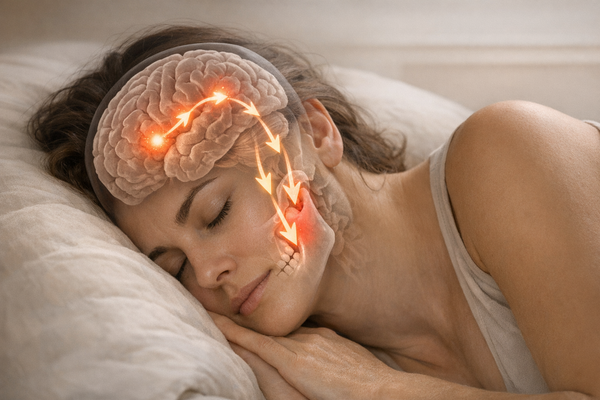
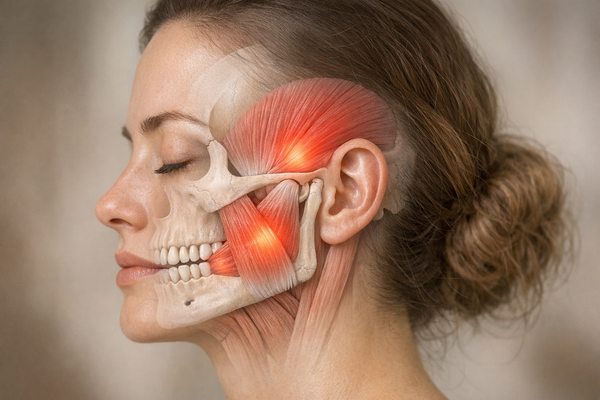
Understanding Ear Pain Linked to TMJ and Bruxism
Explore the ear pain, TMJ, and bruxism link and management strategies.
Ear pain that shows up for no obvious reason can feel like a plot twist you never asked for. You rummage through memories of flights, colds, and loud concerts but nothing fits. Then someone drops the letters TMJ in the conversation and the jaw suddenly becomes prime suspect number one. If you also grind or clench your teeth at night, now you have a probable accomplice called bruxism. This article unpacks how jaw mechanics, muscle overuse, and nervous system wiring can send pain signals that register in your ears. We sift through recent research, call out practical fixes, and keep the jargon low so you can actually use what you learn.
Everything is written for you—the health-curious reader who wants science without the snooze. Links let you dive deeper whenever you feel like playing detective. Ready to connect the dots between your jaw, your sleep, and your sore ear? Let’s get moving.
The Connection Between Ear Pain and TMJ
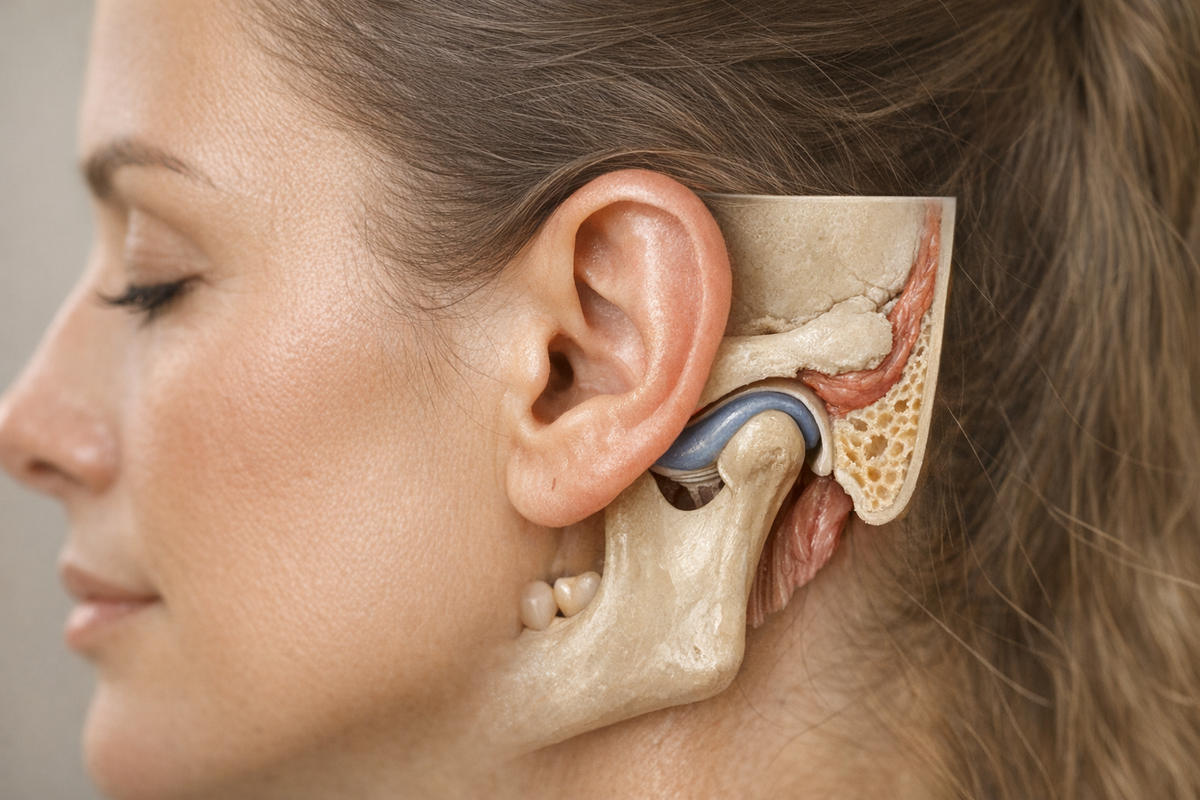
The temporomandibular joint (TMJ) is the sliding hinge that lets your lower jaw open, close, and wiggle side to side. It sits just in front of the ear canal, which means trouble in this small joint can impersonate an earache. Several studies back up the link, including insights on the connection between teeth grinding and ear pain.
A protein-mapping project, Unlocking ADAMTS-5 (2025), showed that inflammatory enzymes inside the TMJ can irritate nearby nerves shared with the outer ear. When that network lights up, your brain cannot always tell where the hurt started, so it labels the nearest landmark—the ear. Researchers call this referred pain.
Symptoms go beyond a dull ache. You might feel fullness, ringing, or even brief bouts of dizziness. A Turkish cohort study of 249 patients, Investigation of Factors Associated with Dizziness, Tinnitus, and Ear Fullness in TMJ Disorders (2023), found that 42 percent of people with temporomandibular disorders (TMDs) reported ear symptoms. Women were almost twice as likely as men to check the “ear trouble” box.
In Nigeria, an otology clinic audit offered another reality check. Otological Manifestation of TMJ Disorder in Ekiti (2021) reviewed 503 ear-pain cases and traced 15.3 percent back to TMJ dysfunction. That matters because antibiotics or ear drops will not silence pain that starts in the jaw joint.
- Key symptoms: earache, muffled hearing, clicking jaw, morning facial stiffness.
- Prevalence: An estimated 5 to 12 percent of adults have a TMJ disorder, and ear pain is among the top three complaints.
- Why it hurts: Shared nerves (auriculotemporal branch of the trigeminal nerve) and shared blood supply mean inflammation spreads the misery.
Understanding this overlap saves time and cash. Instead of hopping from primary care to ENT to dental visits, you can start a targeted conversation about TMJ screening whenever unexplained ear pain sticks around for more than a week.
Bruxism and Its Impact on TMJ and Ear Pain
Bruxism is the medical name for grinding, clenching, or gnashing your teeth—usually while you sleep but sometimes while you sit in traffic or doom-scroll. Those repetitive forces overload the TMJ and can fire up ear pain. Learn more about natural bruxism solutions that could help alleviate symptoms.
The Orofacial Pain review (2024) classifies bruxism as a parafunctional habit influenced by stress, medications, and even sleep apnea. It notes that muscle activity in nighttime bruxers can spike up to six times normal chewing levels. That power surge translates into micro-trauma for the joint’s cartilage and supportive ligaments.
How common is the habit? A global meta-analysis, Prevalence of Temporomandibular Joint Disorders (2021), puts awake bruxism at about 5 percent of adults and sleep bruxism at 8 percent. Yet rates climb to 20 percent in people under chronic stress or taking certain antidepressants.
Signs you may be a grinder:
- Morning jaw stiffness or fatigue
- Flattened or chipped teeth
- Headaches that start at the temples
- Ear pain without infection
Bruxism fuels TMJ inflammation the same way a runner’s high mileage fans knee pain. Overworked muscles tighten, discs can slip out of position, and nerves complain. Because the TMJ lives millimeters from the ear canal, the discomfort reports to your brain as earache. If you wake up with ear pain that fades by lunchtime, nighttime clenching is an especially strong suspect.
Clinical Findings and Research on TMJ, Bruxism, and Ear Pain
Let’s zoom out and see what the broader research landscape shows. Family physicians often grapple with head and neck pain syndromes, so Otolaryngeal and Oropharyngeal Conditions: Temporomandibular Disorders (2021) offers a handy summary. The review flags ear symptoms in up to half of TMD cases seen in primary care. When patients had both TMJ signs (clicking, limited opening) and bruxism, ear pain scores doubled.
An orthodontic research team provided another layer. Orthodontics and Temporomandibular Disorders: An Overview (2023) looked at 38 observational studies and concluded that malocclusion by itself is rarely the lone cause of TMD, but when bruxism coexists, the risk of otologic symptoms climbs sharply. The paper recommends early detection through bite analysis and sleep history.
Imaging studies add objective proof. High-resolution MRI shows that bruxers often develop disc displacement and joint effusion—both correlate with auriculotemporal nerve irritation, which triggers ear pain. Ultrasound studies show hypertrophic lateral pterygoid muscles in chronic grinders, further confirming the mechanical overload theory. For more insights on jaw pain and its various causes, check out Understanding Jaw Pain on One Side: Causes and Solutions.
Bottom line from the literature:
- Ear pain in TMD is not rare—it is textbook.
- Bruxism magnifies joint stress and symptom severity.
- Early diagnosis and targeted therapy cut down on needless ENT referrals and imaging costs.
Effective Management Strategies for TMJ and Bruxism
You cannot wish ear pain away, but you have a menu of evidence-backed options. Guidelines from the BMJ clinical practice guideline on chronic TMD pain (2023) and a rapid review in the International Journal of Oral and Maxillofacial Surgery (2022) outline conservative first steps, more focused interventions, and alternative therapies. We group them below so you can craft a game plan.
Lifestyle Changes
- Stress management – Mindfulness, cognitive behavioral therapy, and even basic diaphragmatic breathing can dial down daytime clenching. Lower muscle tension equals less joint compression. Consider these stress and anxiety triggers that may contribute to jaw clenching.
- Sleep hygiene – Regular bedtimes, reduced caffeine after noon, and limiting screen time reduce micro-arousals that trigger sleep bruxism. The American Academy of Sleep Medicine adds that side sleeping with a supportive pillow keeps the jaw in neutral.
- Diet hacks – For flare-ups, adopt a soft diet for 5 to 7 days. Think oatmeal, smoothies, scrambled eggs. Chewy bagels and steak make the joint work overtime.
- Posture drills – Keep screens at eye level and shoulders relaxed. A forward head posture adds tension across the jaw and neck muscles that share nerve pathways with the ear.
Medical Interventions
- Occlusal splints – Also called night guards, these acrylic trays slide over teeth to spread biting forces and prevent enamel wear. They earned a strong recommendation in the 2023 BMJ guideline for reducing pain intensity by about 30 percent in three months. Learn about top mouth guard options for TMJ relief that might be beneficial.
- Physical therapy – Jaw-specific exercises, manual muscle release, and ultrasound therapy improve range of motion. A 2022 network meta-analysis found PT plus a splint outperformed either alone for pain and clicking reduction.
- Pharmacologic aid – NSAIDs tackle inflammation, while low-dose muscle relaxants taken before bed can cut bruxing episodes. Some providers use short steroid tapers for acute joint effusion, though evidence is mixed.
- Botulinum toxin – When jaw muscles refuse to chill, tiny injections of botulinum toxin type A weaken overactive fibers for three to four months. Studies show up to 70 percent pain relief, but cost and repeat dosing are drawbacks. Discover more about Botox for bruxism and how it may assist in reducing teeth grinding.
Alternative Therapies
- Acupuncture – Needle placement along trigeminal nerve branches has shown modest benefits in small RCTs, though placebo effects cannot be ruled out.
- Low-level laser therapy – Shining specific wavelengths through the skin may reduce joint inflammation. Evidence is promising but not rock solid.
- Yoga and tai chi – Gentle, mindful movement trains body awareness, easing the jaw-neck-shoulder muscle chain. Cheap, low risk, and bonus relaxation points.
- Biofeedback – Surface EMG monitors jaw tension and teaches you to unclench in real time. Think of it as a mindfulness coach that beeps when your teeth touch.

You do not have to pick just one tool. Most people benefit from a combo—say, a night guard, targeted exercises, and stress management. Tracking symptoms in a phone diary helps you see what works and flag patterns like more pain after late-night emails or triple espressos.
The Role of Orthodontics in Managing TMJ Disorders
Braces are not just for yearbook smiles. Malocclusion can push the jaw into awkward positions that overburden the TMJ, especially when bruxism piles on. The overview by Aldayel et al. (2023) notes that orthodontic correction—whether conventional brackets or clear aligners—can redistribute biting forces and improve joint loading. For a different approach to managing bruxism, consider using wearable tech to help detect and reduce symptoms.
Who benefits most?
- Patients with deep bites where lower incisors impinge on palatal tissue
- People whose crossbite forces the jaw sideways, stressing one TMJ more than the other
- Bruxers whose uneven contact leaves one side of the jaw “carrying the load”
Treatment planning now often includes 3D cone-beam CT to map joint anatomy and guide tooth movements that respect TMJ space. Some orthodontists work in tandem with orofacial pain specialists, using splints during the leveling phase to calm symptoms before major tooth shifts begin.
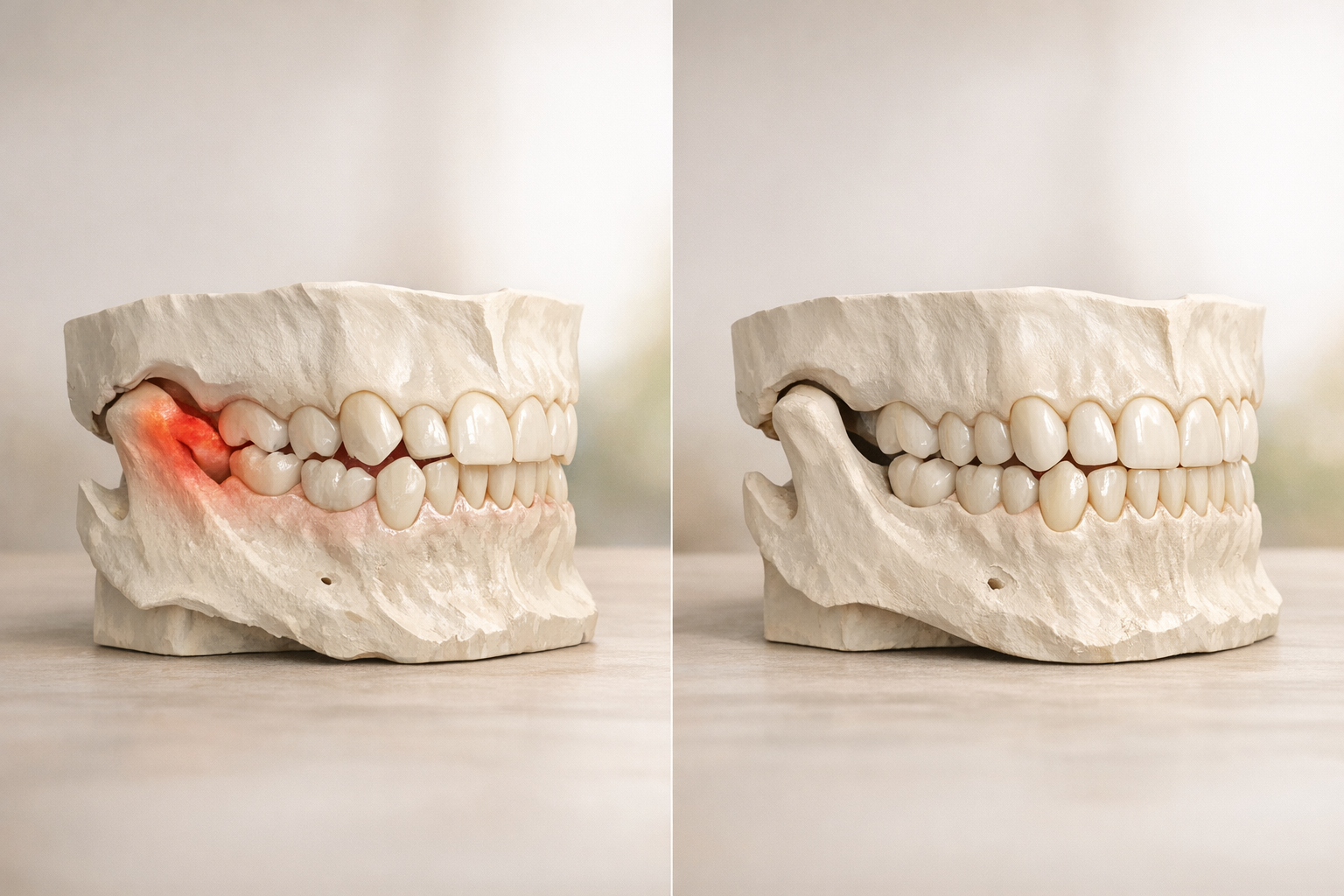
A key takeaway from the 2023 overview: simply straightening teeth does not guarantee TMJ relief, but when orthodontics addresses bite discrepancies linked to joint overload, ear pain often eases as a side effect. Ongoing research uses AI-based bite force simulations to predict which patients will gain the most.
Future Directions in TMJ and Ear Pain Research
TMJ science is sprinting into the molecular era. The Unlocking ADAMTS-5 proteomics paper (2025) opens the door to enzyme-targeted drugs that could halt cartilage breakdown before pain escalates. On the clinical side, the 2023 BMJ guideline calls for head-to-head trials comparing splints, botulinum toxin, and minimally invasive joint lavage in patients whose main symptom is ear pain. Wearable jaw-movement trackers may soon deliver real-time data on bruxism intensity, letting clinicians fine-tune therapy like a sleep apnea CPAP machine does today.
Researchers also eye the brain. Functional MRI studies already show altered pain processing in chronic TMD patients. Future work may test neurofeedback or non-invasive brain stimulation to “reboot” pain circuits. The hope is a treatment mix that hits mechanical overload, inflammation, and nerve sensitization all at once.
Conclusion
Ear pain, TMJ disorders, and bruxism form a three-way tug-of-war. Because the jaw joint hugs the ear canal, inflammation or mechanical overload easily translates into earache, ringing, or fullness. Research from proteomics to population studies shows a clear connection, and evidence-based guidelines now steer us toward conservative, multi-modal care first.
If you wake with sore ears, a stiff jaw, and flat teeth, consider a TMJ checkup rather than another round of ear drops. Lifestyle tweaks, night guards, physical therapy, and selective medical treatments give most people relief without surgery. Orthodontics may help when bite problems keep the joint off balance. Looking ahead, enzyme blockers and smarter wearables promise even more targeted solutions.
Your next step is simple: track your symptoms, discuss TMJ screening with your dentist or primary care provider, and start small changes today. The sooner you break the pain cycle, the faster your ears and jaw can call a truce.