TMJ Ice or Heat? How to Choose the Right Therapy for Jaw Pain Relief
You're lying in bed with your jaw throbbing after another long day of unconscious clenching, and you're wondering: should I grab an ice pack or a heating pad? It's one of the most common questions people with TMJ disorders ask, and the answer isn't as simple as picking one over the other. Both heat and ice have legitimate roles in managing TMJ pain, but using the wrong one at the wrong time can actually make things worse.
Here's what the research actually says about heat therapy, ice therapy, and how to use each one effectively for TMJ and jaw pain relief.
TMJ Ice or Heat: Which One Should You Use?
The short answer is that it depends on what's happening in your jaw right now. Ice and heat do fundamentally different things to your tissues, and matching the right therapy to your specific situation is what makes the difference between relief and frustration.
Use ice when you have acute inflammation, a recent injury or flare-up, or noticeable swelling around the jaw joint. Ice constricts blood vessels, reduces swelling, and numbs pain signals. Think of it as your first responder for sudden, sharp TMJ episodes.
Use heat when you have chronic muscle tension, jaw stiffness, or dull aching pain from clenching and grinding. Heat increases blood flow, relaxes tight muscles, and improves the elasticity of connective tissues around the temporomandibular joint. This is your go-to for the everyday grind of TMJ discomfort.
A 2015 study published in the Journal of Physical Therapy Science found that superficial heat application significantly reduced pain and improved range of motion in patients with myofascial pain dysfunction. Meanwhile, cold therapy has well-established benefits for reducing acute inflammatory responses across musculoskeletal conditions, including the TMJ.
When Heat Therapy Works Best for TMJ
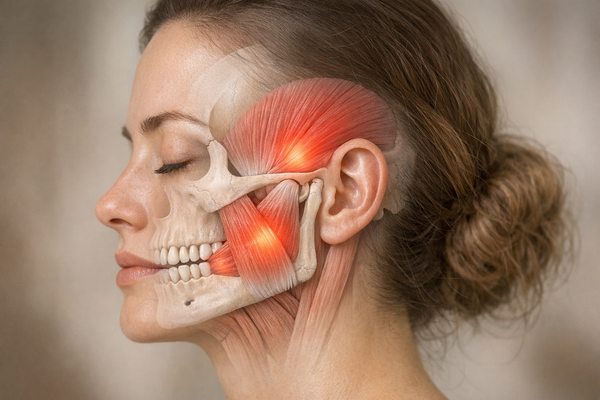
For the majority of people dealing with TMJ pain, heat therapy will be the more useful tool. That's because most TMJ discomfort stems from chronic muscle tension rather than acute joint inflammation. If you're grinding your teeth at night or clenching during the day, the muscles around your jaw (the masseter, temporalis, and lateral pterygoid) are overworked and tight. Heat directly addresses that problem.
Heat therapy works by:
- Increasing blood flow to the jaw muscles, which delivers oxygen and nutrients needed for tissue repair
- Relaxing muscle fibers that have been in sustained contraction
- Reducing pain signals by activating thermoreceptors that compete with pain receptors at the spinal cord level (this is called the gate control theory of pain)
- Improving the viscoelastic properties of connective tissue, making it easier to stretch and move your jaw
Research from the American Academy of Orofacial Pain supports heat application as a first-line home therapy for myogenous (muscle-origin) TMJ pain. It's simple, it's low-risk, and for many people it provides meaningful relief within minutes.
Moist Heat vs. Dry Heat for TMJ
Not all heat is created equal when it comes to your jaw. Moist heat penetrates deeper into muscle tissue than dry heat, and multiple studies have demonstrated its superiority for musculoskeletal pain conditions.
A study in the Journal of Clinical and Diagnostic Research (2014) compared moist heat and dry heat for muscle pain and found that moist heat achieved the same therapeutic effect in roughly half the application time. The moisture helps conduct heat more efficiently through the skin and into the underlying muscle layers.
For TMJ specifically, moist heat for TMJ pain is particularly effective because the masseter and temporalis muscles sit relatively close to the skin surface, making them responsive to topical heat application. A warm, damp towel or a microwaveable moist heat pack can reach these muscles more effectively than a standard dry heating pad.
How to Apply a Warm Compress for Jaw Pain
Here's a step-by-step approach to using a hot compress for TMJ relief:
- Prepare your compress. Dampen a clean towel with warm water and wring it out so it's moist but not dripping. Alternatively, use a microwaveable moist heat pack designed for facial use. The temperature should be comfortably warm (around 104-113 degrees Fahrenheit), not hot enough to burn.
- Position it correctly. Place the compress directly over the jaw joint, which sits just in front of your ear. You can also extend coverage forward along the jawline and upward to the temple area to reach the temporalis muscle.
- Hold for 15-20 minutes. This is the sweet spot recommended by most clinical guidelines. Less than 10 minutes won't achieve full muscle relaxation. More than 20 minutes provides diminishing returns and increases the risk of skin irritation.
- Combine with gentle stretching. While the heat is applied, or immediately after, try slowly opening your mouth and moving your jaw side to side. The warmed muscles will be more responsive to gentle stretching exercises.
- Repeat as needed. You can safely apply heat 3-4 times per day. Many people find it most helpful first thing in the morning (when the jaw is stiff from overnight clenching) and before bed.
If you're also using a mouth guard for TMJ, applying heat before bed can help relax the muscles before you put your guard in, potentially reducing clenching intensity overnight.
When to Use Ice for TMJ Pain
Ice therapy gets its moment when inflammation is the primary issue. This typically means:
- The first 24-72 hours after a TMJ flare-up or injury
- After dental procedures that affect the jaw joint
- When you notice visible swelling around the jaw area
- After particularly intense episodes of clenching or grinding that leave the joint feeling hot or inflamed
Cold therapy reduces inflammation by constricting blood vessels (vasoconstriction), which limits the amount of inflammatory fluid that accumulates in the tissue. It also slows nerve conduction velocity, which is a clinical way of saying it numbs the pain.
How to Ice TMJ Pain Properly
- Wrap your ice pack. Never apply ice directly to the skin over your jaw. Use a thin cloth or towel as a barrier. The skin over the TMJ area is thin, and direct ice contact can cause frostbite or nerve damage.
- Apply for 10-15 minutes maximum. Icing TMJ for longer than 15 minutes can trigger a paradoxical response where your body sends more blood to the area to prevent tissue damage, actually increasing inflammation.
- Wait at least 45-60 minutes between applications. This gives the tissue time to return to normal temperature and prevents cold-related tissue injury.
- Focus on the joint itself. Place the ice pack just in front of your ear, directly over the TMJ. If both sides are affected, alternate or use two packs simultaneously.
Heat vs. Ice for TMJ: A Direct Comparison
Since "is ice or heat better for TMJ" is the question so many people are trying to answer, here's a clear breakdown of when to choose each approach:
Choose heat when:
- Your jaw pain is caused by muscle tension or chronic clenching
- You feel stiffness more than sharp pain
- Your symptoms are ongoing and not from a recent injury
- You want to improve jaw mobility before exercises or stretching
- Morning jaw stiffness is your primary complaint
Choose ice when:
- You have a sudden, acute flare-up with noticeable swelling
- Your jaw joint feels hot to the touch
- You're within 72 hours of a jaw injury or dental procedure
- Sharp, stabbing pain is your primary symptom
- Anti-inflammatory medication alone isn't controlling your symptoms
Use both (contrast therapy) when:
- You have a mix of chronic tension and periodic inflammatory flare-ups
- Heat alone feels good initially but doesn't fully resolve symptoms
- Your healthcare provider has recommended alternating therapy
Contrast therapy involves alternating between heat and cold, typically 3-4 minutes of heat followed by 1 minute of cold, repeated for 20-30 minutes. A 2017 study in the Journal of Oral Rehabilitation found that alternating hot and cold compresses for TMJ provided greater pain reduction than either modality alone in patients with combined myogenous and arthrogenous TMD.
Heat Therapy for Trismus and Limited Jaw Opening
Trismus (restricted jaw opening) is a common complication of TMJ disorders, and heat therapy plays a particularly important role here. When the muscles around the jaw become chronically contracted, they physically limit how far you can open your mouth. Heat directly addresses this by improving the extensibility of muscle and connective tissue.
Clinical protocols for trismus management consistently include heat application as a preparatory step before jaw stretching exercises. The standard approach is to apply moist heat for 15-20 minutes, then immediately perform progressive jaw opening exercises while the tissues are warm and pliable.
A systematic review in the British Journal of Oral and Maxillofacial Surgery identified heat therapy combined with exercises as one of the most effective conservative treatments for trismus associated with TMJ disorders. The key is consistency: doing this once won't fix trismus, but a daily routine of heat plus stretching over several weeks can produce meaningful improvements in jaw opening.
Choosing the Right Heat Pad for Jaw Pain
Not every heating device works well for the TMJ area. The jaw joint sits in an awkward spot for standard rectangular heating pads, and you need something that conforms to the contours of your face. Here are the options worth considering:
Microwaveable moist heat packs: These are the top choice for most people. Products like Bed Buddy or TheraPearl make packs specifically shaped for facial use. They provide moist heat, conform to the jaw area, and are reusable. Heat for 60-90 seconds in the microwave (follow the specific product instructions) and apply with a thin cloth barrier if needed.
Warm towel method: The simplest approach. Run a clean washcloth under hot tap water, wring it out, and apply. The downside is that it cools quickly (5-7 minutes), so you'll need to reheat it midway through your session. The upside is that it's free and always available.
Electric moist heating pads: Some electric heating pads have a moist heat setting that uses a sponge insert. These maintain consistent temperature, which is an advantage over microwaveable packs. Look for one with a small enough form factor to use comfortably on your face.
Warm water soak (for whole-face relief): Soaking a large towel in warm water, wringing it out, and draping it over your entire lower face can provide broader relief if you have bilateral TMJ pain. Some people find this approach more relaxing than a targeted compress.
Combining Heat and Ice with Other TMJ Treatments
Heat and cold therapy work best as part of a broader TMJ treatment approach rather than as standalone solutions. Here's how to integrate them effectively:
With night guards: If you wear a night guard for TMJ, apply heat to your jaw muscles for 15 minutes before inserting your guard at bedtime. This relaxes the muscles and may reduce the intensity of nocturnal clenching. In the morning, if you wake up with jaw stiffness, another round of heat before your morning routine can help.
With jaw exercises: Always apply heat before doing TMJ stretching or strengthening exercises. Cold muscles are more prone to strain, and heat-primed muscles respond better to therapeutic stretching. Save ice for after exercises if the joint feels inflamed or sore from the movement.
With medications: Heat and ice are safe to use alongside over-the-counter anti-inflammatory medications like ibuprofen. In fact, combining topical thermal therapy with oral anti-inflammatories addresses pain through two different mechanisms simultaneously, often providing better relief than either approach alone.
With stress management: Since stress is a major driver of jaw clenching, using heat application as part of a relaxation routine can provide both physical and psychological benefits. The warmth itself triggers a parasympathetic (relaxation) response, which can help break the stress-tension-pain cycle that fuels so much TMJ suffering.
When Heat and Ice Aren't Enough
Thermal therapy is a valuable tool, but it has limits. If you've been consistently applying heat or ice for two weeks without meaningful improvement, or if your symptoms are getting worse, it's time to see a healthcare provider. This is especially true if you experience:
- Locking of the jaw (unable to open or close fully)
- Changes in your bite alignment
- Ear pain, ringing, or hearing changes alongside jaw symptoms
- Numbness or tingling in your face
- Pain that wakes you from sleep regularly
These symptoms may indicate structural issues with the TMJ disc or joint that require professional evaluation and treatment beyond home remedies.
The Bottom Line
For most people dealing with day-to-day TMJ pain from clenching and grinding, heat therapy (especially moist heat) is the better default choice. It relaxes the overworked muscles that are usually responsible for the pain and stiffness. Save ice for acute flare-ups with clear inflammation or swelling. And don't overlook contrast therapy, alternating between the two, which research suggests may outperform either one alone.
The best part about heat and ice therapy is that they're low-cost, low-risk, and available right now. You don't need a prescription, you don't need an appointment, and you can start tonight. Grab a warm towel, press it against your jaw, and give those overworked muscles the break they've been begging for.