Jaw Pain Treatment: Evidence-Based Options That Actually Work
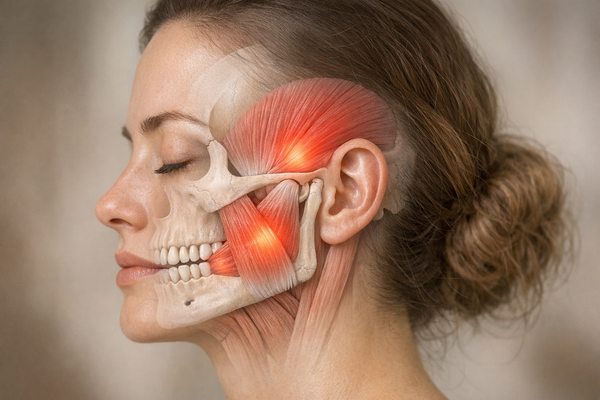
Why Your Jaw Hurts (And Why Generic Advice Doesn't Cut It)
Jaw pain is one of those problems that sounds simple until you're the one dealing with it. You can't eat comfortably, you wake up with your face aching, and every yawn feels like a gamble. The term "TMJ disorder" (or TMD) gets thrown around a lot, but it covers a wide range of conditions affecting the temporomandibular joint, the muscles of mastication, or both. That range is exactly why jaw pain treatment needs to be more targeted than "just relax."
According to the National Institute of Dental and Craniofacial Research, TMD affects over 10 million Americans. A 2020 study published in the Journal of Dental Research (the OPPERA study) found that the annual incidence of first-onset TMD was 3.9% among adults aged 18 to 44. That's not a small number. And yet, a lot of people cycle through treatments that don't address what's actually going on.
This article covers the full spectrum of jaw pain management, from things you can do tonight to professional interventions backed by clinical evidence. The goal is to help you figure out which options match your situation, not just hand you a list.
Home Remedies for Jaw Pain Relief
Before spending money on appointments, it's worth trying the conservative approaches that clinical guidelines actually recommend as first-line treatment. The American Association for Dental Research (AADR) specifically recommends starting with reversible, noninvasive therapies.
Heat and Cold Therapy
Applying moist heat to the side of your face can relax the muscles that tighten around the jaw joint. A warm towel or a microwavable heat pack applied for 15 to 20 minutes can reduce muscle spasm and improve blood flow. Cold packs work better for acute inflammation, especially if your jaw pain started after an injury or dental procedure. Alternating between the two is a common physical therapy recommendation. For a deeper look at the research behind this, check out our guide on how heat treatment helps relieve TMJ pain.
Jaw Exercises and Stretches
A 2010 study in the Journal of Oral Rehabilitation found that simple jaw stretching exercises performed three times daily reduced pain and increased mouth opening in TMD patients within eight weeks. The key exercises include:
- Resisted opening: Place your thumb under your chin and gently push downward while opening your mouth. Hold for 5 seconds.
- Resisted closing: Place your thumb under your chin and your index fingers on the ridge between your chin and lower lip. Push gently while closing your mouth.
- Controlled opening: Slowly open your mouth as wide as feels comfortable. Hold for 5 seconds, then slowly close.
- Side-to-side movement: Place a thin object (like a tongue depressor) between your front teeth. Slowly shift your jaw from left to right.
The important part is consistency. These exercises aren't dramatic, but they build stability in the joint over time.
Soft Diet and Jaw Rest
This one sounds obvious, but it's overlooked more than you'd think. Giving your jaw a break from chewy, crunchy, or hard foods reduces the load on inflamed tissues. That doesn't mean a permanent liquid diet. It means being strategic: skip the beef jerky and whole apples for a few weeks while your jaw calms down. Cutting food into smaller pieces and avoiding extreme mouth opening (no giant sandwiches) makes a real difference.
Stress Management
The connection between jaw clenching and stress is well documented. A 2018 systematic review in the Journal of Oral and Facial Pain and Headache confirmed that psychological stress is a significant risk factor for both bruxism and TMD. If you're clenching during the day, cognitive behavioral techniques like awareness training can help. The basic version: set periodic reminders to check in with your jaw. Are your teeth touching? Is your jaw tense? The resting position should be lips together, teeth slightly apart, tongue resting on the roof of your mouth.
Over-the-Counter Jaw Pain Remedies
When home strategies aren't enough to soothe jaw pain on their own, OTC options can bridge the gap.
Anti-Inflammatory Medications
NSAIDs like ibuprofen (Advil, Motrin) are the go-to for jaw pain because they address both pain and inflammation. A 2015 Cochrane review found moderate evidence supporting the use of NSAIDs for TMD pain management. The standard dosing of 400 to 600 mg every 6 to 8 hours, taken with food, is typically effective for mild to moderate jaw discomfort. Naproxen (Aleve) lasts longer per dose and may be preferable if you're dealing with overnight pain. Acetaminophen (Tylenol) helps with pain but doesn't target inflammation, so it's a second choice for most jaw problems.
Topical Options
Topical menthol or capsaicin creams applied to the jaw area can provide localized relief without systemic side effects. Some people find topical diclofenac gel helpful, though it's typically available by prescription in the US. Over-the-counter lidocaine patches, trimmed to fit along the jawline, are another option for short-term pain management.
How to Treat Jaw Pain with Professional Help
If you've been managing jaw discomfort for more than a few weeks without improvement, professional treatment is the logical next step. Here's what the evidence supports.
Physical Therapy
Physical therapy for TMD is one of the best-supported professional treatments available. A 2019 systematic review in Clinical Rehabilitation found that manual therapy combined with exercise therapy produced significant reductions in pain and improvements in maximum mouth opening. A good TMJ-focused physical therapist will assess your posture, neck mobility, and jaw mechanics together, because they're all connected. Techniques typically include manual joint mobilization, myofascial release, dry needling of trigger points, and a progressive home exercise program. If your jaw pain is linked to muscle tension (which is the most common scenario), PT is often where the real progress happens.
Custom Oral Appliances
Stabilization splints (also called occlusal splints or bite guards) are the most commonly prescribed professional treatment for TMD. They work by reducing clenching forces and preventing tooth contact during sleep. A 2017 meta-analysis in the Journal of Oral Rehabilitation found that stabilization splints provided moderate pain reduction compared to no treatment. The key word here is "custom." Generic one-size-fits-all devices are hit or miss. A properly fitted splint made from impressions of your teeth distributes force evenly and keeps your jaw in a position that reduces strain on the joint. For help choosing the right device, see our comparison of the best mouth guards for TMJ relief.
Botox Injections for Jaw Pain
Botulinum toxin injections into the masseter and temporalis muscles have become a legitimate jaw pain therapy, not just a cosmetic trend. A 2019 randomized controlled trial in Neurology found that botulinum toxin significantly reduced bruxism episodes and associated pain compared to placebo. The injections work by partially relaxing overactive jaw muscles, reducing clenching force by roughly 20 to 30 percent. Effects typically last three to four months. It's not a cure, but for people with severe muscle-driven jaw pain that hasn't responded to other approaches, it can be a turning point. We cover this in detail in our article on Botox for bruxism and teeth grinding.
Prescription Medications
For severe TMJ pain treatment, doctors may prescribe muscle relaxants like cyclobenzaprine, typically for short-term use (two to four weeks). A 2003 study in Cranio found that low-dose cyclobenzaprine taken at bedtime reduced pain intensity and improved sleep quality in TMD patients. Tricyclic antidepressants at low doses (like amitriptyline 10 to 25 mg at bedtime) are sometimes used for chronic jaw pain, as they modulate pain pathways independent of their antidepressant effects.
Can a Mouth Guard Cause Jaw Pain?
This is a question that comes up more than most dentists acknowledge. You get a night guard to protect your teeth, and suddenly your jaw pain gets worse. What's going on?
There are several reasons a mouth guard can cause or worsen jaw pain:
- Poor fit: An ill-fitting guard forces your jaw into an unnatural position all night. Over hours of wear, this can strain the TMJ and surrounding muscles rather than relieve them.
- Wrong type of guard: Soft, rubbery night guards can actually increase clenching in some people. Research suggests that the squishy texture triggers a chewing reflex, leading to more muscle activity, not less.
- Incorrect bite alignment: If the guard doesn't distribute force evenly across your bite, it can create premature contacts, points where your teeth hit the guard first and your jaw compensates by shifting or clenching harder.
- Adjustment period: Some temporary jaw soreness when you first start wearing a guard is normal. But if it persists beyond the first week or two, the guard likely needs adjustment.
If your mouth guard is causing jaw pain, don't just tough it out. Go back to whoever made it and ask for an adjustment. If it's an over-the-counter boil-and-bite guard, consider upgrading to a custom device. For a full breakdown of why this happens and what to do about it, read our article on why teeth and jaw hurt after wearing a night guard.
Jaw Pain Prevention: Stopping the Cycle
Treating jaw pain is important, but preventing it from recurring is the real goal. Most TMD is episodic, meaning it flares up, improves, and flares again. Breaking that cycle requires addressing the underlying drivers.
Address Bruxism Directly
If you grind your teeth at night, that repetitive overloading of the jaw joint is likely the primary engine behind your pain. Understanding what causes teeth grinding can help you target the right interventions, whether that's stress reduction, sleep hygiene improvements, or an oral appliance.
Posture and Ergonomics
Forward head posture, the kind that comes from hunching over a laptop all day, changes the resting position of your jaw and increases strain on the TMJ. A 2014 study in the Journal of Physical Therapy Science found a significant correlation between forward head posture and TMD symptoms. Simple fixes include adjusting your monitor to eye level, taking regular breaks from screen work, and strengthening your neck and upper back muscles. The connection between your jaw and the rest of your body is more significant than most people realize. Jaw tension can even contribute to back pain through the kinetic chain.
Sleep Quality
Poor sleep and jaw pain feed each other in a vicious cycle. Sleep disruption increases muscle tension and pain sensitivity, which worsens bruxism, which further disrupts sleep. Prioritizing sleep hygiene, including consistent sleep and wake times, a cool and dark bedroom, and limiting screens before bed, can meaningfully reduce nighttime clenching.
When to See a Doctor for Jaw Pain
Most jaw pain improves with conservative treatment within four to six weeks. But some situations call for professional evaluation sooner rather than later:
- Jaw locking: If your jaw gets stuck open or closed, even intermittently, that suggests internal derangement of the joint disc.
- Significant changes in your bite: If your teeth no longer come together the way they used to, something structural may have changed.
- Pain that worsens despite treatment: If you've been consistent with home remedies and OTC options for four weeks and your pain is getting worse, not better, it's time for imaging and a professional assessment.
- Ear pain or hearing changes: The TMJ sits directly in front of the ear canal. Dysfunction there can cause ear pain, tinnitus, or a feeling of fullness in the ear.
- Pain after trauma: If your jaw pain started after a blow to the face, a fall, or a car accident, get evaluated to rule out fracture or joint damage.
- Headaches that don't respond to headache treatment: Chronic headaches centered in the temples are frequently referred pain from the jaw muscles. If your headaches haven't responded to typical treatments, a TMJ evaluation may provide the answer.
Start with your dentist or primary care doctor. From there, referrals might go to an oral and maxillofacial specialist, a TMJ-focused physical therapist, or an orofacial pain specialist, depending on your specific situation.
Advanced Treatments for Severe or Chronic Jaw Pain
For the subset of patients whose jaw pain doesn't respond to conservative approaches, additional options exist. These are generally reserved for cases that have failed at least three to six months of standard treatment.
- Arthrocentesis: A minimally invasive procedure where fluid is injected into the joint space to wash out inflammatory debris and break up adhesions. A 2018 systematic review in the International Journal of Oral and Maxillofacial Surgery found success rates of 80 to 90 percent for improving jaw opening and reducing pain.
- Trigger point injections: Local anesthetic injected directly into muscle trigger points can break the pain-spasm-pain cycle in chronic cases.
- Arthroscopy: A small camera inserted into the joint allows direct visualization and treatment of internal problems. Recovery is faster than open surgery, and outcomes are generally favorable for disc displacement issues.
- Open joint surgery: Reserved for severe structural damage, ankylosis, or tumors. This is rare and typically a last resort.
The AADR's position statement is clear: irreversible treatments (including surgery and permanent bite adjustments) should only be considered after reversible options have been thoroughly tried. Most people with TMD never need surgery.
Building Your Jaw Pain Treatment Plan
The most effective approach to treating jaw pain combines multiple strategies rather than relying on a single solution. A reasonable starting framework looks like this:
- Weeks 1 through 2: Soft diet, heat/cold therapy, jaw exercises, NSAIDs as needed, stress awareness.
- Weeks 3 through 4: If not improving, add a custom oral appliance and consider physical therapy.
- Months 2 through 3: If still struggling, discuss prescription options (muscle relaxants, Botox) with your provider.
- Month 4 and beyond: If pain persists, seek evaluation from a TMJ specialist for advanced diagnostics and treatment options.
Jaw pain is treatable. The research consistently shows that the vast majority of TMD cases, roughly 85 to 90 percent according to the NIDCR, improve with nonsurgical management. The key is matching the right treatment to your specific situation and giving each approach enough time to work before moving on. If one remedy for jaw pain doesn't deliver results, that's not failure. It's information that points you toward what will.