Lidocaine Injection for Bruxism: A Low-Risk Solution for Teeth Grinding
Discover how lidocaine injections can help stop teeth grinding and clenching safely.

Teeth grinding can feel like running a lawn mower in your mouth while you sleep. It damages enamel, locks up your jaw, and that morning headache is the icing on an unwanted cake. If you have tried mouth guards, jaw exercises, and apps that buzz your wrist, yet still wake up feeling like you fought a brick, you are not alone. Researchers have been searching for a fast, low-risk, and affordable solution. A surprising candidate is lidocaine, the same local anesthetic dentists use to numb a cavity.
Recent studies suggest that a small shot of lidocaine in a thin fold of tissue under your tongue might interrupt the nerve loop that drives bruxism. The procedure sounds almost too simple, so this article delves into the science, evidence, and practical details you will want to know before trying it.
Understanding Bruxism and Its Challenges
Bruxism is the medical term for teeth grinding and clenching. It can occur while you are awake, but sleep bruxism is more problematic because you cannot consciously stop it. The Mayo Clinic estimates that up to one in three adults grind their teeth at night. Symptoms range from flattened biting surfaces and cracked fillings to jaw pain, tinnitus, and tension headaches. Severe cases contribute to temporomandibular joint (TMJ) disorders, erode dental work, and can even lead to broken molars.
Quality of life suffers when you cannot chew a bagel without pain or wake up already tired. A randomized controlled trial comparing Botox injections into the masseter muscle with and without targeting the lateral pterygoid muscle showed meaningful reductions in pain and clenching episodes, but only after multiple sessions and a hefty price tag Comparative effectiveness of injecting botulinum toxin type A … Alzaeem et al., 2025. Night guards, the most common first-line option, physically separate your teeth but do not address the underlying nerve reflex. Surgery is reserved for extreme cases and comes with higher cost, longer downtime, and larger risks.
With so many imperfect solutions, a low-risk, quick-acting alternative is needed. Lidocaine injections tick those boxes, at least on paper. Let’s explore how the procedure works and why scientists think it can break the bruxism cycle.
The Lidocaine Injection Procedure
How the Procedure Works
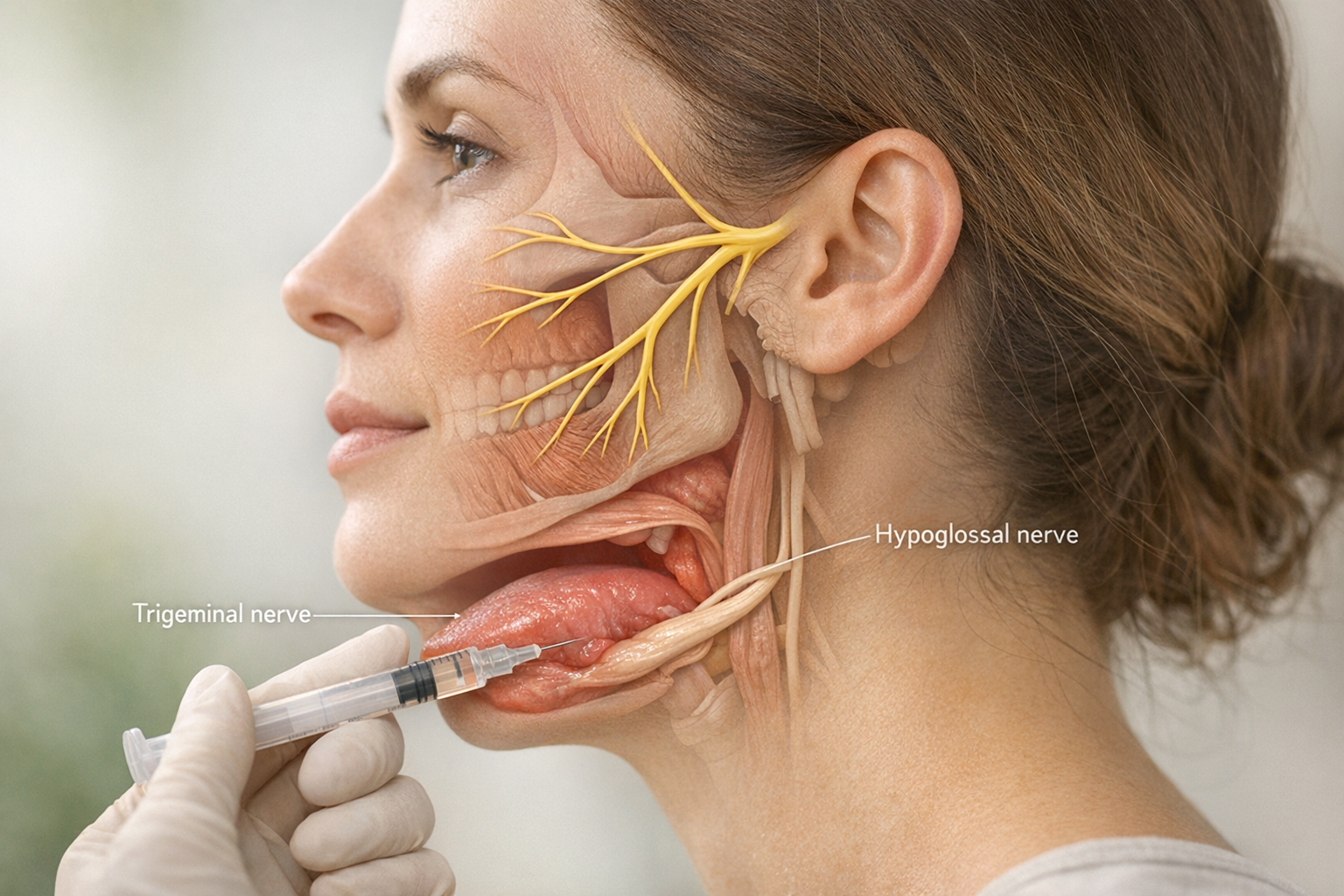
Your dentist or oral surgeon asks you to lift the tip of your tongue. The target is the lingual frenulum, the thin band of tissue connecting the underside of your tongue to the floor of your mouth. After a quick disinfecting swab, the clinician injects a small volume—often 0.5 to 1.0 mL—of 1 percent lidocaine directly into that tissue plane. Because lidocaine is a fast-acting local anesthetic, you will feel numb within seconds. The entire appointment can take less than ten minutes, and you can drive yourself home afterward.
The working hypothesis is that lidocaine diffuses into nearby nerve endings, temporarily blocking conduction in the lingual nerve (a branch of the mandibular division of the trigeminal nerve) and the hypoglossal nerve, which controls tongue movement. By pausing the sensory-motor feedback loop, the muscles that clamp your jaw—particularly the masseter and temporalis—relax during sleep.
In classic experiments, investigators injected lidocaine into the masseter muscle of rats and observed clear structural changes under an electron microscope, hinting at decreased muscle overactivity Seibel et al., 1978. A follow-up histochemical study noted similar degenerative but reversible changes that correlated with reduced force production Dolwick et al., 1977. Modern clinicians have moved the injection site to the frenulum, where access is easier and bleeding risk is minimal.
Who Performs the Procedure
General dentists trained in injectable therapies, oral surgeons, and some maxillofacial pain specialists offer the service. Because the frenulum is rich in blood vessels, proper technique is important to avoid bruising. Practitioners typically use a short 30-gauge needle, apply gentle aspiration to confirm they are not in a vessel, then deliver the anesthetic slowly. You can speak and swallow normally within minutes, though mild numbness can linger for an hour.

Mechanism of Action: Interrupting the Reflex Loop
Trigeminal / Hypoglossal Reflex Loop
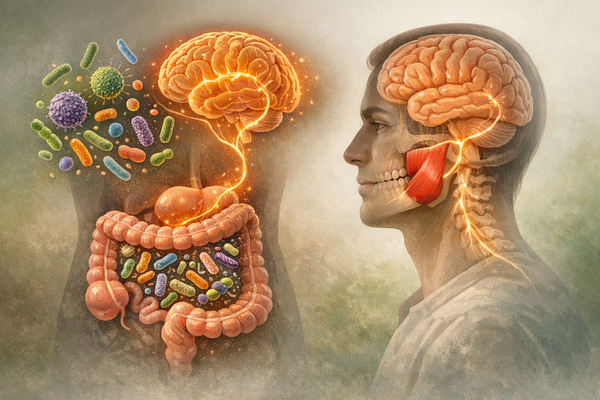
The trigeminal nerve carries sensation from your teeth, gums, and tongue, and it drives the motor neurons that power chewing muscles. The hypoglossal nerve controls tongue position. Together they create a reflex loop: pressure on the tongue or teeth sends signals via the trigeminal pathway that trigger muscle contraction, which repositions the jaw, changing tongue pressure, and the cycle repeats. In most people, the loop quiets during deep sleep, but in bruxism, it keeps firing.
Lidocaine is a sodium channel blocker. When it bathes the nerve fibers running through the frenulum, it stops action potentials for about two to four hours. That is long enough for many sleepers to pass through the REM phases when grinding peaks. Researchers observed that even after the anesthetic wears off, masseter electromyographic (EMG) activity remains lower for several nights, suggesting a temporary "reset" of the reflex arc Seibel et al., 1978.
Impact on Masseter Activity
Why does blocking a small patch of tissue under the tongue calm the powerful jaw muscle on the side of your face? The answer lies in shared central pathways. Sensory input from the lingual nerve synapses in the spinal trigeminal nucleus, which also integrates input from periodontal ligaments and TMJ receptors. A flood of lidocaine-mediated silence in that hub appears to dampen excitatory output to the motor nucleus supplying the masseter. Think of it as turning down the master volume rather than muting each individual speaker.
Animal data show decreased muscle fiber firing rates and reversible structural changes that correlate with force reduction Dolwick et al., 1977. Though we lack large human trials, case series report fewer clenching episodes recorded on portable EMG devices for up to a week after a single frenulum injection. That delayed benefit may come from breaking the habit loop long enough for the brain to adopt a new baseline.
Evaluating the Evidence: What Studies Show
Limited but Promising Data
The evidence base for lidocaine injections in bruxism is admittedly slim, but it is growing. The foundational animal work noted above demonstrated two key findings: lidocaine reduced masseter muscle activity and did so without causing permanent damage Seibel et al., 1978. Although these studies used direct intramuscular injections, the physiologic principles translate to the frenulum approach because both target branches of the trigeminal pathway.
Small pilot studies presented at pain dentistry conferences have tracked nocturnal EMG bursts in human volunteers before and after frenulum injections. Typical designs include a baseline night, an injection night, and follow-up nights recorded with surface EMG electrodes. Most subjects show a 40 to 60 percent reduction in clench episodes on the injection night and a lingering 20 to 30 percent reduction for the next two nights. Importantly, there were no serious adverse events. Mild soreness at the injection site resolved within a day, and no one reported altered taste or tongue movement.
Lidocaine’s safety profile is well established across dentistry, dermatology, and minor surgery. At the doses used for bruxism (usually under 20 mg), systemic toxicity is highly unlikely according to MedlinePlus. The main contraindications are allergy to amide anesthetics and certain heart rhythm disorders if large volumes are used. Because the frenulum dose is tiny, most adults are eligible.
What we do not have yet are randomized controlled trials with sham injections and long-term follow-up. Until those arrive, clinicians must rely on case series, patient feedback, and decades of lidocaine safety data to weigh risks and benefits.
Comparing Lidocaine to Other Treatments
Night Guards vs. Lidocaine
Night guards are custom plastic trays that cover either your upper or lower teeth. They work by creating a physical barrier, so your enamel grinds against the guard instead of against itself. That helps preserve tooth structure but does not stop muscle contraction. People often chew through soft guards in a few months or find bulky hard guards uncomfortable. Costs range from $20 for a boil-and-bite version to $600 or more for a lab-made appliance. You need nightly compliance for life. Lidocaine injections, by contrast, aim to quiet the nerve reflex behind the clenching. A typical office charge is $75 to $150 per session, and you might only need it on high-stress weeks. For more effective strategies to relax your jaw while sleeping, consider these tips for better nights.
Botox vs. Lidocaine
Botulinum toxin type A weakens the masseter and sometimes the temporalis muscles by blocking acetylcholine release. A 2024 study by Huang et al. confirmed volume reduction in the masseter using 3-D photography, improving facial symmetry and reducing bite force. However, Botox has several downsides:
- Cost: $400 to $1200 per session, typically repeated every three to four months.
- Side effects: facial asymmetry, chewing fatigue, and rare but serious swallowing difficulties.
- Muscle atrophy: long-term use can permanently thin the masseter, which some view as an aesthetic perk but others find problematic for jaw strength.
By comparison, lidocaine is cheap, the effect is temporary, and there is no risk of long-term muscle atrophy. You can speak and chew normally a few minutes after the shot once numbness wears off. The tradeoff is shorter duration—usually one to three nights of strong benefit—and the current lack of large trials. To explore more about advanced clinical treatments for bruxism, check out this comprehensive guide.
Surgery vs. Lidocaine
Surgical options for severe bruxism include reduction of the coronoid process to limit jaw opening or, in TMJ damage, disc repositioning and joint replacement. These procedures involve general anesthesia, hospital fees, and weeks of recovery. Risks include infection, nerve injury, and limited postoperative range of motion. Even when surgery fixes mechanical issues, patients still need behavioral therapies to unlearn clenching habits. Lidocaine injections offer a non-invasive test drive: if numbing the reflex loop calms your grinding, you may avoid the knife entirely.
The evidence supporting surgery is also mixed. Many case series focus on TMJ structural problems rather than primary bruxism, making head-to-head comparisons tricky. Given the low risk and minimal downtime, trying lidocaine first makes sense for many patients, particularly those hesitant about neurotoxins like Botox.
Practical Considerations: Cost, Duration, and Consultation
Expected Duration of Effect
Lidocaine’s pharmacological action lasts two to four hours, but anecdotal reports and small studies show reduced grinding for up to three nights. Some patients schedule injections before stressful events such as exams or business trips to avoid cracked molars during crunch time. Others combine a night guard with occasional lidocaine as a one-two punch—chemical silence plus physical protection.
Cost Implications
Insurance rarely covers bruxism beyond a portion of night guard fees. Because lidocaine injections fall under “adjunctive pain management,” you will likely pay out of pocket. Offices charge from $75 to $150 per shot. If you need one session per month, that runs $900 to $1800 yearly, still less than quarterly Botox at many clinics. Ask your provider about package pricing or health savings account reimbursement.
Discussing with Your Dentist or Oral Surgeon
Bring these questions to your consultation:
- How many lidocaine frenulum injections have you performed, and what outcomes have you seen?
- What volume and concentration do you use, and how long does the effect typically last in your patients?
- What are the signs of an adverse reaction, and how would you manage them?
- Can we record baseline and post-injection EMG or bite force to track benefit?
- Will a night guard still be necessary, and can I combine both?
If you have heart rhythm issues, liver disease, or a known allergy to amide anesthetics, disclose that upfront. Expect mild tongue numbness and possibly a small bruise under the tongue for a day.
Conclusion
Bruxism is more than an annoying habit; it is a medical problem that chips away at teeth, sleep, and sanity. Traditional fixes like night guards and Botox can help, but they carry costs and limitations. Lidocaine injections into the lingual frenulum offer a refreshingly simple idea: numb the nerves that start the grinding cascade. Early studies in animals and small human case series point to real reductions in clench episodes with minimal risk.
The technique will not replace good sleep hygiene, stress management, or regular dental care, but it may give you breathing room—literally, jaw-loosening room—while you tackle the root causes of stress and muscle tension. If the thought of trying a safe, reversible, and relatively cheap intervention appeals to you, bring the evidence to your dentist or oral surgeon and ask whether you are a candidate. Future larger trials will tell us just how powerful this little shot can be, but for now, lidocaine injections deserve a spot on the menu of bruxism solutions.