Jaw Pain Anxiety or Heart Attack: How to Tell the Difference
Learn to distinguish jaw pain from anxiety vs heart attack. Essential for health-conscious readers.
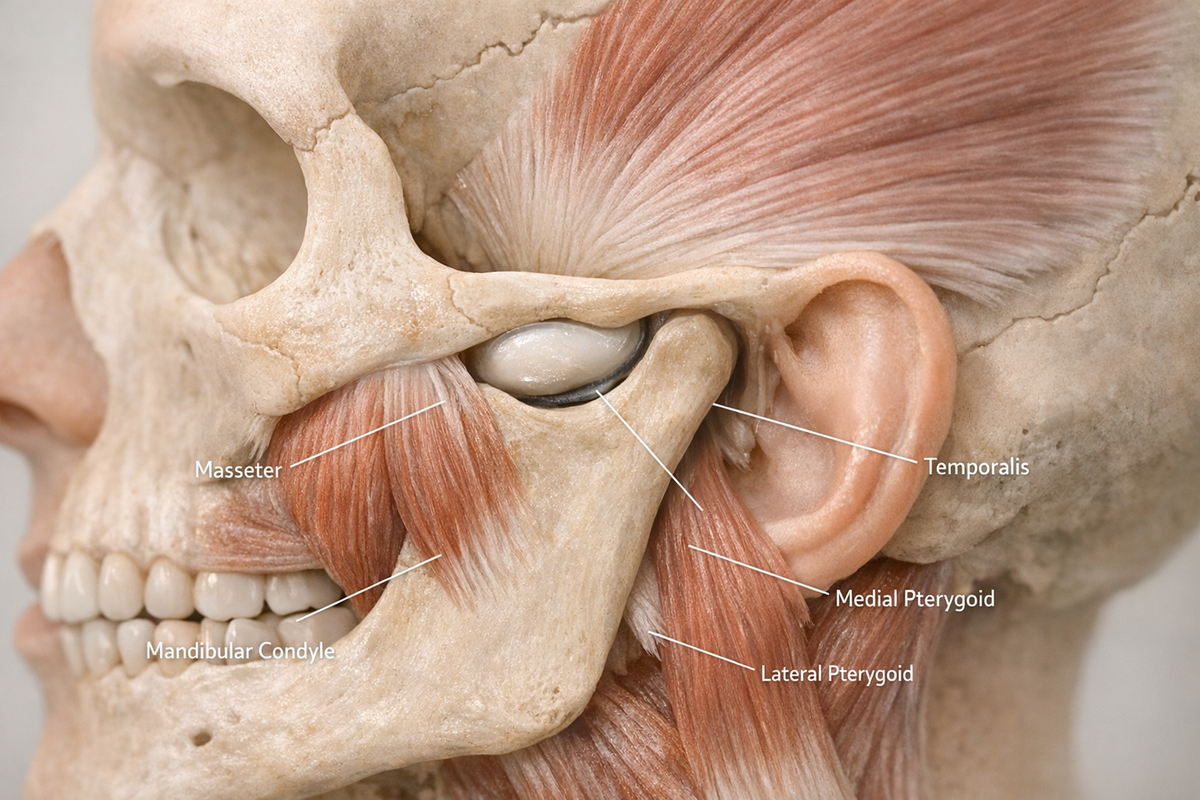
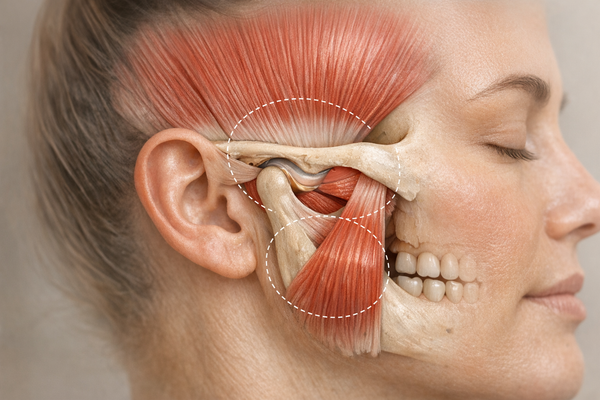
If you wake up with a throbbing jaw, it can feel like your face is trying to file a complaint with management. The big question is whether that ache is coming from anxious muscle clenching or from something far more serious, like a heart attack. The fear is understandable because the same piece of real estate—your lower face—can broadcast both messages. This article walks you through the science so you can tell which alarm bell is ringing and what to do next.
Everything below is distilled from peer-reviewed studies, mainstream medical guidelines, and seasoned clinical wisdom. You will see the research linked in real time, so you can fact-check while you sip coffee and massage that stubborn masseter muscle. Let’s dig in.
Understanding Jaw Pain: Anxiety or Something More?
Causes of Jaw Pain
Jaw pain is not one single condition. It is an umbrella term that covers muscle soreness, joint dysfunction, nerve irritation, dental problems, and even referred pain from the heart. One of the most common structural causes is a temporomandibular joint disorder, often shortened to TMJ or TMD. Studies indicate that TMD affects up to 12 percent of adults in short-term studies, with notable spikes among people who grind their teeth at night (bruxism).
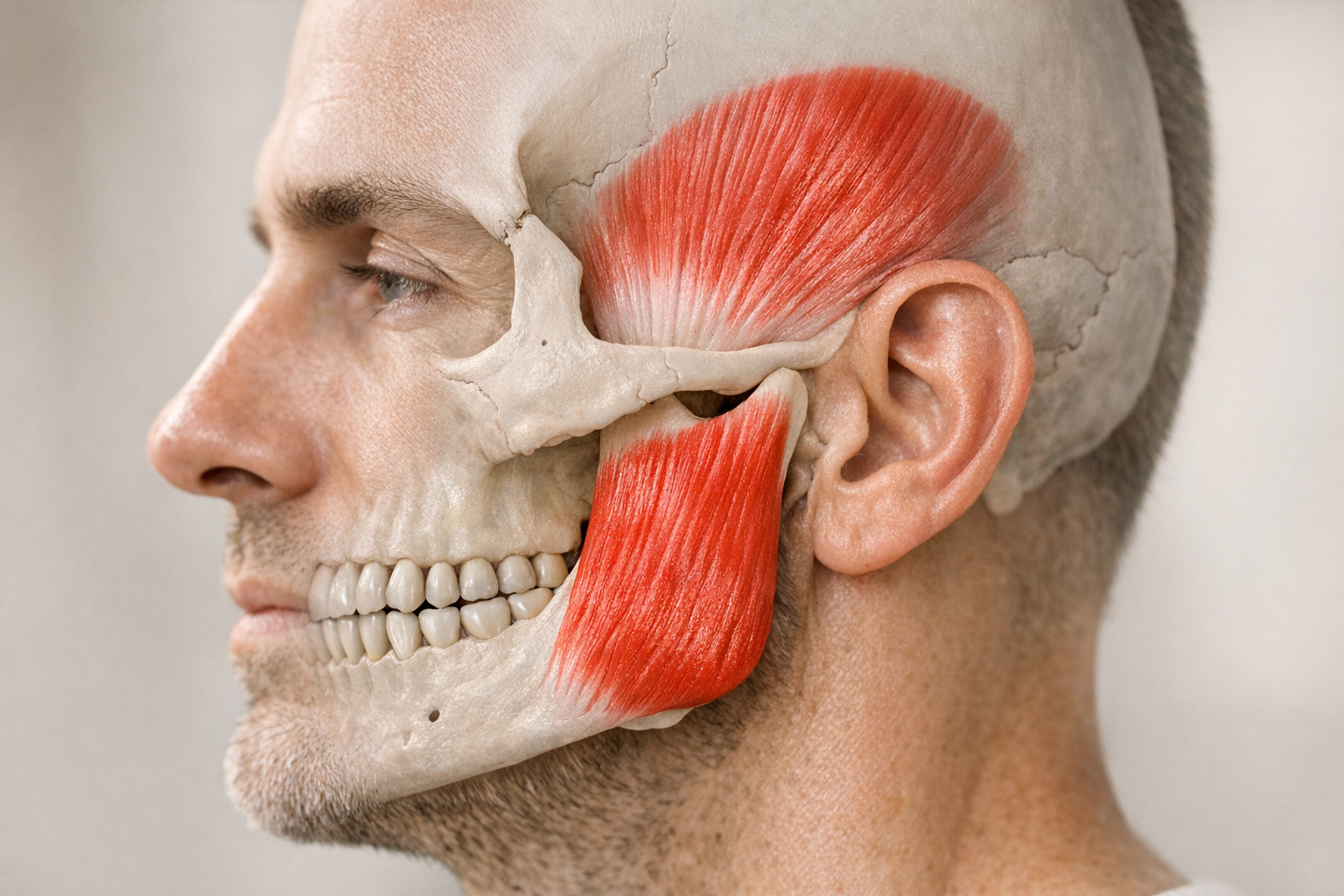
Muscular overuse also plays a starring role. Picture your masseter and temporalis muscles doing overtime when you chew gum all day, bite your nails, or clamp your teeth during high-stakes Zoom calls. Because the jaw is part of a kinetic chain that includes the neck and upper back, poor posture can amplify every twinge. Tilt your head forward to look at a phone and the leverage forces on the TMJ nearly double, according to a biomechanical simulation from the University of Otago. People who rack up four or more daily hours in the classic “tech-neck” position showed a 26 percent rise in jaw-muscle electromyographic activity. The fix is as simple as lifting screens to eye level and sprinkling in chin-tuck exercises, but the payoff can be dramatic.
Add dental infections, sinusitis, arthritis, or even tumors of the salivary glands to the list, and you see why jaw pain is a tricky detective case.
Importantly, pain does not always stay loyal to its birthplace. Heart tissue and jaw tissue share the same spinal nerve roots, so inflammation in the heart can masquerade as an ache along your jawline. That overlap is the reason chest-free, silent heart attacks sometimes present as nothing more than jaw or neck pain, especially in women and people with diabetes.
Role of Anxiety in Jaw Pain
Your brain is hardwired to prepare the body for action whenever you feel threatened. That means faster heartbeats, shallower breaths, and—crucially—tightened jaw muscles primed to fight or flee. Chronic stress keeps that system stuck in the on position, leading to clenched teeth during the day and bruxism at night. In animal models of stress, cortisol spikes are linked to both anxiety-like behaviors and measurable changes in the hippocampus. While mice do not file dental insurance claims, the pathway is surprisingly similar in humans.
Another under-appreciated driver is stimulant overload. Large pours of coffee, energy drinks, and certain pre-workout powders jack up adrenaline, nudging muscles toward tonic contraction. Clinicians note that patients who cap caffeine before 2 PM often see their nocturnal grinding drop within a single week. Erratic sleep schedules make matters worse: REM cycles—prime time for emotional processing—get clipped, so the jaw ends up “chewing on” unfinished stress overnight. A predictable lights-out time is therefore a mechanical intervention in disguise.
The net result is “jaw tension anxiety.” You might feel a dull, constant ache that worsens when you are on deadline or scrolling bad news. You may also hear clicking sounds in the joint because your tightened muscles destabilize the jaw hinge, pulling it slightly out of alignment.
Bottom line: anxiety is both a trigger and a fuel source for jaw pain. Keeping stress in check is therefore a first-line treatment, not a wellness afterthought.
Signs of Anxiety-Related Jaw Pain
Symptoms
Anxiety-driven jaw pain usually follows a recognizable pattern:
- A dull, aching sensation along one or both sides of the jaw that flares during stressful periods
- Morning soreness from nighttime teeth grinding
- Headaches originating at the temples and wrapping around the forehead
- Audible clicking or popping when you open wide
- No accompanying chest pressure, arm numbness, or shortness of breath
If you are unsure whether clenching is really happening, try the “tongue test.” Place the tip of your tongue gently between your front teeth whenever worry thoughts creep in. If you catch yourself biting down, the habit is officially active and needs attention. Another low-tech tool is a brief jaw diary: rate discomfort from 0–10 four times a day and jot what was happening right beforehand. Patterns often leap off the page and pinpoint the exact meeting, phone call, or doom-scroll that turns tension into pain.
A study using the Hamilton Anxiety Rating Scale on medical students found that higher anxiety scores correlated with self-reported jaw stiffness, confirming a mind-jaw feedback loop. Physical therapists often label this loop “stress clench syndrome,” an unofficial term but one patients remember easily.
Psychological Triggers
The trigger list reads like a modern to-do list: looming exams, work presentations, doom-scrolling before bed, and even high-intensity workouts without adequate cooldowns. Each stressor nudges the sympathetic nervous system—which controls fight-or-flight—into high gear. The jaw muscles, being among the strongest in the body, respond instantly.
Resources such as the Anxiety and Depression Association of America emphasize that jaw tension often appears alongside classic anxiety symptoms: racing thoughts, sweaty palms, and elevated heart rate. Unlike a heart attack, these episodes usually pass once you calm down, meditate, or watch ten minutes of cat videos. Awareness of this psychological runway helps you intercept the tension before pain sets in.
Jaw Pain on One Side: What Does It Mean?
Possible Causes
Unilateral jaw pain sounds scarier than bilateral pain, mainly because it feels lopsided and unfamiliar. But many benign culprits live on that one side:
- Chewing food predominantly on one side, fatiguing the masseter muscle
- Sleeping on one side with your hand under the jaw, compressing the joint
- Dental issues like a cracked tooth or localized infection
- Early TMJ degeneration that targets a single joint surface
Consider Mia, a 28-year-old graphic designer who favored peppermint gum and balanced her phone between shoulder and jaw while multitasking. By the third design sprint of the week, she developed stabbing pain just below her left ear. A dental X-ray showed no decay; her PT traced the issue to asymmetrical chewing compounded by the phone clamp. Two weeks of switching chewing sides, using earbuds, and applying moist heat resolved the pain. The take-home lesson: tiny quirks in daily routine can snowball into unilateral misery.
Less frequent but noteworthy causes include cysts, osteomyelitis, and salivary gland tumors. A rare case report described salivary duct carcinoma presenting first as vague one-sided jaw pain, underlining why persistent, unexplained pain deserves a dental or ENT consult.
When to Worry
One-sided pain crosses into red-flag territory if you also experience:
- Numbness radiating into the ear or arm
- Swelling that you can see or feel
- Difficulty swallowing or opening the mouth fully
- Pain that spikes with physical exertion or emotional stress (possible cardiac involvement)
If any of these occur, schedule medical evaluation promptly. A clinician can rule out cardiac ischemia, neuralgia, or malignancy with targeted imaging and blood work.
Heart Attack Indicators: Jaw Pain and Beyond
Recognizing Heart Attack Symptoms
Heart attacks do not always shout; sometimes they whisper. According to the American Heart Association, only half of patients report the textbook crushing chest pressure. The rest show atypical signs: shortness of breath, cold sweats, nausea, or jaw pain.
Why the jaw? Cardiac nerves converge with cervical spinal nerves that also serve the jaw and neck. Ischemic pain therefore travels a neural expressway to the mandible. Studies have found that roughly 8–10 percent of patients recalled jaw pain as an early warning sign.
Remember, medical nuances matter: people with longstanding diabetes may have blunted nerve signaling (autonomic neuropathy) that mutes traditional chest pain. For them, jaw discomfort plus unexplained fatigue can be the only neon sign. A meta-analysis in the Journal of Diabetic Complications estimated that silent or atypical presentations occur in up to 34 percent of diabetic heart attacks—proof that a low threshold for emergency care saves lives.
Jaw Pain as a Warning Sign
Heart-related jaw pain generally feels different from anxiety pain in three key ways:
- It appears suddenly, often during physical exertion or emotional shock.
- It may radiate downward into the chest or upward into the teeth.
- It is frequently accompanied by systemic symptoms such as dizziness, sweaty skin, or a feeling of impending doom.
Data from Mayo Clinic show that women are more likely than men to present without chest pain, relying on subtler cues like jaw discomfort. Awareness of this gender gap can speed up medical intervention, shaving crucial minutes off door-to-balloon time.
Differentiating Anxiety Jaw Pain from Heart-Related Pain
Symptom Comparison
| Feature | Anxiety Jaw Pain | Heart-Related Jaw Pain |
|---|---|---|
| Onset | Gradual, linked to stress | Sudden, may follow exertion |
| Location | Often bilateral but can switch sides | Usually left-sided but may be central or right |
| Duration | Minutes to hours, relieved by relaxation | Continuous or worsening over 15 minutes |
| Associated symptoms | Headache, teeth grinding | Chest pressure, arm tingling, cold sweat |
| Response to jaw massage | Often improves quickly | No significant relief |
The comparison draws from the same cardiac rehab cohort noted above, which tracked anxiety and depression scores alongside physical symptoms. Participants with anxiety-only pain showed clear relief with muscle relaxants and counseling, while cardiac patients required angioplasty or medication.
Seeking Medical Help
Use the “Rule of Twos” as a shortcut:
- If jaw pain lasts longer than two continuous minutes during rest
- If it scores above two on a 0–10 difficulty-talking scale
…then call emergency services. You lose nothing by checking. Internalizing symptoms research underscores that delayed care worsens both physical and mental health outcomes.
Conversely, if pain predictably coincides with stressful events, lacks systemic red flags, and eases with stretching or relaxation, schedule a dental or psychological evaluation instead of an ambulance ride.

Practical Steps for Managing Jaw Pain
Lifestyle Changes
Your jaw may be small, but it loves a multi-pronged care plan:
- Night guard. Over-the-counter versions are helpful, but a dentist-made guard fits better and can reduce morning soreness by up to 70 percent in observational TMJ studies.
- Mindful breaks. Set a phone alarm every two hours to unclench your jaw. Literally say, “lips together, teeth apart.”
- Magnesium-rich foods. Leafy greens and nuts help muscle relaxation. Supplements may benefit those with documented deficiency.
- Box breathing. Inhale for four counts, hold for four, exhale for four, hold for four. Research on stress models suggests it lowers cortisol, indirectly relaxing jaw muscles.
- Jaw stretches. Place the tip of the tongue on the palate behind your top teeth, then slowly open and close the mouth ten times.
- Ergonomic workstation. Align screens at eye level and keep elbows at 90 degrees. Proper posture unloads the neck and, by extension, the jaw.
Professional Treatments
If lifestyle tweaks do not cut it, bring in the pros:
- Dental assessment. You may need occlusal adjustment, bite splints, or treatment for decay and infection.
- Physical therapy. A PT can teach resistant-release techniques that lengthen the temporalis and masseter muscles.
- Cognitive behavioral therapy (CBT). CBT tackles the thought loops that fuel jaw-clenching anxiety. Randomized trials place its success rate near 60 percent for reducing somatic symptoms.
- Medication. Short-term NSAIDs curb inflammation, while muscle relaxants break the spasm cycle. Always consult a clinician for dosage and duration.
- Botulinum toxin. Off-label jaw injections weaken overactive muscles for three to six months but carry costs and possible side effects.
Conclusion
Jaw pain is a message, not a life sentence. Sometimes the message is “Take a breath, you are stressed,” and sometimes it is the heart waving a red flag. Spotting the difference hinges on patterns: anxiety pain is slow, stress-linked, and muscle-dominated, while cardiac pain is sudden, exertion-linked, and system-wide. Use the symptom comparison table, the Rule of Twos, and above all, your gut instinct. If you are on the fence, err on the side of a medical check.
Meanwhile, protect your jaw with nightly guards, mindful breaks, ergonomic tweaks, and evidence-based relaxation techniques. Your future self—and your dentist—will thank you.