jaw can fall backward, narrowing the airway. If the airway flutters or collapses, your brain may trigger micro-arousals to activate muscles, including the jaw. A 2024 clinical review by Patil and colleagues argues that the jaw reflex helps keep the airway open. For more understanding of how bruxism can affect other areas of your body, you might want to read about the jaw-back connection.
Side sleeping changes things. The pillow may press the mandible sideways, altering bite alignment. Lateral force can strain the TMJ, especially if pillow height twists your neck.
Prone sleeping requires turning the head to one side for breathing. This rotation twists the lower jaw, often pushing it forward. Some small studies suggest this shift might relieve apnea events but can also tighten one side of the jaw muscles.
Posture also influences sleep quality. Supine positions often produce more REM sleep but allow the tongue to slide backward, worsening snoring and apnea in those with OSA. Lateral positions reduce that risk, possibly lowering bruxism-triggering arousals. However, no single position is perfect. You have to balance airway comfort against jaw muscle load.
In adults with diagnosed OSA, a 2024 study by Kuang, Lobbezoo, and Li recorded muscle activity in various sleeping postures and found that bruxism events decreased by about 23 percent in side sleeping compared to supine. However, results varied, showing that anatomy and pillow type still matter.
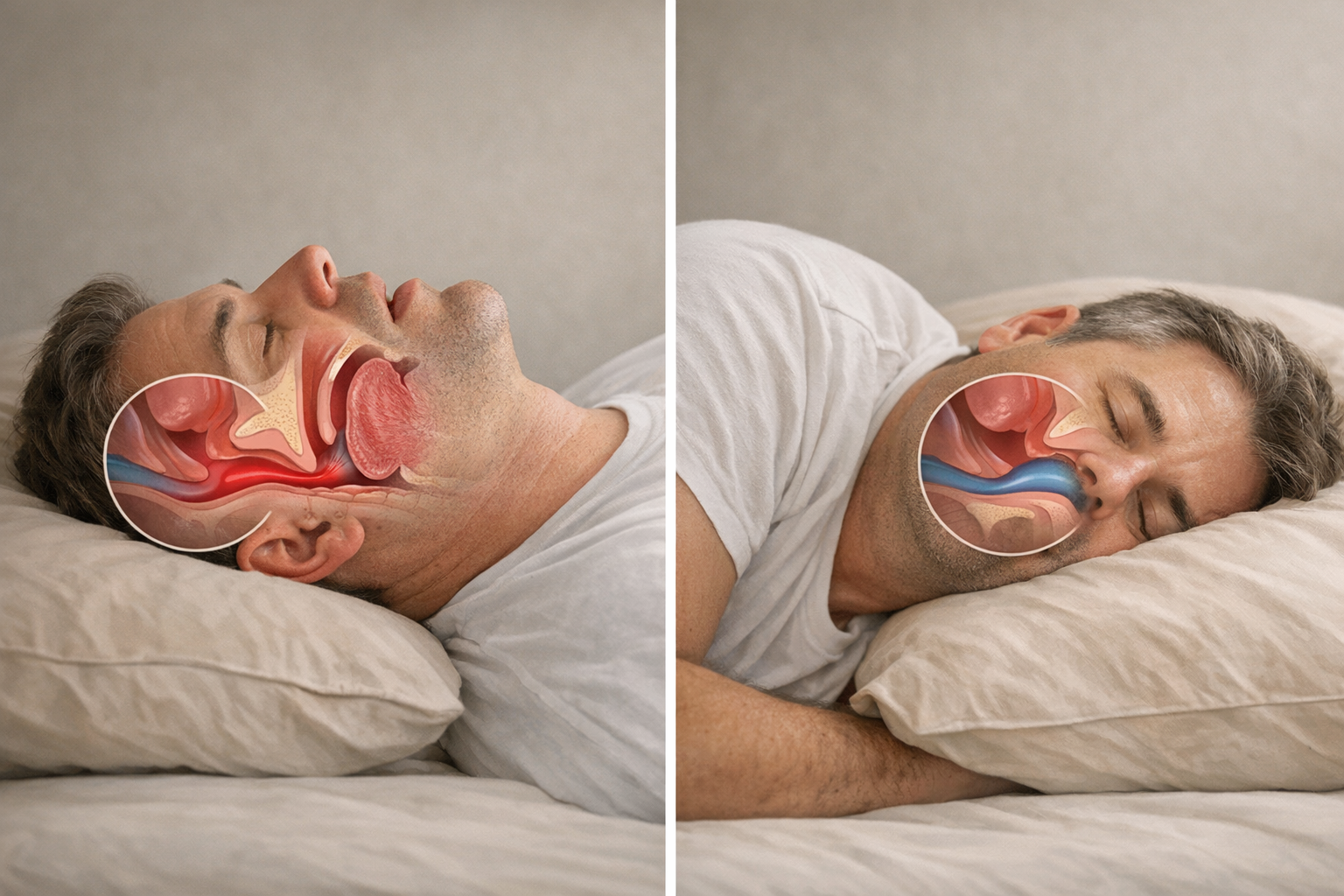
Sleep Positions and Their Role in Jaw Pain
Supine Position and Jaw Pain
Back sleeping often gets promoted for spinal alignment, yet it can stress your jaw. When you lie supine, gravity pulls the mandible backward toward the throat, compressing the TMJ and stressing the masseter and temporalis muscles.
A randomized controlled trial published in the Journal of Sleep Research explored a twist on the classic supine posture. Zhong, Li, and Zou placed participants in a low-Fowler’s position, elevating the head and torso by about 30 degrees, while giving half of them methazolamide to reduce carbonic anhydrase activity. The control group stayed flat. Over two weeks, the inclined group experienced a significant dip in bruxism episodes compared to the flat-supine group, suggesting that head elevation eases airway obstruction and calms jaw reflexes.
Flat supine position also magnifies snoring noise, triggering micro-arousals resolved by brief muscle contractions, including jaw muscle bursts. These contractions may not wake you but can leave your jaw tired by morning.
Side Sleeping and Bruxism
Side sleeping is common but not free from jaw issues. Lateral positions vary depending on which side faces the pillow, pillow height, and shoulder width.
The same 2024 work by Kuang et al. measured surface electromyography (EMG) of the masseter overnight. They observed that jaw-clenching bursts clustered after REM periods when subjects shifted sides. Researchers suspect the brief jaw realignment needed to change sides sparks reflex contractions.
Side sleeping can also strain the jaw due to direct mechanical pressure. If the pillow presses the mandible upward, it pushes the condyle deeper into the joint socket. People who habitually sleep on one side often report morning pain on that side. The American Dental Association advises using a pillow thick enough to keep the neck straight but soft enough to reduce cheek compression.
Many clinicians prefer side sleeping over back sleeping for people with OSA, because maintaining airway patency is crucial. A quick posture check: if your ear, shoulder, and hip form a straight line when you lie on your side, you're likely reducing airway collapse without overloading the jaw.

Exploring the Link Between Bruxism and Sleep Disorders
Bruxism and Obstructive Sleep Apnea
Obstructive sleep apnea is a breathing disorder marked by repeated airway blockages. Many patients with OSA unknowingly grind their teeth. The big question is which comes first. Current evidence suggests the two are partners rather than separate issues.
Patil and colleagues proposed an “airway guarding theory” where bruxism follows a partial airway collapse. The jaw thrusting during grinding moves the tongue base forward, opening the airway. In this view, bruxism is less a bad habit and more an emergency reflex. For a deeper dive into how bruxism and sleep disorders intertwine, see our comprehensive guide on what causes teeth grinding.
Magnetic resonance imaging supports the mechanical link. In a 2025 cross-sectional imaging study, Topaloglu Yasan et al. viewed TMJs in sleep bruxers and found that condylar position shifted posteriorly after apnea events. This shift aligns with teeth clenching because masseter contraction would logically lift the mandible to open the airway.
Even so, not every grinder has OSA. The Sleep Foundation points out that mild bruxism can exist without any breathing disorder, especially in younger adults who may grind in response to stress or caffeine.
Other Sleep Disorders
Restless legs syndrome (RLS) and periodic limb movement disorder share some neurochemical pathways with bruxism. Both involve dopamine activity surges and micro-arousals that disrupt sleep structure. No major trials directly link posture in RLS to jaw pain, but clinicians suspect that tossing and turning to calm restless limbs can increase jaw muscle tone.
Insomnia also worsens the issue. Lying awake often leads to subconscious clenching or grinding. Over the night, that static contraction exhausts the muscle, making morning pain feel worse.
The lesson: if you have persistent jaw pain, consider a full sleep evaluation rather than just a dental checkup. An overnight sleep study can identify breathing pauses, leg movements, and arousals that might be disturbing you.
Managing Jaw Pain and Bruxism
Lifestyle Changes
Before jumping to splints or medications, tweak the basics. Many don't realize how small changes can quiet an overactive jaw.
- Posture hygiene. Keep screens at eye level, shoulders relaxed, and your tongue on the roof of your mouth during the day. Good daytime posture trains the jaw into a neutral resting position.
- Stress management. You can't eliminate every deadline, but you can add breathing exercises or a short evening walk. The Cleveland Clinic notes that calming your nervous system before bed reduces nighttime clenching risk.
- Limit stimulants. High caffeine and alcohol intake make sleep lighter and jaw activity higher. A simple rule: no coffee after 2 p.m. and limit alcohol to one drink with dinner. For further reading on the effects of alcohol, check out how alcohol can affect teeth grinding.
- Optimize your pillow. For side sleepers, the pillow should fill the space from your ear to your shoulder tip. For back sleepers, a thinner pillow keeps the jaw from pitching forward.
A combined approach can also include kinesiology taping on the masseter or along the jawline. In the randomized study by Coşkun Karataş and Menek, taping plus targeted exercise lowered pain scores by 47 percent after four weeks.
Therapeutic Interventions
If lifestyle tweaks aren't enough, dental and physical therapy options are available.
Occlusal splints. The classic acrylic night guard separates the upper and lower teeth. That buffer prevents enamel wear, but evidence on pain relief is mixed. A 2025 randomized controlled study compared splints with two exercise regimens. Karabicak and colleagues found that jaw-and-posture exercises performed as well as splints in reducing bruxism bursts. The takeaway: splints protect teeth, but they don't stop muscle activity entirely. For more information on choosing the right splint, explore our comparison of occlusal vs night guards.
Jaw exercises. Simple isometric holds and controlled openings strengthen stabilizer muscles and improve blood flow. Pairing jaw exercises with neck and shoulder retraining provides better relief than jaw work alone, supporting the integrated posture theory.
Physical therapy and massage. Trigger point release in the masseter and temporalis can loosen stiff tissue. Some therapists use dry needling to deactivate chronic knots, though evidence is still emerging.
Medication. Low-dose benzodiazepines or muscle relaxants may reduce nocturnal activity, but they have side effects and can worsen OSA. Most specialists reserve them for short trials.
Botulinum toxin. Small doses injected into the masseter reduce muscle force. The downside is temporary weakness when chewing tough foods, and repeated injections every three to four months.
Choosing a therapy often depends on your goals. If you mainly worry about tooth damage, a splint makes sense. If pain and muscle fatigue dominate, exercise and physical therapy might provide more relief.
The Role of Technology in Diagnosing Bruxism
Advancements in Diagnostic Tools
Diagnosing sleep bruxism used to rely on partner complaints and morning jaw ache. Today, clinicians can use EMG pads to record every muscle twitch. Portable EMG recorders can be used at home, logging jaw contractions across the night without a bulky sleep-lab setup. For those interested in tech solutions, our article on managing bruxism with wearable tech offers insights into emerging tools.
Zeb and co-authors built a multi-sensor array that captures EMG data while also noting body posture using accelerometers. Their machine-learning model identified bruxism events with 92 percent accuracy across different sleeping positions. This accuracy suggests future wearables could coach you in real time, gently buzzing when jaw muscles overload.
Future Directions
Combining positional sensors, pulse oximetry, and jaw EMG may soon create an all-in-one sleep bite guard. Imagine a slim mouthguard that tracks grinding, checks breathing pauses, and nudges you to roll onto your side if your airway collapses. Several start-ups are already exploring this space. As machine learning improves, these tools could move from specialist clinics to your bedside drawer.
Conclusion
Jaw pain after sleeping is not just a dental quirk. It can indicate that your sleep posture, airway health, and stress levels are misaligned. Evidence from randomized trials shows that back sleeping without head elevation can worsen bruxism, while side sleeping reduces airway collapse but may press the jaw if the pillow is incorrect. Bruxism often partners with disorders like obstructive sleep apnea, so addressing one without considering the other can miss the mark.
Your action plan: check your pillow height, try a gentle head incline if you sleep on your back, and add jaw relaxation exercises to your bedtime routine. If pain persists, consult a dentist or sleep specialist about an occlusal splint or a sleep study. While technology is improving at detecting nighttime grinding, the simplest solution may be adjusting to a better-supported position tonight.