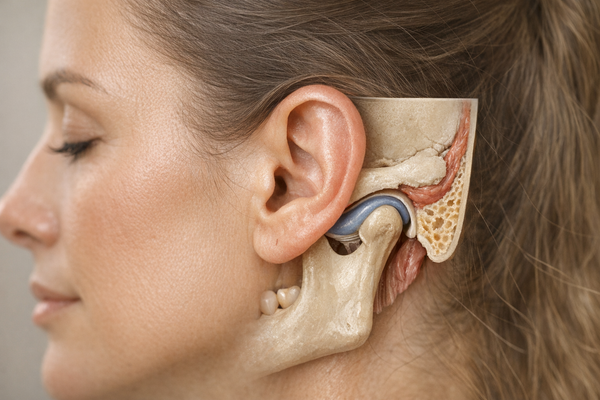
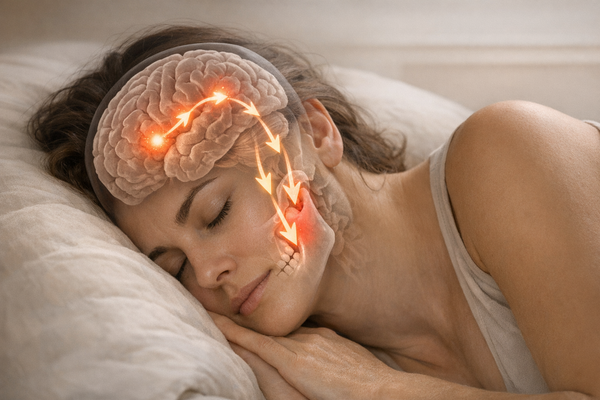
Unconsciously Clenching Jaw: The Impact of Stress and Sleep Disorders
Explore how stress and sleep disorders lead to unconscious jaw clenching.

You wake up, rub your eyes, and notice your jaw feels like it spent the night power-lifting. You didn't decide to clench your teeth for eight straight hours, yet here you are with sore jaw muscles and maybe a tiny headache. That involuntary grinding is called unconscious jaw clenching, and it can happen while you're awake or asleep. Scientists have been studying this for decades, and recent research connects stress, sleep disorders, and those tight jaw muscles. For more insights on jaw pain causes, you might want to explore the differences between jaw pain from anxiety and heart attacks.
Below you will find what the research says, along with practical ways to ease jaw tension. Keep reading if you want fewer cracked molars and more restful shut-eye.
Understanding Unconscious Jaw Clenching
Unconscious jaw clenching, often called "bruxism," is the repetitive clamping or grinding of teeth without deliberate intent. Dentists see it daily, yet many people don't realize they're doing it until a tooth chips or a partner complains about a nighttime grinding soundtrack. A recent functional near-infrared spectroscopy study led by Noor et al. confirmed that much of the clenching occurs outside conscious control. The researchers found surges in muscle oxygenation even when participants reported they were "relaxed."
Prevalence numbers vary. Research by Sharma and colleagues suggests that roughly 20% of kids grind or clench during sleep. Adult rates hover around 8-16%, depending on stress load and sleep quality. While bruxism can stem from medication side effects, malocclusion, or genetics, stress and sleep disorders are the most consistent factors behind the habit. To understand more about the surprising causes of teeth grinding during sleep, visit surprising causes of teeth grinding.
By comparing clench frequency against salivary cortisol (a stress hormone) and polysomnography results, scientists found a tight correlation. When cortisol spikes, jaw muscles receive more neural firing and stiffen, even in deep sleep. Add a sleep disorder that disrupts REM cycles, and the nervous system tosses in extra micro-arousals. Those tiny awakenings often come with a burst of muscle activity, including jaw clenching. This is why "unconsciously clenching jaw" appears in dental, psychological, and sleep medicine journals alike.
Bottom line: unconscious jaw clenching is common, understudied, and closely linked to stress chemistry and broken sleep.
The Role of Stress in Jaw Tension
Stress is not just a feeling—it's a full-body biochemical cascade. When your brain perceives a threat, such as a work deadline or a loud horn, the hypothalamic-pituitary-adrenal axis pumps out cortisol and adrenaline. These hormones prime muscles for action. Unfortunately, your masseter, the powerhouse jaw muscle, doesn't get the memo that an email inbox is not a saber-toothed tiger.
In a clinical trial examining temporomandibular disorder patients, Lee et al. found that individuals with higher perceived stress scores demonstrated significantly more nighttime jaw activity when monitored with electromyography. The authors concluded that "psychological load predicts myogenous bruxism better than occlusal factors," meaning the mind beats the bite every time. If you are looking for ways to manage TMJ pain, check out TMJ pain management.
Psychologists call the muscle tightening that follows chronic worry "jaw tension anxiety." It's the bodily signature of rumination and hyper-vigilance. The American Psychological Association notes that sustained mental strain keeps peripheral muscles in a semi-contracted state, making clenching a near-automatic reflex.
Interestingly, the relationship is bidirectional. Clenching itself feeds back into the brain and can heighten the sensation of stress. When jaw muscles fatigue, pain signals travel along the trigeminal nerve, nudging the limbic system—the emotion hub—to perceive more distress. It's a loop that can run 24-7 unless interrupted.
Stress-Induced Anxiety and Jaw Clenching
Yeon-Hee Lee's study focused on patients with clinically diagnosed anxiety disorders and measured bite force during worry-inducing tasks. The group showed a 40% increase in clench intensity compared to controls, supporting the idea that anxiety fuels jaw tension anxiety directly. Moreover, participants who practiced four weeks of deep-breathing exercises cut their clench episodes in half, demonstrating that stress management can calm the mandible. For more information on how stress and anxiety contribute to clenching, explore stress and anxiety triggers.
Digital behavior trackers back this up. Wearable EMG headbands show that email notifications and social media pings create micro-spikes in masseter activity. That means your phone buzz may be nudging your jaw into a clamp before your conscious mind registers annoyance. If you crave proof, set your device to silent for a day and notice whether your face feels looser.

Sleep Disorders and Their Impact on Bruxism
Your jaw is supposed to take a nap when you do. Unfortunately, sleep disorders like insomnia, obstructive sleep apnea (OSA), and restless legs syndrome disrupt the normal muscle relaxation of slumber. Each time your airway narrows or your brain startles awake, muscles contract to protect you. That includes the ones around your mouth, leading to stress jaw tension even while unconscious. To discover how sleep positions influence nighttime teeth grinding, learn about sleep positions and teeth grinding.
Szostak et al. conducted an observational study with over 300 adults and linked higher apnea-hypopnea indices (the score doctors use to grade sleep apnea) to more severe sleep bruxism. The authors speculated that clenching helps stabilize the airway in partial collapse, but the cost is enamel wear and morning jaw soreness.
Teenagers are not immune. A cross-sectional survey using the Epworth Sleepiness Scale by López-Soto and co-authors found that young adults who rated themselves "excessively sleepy" had double the odds of reporting night-time tooth grinding. Because their orthodontic work is still in progress, the damage can be more severe.
Poor sleep quality also amplifies daytime stress, which then circles back to more clenching. The National Sleep Foundation explains that fragmented sleep elevates amygdala reactivity, making the brain more sensitive to daily hassles. That's how "stress jaw tension" becomes a round-the-clock affair.
Common Sleep Disorders Linked to Jaw Clenching
- Obstructive Sleep Apnea (OSA): Repeated oxygen dips prompt micro-arousals, each paired with jaw muscle activation. Dental sleep specialists often discover OSA in patients who present with unexplained molar fractures.
- Insomnia: Difficulty falling or staying asleep keeps the sympathetic nervous system on high alert. In this wired state, muscles seldom relax fully, encouraging nocturnal bruxism.
- REM Behavior Disorder: People physically act out dreams and often clamp their jaws during intense dream segments.
- Restless Legs Syndrome: Though it affects limbs, the cross-talk in motor pathways can spill over to facial muscles, sparking clench episodes.
Polysomnography labs routinely measure chin EMG as a marker of sleep stage. High readings in non-REM periods flag potential bruxism. Integrating these findings with airway pressure sensors helps doctors decide whether a CPAP machine, mandibular advancement device, or behavioral therapy is the best first step.
Neuromuscular Factors in Jaw Clenching
Stress and sleep disorders light the fuse, but the actual explosion happens in the muscles and nerves that open and close your mouth. The masseter and temporalis muscles top the list. They receive innervation from the trigeminal nerve, the largest cranial nerve, which also carries pain and touch information from the face. This two-way highway explains why jaw pain can set off headaches and vice versa. If you are wondering about the connection between teeth grinding and ear pain, explore the connection here.
A large population study by Teichert Filho et al. underscored how different bruxism patterns—awake, sleep, or combined—align with temporomandibular disorder (TMD) subtypes. Myogenous TMD (muscle-based) showed the strongest overlap with combined bruxism, suggesting that some people have neuromuscular wiring that makes jaw muscles more excitable. Meanwhile, Noor's AI-driven spectroscopy work detected that even a small rise in mental workload boosted mandibular muscle oxygenation faster than in limb muscles, pointing to a hypersensitive motor reflex.
From a neurochemical angle, elevated levels of glutamate and decreased gamma-aminobutyric acid (GABA) within the trigeminal motor nucleus can produce hyper-excitability. That means a simple jaw-opening reflex morphs into an all-night grind. Sleep deprivation further lowers GABA, making matters worse. Genetic factors may also tweak muscle fiber types so they fatigue slowly, allowing clenching to carry on for hours without awareness.
How Neuromuscular Conditions Contribute
Some patients develop bruxism as a side effect of medications that alter dopamine, such as certain antidepressants. Dopamine modulates motor circuits, and when levels shift, jaw muscles can spasm. Additionally, individuals with cervical spine issues often compensate by changing head posture, which changes jaw muscle load. Physical therapists see a steady stream of "mystery" headaches that are actually after-shocks of nocturnal jaw clenching compounded by neck tension. For more information on the jaw-back connection in teeth grinding, visit how teeth grinding could be causing your back pain.
Understanding these neuromuscular layers matters because therapy that targets only stress (like mindfulness) might miss an overactive trigeminal pathway. Likewise, fitting a mouthguard tackles tooth wear but not neural overdrive. The fix is usually multi-tiered.
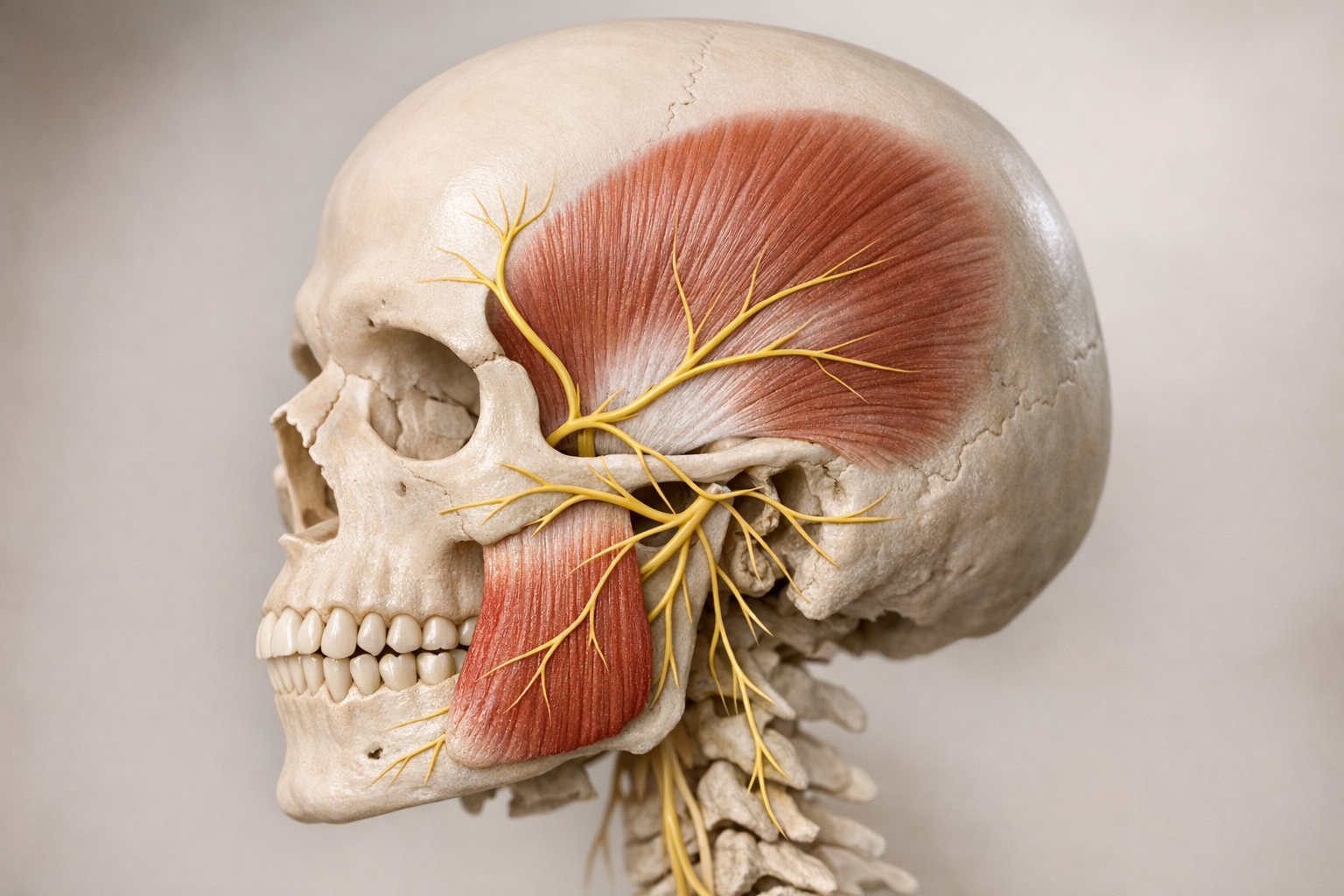
Managing and Reducing Jaw Clenching
Good news: you don't need a Ph.D. in neurobiology to loosen your jaw. Evidence-based strategies range from mindfulness apps to prescription sleep devices. The key is matching the tool to the trigger—stress, sleep disorder, or neuromuscular glitch. Don't be shy about mixing and matching under professional guidance.
Therapeutic Approaches
- Occlusal Splints: Custom mouthguards shield enamel and distribute bite forces. They don't cure bruxism, but they stop the collateral damage. Dentists often start here while broader treatments take effect. Learn more about the differences between OTC and custom night guards.
- Topical Cannabidiol (CBD): A pilot trial on temporomandibular patients by Walczyńska-Dragoń et al. reported that CBD gels applied to jaw muscles reduced pain scores and improved sleep quality. CBD appears to modulate TRPV1 receptors, dialing down both inflammation and muscle hyperactivity.
- Botulinum Toxin Injections: Small doses weaken the masseter for 3-4 months, giving muscles a break from overuse. Side effects are minimal when performed by an experienced injector, although chewing tough foods may feel odd at first.
- Continuous Positive Airway Pressure (CPAP) or Mandibular Advancement Devices: For OSA-linked bruxism, addressing airway obstruction often reduces clenching frequency because the body no longer jerks awake to breathe.
- Biofeedback: Wearable EMG devices vibrate when they detect clenching, teaching users to relax. Think of it as Pavlov for your jaw.
Lifestyle Changes
Therapies above work best when paired with adjustments that lower baseline arousal:
- Daily Stress Management: Guided breathing, progressive muscle relaxation, or yoga reduce cortisol. The Mayo Clinic lists exercises that take five minutes and can be done at your desk.
- Screen-Free Wind-Down: Blue light and doom-scrolling raise alertness. Put devices away an hour before bed and read a paper book or stretch instead.
- Caffeine Curfew: Stop stimulants by early afternoon to avoid nighttime arousal that sparks clenching. Find out why avoiding caffeine late at night is crucial.
- Balanced Bite: Don't chew gum all day—extra jaw workouts train muscles to stay tense.
- Sleep Hygiene: Keep a consistent schedule, cool bedroom temperature, and consider white noise. The American Sleep Association details easy tweaks.
- Physical Activity: Cardio lowers anxiety hormones and improves slow-wave sleep, both clench deterrents.
- Postural Awareness: Ergonomic chairs and monitor risers keep your head over your spine, reducing compensatory jaw tension.
Combine two or three of these habits, and you can chip away at both the psychological and neuromuscular roots of jaw tension. Small wins add up—closing a stressful email without biting down too hard counts as progress.
Conclusion
Unconsciously clenching your jaw is like leaving a car in park with the engine revving. Stress pours in the fuel, sleep disorders stomp on the gas, and hyper-responsive jaw muscles keep the tachometer red-lined. The science is clear: cortisol spikes, micro-arousals, and trigeminal overdrive all lead to bruxism. Rigorous studies—from Noor's AI-guided spectroscopy to Szostak's sleep-lab analyses—map out the pathways.
You can't bubble-wrap your life against every deadline or noisy neighbor, but you can reduce jaw damage by treating the roots. Start by assessing stress levels, screen for sleep apnea, and investigate neuromuscular quirks. Layer on protective gear like mouthguards and consider evidence-backed therapies such as topical CBD or biofeedback. Round things out with lifestyle tweaks—deep breathing, regular workouts, and sane caffeine use.
The reward is quieter nights, fewer cracked fillings, and a jaw that wakes up as relaxed as the rest of you.