Understanding Sleep Disorders and Their Connection to Bruxism
Explore how sleep disorders like apnea relate to bruxism and worsen teeth grinding.

Many people grind through stressful days, but a surprising number continue this habit after the lights go out. That nighttime jaw workout is called bruxism, and recent research shows it is more than a dental issue. It can be linked with serious sleep disorders, especially obstructive sleep apnea (OSA), creating a feedback loop that affects both sleep quality and oral health. This article explores the latest findings, why your molars might be suffering, and how to break the cycle of bruxism and sleep disorders.
We'll rely on peer-reviewed studies and plain language. By the end, you'll understand how bruxism and sleep disorders interact, their impact on both kids and adults, and steps you can take to protect your smile while you sleep.
What is Bruxism?
Bruxism is the medical term for teeth grinding or jaw clenching. It acts like an intense workout for your jaw muscles and typically appears in two forms: awake bruxism and sleep bruxism. Sleep bruxism receives more research attention because it occurs when you're unconscious, making it harder to notice and control. The Standardised Tool for the Assessment of Bruxism defines it as “masticatory muscle activity during sleep” that is distinct from disorders like epilepsy or rhythmic movement disorder.
Types of Bruxism
Awake bruxism often occurs with stress, concentration, or poor posture. You might catch yourself tightening your jaw while working on emails.
Sleep bruxism happens during light non-REM phases and sometimes during REM. Because you're asleep, you might not hear or feel it. According to Leung et al., muscle activity during sleep can spike to six times the force of normal chewing.
Common Symptoms
- Audible grinding noises reported by a partner
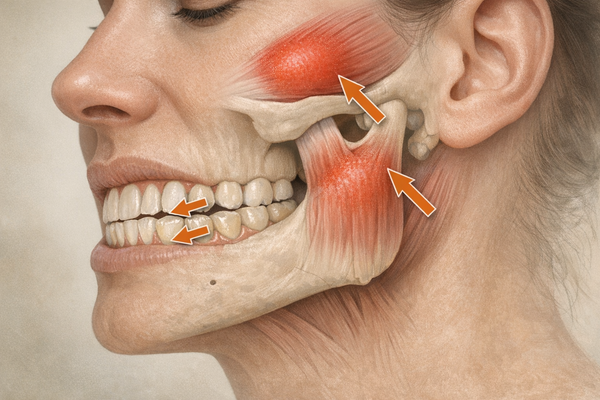
- Morning jaw or temple pain
- Flattened or cracked teeth
- Headaches beginning near the ears
- Limited jaw opening or clicking
These symptoms are usually harmless but can indicate a larger sleep issue. If bruxism appears with daytime sleepiness, dry mouth, or snoring, it might signal an underlying sleep disorder.
The Link Between Bruxism and Sleep Disorders
Teeth grinding and disturbed sleep often occur together, leading researchers to explore their relationship. The short answer is they often come hand-in-hand. A systematic review by García Doblado et al. analyzed data from 1,300 patients, finding that up to half of those diagnosed with OSA also showed signs of sleep bruxism. This is significantly higher than the 8–10 percent bruxism rate in the general population. Another meta-analysis by Doblado, Barrera, and Pastor confirmed this overlap, suggesting shared risk factors such as airway obstruction and neurotransmitter changes could link the two.
Bruxism and Sleep Apnea
In obstructive sleep apnea, throat muscles collapse, blocking airflow and causing the brain to wake you up for air. These micro-arousals often align with bursts of tooth grinding observed in polysomnography (the gold-standard sleep study). Some scientists suggest bruxism might be the body's attempt to reopen the airway by moving the jaw forward. A study by Przegrałek et al. proposed that mild grinding episodes might act like mini-resuscitations for moderate apnea cases.
Key numbers to remember:
- Up to 50% of people with OSA grind their teeth during sleep
- Bruxism episodes often occur within 5–10 seconds of an apnea-related arousal
- Men with severe OSA have three times the odds of bruxism compared to healthy sleepers, according to the American Sleep Association
Other Sleep Disorders
While apnea often gets the most attention, bruxism can also be linked to other sleep disorders:
- Restless Legs Syndrome – Frequent limb movements can lead to partial awakenings that coincide with jaw contractions.
- Insomnia – Fragmented sleep increases muscle activity and stress hormone levels, both of which can lead to grinding.
- REM Behavior Disorder – Acting out dreams involves full-body movement, including the jaw.
The Sleep Foundation notes that overlap is common enough that dentists now screen for sleep complaints, and sleep doctors inquire about tooth wear. Essentially, bruxism rarely occurs in isolation when sleep quality declines.

How Bruxism Exacerbates Sleep Disorders
Once bruxism is part of the equation, it can worsen existing sleep disorders. When jaw muscles contract, heart rate and sympathetic nerve activity increase. This "fight or flight" response pulls you into lighter sleep stages, leading to more apnea events and grinding. It's like hitting a snooze button that prevents the brain from achieving deep, restorative sleep.
Impact on Sleep Quality
A physiology study on altitude-induced hypoxia by Pena et al. found that bruxism episodes coincided with drops in blood oxygen, suggesting that each grinding episode can amplify the stress of limited airflow. The result is elevated nighttime cortisol, higher blood pressure, and unrefreshed mornings.
Common sleep quality impacts include:
- Frequent micro-arousals (more than 5 per hour disrupt deep sleep)
- Increased light non-REM stage 1 sleep
- Reduced slow-wave sleep, which is crucial for memory consolidation
- Daytime sleepiness scored 4–5 points higher on the Epworth scale compared to non-grinders
Long-term Effects
Chronic teeth grinding affects more than just enamel. Over time, the stress hormones and blood pressure spikes associated with night-time jaw activity increase the risks for:
- Hypertension and cardiovascular disease
- Mood disorders like anxiety or depression
- Temporomandibular joint (TMJ) dysfunction, which can cause additional pain-related insomnia
- Tooth loss or expensive dental restorations
The cycle can seem endless: poor sleep leads to grinding, grinding disrupts sleep, and both contribute to medical expenses and daytime fatigue. Understanding and breaking this loop is key to achieving restful nights.

Sleep Disorders Linked to Pediatric Bruxism
Children aren’t immune to bruxism. Up to a third of kids grind their teeth at night, although many outgrow it by their late teens. Pediatric bruxism presents a slightly different picture because factors like growing faces, airway anatomy, and neurodevelopmental aspects are involved.
Children and Adolescents
A narrative review by Leung et al. notes that bruxism prevalence peaks around ages 6–11, roughly when the first adult molars appear. Teens generally see a decline, but not all kids are so fortunate. A review by Huynh and Fabbro identified risk factors like ADHD, high screen time, and orthodontic issues.
One often-overlooked factor is dental pain. A study of 2,400 Chinese schoolchildren by Zhang et al. found that untreated cavities tripled the odds of sleep disturbances, including grinding. In other words, cavities can keep young jaws active at night, and grinding can worsen decay by damaging fillings.
Pediatric Sleep Disorders
A systematic review by Orradre-Burusco et al. linked pediatric bruxism with:
- Primary snoring and mild OSA – Enlarged tonsils and adenoids narrow airways, causing jaw thrusting to breathe.
- Night terrors – Partial arousals in slow-wave sleep correspond with rhythmic muscle contractions.
- Attention-deficit/hyperactivity disorder (ADHD) – Stimulant medications, anxiety, and sleep fragmentation all increase grinding risk.
Parents often notice tooth wear during morning brushing, but kids rarely complain. Thus, pediatric dentists and doctors should inquire about snoring, restless sleep, and daytime behavior issues to catch a potential airway-grinding link early.
Managing Bruxism and Related Sleep Disorders
While you can't control what happens after you drift off, you can improve your odds. Management involves lifestyle changes, dental safeguards, and sometimes medical devices that address both apnea and grinding.
Lifestyle Changes
- Stress management – Practices like yoga, mindfulness, or even a walk can lower daytime tension that spills into nighttime clenching.
- Caffeine and alcohol curfew – These substances increase muscle activity and reduce REM stability. It's best to avoid them 4–6 hours before bed, according to the Mayo Clinic.
- Sleep hygiene – Consistent bedtimes, dark rooms, and cool temperatures help the brain enter deeper sleep without frequent awakenings.
- Jaw awareness exercises – Placing the tip of the tongue behind the upper front teeth and relaxing the jaw during the day can retrain muscle memory.
Medical Interventions
According to the assessment tool by Manfredini et al., treatment often starts with a custom night guard to cushion forces. However, if apnea is present, a mouthguard alone may not be enough.
- Mandibular advancement devices (MADs) – These oral appliances move the jaw forward, opening the airway and reducing both apnea events and grinding episodes.
- Continuous positive airway pressure (CPAP) – The gold-standard OSA treatment keeps the airway open with pressurized air. Some patients notice a reduction in bruxism episodes within weeks.
- Botulinum toxin injections – For severe jaw muscle hypertrophy, low-dose Botox can reduce clenching strength for 3–6 months.
- Orthodontic or ENT surgery – Correcting bite misalignment, enlarged tonsils, or nasal obstruction can address the root cause of airway compromise and secondary bruxism.
Always coordinate care between your dentist, sleep physician, and primary doctor. A splint that seems to work wonders for tooth wear might worsen apnea if it blocks the tongue space, so verifying with a sleep study is wise.
The Role of Oral Health in Sleep Disorders
Your mouth is the gateway to the respiratory system. Poor oral health can contribute to inflammation, alter jaw posture, and even affect airway size.
Impact on Dental Health
A literature review by Maniaci et al. reported that untreated OSA patients face twice the odds of periodontal disease compared to healthy sleepers. The theory is that mouth-breathing during apnea dries saliva, which serves as a natural buffer against bacteria.
Combine dry mouth with grinding, and you have a dental duo of destruction:
- Enamel microcracks invite decay and sensitivity
- Exposed dentin accelerates erosion from acidic foods
- Gum recession exposes roots, increasing infection risk
- Poorly fitting crowns from wear can trap plaque
Preventive Measures
- Twice-daily fluoride brushing – Strengthens enamel against microfractures.
- Hydration and saliva boosters – Sugar-free gum and xylitol lozenges encourage saliva production.
- Regular dental checkups – Detect early wear facets before they reach the nerve.
- Screening questionnaires – Tools like the STOP-BANG or Berlin questionnaires can flag potential apnea for referral.
- Interdisciplinary notes – Dentists should share radiographs and wear patterns with sleep doctors to address all aspects.
Think of your teeth as records of your nightly habits. Wear patterns and gum health can reveal what sleep labs might miss, making dental visits a stealth screening tool for hidden sleep disorders.
Conclusion
Teeth grinding is more than just a noisy habit. Current evidence indicates a strong connection between bruxism and sleep disorders like obstructive sleep apnea. Grinding can be both a symptom and a cause, disrupting sleep quality, increasing cardiovascular stress, and straining dental budgets. Children are also affected, with risk spikes related to airway problems and behavioral disorders.
Fortunately, with targeted lifestyle changes, dental devices, and sleep-focused medical care, the cycle can be broken. If you or your child wakes up with sore jaws, flattened teeth, or unexplained fatigue, don't ignore it. Speak to your dentist and a sleep specialist. Addressing both the grinding and the underlying sleep disorder can protect your smile and provide the restorative rest your body needs.