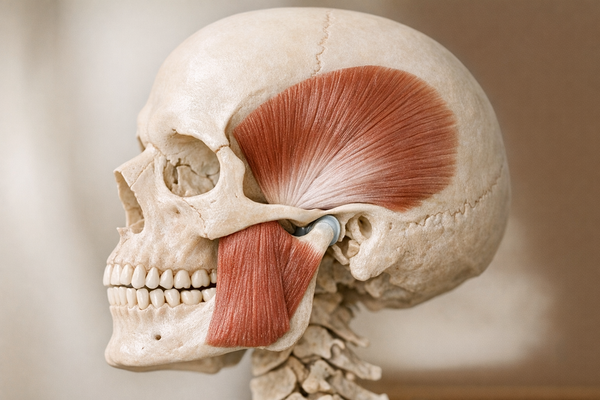
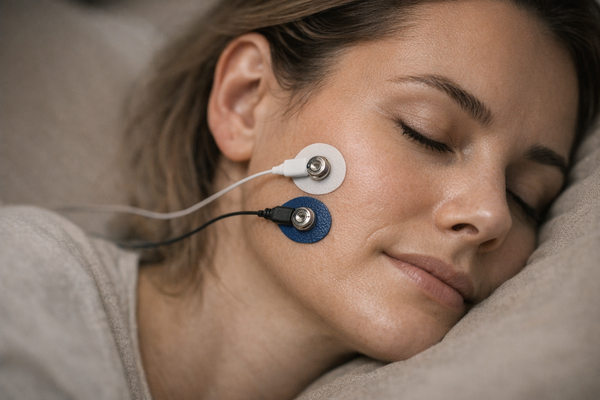
Understanding Jaw Tension: Is It Stress or Something More?
Explore stress-induced jaw tension vs other causes and diagnostic insights.
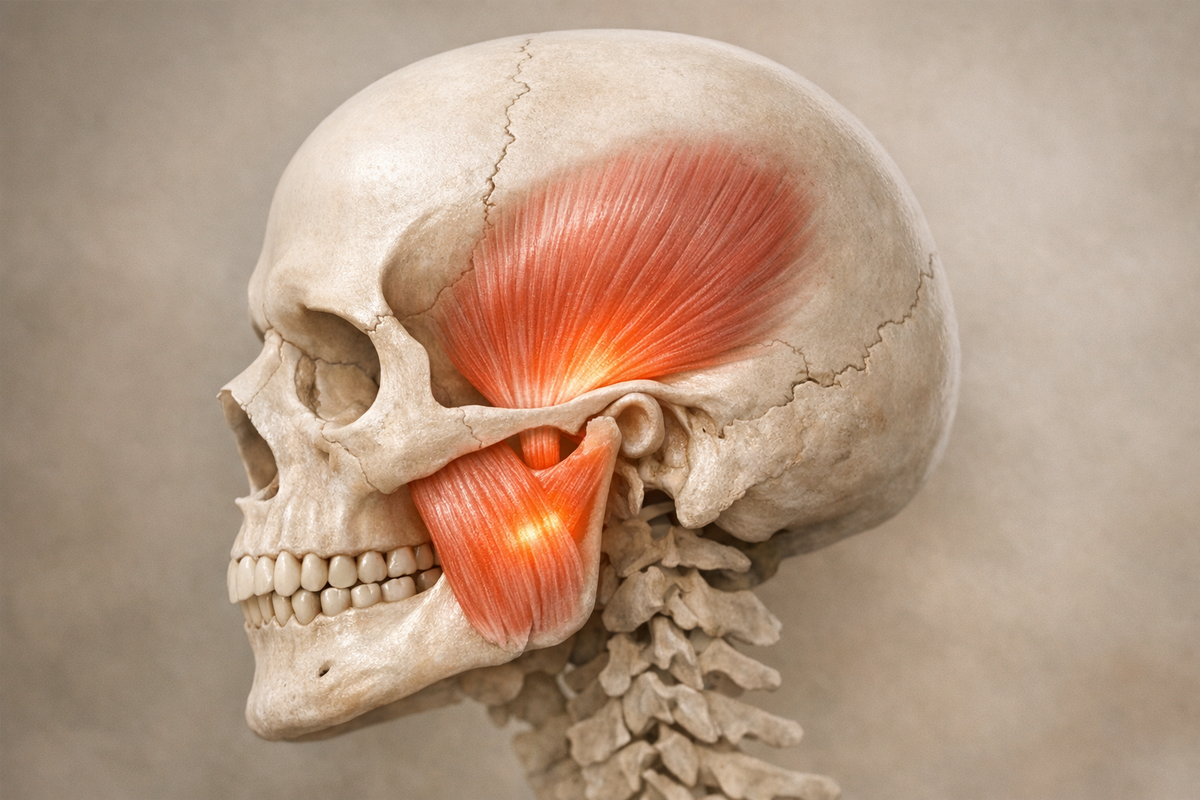
You wake up with a stiff jaw, feel a pop when you chew, or notice a dull ache climbing toward your temples. Your first thought might be, “Great, I must be grinding my teeth again.” That could be true. But the full story of jaw tension is more complex and, fortunately, more fixable than you might think. Recent research provides insights into whether stress, a mechanical issue, or a combination of both is causing that stubborn clench. Keywords like “jaw tension,” “stress,” and “bruxism” are essential to understanding what’s happening.
Explore what studies reveal, how to distinguish between different causes, and what steps you can take without getting lost in dental jargon.
Causes of Jaw Tension
Jaw tension is the sensation of tight, sore, or overworked jaw muscles. It can be a mild annoyance or turn into chronic pain that disrupts sleep and eating. While stress is often blamed—and it is a significant factor—research shows several other culprits can affect those small but mighty muscles around your temporomandibular joint (TMJ).
Stress and Anxiety. Stress triggers the release of adrenaline and cortisol, preparing your muscles for action, including the jaw muscles. You might unknowingly clench during a tense work call or while sleeping. Over time, this “stress jaw tension” leads to a cycle of muscle guarding and soreness. A 2024 review by Voß et al. links psychological stress to increased jaw muscle activity, as measured by electromyography. Explore more about how stress and anxiety lead to nighttime teeth clenching.
Bruxism (Teeth Grinding or Clenching). Sleep bruxism affects about 8–15 percent of adults. Episodes can be driven by stress hormones or arousals during specific sleep phases. The constant tug between the upper and lower teeth forces muscles to stay active, causing microscopic damage. Discover natural remedies for bruxism that go beyond the mouth guard.
Temporomandibular Disorders (TMDs). TMDs involve joint, muscle, or both. Issues like joint disk displacement, arthritis, or jaw misalignment can cause muscles to contract to stabilize the area. A 2025 systematic review by Chahrour and Reda shows that joint changes often coincide with muscle hyperactivity. Learn about effective TMJ exercises for jaw pain relief.
Malocclusion and Dental Issues. Crooked teeth or a high filling alter how your teeth meet, leading muscles to adapt and sometimes lock into a tense posture.
Poor Posture and Tech Neck. Leaning over a laptop pulls your head forward, forcing jaw muscles to counterbalance. This low-grade contraction can feel like tension over time. Understand how sleep positions can influence nighttime teeth grinding.
Medications and Stimulants. Certain antidepressants or a late-night espresso can heighten muscle tone, causing clenching spells. Discover why stimulants make you clench your jaw.
In real life, these causes often overlap. Stress can amplify bruxism, which irritates the joint, leading to more stress. Identifying the main cause is the first step toward relief.
Understanding Stress-Induced Jaw Tension
Stress isn’t just “in your head.” It has a biological footprint that appears in jaw muscles quickly. Understanding this chain reaction can help you break it.
The Fight-or-Flight Reflex. When your brain detects a threat—like running late or receiving a passive-aggressive email—it activates the hypothalamic-pituitary-adrenal (HPA) axis, releasing cortisol and catecholamines. These chemicals increase muscle readiness to contract.
Jaw muscles contain many fast-twitch fibers, making them ideal for quick clenching. Electromyography studies in the Voß et al. review show that participants under acute mental stress generate 20–40 percent more masseter activity compared to those watching calm videos.
Overnight Stress Loops. During sleep, your brain cycles through light, deep, and REM stages, with micro-arousals occurring during transitions. Chronic stress can trigger these arousals, causing the jaw to snap shut. Repeated hundreds of times, this leads to morning jaw ache. This is often a sign of morning jaw pain indicating nighttime teeth grinding.
The Pain-Tension-Pain Loop. Muscles held semi-contracted receive less blood flow, causing metabolic waste like lactic acid to pool and irritate nerve endings. Your brain interprets this as pain, further increasing muscle tone. A 2024 case report by Li et al. describes higher pain scores in patients recovering from jaw surgery who reported elevated stress and sleep disturbance.
Central Sensitization. Long-term stress can lower pain thresholds by altering how your spinal cord and brain process signals. This means a light clench feels more painful, making you more aware of the jaw and fueling additional tension.
Takeaway: Stress is a traceable physiological event that affects your jaw muscles. Addressing stress hormones and sleep quality can often reduce the entire chain of events. Consider exploring natural ways to relieve jaw tension from stress.
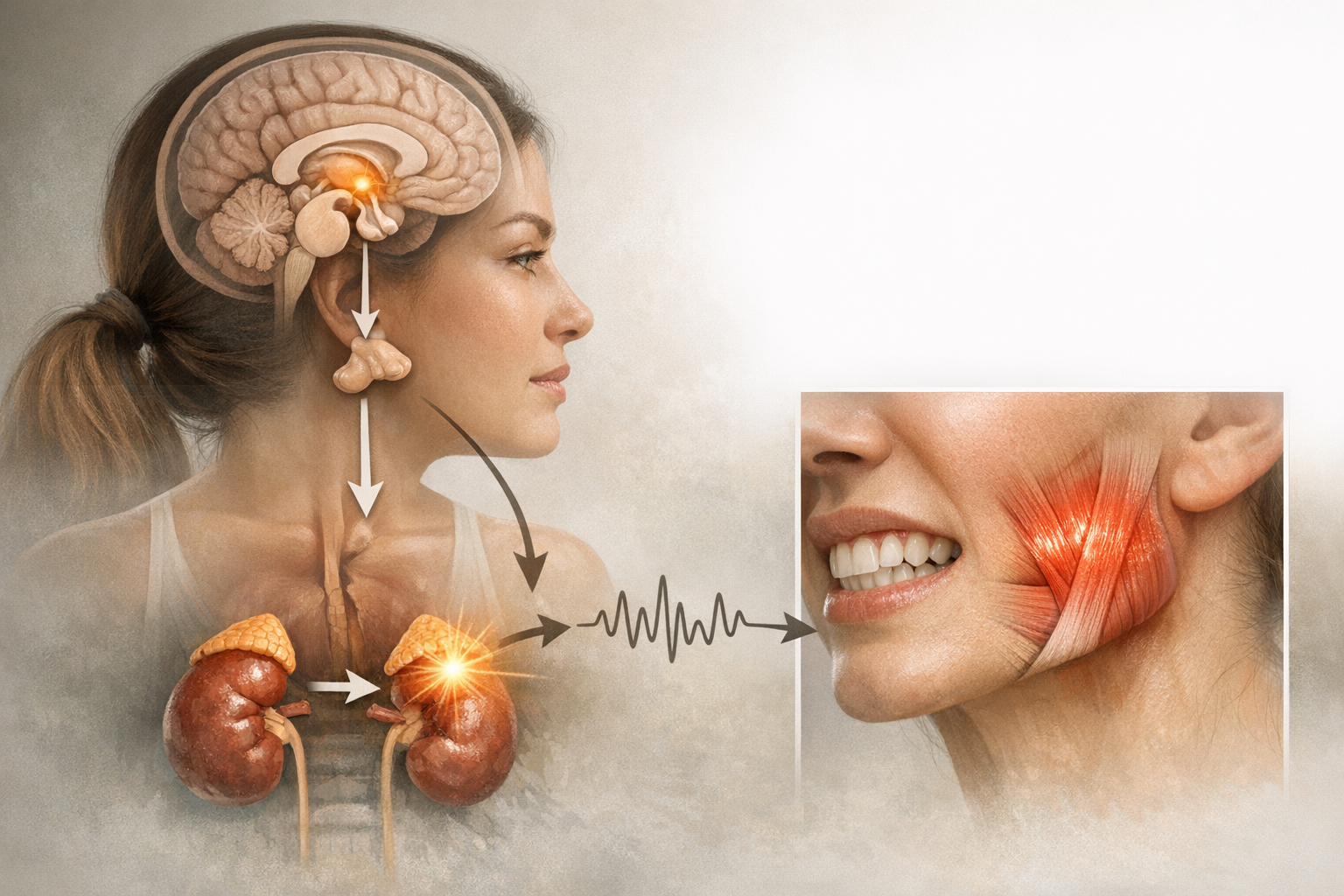
Differentiating Stress-Related Jaw Tension from Other Causes
How do you know if it’s stress or something mechanical? Use the checklist below, remembering that many people experience a combination of issues.
Signs of Bruxism
- Audible Grinding. A partner hears clicking or scraping at night. Stress alone rarely makes noise, but bruxism does.
- Tooth Wear. Flat-topped molars or chip lines along the edges indicate grinding more than tension. Your dentist can identify this quickly.
- Morning Symptoms. If jaw fatigue peaks after waking and fades by midday, sleep bruxism may be the main issue. Understand why jaw pain after sleeping could be related.
- Bite Marks on the Tongue or Cheeks. Repetitive clenching presses soft tissue against teeth.
In the review by Chahrour and Reda, occlusal splints reduced pain and muscle activity in bruxism-dominant patients even when stress management was minimal, indicating a mechanical component to their symptoms.
Temporomandibular Disorders (TMDs)
- Joint Noises. Clicking or popping sounds during mouth movements suggest disk displacement or arthritic changes.
- Restricted Mouth Opening. Less than 35–40 mm inter-incisal opening (about three finger widths) indicates a joint issue rather than muscle tension.
- Side-to-Side Deviation. The lower jaw may drift to one side on opening if the disk is out of place.
- Localized Joint Pain. Pressing just in front of the ear hurts, unlike diffuse muscle-only discomfort.
A cohort analysis by Da-Cas et al. in 2024 found that female sex, joint hypermobility, and a history of trauma are stronger predictors of TMDs than perceived stress scores, highlighting distinct risk profiles. For more on effective management, see our evidence-based guide on TMJ pain relief methods.
Distinguishing factors can overlap, so clinicians rely on structured exams like the Diagnostic Criteria for TMD (DC/TMD) protocol. If your symptoms cluster in one area, you can tailor treatment and avoid random remedies.
Red-flag overlaps. Bruxism and TMDs often spike during stressful periods. Chronic tension can worsen a joint problem, while joint pain can increase stress. It’s less about choosing a single cause and more about understanding which issue started first.
According to a 2024 clinical review by Lima and Mendes, up to 70 percent of TMD patients report bruxism behaviors. Separating cause from effect requires a stepwise diagnostic approach.
Diagnostic Approaches to Jaw Tension
Clinical Evaluations
Your journey often starts in the dental chair or a physical therapy room. Expect professionals to:
- Take a Detailed History. They’ll ask about stress levels, sleep quality, headaches, medication use, and prior injuries.
- Palpate Muscles and Joints. Light pressure identifies tender bands in the masseter or pterygoid. Joint palpation reveals local capsule pain.
- Measure Range of Motion. You may be asked to open, close, and shift your lower jaw while distances are recorded.
- Listen for Noises. A stethoscope or Doppler device can detect disk clicks.
- Check Dental Wear. Flattened cusps or fractured enamel suggest bruxism, guiding the next steps.
Cook et al. 2025 argue that a hands-on exam remains the gold standard because imaging can’t see muscle tone or trigger points directly.
Imaging Techniques
When red flags arise—like locking, trauma, or suspected arthritis—imaging is needed.
- Panoramic Radiograph. A basic 2-D X-ray that rules out fractures or significant joint changes.
- Magnetic Resonance Imaging (MRI). The best tool for visualizing the disk, joint inflammation, or effusion, distinguishing muscular from intra-articular issues.
- Cone-Beam Computed Tomography (CBCT). Offers high-resolution images of bony structures at a lower dose than medical CT scans.
- Electromyography (EMG). Surface electrodes measure muscle activity at rest and during movement, highlighting clenching intensity.
In the Lima and Mendes review, imaging is recommended only when it will change management plans, considering cost and radiation exposure.
Combining a thorough history, physical exam, and targeted imaging helps avoid misdiagnoses and speeds up effective care.
Managing Jaw Tension: From Stress Reduction to Medical Interventions
Stress Management Techniques
Since stress is the easiest issue to address, start here even if you suspect deeper problems.
- Diaphragmatic Breathing. Slow belly breaths lower sympathetic output. Two sets of 10 breaths before bed can reduce nocturnal clenching events, as noted in the Voß et al. review.
- Progressive Muscle Relaxation. Contract and release muscle groups, saving the jaw for last, to recognize and release tension quickly. Consider other natural solutions for jaw tension relief.
- Mindfulness-Based Stress Reduction (MBSR). Guided meditations reduced self-reported jaw tension by 30 percent in the Li et al. case series.
- Sleep Hygiene. Dark rooms, consistent bedtimes, and caffeine curfews reduce micro-arousals that trigger night-time clenching. Improve your sleep quality by following the role of sleep hygiene in managing bruxism.
- Posture Fixes. Align your monitor at eye level, keep shoulders relaxed, and check in every hour. Cleveland Clinic’s guide on TMJ disorders and posture offers easy desk tweaks.
Medical Treatments
If self-care doesn’t help, consider targeted therapies.
- Occlusal Splints (Night Guards). Custom acrylic trays protect teeth and redistribute bite forces. The Chahrour and Reda review found that splints reduced pain scores by 50 percent on average across nine trials. Discover the best over-the-counter night guards for bruxism.
- Physical Therapy. Manual stretching, trigger-point release, and ultrasound expedite muscle recovery. Exercises to open and glide the jaw add endurance.
- Behavioral Therapy. Cognitive behavioral therapy (CBT) helps identify grinding triggers and replace them with neutral habits. The National Institute of Dental and Craniofacial Research notes CBT’s sustained benefits beyond the splint alone. See their resource at NIDCR TMJ page.
- Pharmacologic Options. Short courses of NSAIDs reduce inflammation. Low-dose muscle relaxants at night ease severe bruxism but are usually temporary fixes.
- Botulinum Toxin Injections. For resistant cases, small doses into the masseter weaken clench strength for three to four months, though cost and potential chewing fatigue are drawbacks.
- Surgical Interventions. Arthrocentesis or joint replacement is rare and reserved for structural pathology that doesn’t respond to conservative care.
According to Li et al., multidisciplinary treatment spanning dental, pain, and mental-health services yields the most consistent relief, especially when sleep issues coexist. Learn how TMJ pain management can help alleviate discomfort.
When to Seek Professional Help
You can safely try breathing drills and night guards at home, but certain signs mean it’s time to consult a professional:
- Pain lasting more than two weeks or interfering with work, eating, or sleep
- Jaw locking open or closed, even briefly
- Noticeable decrease in mouth opening range
- Frequent headaches or ear pain related to chewing
- Unexplained tooth wear or fractures despite good dental hygiene
A 2024 clinical review by Lima and Mendes advises early evaluation, as lingering joint inflammation can develop into degenerative changes within months. Ignoring chronic tension allows easy-to-treat muscle knots to evolve into complex joint damage. Discover how ear pain can be linked to TMJ and bruxism.
Conclusion
Jaw tension is common, but it’s not one-size-fits-all. Stress activates muscle tension, bruxism grinds enamel down, and temporomandibular disorders add a mechanical twist. Determining which issue is most significant requires a clear history, a hands-on exam, and, when needed, imaging.
Begin by managing stress with breath work, mindfulness, and improved sleep. Add dental guards or physical therapy when clenching or joint issues arise. Always consult a professional if pain persists or function declines. Your jaw is small, but its impact on everyday comfort is significant. Fortunately, a tailored plan informed by the research above can loosen that clench, allowing you to bite, talk, and laugh without worry.