How to Relax Your Jaw When Sleeping: Tips for Better Nights
Discover effective strategies to relax your jaw while sleeping and reduce bruxism for better sleep.

You wake up with a dull ache near your ears, your cheeks feel like they did push-ups all night, and your partner swears you sound like a pestle grinding spices in your sleep. Welcome to the frustrating world of nocturnal jaw tension, also called sleep bruxism. The good news: you can train your jaws to relax while you snooze. Below, you will find research-backed strategies, gadgets worth considering, and lifestyle tweaks that do not involve moving to a mountaintop monastery.
Everything here is rooted in peer-reviewed studies or reputable medical organizations, so you can stop doom-scrolling half-baked tips. Let's dive in.
Understanding Sleep Bruxism and Jaw Tension
Sleep bruxism refers to repetitive jaw-muscle activity during sleep, meaning clenching, grinding, or both. Estimates suggest 5 to 15 percent of adults experience this, often without realizing it until a dentist spots flattened molars or a partner complains about the noise. A solid overview comes from a 2024 narrative review by Leung et al. which highlights that bruxism often coexists with other sleep disorders.
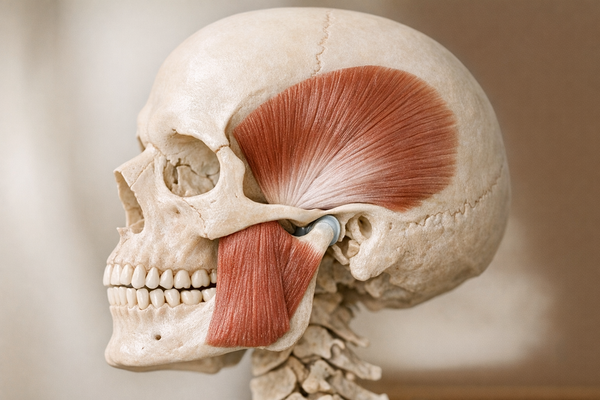
Why does jaw tension happen? Think of your masseter and temporalis muscles as over-enthusiastic security guards. They contract when you are stressed, when your bite feels off, or when your airway narrows. Repeated overnight contractions lead to micro-trauma in jaw joints, morning headaches, and even cracked teeth. If you're unsure whether your jaw pain is related to anxiety or something more serious, our guide on Jaw Pain Anxiety or Heart Attack provides crucial insights.
Genetics also play a role. Twin studies suggest hereditary factors account for up to 50 percent of grinding tendencies. Certain medications—particularly selective serotonin reuptake inhibitors (SSRIs) and amphetamine-based ADHD drugs—can increase nervous system activity at night. If you have recently changed prescriptions and notice new jaw pain, talk with your prescriber before assuming a dental appliance is the lone fix. For more on how medications like Adderall can contribute to bruxism, read about Adderall and Teeth Grinding.
Emerging tech is uncovering new links between bruxism and obstructive sleep apnea (OSA). A 2024 deep-learning EMG study by Rehman et al. used chin muscle signals to screen for OSA, highlighting how jaw-muscle overactivity may be both a clue and a contributor to breathing issues. When the airway collapses, you may reflexively clench to stiffen surrounding tissues, like propping open a sagging tent. Learn more about how sleep positions can influence your nighttime teeth grinding in our article on How Sleep Positions Influence Nighttime Teeth Grinding.
Bottom line: jaw tension is not just a dental nuisance. It is a whole-body sleep problem that deserves a holistic fix.
Effective Jaw Relaxation Techniques for Sleep
Before investing in gadgets, try training your muscles to relax on cue. Two evidence-based methods stand out: progressive muscle relaxation and targeted orofacial exercises.
Progressive Muscle Relaxation
Progressive muscle relaxation (PMR) is a classic technique that involves tightening and then loosening muscles. A 2025 randomized controlled trial by Marițescu et al. found that adults practicing PMR for eight weeks slept longer and reported less subjective stress than a control group. Although the study focused on people with cystic fibrosis, the mechanism—lower sympathetic nervous system arousal—applies to anyone with a clenched jaw.
Here is a quick bedtime PMR script tailored to your face:
- While lying down, inhale and clench your jaw gently for five seconds.
- Exhale and let your jaw drop, visualizing the muscles melting like butter.
- Move to your brow: furrow hard, release.
- Scrunch your eyes, release.
- Work down the neck and shoulders, then finish with slow belly breaths.
The key is awareness. By feeling the contrast between tension and release, you teach your brain to detect and stop unconscious clenching later in the night.
Guided audio tracks can help if you struggle to focus. Apps such as Insight Timer and Calm host free PMR recordings—set one to start ten minutes before your target bedtime so the lights-out ritual becomes automatic. Some people pair earbuds with a low-cost surface-EMG headband (e.g., Muse S) that vibrates lightly when jaw activity spikes, providing real-time biofeedback.
Orofacial Exercises
If PMR is passive stretching, orofacial exercises are akin to weight training for proper muscle balance. A 2025 experiment by Magdič et al. showed that simple cheek and tongue movements reduced reflex activity in the calf muscle, suggesting a whole-body calming effect through the nervous system.
Sample nightly routine (five minutes):
- Jaw drape: Let the lower jaw hang, then say a slow “mah-nah-mah-nah” to keep it loose.
- Tongue push-ups: Press the tip of the tongue to the palate just behind the front teeth for five seconds, repeat ten times.
- Cheek puff: Fill one cheek with air, hold for three seconds, switch sides. Three sets.
- Shoulder rolls: Ten forward, ten backward. Jaw muscles attach near the collarbone, so releasing the shoulder girdle is key.
Do not worry about looking silly. You are training muscle memory so that when sleep kicks in, your default setting is open and easy rather than clamp-mode. Many patients report fewer daytime “micro-clench” episodes after just two weeks because their default oral posture shifts to lips-together, teeth-apart.

Pairing PMR with orofacial drills tackles both neural relaxation and mechanical alignment—your best low-cost bet before moving to dental devices.
The Role of Occlusal Splints in Managing Bruxism
If self-help drills are the warm-up, occlusal splints are the mouthguards that take the night shift. They do not stop jaw muscle activity, but they redistribute forces and protect your enamel. Think bumper lanes at a bowling alley.
A 2024 systematic review by Sultan et al. compared hard acrylic, soft silicone, and dual-laminate splints. Hard splints outperformed soft ones in reducing micro-wear on teeth over 12 weeks, but user comfort leaned in favor of softer designs. Dual-laminate guards offered a Goldilocks compromise—rigid bite surface with cushioned inner layer. For those considering their options, our comparison of Over the Counter Night Guard vs Custom Fitted Night Guard can help guide your decision.
How splints work:
- They create a uniform biting surface, reducing the chance of one rogue tooth triggering a muscle reflex.
- They slightly increase the vertical dimension of the bite, giving elevator muscles (masseter, temporalis) less mechanical advantage to clamp down.
- They serve as biofeedback—if you wake to a mouth full of chewed plastic, you know grinding happened and can adjust stress habits.
Splint ownership comes with homework. Rinse nightly with lukewarm water, brush gently using liquid hand soap (toothpaste is abrasive), and soak in a non-alcoholic denture cleanser once a week to prevent odor. Store in a vented case—leaving it in a steamy bathroom breeds bacteria. Schedule a six-month check-in so your dentist can polish out grooves before they deepen into fracture lines.
Types at a glance:
- Custom lab-made hard acrylic: Highest durability, best fit, pricey.
- Boil-and-bite soft: Cheap, decent starter, wears down faster.
- Dual-laminate: Middle ground, often custom-fabricated.
- Anatomic splints (Michigan, Tanner): Designed to guide jaw into a therapeutic position, usually dentist-prescribed.
The American Dental Association recommends professional evaluation before long-term splint use to avoid shifting your bite the wrong way. A quick read on their site can help you prep for the dental visit. Additionally, our TMJ Mouth Guard guide offers comprehensive insights into selecting the most suitable option for TMJ pain.
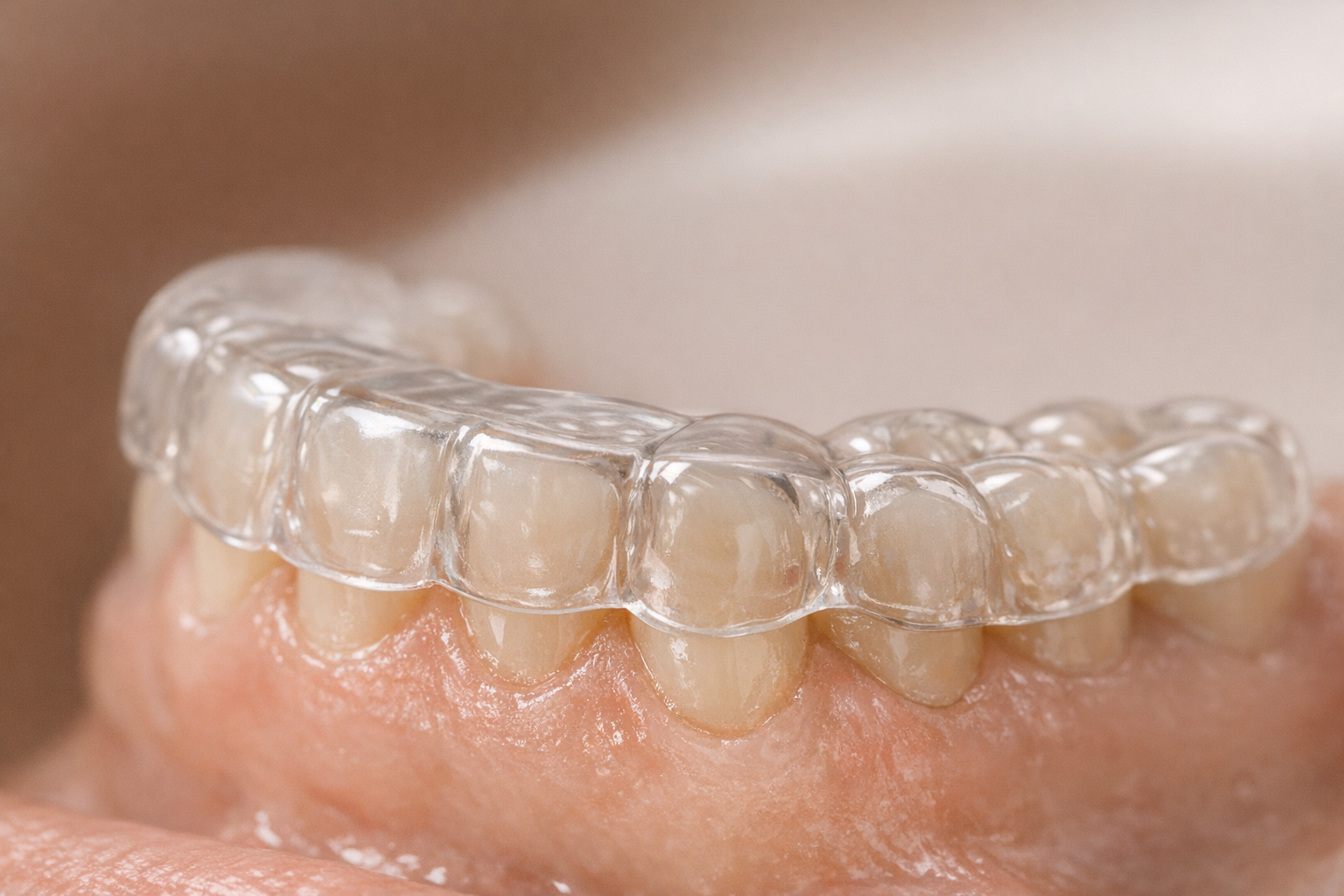
Remember: splints protect teeth but do not cure the root cause of clenching. Combine them with relaxation routines for a comprehensive approach.
Exploring Medical Interventions: Botulinum Toxin Injections
When exercises and plastic shields fail, some turn to injections. Botulinum toxin type A (BoNT-A) works by blocking acetylcholine release at the neuromuscular junction, essentially telling overactive muscles to relax for three to four months. For a deep dive into the use of Botox for bruxism, our article on Botox for Bruxism provides valuable insights.
A 2025 systematic review by Yacoub et al. pooled data from 15 clinical trials and found that BoNT-A reduced self-reported pain scores by around 60 percent within one month compared to placebo saline. Bite-force measurements also dropped, meaning less destructive grinding.
Typical dosing ranges from 25 to 40 units per masseter, spaced evenly across three to four injection points. Most clinicians start low and titrate up in later sessions, so do not judge efficacy by the very first round. Insurance coverage varies; codes usually fall under “therapeutic chemodenervation,” so call ahead to avoid surprises.
Pros:
- Rapid symptom relief—many notice change within a week.
- Minimal downtime—you can go back to work the same day.
- No permanent alteration of bite.
Cons and caveats:
- Chewing fatigue can occur, especially with big meals.
- Smile asymmetry if toxin diffuses to facial muscles (rare when administered by experienced clinicians).
- Costly: injections every 3-4 months add up.
- Not a solo act—you still need to manage stress and sleep quality.
Side effects in the review were mild and transient, but choose a clinician familiar with orofacial anatomy—usually an oral and maxillofacial surgeon or a board-certified dermatologist. Pregnant or breast-feeding individuals should postpone treatment until cleared by their OB-GYN.
Lifestyle Changes to Reduce Jaw Tension
Your jaw does not operate in a vacuum. Stress hormones, caffeine habits, and erratic sleep schedules all affect muscle tension. Two practical pillars—stress management and sleep hygiene—pack the most impact.
Stress Management
It is no surprise that stress leads to clenching, but the neuroscience is intriguing. Cortisol and adrenaline prime skeletal muscles for action. If that action never occurs (say you are binge-watching dramas instead of sprinting from a tiger), the surplus energy may exit through nocturnal grinding. To better understand the relationship between stress, anxiety, and jaw tension, our article on Unconsciously Clenching Jaw explores these triggers in detail.
A 2025 study by Matsumoto et al. comparing muscle relaxation styles showed that slower “ramp” methods lowered motor cortex excitability more than ballistic shaking. Translation: ease into relaxation, do not force it.
Try these low-tech interventions:
- Box breathing: Inhale for four counts, hold for four, exhale for four, hold for four. Repeat for two minutes before bed.
- Journaling: Dump worries onto paper so your brain does not replay them overnight.
- Digital sunset: Power down blue-light devices an hour before sleep to reduce sympathetic buzz.
- Slow yoga or tai chi: Gentle movements tie breathing to muscle lengthening, a natural antidote to tension.
- Magnesium-rich snacks: A small banana or handful of pumpkin seeds provides magnesium—shown in small trials to lower excitatory neurotransmitter release and support muscle relaxation.
Learning curves matter. A 2025 systematic review by Ramadhani and Arifin noted that athletes improved concentration the longer they practiced PMR, hinting that consistency beats intensity.
Sleep Hygiene
Good sleep habits make relaxation stick. Think of hygiene as the runway and your jaw as the plane. Smooth runway, smooth landing.
- Regular schedule: Go to bed and wake up within the same 30-minute window daily. Circadian rhythm anchors reduce nighttime micro-arousals that trigger clenching.
- Dark, quiet room: Eye masks and earplugs cost little but cut down sensory spikes that wake muscles.
- Limit stimulants: Caffeine after 2 p.m. and alcohol right before bed can fragment sleep architecture, leading to more grinding episodes. Our article on Avoiding Caffeine Late at Night explains why this is particularly important for those who grind their teeth.
- Side sleeping: Lying on your back may allow the lower jaw to fall backward, narrowing the airway. Side positions often reduce both snoring and bruxism incidents.
- Temperature sweet spot: Around 65–68 °F (18–20 °C) supports deeper stages of sleep and lower muscle tone.
For more guidance, check the Mayo Clinic’s user-friendly primer on TMJ disorders and sleep: Mayo Clinic TMJ tips.
Integrating Mandibular Advancement Devices with CPAP
If you have been diagnosed with obstructive sleep apnea and use CPAP, you might wonder what happens if jaw advancement devices join the party. Enter combination therapy. The upcoming PAPMAT trial (Law et al., 2025) is testing whether adding a mandibular advancement device (MAD) lowers the air pressure needed for CPAP while also curbing bruxism.
Potential benefits:
- MAD pulls the lower jaw slightly forward, opening the airway and decreasing the reflex to clench.
- Lower CPAP pressures mean fewer mask leaks and greater comfort.
- Two treatments address both breathing and grinding rather than playing symptom whack-a-mole.
- Bluetooth-enabled MADs can transmit adherence data to your sleep physician, similar to modern CPAP machines, making remote progress checks easier.
Challenges:
- Fitting an MAD under a CPAP mask can feel bulky.
- Insurance coverage for combined devices is unclear.
- Requires coordination between sleep physicians and dentists.
While final PAPMAT results are pending, early data suggest improved adherence rates when therapies are combined. Talk with your sleep specialist if you suspect OSA is contributing to your jaw tension cycle.
Conclusion
Your jaw muscles are loyal employees—they keep working until told to clock out. By pairing body-based relaxation techniques, protective splints, and targeted medical interventions, you set clear office hours. Research shows PMR and orofacial drills calm neural circuits, splints shield enamel, BoNT-A reduces hyperactive muscles, and good sleep hygiene removes upstream stressors. If you still wake up feeling like you chewed a boot, bring these strategies and study links to a qualified dentist or sleep physician for personalized guidance. Better nights—and quieter mornings—are within reach.