Natural Bruxism Solutions: How to Stop Grinding Teeth in Sleep
Discover natural remedies for bruxism beyond the mouth guard.
If you wake up with a sore jaw, sensitive teeth, or a partner complaining about the midnight sound of a trash compactor in bed, you are not alone. Sleep bruxism, the clinical term for nighttime teeth grinding, affects up to 15 percent of adults. Dentists usually recommend a mouth guard, and yes, a custom splint can protect your enamel. But what if you want to address the root causes instead of wearing plastic every night? Recent studies indicate that natural and non-invasive strategies can calm the jaw, improve sleep quality, and even retrain the brain-to-muscle connection.
Explore an evidence-packed overview of today’s most promising approaches, from progressive muscle relaxation to high-tech neuromodulation. Each section translates clinical jargon into plain language, keeping the tone frank and practical. Ready to let your molars relax? Let’s dive in.
Understanding Bruxism: Causes and Symptoms
What is Bruxism?
Bruxism is a movement disorder where you grind, clench, or gnash your teeth. It occurs in two forms: sleep bruxism, happening during non-rapid eye movement and REM sleep, and awake bruxism, which occurs while you are conscious and often concentrating. A 2024 scoping review by Oliveira et al. underscores that the behavior is multifactorial, driven by genetic, neurologic, and psychological triggers. For more insights into what causes teeth grinding, you can explore our detailed article on teeth grinding causes.
Common Symptoms
- Dull morning headaches
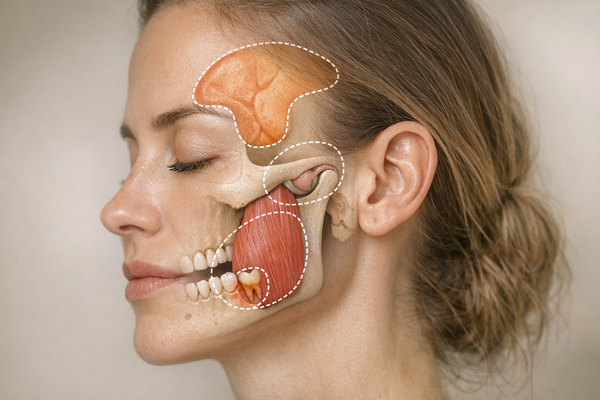
- Jaw muscle fatigue or pain
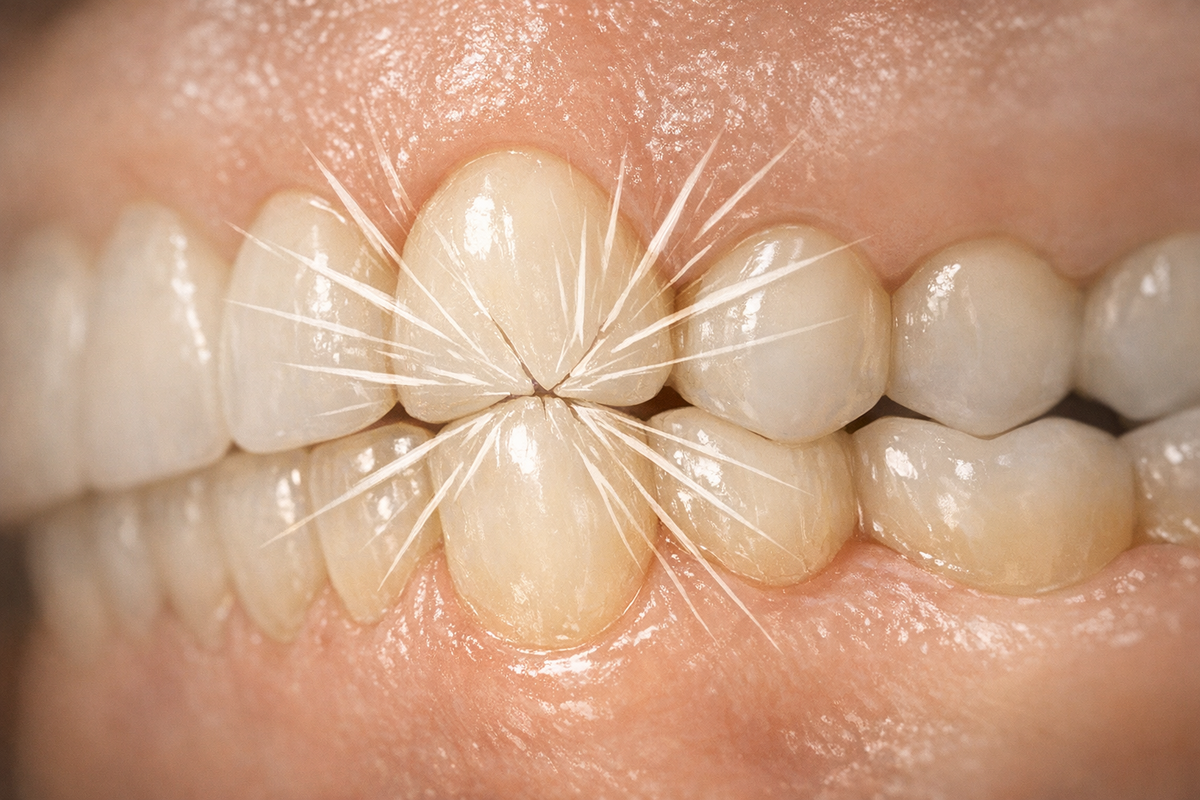
- Cracked or worn tooth enamel
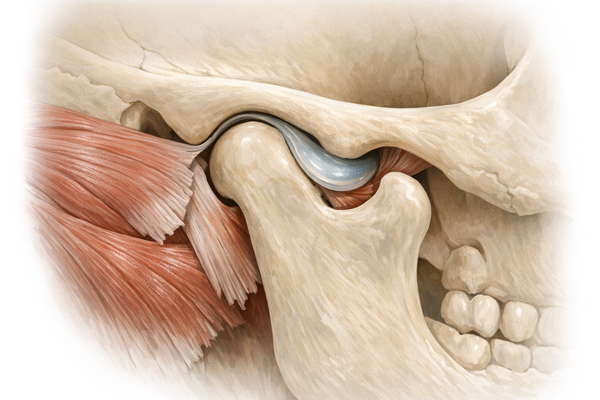
- Clicking in the temporomandibular joint (TMJ)
- Disturbed sleep for you or your bed partner
Because many people grind subconsciously, dentists often discover the issue first when they see flattened cusps or micro-fractures.
Contributing Factors
The same review by Oliveira et al. highlights genetic polymorphisms in dopamine and serotonin pathways that may prime certain brains for overactive jaw muscles. Yet genes do not act alone. Stress, sleep fragmentation, lifestyle habits (like caffeine and alcohol), and some medications can amp up the central nervous system and trigger rhythmic muscle activity. Bruxism is less a dental problem and more a whole-body puzzle. Understanding the impact of caffeine and other lifestyle factors can offer additional insights.
Medication-Induced Bruxism
Certain prescription drugs ramp up neural activity in ways that can spill over into the jaw. Selective serotonin re-uptake inhibitors (SSRIs) and amphetamine-derived ADHD medications are common culprits. For example, David, a 38-year-old software engineer, noticed intense nighttime grinding within two weeks of starting escitalopram for anxiety. When his psychiatrist reduced the dose and split it between morning and afternoon, the bruxism eased without sacrificing mood control. For those dealing with stimulant-induced grinding, explore our article on Adderall and Teeth Grinding.
Medications most often linked to grinding include:
- SSRIs and SNRIs (fluoxetine, sertraline, venlafaxine)
- Stimulants for ADHD (methylphenidate, amphetamine salts)
- Atypical antipsychotics (olanzapine, risperidone)
- Dopamine agonists used in Parkinson’s disease
If you suspect a drug trigger, do not stop suddenly. Discuss your symptoms with the prescriber—often a timing tweak or alternative medication calms the jaw without derailing treatment goals.
The Role of Relaxation Techniques in Managing Bruxism
Progressive Muscle Relaxation
When your nervous system constantly operates in fight-or-flight mode, the jaw muscles rarely relax. Progressive muscle relaxation (PMR) involves tensing and then slowly releasing muscle groups from toes to forehead, ending with the masseter and temporalis. A 2025 randomized clinical trial by Tandon et al. compared PMR plus sleep hygiene against a standard occlusal splint. After eight weeks, both groups reported lower perceived stress, but the PMR group logged a sharper drop in bruxism episodes per hour of sleep, as measured by electromyography.
To try PMR yourself:
- Lie in bed on your back. Breathe in for four counts, hold for two, and breathe out for six.
- Clench your fists for five seconds, then release. Notice the difference in tension.
- Work upward through calves, thighs, abdomen, shoulders, and finally the jaw.
- When you reach the jaw, bite lightly for five seconds, release, and let the tongue rest on the palate.
Practice nightly for at least two weeks to give neural circuits time to adapt.
Guided Imagery: An Under-the-Radar Add-On
If you struggle to feel the subtle drop in muscle tone, layering guided imagery on top of PMR can magnify the effect. Picture warm sunlight melting away tension in each area you relax. Small imaging studies show that sensory visualization recruits the same cortical areas that govern real motor output, giving your brain a double reminder to let go. Free audio tracks are plentiful on meditation apps—search for “jaw relaxation” or “body scan.”
Sleep Hygiene Practices
Even perfect relaxation training will flop if you keep scrolling TikTok under the covers. Blue light delays melatonin release and fragments sleep stages. Build a routine that supports circadian rhythm:
- Power down screens an hour before bed.
- Keep the bedroom at 60–67 °F (15–19 °C).
- Limit caffeine after lunch and alcohol within three hours of bedtime.
- Use consistent wake and sleep times, even on weekends.
Consider objective feedback: many smartwatches now track micro-arousals that correlate with grinding spikes. If data confirm restless nights, a $30 pair of blue-blocking glasses or a weighted blanket may be the cheapest “device” you ever buy. For more on how sleep influences bruxism, see our article on sleep positions and teeth grinding.
Dietary Changes and Their Impact on Bruxism
Anti-inflammatory Diet
Chronic stress sparks systemic inflammation, and inflamed tissues can sensitize nerves, including the trigeminal system that supplies the jaw. A 2025 review by Liye An et al. links high-sugar, ultra-processed diets to elevated cytokines that worsen oral muscle pain. Conversely, Mediterranean-style eating—rich in omega-3 fatty acids, leafy greens, nuts, and colorful fruits—dampens inflammatory cascades.
Key anti-inflammatory swaps:
- Replace refined grains with quinoa or brown rice.
- Use olive oil instead of seed oils high in omega-6.
- Snack on walnuts or almonds rather than chips.
- Eat fatty fish (salmon, sardines) twice a week.
Micronutrients That Matter
Magnesium supports muscle relaxation by antagonizing calcium influx in nerve terminals. Low levels, common in people who rely on processed food, can keep jaws on a hair-trigger. Leafy greens, pumpkin seeds, and dark chocolate (70% cacao) are tasty fixes. Calcium and vitamin D also stabilize neuromuscular firing—so pair that chocolate square with a glass of fortified plant milk if dairy is off the table. For more on magnesium's role, see our article on magnesium deficiency and teeth grinding.
Gut Health
Your gut microbiome talks to the brain via the vagus nerve, shaping mood and stress resilience. The same Liye An paper notes that dysbiosis—an imbalance of gut bacteria—can heighten anxiety and muscle tension, creating fertile ground for bruxism. Prebiotic fibers (in onions, garlic, and oats) plus fermented foods (kefir, kimchi) feed beneficial microbes, which churn out short-chain fatty acids that tone down inflammation.
You do not need to count colony-forming units like a lab tech. Aim for 25–30 g of fiber daily and a serving of fermented food. If digestive woes persist, a registered dietitian can help tailor a plan. For inspiration, a “jaw-friendly” sample plate might include grilled salmon over quinoa, a side salad with mixed greens and olive oil, and a small bowl of kefir-based tzatziki.

Innovative Approaches: Neuromodulation and Electrical Stimulation
Transcutaneous Auricular Vagus Nerve Stimulation
Enter the gadget era. Transcutaneous auricular vagus nerve stimulation (TAVNS) delivers low-level electrical pulses to the cymba concha region of the ear, hitchhiking on the auricular branch of the vagus nerve. In a 2026 randomized controlled trial by Guzel Hazel Celik et al., participants used TAVNS for 20 minutes before bedtime over four weeks. Compared with sham stimulation, the active group saw a 47 percent reduction in nighttime muscle bursts on polysomnography and reported fewer morning headaches.
Real-world note: Ana, a 29-year-old graduate student, bought an over-the-counter TAVNS ear clip for about $160 after her dentist suggested it. She wears it while reading in bed; within two weeks, she no longer woke up with temple soreness. Side effects were limited to a slight warmth around the ear that faded within minutes.
Contingent Electrical Stimulation
Contingent electrical stimulation (CES) takes biofeedback to the next level. Devices such as GrindCare® stick to the skin over the temporalis muscle and monitor electromyographic activity. When they detect a clench, they deliver a rapid, painless pulse that prompts immediate muscle relaxation. A 2025 perspective by Sladeckova et al. argues for short-term use during tooth wear rehabilitation, noting that CES can cut bruxism episodes by up to 60 percent within two weeks.
Unlike a mouth guard, CES aims to rewire the reflex arc. Over time, the brain learns that clenching triggers an unpleasant buzz and backs off. Think Pavlov, but instead of a bell, it is a microcurrent.
Alternative Therapies: Acupuncture and Physical Therapy
Laser Acupuncture
If needles make you squeamish, low-level laser acupuncture might be the gateway. A 2025 randomized controlled trial by Rashed et al. on children with bruxism used a 904 nm infrared laser on classical acupuncture points (ST6, ST7, LI4). Over eight sessions, the laser group showed greater reductions in nocturnal muscle activity than a physical therapy control. Though pediatric, the findings hint that photobiomodulation can modulate neurotransmitters such as serotonin, which in turn calm masticatory muscles.
Laser acupuncture is non-thermal and painless. Sessions are short—often ten minutes—and adverse events are rare.
Physical Therapy Benefits
Manual stretching of the masseter and pterygoid muscles, postural correction, and cervical spine mobilization can unstick tight fascia that feeds into jaw mechanics. The same Rashed study reported that children receiving physical therapy still improved, just not as dramatically as the laser group. Adult protocols typically include:
- Gentle intraoral massage of the medial pterygoid
- Isometric strengthening of cervical flexors
- Retraining tongue posture using the “N” position (tip behind upper incisors)
Desk jockeys take note: forward-head posture increases TMJ load by up to 10 kg. A simple chin-tuck exercise—glide the head straight back, hold five seconds, repeat ten times—performed twice daily can offload the jaw. Set a phone reminder so good posture does not rely on willpower alone. If you experience jaw pain, our guide on jaw pain treatment may offer additional strategies.
Link Between Bruxism, Stress, and Sleep Disorders
Stress-Induced Bruxism
Teeth grinding is basically your body’s Morse code for “I’m stressed.” The Liye An review details how cortisol—and its inflammatory sidekicks IL-6 and TNF-α—heighten muscle excitability. Meanwhile, a 2024 scoping review by Nascimento et al. in children and teens found that psychological stressors correlated with both awake and sleep bruxism, often co-occurring with tension-type headaches.
Picture an accountant closing fiscal-year books: shoulders hunched, jaw clamped, breathing shallow. Five minutes of paced breathing—inhale four, exhale eight—before a stressful task can pre-empt that clamp-down. Pair it with a sticky note on the monitor reading “Unclench.” Small, silly cues work.
Bruxism and Sleep Quality
Poor sleep begets grinding, which in turn degrades sleep. It is a loop worth breaking. Fragmented sleep elevates catecholamines, priming jaw muscles for overactivity. Conversely, solid slow-wave sleep boosts growth hormone release, which repairs muscle microtears. For more on whether night guards affect sleep quality, consider our article on night guards and sleep.
For stubborn insomnia, consider a sleep study to rule out obstructive sleep apnea (OSA). Data from the Sleep Foundation show that up to a quarter of OSA patients also grind, possibly due to arousal-related muscle bursts. Treating apnea with CPAP or oral advancement devices often tames the grinding too.
Conclusion: A Holistic Approach to Bruxism Management
Bruxism is not just a dental nuisance. It is a window into how your nervous system, diet, stress levels, and sleep architecture interact. Research reviewed here points to a toolbox far bigger than the classic mouth guard: progressive muscle relaxation, guided imagery, anti-inflammatory eating, micronutrient optimization, vagus-nerving gadgets, laser acupuncture, physical therapy, and stress control. None is a silver bullet, but together they form a holistic plan that tackles root causes instead of masking symptoms. Talk with your dentist, physician, or physical therapist about mixing and matching these natural solutions. Your jaw—and whoever shares your pillow—will thank you.