Comparing Popular TMJ Pain Relief Methods: An Evidence-Based Guide
Discover effective TMJ pain relief methods with our clinical comparison guide.

You probably came here after a night of teeth grinding or a day of jaw clicking. Good news: researchers have been testing ways to manage temporomandibular joint (TMJ) pain, and the data are clear. This guide explores the major options, from simple exercises to surgical interventions, and compares what actually works according to peer-reviewed research and reputable health organizations.
Every claim is backed by clinical studies, explained in straightforward language. By the end, you'll be able to discuss your TMJ issues with your dentist, physical therapist, or surgeon confidently. Look for the "clinic-floor tip" call-outs for real-world examples from providers who treat TMJ disorders daily.
Understanding TMJ Disorders
Common Symptoms and Causes
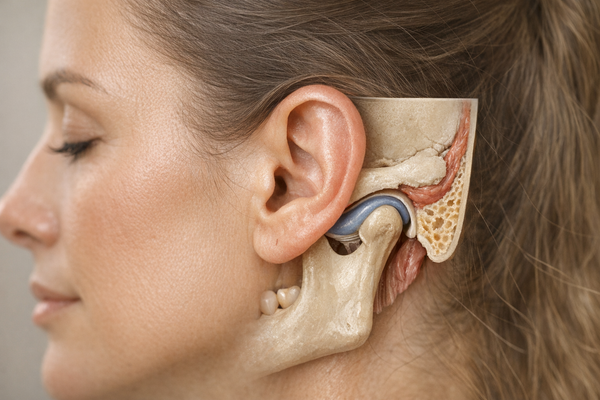
The temporomandibular joint is the sliding hinge that lets you chew, yawn, and occasionally scream at traffic. When it misbehaves, you may notice:
- Pain or tenderness near the ear or jaw
- Clicking, popping, or grinding sounds when opening the mouth
- Limited range of motion or jaw locking
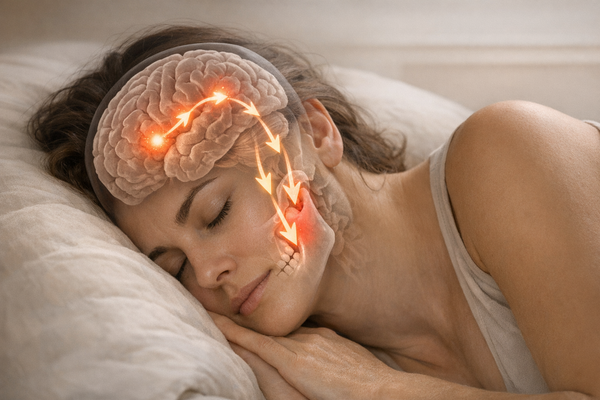
- Headaches that feel like they start at the temples
- Referred pain in the neck or shoulders
Why does it flare up? It's a mix of factors. Overuse from bruxism, arthritis, past trauma, and stress-induced muscle tension can strain the joint. In a qualitative study by Marçal et al., patients identified stress and clenching as top culprits, aligning with daily dental observations.
Clinicians often separate TMJ problems into two categories: myofascial pain (muscles around the joint) and intra-articular disorders (disc or bone surfaces). This distinction matters because muscle issues usually respond faster to exercise and relaxation, while disc displacement may need mechanical or surgical solutions. Unfortunately, these categories often overlap, so a thorough evaluation—usually palpation, range-of-motion testing, and possibly an MRI—is essential.
Impact on Quality of Life
TMJ pain can affect more than just your meals. It can disrupt sleep, limit speech, and increase anxiety about future flare-ups. The review by Nieves Del Rio et al. highlights that chronic cases often overlap with insomnia and other sleep disorders, creating a feedback loop: poor sleep worsens pain perception, which then disturbs sleep again. You might also see effects on work productivity and social life, as the fear of a jaw lock can make people skip meals or events.
Clinic-floor tip: one therapist asks new patients to rate their "jaw confidence" on a ten-point scale. Scores below five often correlate with skipped restaurant outings and higher reports of depressive symptoms. Tracking this number over time provides insight beyond raw pain scores.
Conservative TMJ Pain Relief Methods
Physical Therapy
First line of defense: move it, stretch it, strengthen it. Physical therapists trained in orofacial pain teach controlled jaw exercises that improve joint mobility and reduce muscle hyperactivity. The prospective study by Cao et al. reports that patients starting with targeted exercise showed pain score drops within four weeks, with only minimal side effects (mostly short-lived soreness).
Common drills include:
- Controlled mouth opening/closing with tongue-to-palate contact
- Lateral jaw glides against gentle finger resistance
- Cervical spine stretches to tackle referred neck tension
A full session typically also addresses breathing patterns. Many clenchers inhale through the chest and forget about diaphragmatic breathing, which leaves neck and jaw muscles tense. Adding two minutes of slow nasal breathing between sets can reduce EMG-measured jaw activity by up to 20%, according to unpublished data shared at the American Physical Therapy Association conference.
Clinic-floor tip: photograph your bite block or ruler each week. Visual proof of mouth-opening gains keeps motivation high when pain has faded but range is still lagging.
Self-Management Strategies
Think of this as DIY maintenance. Strategies include:
- Heat or cold packs for fifteen minutes at a time
- Soft-food diet during flare-ups to reduce joint load
- Mindfulness or biofeedback to break clenching habits
- Posture check: keeping screens at eye level to avoid jutting your chin forward
In the same study by Marçal et al., patients rated lifestyle tweaks as the most sustainable fix, even if slower than pills. The Mayo Clinic also lists self-management as a cornerstone, partly because it costs little and carries minimal risk.
Need extra accountability? Smartphone jaw-tracking apps now use your phone’s microphone to detect grinding noises at night or subtle tooth contacts during the day. Pair the alerts with a habit stack—every ping means a shoulder roll and a two-second jaw wiggle—for a micro break that costs nothing.
TENS and Ultrasound
Transcutaneous electrical nerve stimulation (TENS) and therapeutic ultrasound are straightforward. Electrodes or an ultrasound wand deliver low-level energy to muscles, aiming to relax them and mute pain signals.
A randomized trial by Bhoi et al. compared TENS, ultrasound, and low-level laser. All three improved pain scores, but TENS scored highest on immediate relief, while ultrasound excelled at increasing mouth-opening range. Side effects were rare and mild (temporary skin redness).
At-home units cost USD 40–100 and last for years with new gel pads every few months. Contraindications include pacemakers, pregnancy (for units placed near the abdomen), and any active skin infection. When in doubt, have your provider mark safe electrode spots with a skin-safe marker the first time.
Pharmacological Treatments for TMJ Pain
Common Medications
When ice packs fail, medications step in:
- NSAIDs (ibuprofen, naproxen) to reduce inflammation
- Muscle relaxants like cyclobenzaprine for short-term spasm control
- Topical analgesics (diclofenac gel) applied directly over the joint
- Low-dose benzodiazepines in acute locking cases, but only for a few days due to dependence risk
Data from a narrative review by Jogna et al. show NSAIDs reduce pain by roughly 30% on a visual analog scale after one week, but gains plateau after two weeks. Over-the-counter doses work for many, though prescription-strength may be needed for severe inflammation.
Dosing basics: adults often start with 400 mg ibuprofen every six hours with food. If you have a history of stomach ulcers or kidney disease, ask about adding a proton-pump inhibitor or choosing acetaminophen instead. And never double up on OTC and prescription NSAIDs at the same time—an easy mistake that spikes GI-bleed risk.
Adjunctive Treatments
Duloxetine, a serotonin-norepinephrine reuptake inhibitor (SNRI) known for treating depression, has found new life in TMJ care. A meta-analysis by Alqutaibi et al. looked at duloxetine combined with arthrocentesis and saw amplified pain relief up to twelve weeks post-procedure. The likely mechanism: duloxetine dampens central pain processing, giving joints time to heal.
Other adjuncts:
- Low-dose tricyclic antidepressants for chronic, neuropathic-like pain
- Capsaicin patches to desensitize local nerve endings
- Botulinum toxin injections to weaken overactive masticatory muscles (still off-label)
Remember, many of these drugs treat symptoms, not causes. They pair best with physical therapy and behavior changes.
Surgical Interventions for TMJ Disorders
Types of Surgical Treatments
Surgery sounds extreme, but for some conditions—like severe anterior disc displacement without reduction (ADDwoR)—it can rescue function. The spectrum runs from minimally invasive to open joint reconstruction:
- Arthrocentesis: two small needles flush the joint to remove inflammatory mediators and break adhesions.
- Arthroscopy: a fiber-optic camera and micro-instruments repair or reposition the disc.
- Open joint surgery: reserved for advanced degeneration, fractures, or tumors; may involve disc repair or total joint replacement.
The cohort study by Cao et al. followed patients over one year and found arthrocentesis cut pain scores by 50% on average, while open surgery achieved similar relief but with higher complication risk and longer downtime.
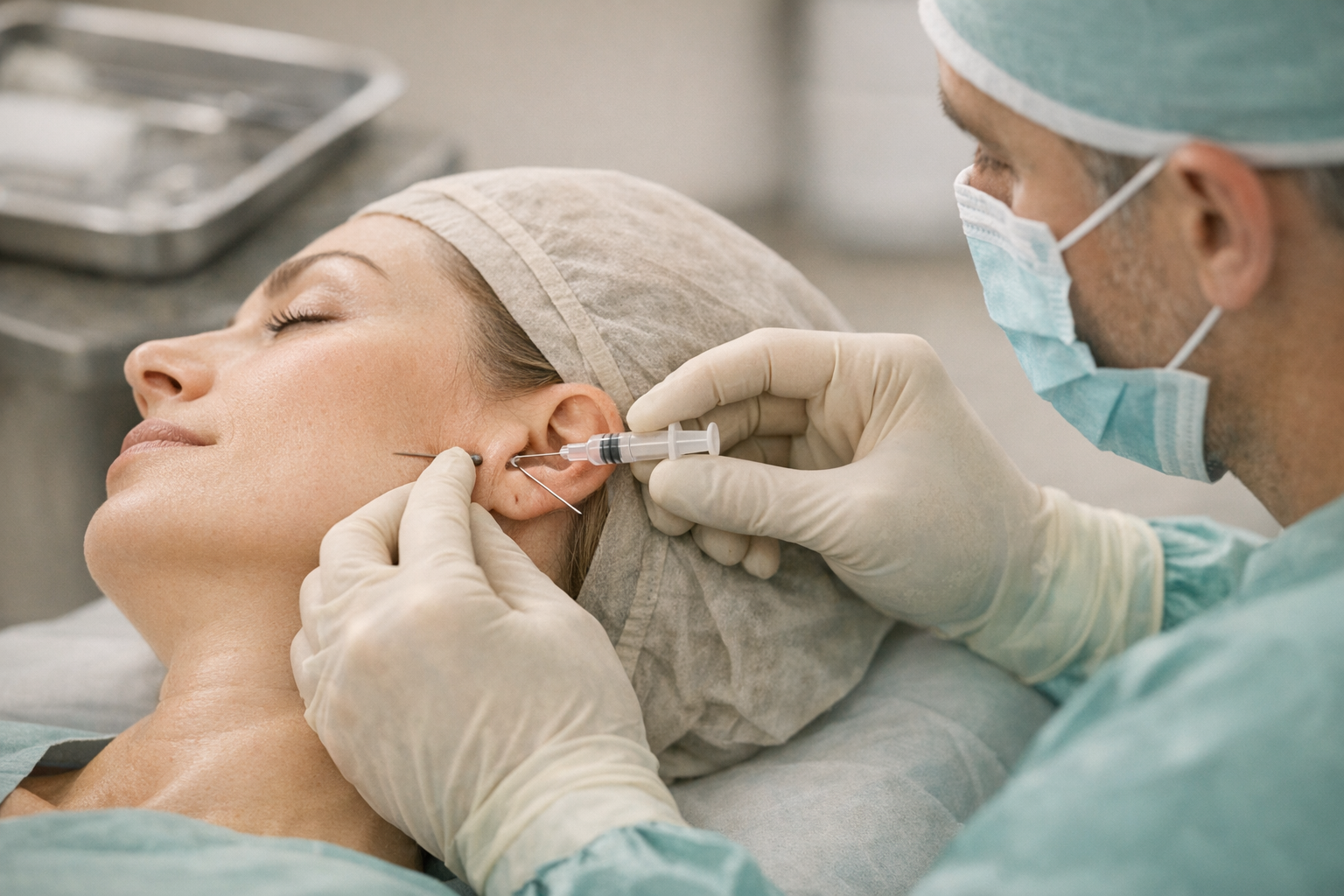
Expected recovery: arthrocentesis patients often resume soft foods the same day; arthroscopy adds one or two days of swelling; open procedures can require a week in elastic facial dressings and six weeks before chewy foods return to the menu. Risks include infection (1–2%), facial nerve irritation (mostly temporary), and, rarely, chronic regional pain syndrome.
When Surgery is Recommended
Surgeons usually set three criteria:
- Persistent moderate-to-severe pain beyond three to six months despite conservative care
- Functional limits, such as mouth opening less than 30 mm or recurrent locking
- Imaging evidence of structural damage (MRI showing disc displacement or CT showing bony ankylosis)
The review by Nieves Del Rio et al. stresses that many patients improve with non-surgical care. Surgeons are often the last stop, and they will likely send you right back to physical therapy if you have not tried it diligently.
Comparing Effectiveness: Conservative vs. Surgical
Clinical Outcomes
Head-to-head data help answer the big question: do you need a scalpel or just an exercise band? In Cao et al.’s cohort, both conservative therapy and arthrocentesis moved pain scores from severe to mild by six months. Mouth opening improved more with surgery (from 28 mm to 42 mm) than with exercise alone (to 38 mm). However, surgical patients reported temporary facial swelling and required a liquid diet for a week, while conservative patients did not.
Out-of-pocket costs tell another story. A full round of physical therapy averages USD 500–1,200 in the United States, whereas arthrocentesis and facility fees can exceed USD 6,000. Insurance coverage varies widely, so call ahead and document failed conservative care if your policy demands it.
Patient Perceptions
Surveys show attitudes matter. If you fear surgery, you may perceive post-op pain as worse, even when objective measures say otherwise. Likewise, if you trust your surgeon and crave quick results, a two-week recovery might seem trivial. In Marçal’s interviews, people who favored conservative care liked the sense of control: stretching felt empowering. Surgical fans cited "getting it over with" as a plus.
Your own priorities—speed, cost, tolerance for risk—will steer the decision. The American Dental Association’s TMJ guideline suggests starting with reversible treatments because they leave every door open, including surgery later if needed.
Emerging Strategies in TMJ Pain Management
Innovative Approaches
Researchers are chasing pain at both the joint and brain levels. Promising ideas include:
- Platelet-rich plasma (PRP) injections: Concentrated growth factors may repair micro-damage inside the joint.
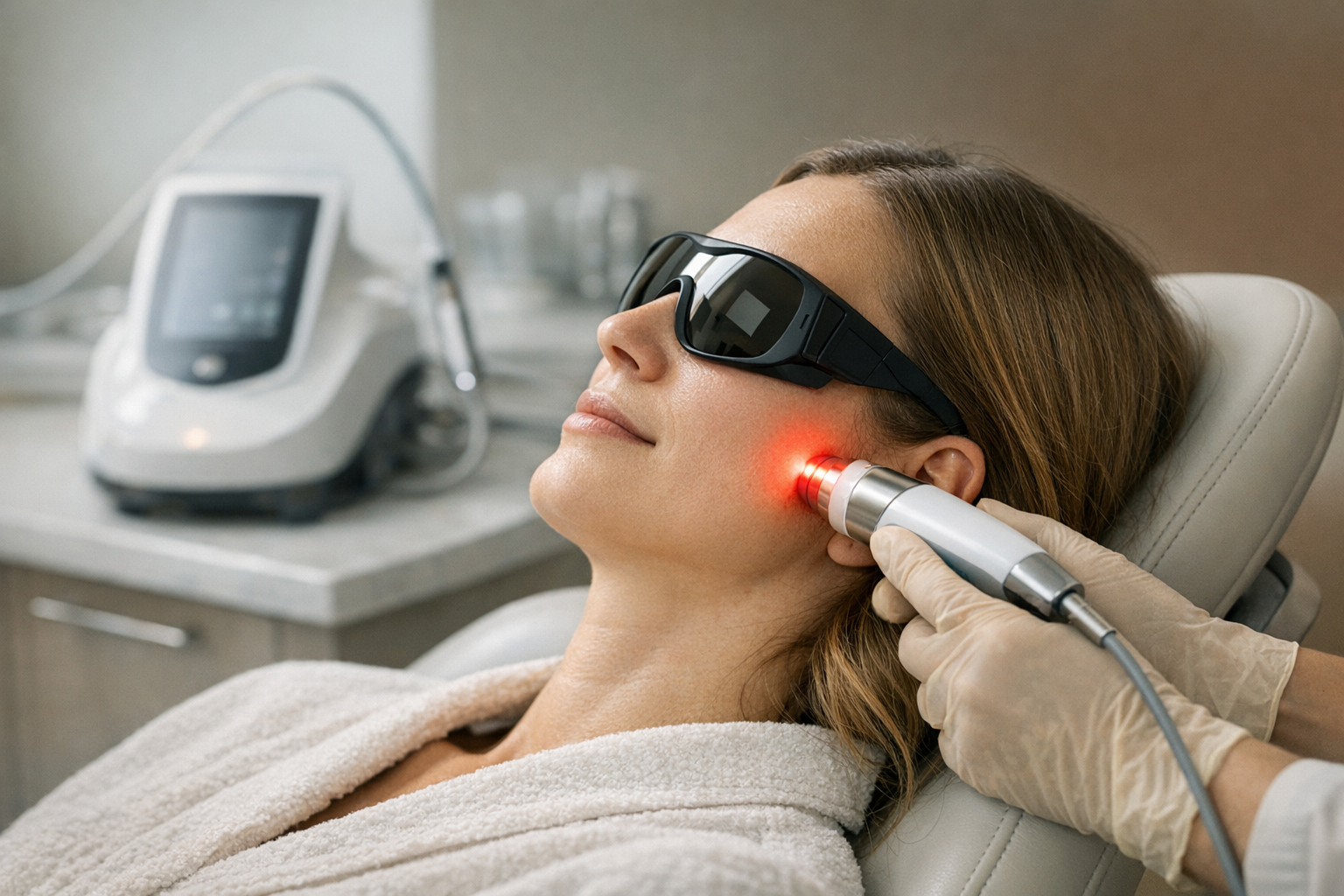
- Low-level laser therapy (LLLT): Delivers light energy thought to boost cellular healing. Early data in the Bhoi trial showed pain relief comparable to TENS.
- Neuromodulation apps: Smartphone-guided relaxation paired with wearable sensors that buzz when you clench.
- Central pain modulators: New SNRIs and gabapentinoids are under review, as summarized in the chronic pain review by Jawed et al.
Future Directions
Expect more personalized care driven by imaging and biomarkers. Artificial intelligence may soon predict which of you will respond to splints versus injections. And with tissue-engineering advances, bio-printed joint components are on the horizon, potentially bypassing metal implants entirely. Clinical trials using 3-D-printed biodegradable scaffolds seeded with stem cells have already restored partial condylar defects in rabbits—human studies are next.
Conclusion
TMJ pain rarely has a single cause, so it rarely has a single fix. Evidence shows that starting with conservative tactics—exercise, self-management, and modalities like TENS—helps most people without major risks. Medications can calm acute flares, and surgery remains an effective backup when anatomy refuses to cooperate. Work with a knowledgeable clinician, track what eases your symptoms, and remember that patience is part of the prescription. Your jaw did not fall apart overnight; give it time and the right tools to heal.