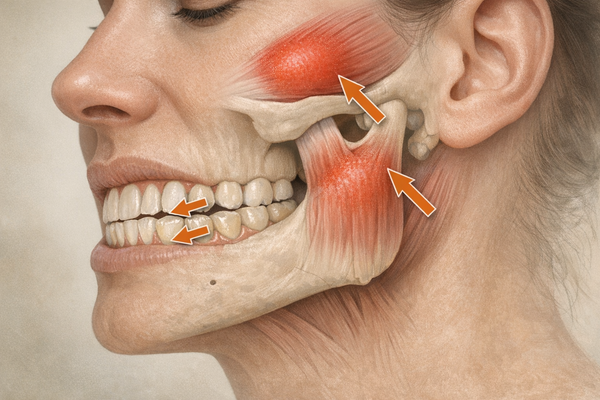
Exploring Biofeedback Therapy for Bruxism Treatment
Discover how biofeedback offers a promising approach to bruxism therapy, examining its effectiveness and mechanisms.
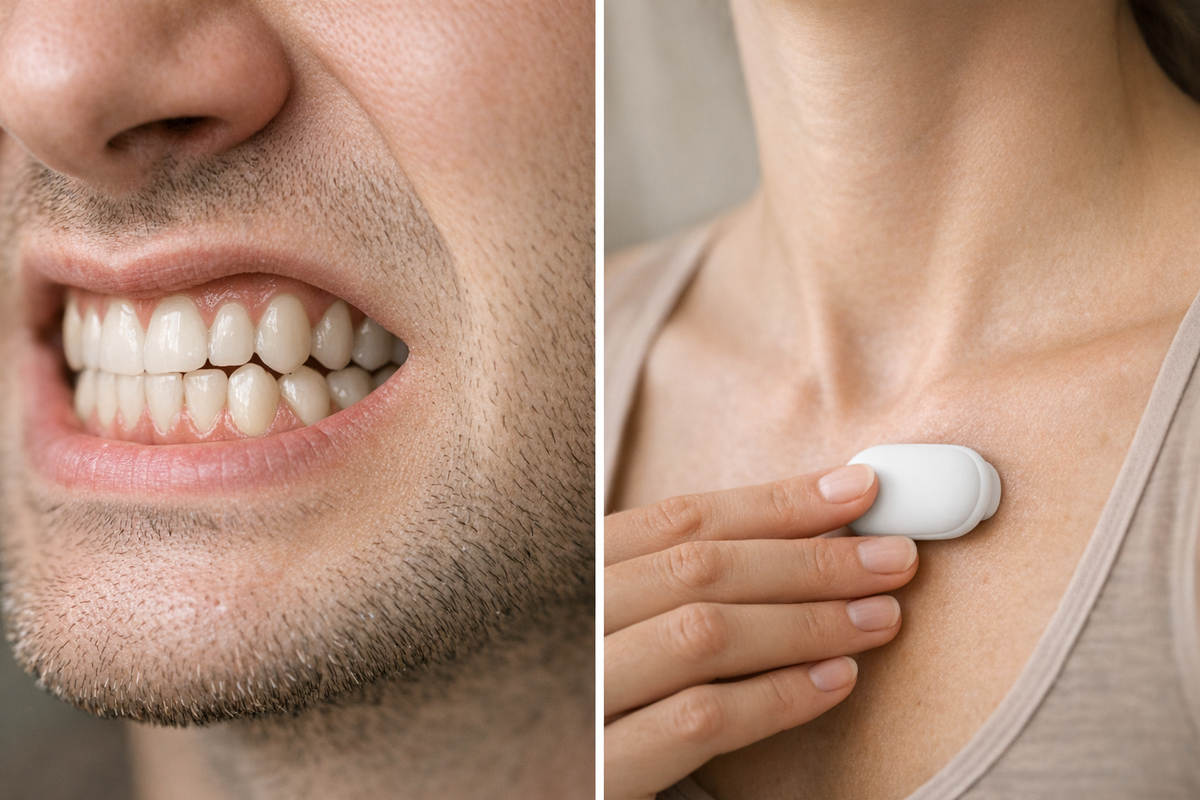
If you wake up with a sore jaw or find yourself going through mouth guards frequently, you're not alone. Teeth grinding, or bruxism, affects many adults and can cause more than just enamel damage. Fortunately, technologies like biofeedback therapy are moving from research labs to personal use. This article explores what recent studies say about biofeedback, how these devices work, and whether they're a good investment for you.
This discussion relies on peer-reviewed evidence and aims to keep things clear and relatable. No confusing jargon—just straightforward answers you might find useful at your next dental appointment.
Understanding Bruxism: Causes and Challenges
What is Bruxism?
Bruxism is the repetitive clenching or grinding of teeth, often during sleep but sometimes when you're awake. According to the Mayo Clinic, this habit can lead to headaches, cracked fillings, and even jaw disorders if left unchecked. A study by Jabłońska and colleagues (2025) estimates that up to 30 percent of adults have some level of sleep bruxism, with numbers increasing during stressful times.
Bruxism isn't constant throughout the night. Research using polysomnography shows two main peaks: one in light sleep just after you fall asleep and another during REM sleep. Many people who believe they grind only a little are unaware of these periods because they occur outside deep-sleep phases when waking is most common.
Experts categorize bruxism into two main types:
- Sleep bruxism: Involuntary muscle activity during light or REM sleep cycles.
- Awake bruxism: Semi-voluntary jaw clenching often linked to concentration or anxiety. Learn more about the impact of stress and sleep disorders on jaw clenching.
Common Causes and Implications
Why do people grind their teeth? The full answer is still unclear. Multifactorial models, summarized in a 2023 overview by Costa et al., point to several possible causes:
- Stress and anxiety: Cortisol spikes can trigger muscle activity. Discover how stress and anxiety lead to nighttime teeth clenching.
- Sleep disorders: Conditions like obstructive sleep apnea may share pathways with bruxism.
- Medications: Some antidepressants and stimulants mention jaw clenching as a side effect.
- Occlusal factors: Misaligned bites might contribute, though evidence is mixed.
Consider a 34-year-old attorney preparing for a case late at night. Her stress levels are high, she's on her second cup of coffee, and she's clenching her teeth subconsciously. By the time she goes to bed, her jaw muscles are already tense, setting the stage for sleep-related bruxism. Multiply that scenario by thousands of stressed professionals, and it's clear why dentists call bruxism a silent epidemic.
The effects go beyond chipped teeth. Chronic grinding can inflame the temporomandibular joint (TMJ), reduce sleep quality, and increase healthcare costs. Traditional treatments like night guards address symptoms but often ignore the underlying muscle overactivity. This gap opens the door for biofeedback, which focuses on retraining the jaw rather than just protecting it. Explore how lifestyle changes can naturally reduce bruxism symptoms.
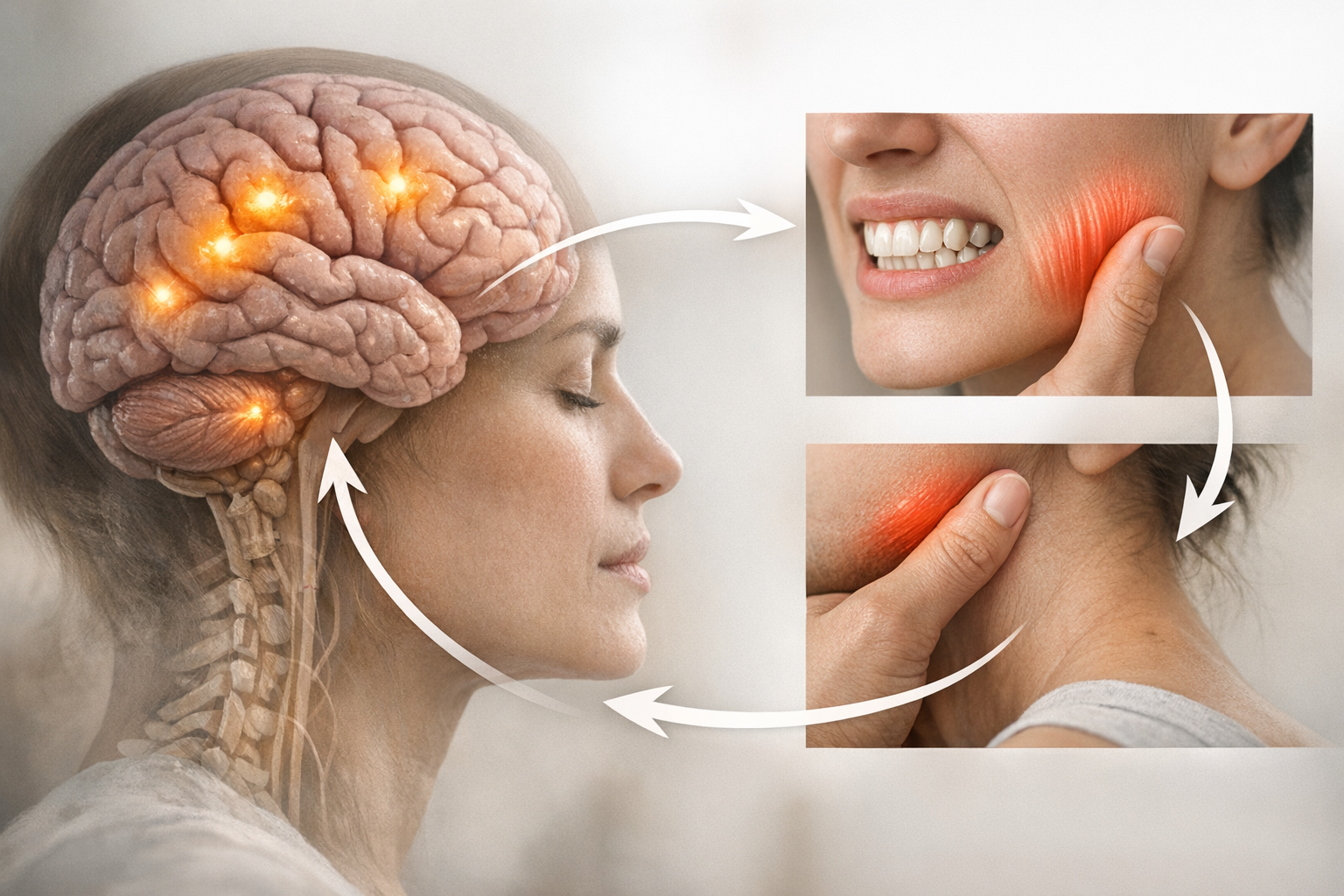
Introduction to Biofeedback: Mechanisms and Applications
How Biofeedback Works
Biofeedback transforms hidden body signals into real-time data you can see or hear. It's like your nervous system holding up a mirror. Sensors detect physiological markers—muscle tension, heart rate, skin temperature—and relay them to a screen or buzzer. The user learns to adjust those signals through relaxation or targeted movement.
The concept dates back decades, but recent technology has made it more accessible. According to an industry report by Yu Zheng (2025), newer devices use electromyography (EMG) signals at high resolution while conserving battery power, making home use feasible. Many devices now connect with phones or smartwatches, allowing users to review grind stats alongside sleep-stage data—a dream for data enthusiasts.
On the clinical front, a review in Heliyon by Calderone et al. (2025) found biofeedback beneficial for chronic pain, hypertension, and migraines by teaching patients to control muscle activity or autonomic responses. The takeaway? If a symptom is linked to a measurable signal, biofeedback could help.
Applications Beyond Bruxism
You might have seen biofeedback in various settings:
- Pelvic floor rehabilitation: Sensors help muscle training post-childbirth or surgery.
- Post-stroke therapy: EMG feedback aids motor pattern rewiring.
- Sports performance: Heart-rate variability monitors keep athletes in optimal zones.
- Mindfulness technology: Headbands play relaxing sounds when brainwaves indicate calmness.
This method is not a cure-all. It requires user engagement and can overwhelm if the interface is not user-friendly. Costs and insurance coverage also vary widely, which we'll discuss later.
Biofeedback for Bruxism: How It Works
Biofeedback Devices for Bruxism
For bruxism, sensors often monitor the masseter or temporalis muscles. Device types include:
- Intraoral appliances: Slim mouthpieces with EMG electrodes detect grinding inside the mouth.
- Surface EMG patches: Adhesive pads attach to the jawline and sync with a smartphone app.
- Ear-centric devices: Small sensors clip behind the ear near the temporalis muscle. These devices are similar to wearable tech used to manage bruxism.
A notable prototype described in a 2025 paper by AL-Hamad et al. involves an intraoral splint with flexible EMG leads and a microprocessor. When grinding exceeds a threshold, the device vibrates gently, prompting the user to unclench without waking fully.
Mechanisms in Action
How does a buzz or beep help with bruxism? Three theories are discussed:
- Operant conditioning: The vibration acts as negative reinforcement, training the brain to stop jaw muscle activity during sleep.
- Startle interruption: The stimulus may briefly disrupt the muscle cycle without disturbing sleep.
- Enhanced proprioception: By highlighting subtle muscle movements, the device increases awareness, reducing daytime clenching under stress.
Most devices include a calibration phase, allowing users to view raw EMG data and adjust sensitivity to avoid excessive buzzing or missing smaller clenches. In lab settings, EMG amplitude often decreases within a few sessions. A study by Zakaria and El Dakrory (2022) on myofascial pain sufferers showed a 40% reduction in pain after eight weeks of EMG biofeedback, suggesting a decrease in grinding frequency as well.

Effectiveness of Biofeedback in Bruxism Therapy
Comparative Studies
Does biofeedback outperform standard care? A couple of systematic reviews offer insights.
Vieira et al. (2023) examined 10 randomized trials on awake bruxism. Biofeedback groups saw a 60% reduction in EMG burst frequency, outperforming relaxation and pharmacotherapy. The evidence was rated as moderate due to small sample sizes.
A second review by the same team in the International Journal of Environmental Research and Public Health (2023) looked at both sleep and awake bruxism. They found biofeedback "demonstrated superior or equivalent outcomes" compared to occlusal splints, especially in reducing daytime clenching.
Success Rates and Patient Outcomes
Beyond EMG data, patients care about pain, dental health, and sleep quality. Here's what the evidence shows:
- Symptom relief: 50-80% of users report reduced morning jaw pain within a month of use. Learn why morning jaw pain could indicate bruxism.
- Dental wear: The AL-Hamad trial found a 33% drop in new enamel cracks over six months.
- Sleep disruption: Polysomnography data show minimal changes in total sleep time, indicating feedback rarely wakes users.
- User satisfaction: Over 70% preferred biofeedback over traditional guards, finding devices lighter and more interactive.
However, the technology isn't flawless. About 20% of participants stopped using it due to skin irritation or device noise. Long-term adherence needs more study. A 2024 meta-analysis in Sleep Medicine Reviews suggests combining regular dental check-ins with app reminders improves retention by 15%.
Alternative Treatments: A Comparative Look
Occlusal Splints
Night guards are a common dental prescription. They distribute bite forces and protect enamel. A review by Sultan et al. (2024) compared soft and hard splints and found similar reductions in self-reported grinding, though neither reduced EMG bursts as much as biofeedback in direct comparisons.
Pros include affordability and no electronics. Cons involve bulkiness and the fact that guards don't stop muscle contractions; they just cushion them. For more information on choosing the right guard, see our guide to the best over-the-counter night guards.
Behavioral Therapies
Cognitive behavioral therapy (CBT) and stress management aim to reduce central arousal triggers. A 2022 review in the Journal of Dental Sleep Research reported mild to moderate symptom reductions, with outcomes varying based on therapist skill and patient commitment. Biofeedback can enhance these methods by providing data for self-monitoring.
Splints, CBT, and medications address parts of the bruxism puzzle. Biofeedback offers targeted muscle training, though possibly at a higher cost.
Practical Considerations: Is Biofeedback Right for You?
Who Should Consider Biofeedback?
The ideal biofeedback candidate:
- Has mild to moderate bruxism confirmed by a dentist or sleep specialist.
- Finds night guards or relaxation exercises insufficient or cumbersome.
- Is willing to engage with technology and track personal data.
- Does not have untreated epilepsy or pacemakers that could interfere with sensors.
In the Vieira review, motivation was a stronger predictor of success than age, gender, or bite alignment. The device's effectiveness depends on your willingness to use it.
Potential Challenges and Considerations
Consider these factors before purchasing:
- Cost: FDA-cleared jaw sensors range from $300 to $800, with limited insurance coverage.
- Learning curve: A calibration phase is necessary for the device to learn your muscle baseline, which may cause false alarms initially.
- Skin and oral comfort: Adhesive allergies and gag reflexes can be problematic.
- Data privacy: Cloud-synced apps store sensitive data, so review privacy policies.
- Professional guidance: Check-ins with a biofeedback-trained dentist are recommended, as noted by the American Dental Association. You may also benefit from learning about ear pain linked to TMJ and bruxism.
Experienced users suggest trimming excess adhesive from patches to reduce skin irritation, replacing sensors after workouts, and syncing the app before bedtime. A quick stretching routine—chin tucks and gentle jaw glides—can lower baseline EMG levels, improving device effectiveness.
If these challenges seem manageable, biofeedback could be beneficial. Over half of participants in the 2023 systematic review maintained benefits six months after stopping nightly feedback, indicating potential for lasting change.
Conclusion: The Future of Biofeedback in Bruxism Treatment
Biofeedback offers a new approach to bruxism care, focusing on active muscle retraining rather than passive protection. Early studies show significant reductions in grinding, pain, and dental wear, often surpassing splints alone. The technology is evolving, and larger trials are needed, but the trend is promising.
If you're tired of relying on mouth guards, consult your dentist or sleep specialist about biofeedback. With the right support and commitment, you could teach your jaw some quieter habits.