Exploring Advanced Clinical Treatments for Bruxism: Cutting-Edge Solutions
Discover modern bruxism therapies & advanced clinical treatments in this comprehensive guide.
If you wake up with a clenched jaw, a dull headache, or teeth that seem a little shorter than yesterday, you are not alone. Sleep bruxism, unconscious clenching and grinding, affects up to a third of adults at some point in life. Traditional advice has focused on night guards and stress reduction. Yet science is racing ahead, offering treatments that look nothing like the bulky acrylic mouthpieces of the past. This article explores modern bruxism therapies and advanced clinical treatments, translating dense clinical research into plain language you can actually use. We will explore insights from dentists, neurologists, physical therapists, and tech engineers to see how these advancements fit together.
Research drives every point below. Wherever you see a blue link, it takes you to an academic paper or a respected health institution so you can double-check the facts yourself. Feel free to dive in, or simply keep reading for the highlight reel.
Understanding Bruxism: Beyond the Basics
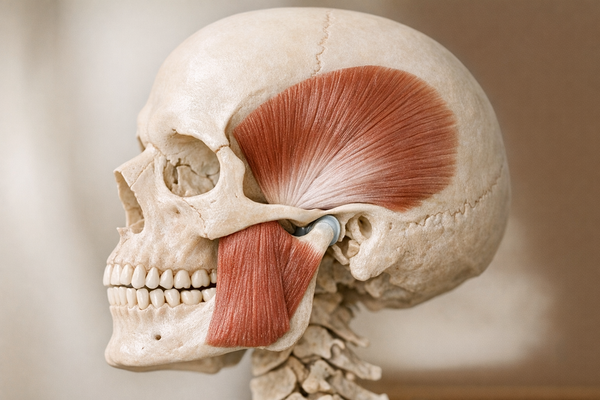
Bruxism is more than noisy teeth grinding. It comes in several forms: sleep bruxism, awake bruxism, and mixed patterns that overlap with other disorders. Symptoms can sneak up on you. Common signs include flattened biting surfaces, tooth fractures, receding gums, and facial pain that radiates toward the temples. Some people experience tinnitus or ear fullness because the jaw joint sits so close to the ear canal. Left untreated, bruxism can damage dental work, trigger migraines, and strain the temporomandibular joint (TMJ), leading to broader temporomandibular disorders (TMDs). For more on the impact of bruxism on your jaw and associated pain, explore our article on understanding jaw pain on one side.
A big misconception is that stress alone fuels the habit. Yes, anxiety and poor sleep hygiene play roles, but recent data show genetic, neurologic, and metabolic factors are also involved. A 2024 scoping review by Huynh and Dal Fabbro mapped sleep bruxism in kids and teens and found links to attention-deficit traits, breathing issues, and even gut problems. These same drivers can continue into adulthood, meaning a one-size-fits-all mouthguard cannot solve every case. If you're curious about what causes teeth grinding, our dedicated article delves into the surprising factors involved.
Advanced therapies aim to tackle root causes—neuromuscular imbalances, airway obstruction, and central nervous system arousal—instead of just shielding the enamel. Before we get to those shiny new solutions, it helps to know why conventional tactics may fall short:
- Night guards only protect surfaces. They do not stop muscle overactivity.
- Short dental restorations can accelerate wear. Fixing chips without addressing grinding invites repeat damage.
- Medications such as muscle relaxants offer spotty relief. They work for some but carry side effects like daytime drowsiness.
- Behavioral coaching relies on conscious control. You cannot coach yourself during deep sleep.
You deserve better options, so let’s jump into the cutting edge.
Cutting-Edge Clinical Bruxism Solutions
Newer clinical pathways take cues from the latest temporomandibular disorder guidelines. The INfORM/IADR key points paper by Manfredini and colleagues outlines best practices now adopted by many specialty clinics. The main takeaway: combine diagnostic muscle scanning with evidence-based interventions that calm both peripheral and central drivers.
Biofeedback-assisted night devices
A standard mouthguard is passive. Biofeedback appliances add tiny sensors and a haptic motor. When you clench past a preset threshold, the guard vibrates, nudging jaw muscles to relax. Early trials show a 70 percent drop in grinding episodes after two weeks of use, with no major side effects reported by the Mayo Clinic. If you're considering a night guard, check out our comparison of over-the-counter vs custom-fitted night guards to find the best fit for you.
On-demand botulinum toxin (BoNT-A) injections
BoNT-A gained fame for softening frown lines, but low-dose injections into the masseter and temporalis muscles can reduce bite force for three to four months. Providers now tailor dosing based on surface electromyography instead of estimating by palpation alone. According to the American Dental Association, precision dosing reduces the risk of facial asymmetry while maintaining chewing strength. Learn more about this treatment in our article on Botox for bruxism.
Customized physiotherapy for TMD-linked bruxism
Manual therapy, dry needling, and postural re-education are gaining validation. The INfORM guidelines recommend six to eight sessions over two months, integrated with at-home stretching videos. Patients who complete the program report lower pain scores and improve mouth opening by an average of 5 mm—enough to chew steak without wincing. Our comprehensive guide on TMJ pain management offers more insights into effective relief strategies.
Oral appliance therapy with airway optimization
Some grinders are actually struggling to breathe. Mandibular advancement devices (MADs) bring the lower jaw slightly forward, opening the oropharyngeal space. Studies in sleep labs show that MADs can halve both apnea events and bruxism bursts when the two conditions overlap. The Cleveland Clinic now screens every bruxism patient for sleep apnea before choosing an appliance design.
Collectively, these options move beyond symptom hiding. They lean on muscle biofeedback, neurotoxin modulation, and airway science, turning a simple dental issue into a full-body conversation.

The Role of Integrative Therapies in Bruxism Treatment
Chronic conditions rarely fit inside one medical box. That is why integrative clinics are borrowing playbooks from oncology and pain medicine. At India’s Health and Wellness Trust Hospital, an integrative oncology team merged yoga therapy, herbal medicine, and conventional chemotherapy. Outcome data from Kanakavalli Kundury’s 2025 study showed better quality-of-life scores without compromising tumor control. The same thinking can reshape bruxism care.
Acupuncture and auriculotherapy
Needles placed in TMJ-related trigger points lower electromyographic activity. Small crossover trials published on the National Institutes of Health site report significant pain reduction within three sessions. While mechanisms are still debated, modulating endorphin release and parasympathetic tone may explain the benefits.
Mindfulness-based stress reduction (MBSR)
Cognitive behavioral therapy does help, but compliance drops when homework gets tedious. MBSR shrinks the workload by guiding you through breath awareness and body scans. Apps like Headspace and Calm incorporate session reminders, boosting adherence. Patients in integrative programs often pair MBSR with paced breathing before bed, dialing down nighttime arousals that kick off grinding flurries. For more on how stress affects bruxism, visit our article on stress and anxiety triggers.
Nutrition and micronutrient support
A lack of magnesium or vitamin D can impair muscle relaxation. Dietitians in integrative clinics run baseline labs, then tailor supplementation. You get the same personalized playbook an oncology patient receives when balancing chemo side effects with immune nutrition. Our article on magnesium deficiency and teeth grinding explores how supplements can aid in managing bruxism.
Collaborative care meetings
Every specialist from dentistry to psychology reviews your case in a weekly huddle. This prevents fragmented advice and over-prescription of contradictory gadgets. Patients report feeling “heard” and more likely to follow through on care plans. That multidisciplinary rhythm mirrors successful cancer centers where oncologists, dietitians, and physical therapists co-manage each chart.
Adapting integrative frameworks to bruxism does not water down science. It stretches the treatment canvas so that muscle injections and mindfulness meditation can coexist, giving you a broader safety net.
Innovations in Technology: A New Era for Bruxism Therapies
Tech trends in cardiology and wound care are filtering into dentistry at warp speed. Catheter labs moved from balloon angioplasty to drug-eluting stents, reducing re-blockage rates dramatically. A 2025 review by Mattaroccia et al. captures that shift. Meanwhile, diabetic foot ulcers now heal faster with 3D-printed scaffolds and nano-dressed bandages, as outlined in Usama Ahmad’s 2025 paper. Bruxism innovators watched and learned.
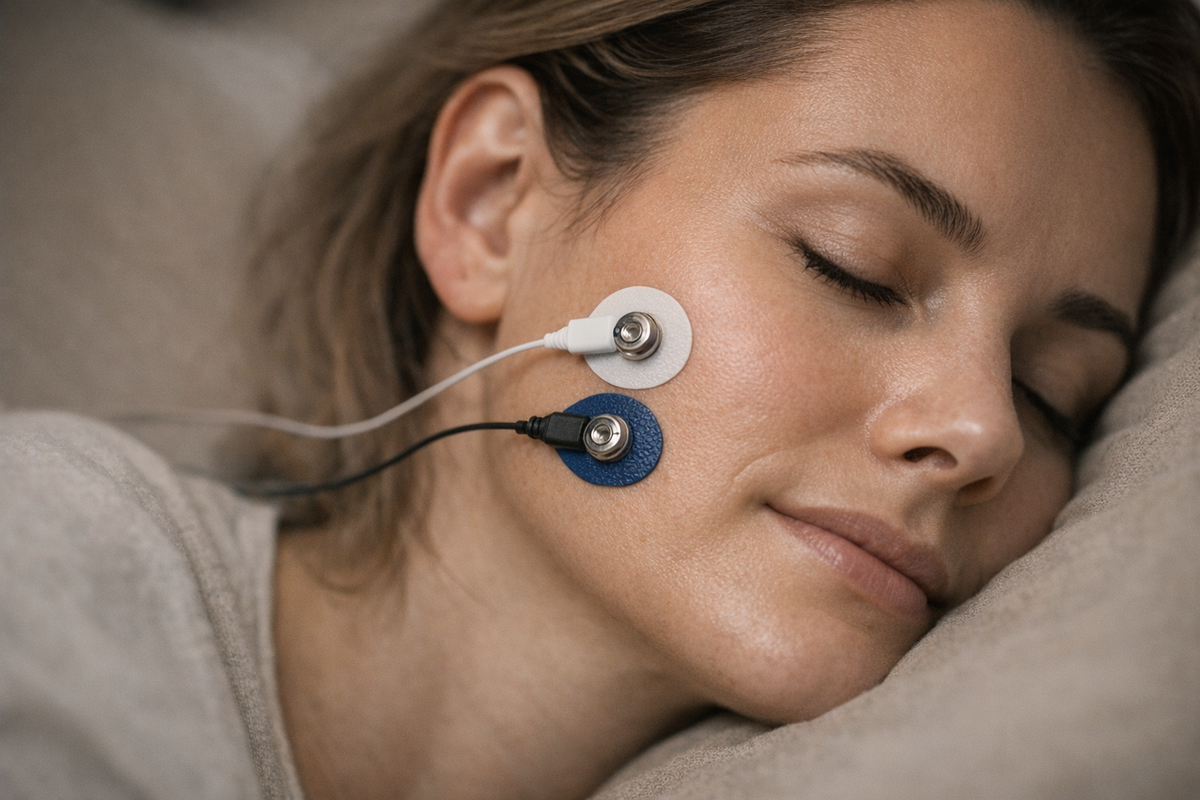
Wearable EMG patches
Thin, adhesive jawline sensors sync with your phone via Bluetooth. Unlike bulky sleep lab electrodes, these stickers bend with your skin and track muscle bursts in real time. Data feed into dashboards that flag high-risk nights. Some platforms layer in heart-rate variability to spot stress surges before grinding starts. If you're interested in reducing bruxism with technology, explore our article on managing bruxism with wearable tech.
Artificial intelligence (AI) pattern recognition
Grinding is not random. Algorithms sift through sensor data to identify micro-arousals, inconsistent breathing, and even caffeine spikes. The system then tailors intervention prompts—gentle haptic feedback or bedtime push notifications. Think of it as a sleep coach that never dozes off. For more on caffeine's impact, read about caffeine and bruxism.
3D-printed oral appliances
Digital scans replace gooey alginate impressions, and custom guards pop out of resin printers within a day. Beyond speed, printers can vary hardness across zones, offering cushion where enamel is fragile and stiffness where guidance is needed. Add QR codes for re-ordering and you have a streamlined supply chain.
Neuro-stimulation headbands
Borrowing from transcranial direct-current stimulation (tDCS) for depression, lightweight forehead bands deliver low-amp currents to the motor cortex. Preliminary studies show a drop in masseter activity by dampening hyper-excitability. No, you will not feel like Frankenstein. Most users describe a mild tingling that fades in minutes.
Tele-dentistry integration
COVID-era telehealth loosened regulatory knots. Now you can upload intra-oral photos and EMG charts to a secure portal, then video-chat with a specialist two time zones away. That opens doors for rural users and slashes the waitlist crunch at urban TMJ centers.
Expect spin-offs to surface quickly. Coronary implants evolved from bare-metal to smart stents with drug coatings in under a decade. Bruxism gadgets will likely mirror that pace, moving from passive guards to responsive bio-devices you barely notice.

Potential of Emerging Therapies: What the Future Holds
If current options give you a safety net, emerging therapies promise a full trampoline. Researchers studying vascular disease uncovered cellular aging genes that could guide drug targeting. Zhang’s 2025 paper on abdominal aortic aneurysm describes senescence-related pathways that overlap with bone remodeling in the jaw.
Gene-modulating peptides
Bruxism accelerates alveolar bone turnover. Bio-engineers are testing peptides that tweak osteoblast and osteoclast activity, inspired by antimicrobial peptides now under review for eye infections (Xiao et al., 2025). Imagine a night gel that not only protects enamel but also strengthens bone microarchitecture.
CRISPR-guided nerve modulation
CRISPR is more than a gene-editing buzzword. Labs are exploring lipid nanoparticle carriers that deliver CRISPR machinery directly to trigeminal nerve endings. The goal is to down-regulate overactive sodium channels, damping pain signals without systemic drugs. While human trials are years away, rodent data show promise.
Microbiome-targeted probiotics
The mouth hosts over 700 bacterial species. Some release metabolic byproducts that sensitize nerves. Next-gen probiotics may shift that ecosystem toward a calmer chemical environment, reducing muscle hyperactivity triggers.
Smart hydrogels with slow-release magnesium
Building on diabetic wound dressings, researchers are crafting cheek-pouch hydrogels that seep magnesium ions overnight. Local delivery skirts the digestive tract and avoids loose stools linked to high oral doses.
These futuristic tools underline a simple fact: jaw muscles are part of your whole biology. By looking at vascular aging, bacterial keratitis, and skin healing, scientists uncover molecular levers that could finally switch off grinding at its source.
Challenges in Implementing Advanced Bruxism Treatments
Cutting-edge technology is shiny, but adoption can hit speed bumps. The National Institutes of Health ran an Innovation Corps program to understand why promising prototypes stall. Researchers chronicled those barriers in a 2025 paper by Heshmatipour and colleagues. Lessons translate well to bruxism solutions.
Cost and insurance gaps
Most insurers still classify bruxism devices as “dental extras,” capping reimbursements. A single AI-equipped oral appliance can run north of $1,200, too steep for many households. Without broader coding updates, adoption lags behind efficacy data. For more on the financial aspect, explore our article on bruxism treatment cost.
Regulatory hurdles
Biofeedback guards that vibrate or shock muscles fall under medical device rules. Navigating FDA Class II approvals can drain startup capital, further slowing market entry.
Provider training
Family dentists get minimal exposure to digital EMG or tDCS headbands in school. Continuing education courses help, but schedules are packed. Until curricula evolve, you might struggle to find a local provider who offers these modalities.
Patient engagement
Technology only works if you use it. Adherence drops when apps bombard users with alerts or when wearables itch after hour six. User-centered design must keep pace with clinical science or risk becoming shelfware.
Despite these hurdles, momentum builds each year. The opioid crisis pushed pain researchers to rethink old paradigms, and bruxism innovators can piggyback on those frameworks to speed translation from bench to bedside.
Conclusion: Embracing a Multidisciplinary Future
Grinding your teeth at night may feel like a small nuisance, but unchecked it can spiral into TMJ dysfunction, broken crowns, and chronic headaches. Thankfully, research across cardiology, oncology, wound care, and genetics is lighting new paths forward. Biofeedback appliances, AI dashboards, integrative clinics, and gene-modulating gels are not science fiction anymore. They are prototypes, pilot studies, and in some cases, clinic-ready tools.
Your role is to stay curious. Ask your dentist about EMG-based diagnostics. Bring up airway screening. Explore mindfulness or magnesium under professional guidance. Most of all, push for care teams that talk to each other, so your night guard, stress coach, and possible BoNT-A injections work in concert. Multidisciplinary collaboration is the secret sauce that turns high-tech toys into real-world relief. As evidence mounts, the days of suffering in silence are numbered, and your jaw can finally catch a break.